BPH Guide: Symptoms, Diagnosis, Treatment
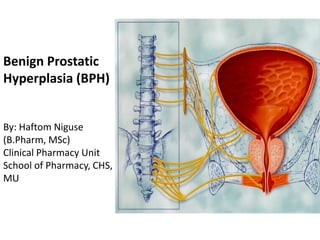
- 1. Benign Prostatic Hyperplasia (BPH) By: Haftom Niguse (B.Pharm, MSc) Clinical Pharmacy Unit School of Pharmacy, CHS, MU
- 2. Introduction • Benign prostatic hyperplasia (BPH) occurs as a result of androgen-driven prostate growth. • It is a common cause of urinary dysfunction symptoms in elderly men • BPH rarely is detected in men <40 years of age. • After age 40, the prevalence of BPH is age dependent. • Approximately 75% of men who live to the age of 70 develop clinical symptoms of BPH. • the initiation of BPH may not be environmentally or genetically influenced.
- 3. Pathophysiology • The cause of BPH is unclear • most hypotheses are based on hormonal and aging processes. • normally functioning testes are essential for BPH to develop • For testosterone to be active, it must be metabolized to dihydrotestosterone (DHT) by 5 α-reductase • DHT is responsible for normal and hyperplastic prostate growth. • 5 α-reductase (type I and type II). Type II is found predominantly in the prostate
- 5. Pathophysiology • There is both a static and a dynamic component to prostate enlargement. – Static (gradual enlargement of the prostate) – Dynamic (increase α-adrenergic tone and constrict the prostate and bladder neck) • Drugs that can exacerbate symptoms: – testosterone, α-adrenergic agonists (e.g.decongestants), and anticholinergic agents (e.g., antihistamines, phenothiazines, TCA, anticholinergics).
- 6. Clinical presentation • Obstructive signs and symptoms – result when dynamic and/or static factors reduce bladder emptying. – Patients experience urinary hesitancy; urine dribbles out of the penis, and the bladder feels full even after voiding. • Irritative signs and symptoms – result from long-standing obstruction at the bladder neck. – Patients experience frequency, urgency, and nocturia. • Symptoms vary over time. – Mild disease may stabilize whereas other patients experience progressive disease over time.
- 7. BPH Pathophysiology Normal BPH Hypertrophied detrusor muscle Obstructed urinary flow PROSTATE BLADDER URETHRA Kirby RS et al. Benign prostatic hyperplasia. Health Press, 1995.
- 8. Diagnosis • objective measures of bladder emptying (e.g., peak and average urinary flow rate, post-void residual urine volume) • laboratory tests (e.g. urinalysis, blood urea nitrogen, and prostate-specific antigen [PSA]). • Medication history and dietary supplements. • On digital rectal examination, the prostate is usually, enlarged (more than 20 g), soft, smooth, and symmetric.
- 9. Desired outcome BPH Treatment Success measured by: • ↓ bothersome symptoms • ↑ QOL • ↓ prostate size or arrest further growth • ↑ in peak flow rate / Relieve obstruction • Prevention of long-term complications • Acceptable adverse events profile
- 10. Treatment • Management options – Watchful waiting – Drug therapy – Surgical intervention. • The choice depends on the severity of signs and symptoms.
- 11. Watchful waiting • Watchful waiting involves reassessment at yearly intervals. • It is appropriate for patients with mild disease and for those with moderate disease with only symptoms • Patients should be educated about behavior modifications – fluid restriction before bedtime – avoiding caffeine and alcohol – frequent emptying of the bladder, – avoiding drugs that exacerbate symptoms.
- 12. Pharmacologic therapy • It is appropriate for patients with moderately severe and as an interim measure in severe BPH. • It interferes with the stimulatory effect of testosterone on prostate gland – -adrenergic blockers – Dynamic component – 5 -reductase inhibitors – Anatomic component – Anticholinergic Therapy – Storage Sx’s
- 13. • Initial therapy with an α-adrenergic antagonist provides faster onset of symptom relief. • A 5α-reductase inhibitor is preferred as initial therapy in patients with a prostate gland >40g. • Combination therapy should be considered for symptomatic patients with a prostate gland >40 g and PSA ≥1.4 ng/mL
- 14. α-Adrenergic Antagonists • α-Adrenergic antagonists relax the smooth muscle in the prostate and bladder Neck – increase urinary flow rates by 2 to 3 mL/sec in 60% to 70% of patients – reducing post-void residual urine volumes. • Terazosin, doxazosin,and alfuzosin are second- generation α-adrenergic antagonists. • their adverse effects include first dose syncope, orthostatic hypotension, and dizziness. – (b/c they antagonize peripheral vascular α1- receptors )
- 15. α-Adrenergic Antagonists • these drugs should be taken at bedtime – to minimize orthostatic hypotension and first-dose syncope with terazosin and doxazosin. • Alfuzosin is less likely to cause cardiovascular adverse effects than other second-generation agents. • Tamsulosin and Doxazosin produce durable responses for 6 and 10 years, respectively • Patients should be slowly titrated to a maintenance dose
- 17. α-Adrenergic Antagonists Tamsulosin • The only third-generation α-adrenergic antagonist, • It is selective for prostatic α1a -receptors. • It does not cause peripheral vascular smooth muscle relaxation. • It is suitable for patients who want to avoid the delay of dose titration. • Dose : 0.4 mg at bed time 2 hours after dinner
- 18. α-Adrenergic Antagonists • Tamsulosin • It is a good choice for patients who cannot tolerate hypotension; – (pts who have severe coronary artery disease, volume depletion, cardiac arrhythmias, severe orthostasis, or liver failure; or are taking multiple anti-hypertensives). • Potential drug interactions. – Tamsulosin decreases metabolism of cimetidine and diltiazem. – Carbamazepine and phenytoin increase catabolism of α-adrenergic antagonists
- 19. 5α-Reductase Inhibitors (5α-RI) • 5α-RI (Dutasteride and Finasteride)interfere with the stimulatory effect of testosterone. • They slow disease progression and decrease the risk of complications. • Dutasteride inhibits types I and II 5α- reductase, whereas finasteride inhibits only type II. • Dutasteride more quickly and completely suppresses intraprostatic DHT (vs. 80% to 90% for finasteride) and decreases serum DHT by 90% (versus 70%).
- 20. 5α-Reductase Inhibitors (5α-RI) • 5α-RI may be preferred in patients with: – uncontrolled arrhythmias, – poorly controlled angina, – use of multiple antihypertensives, – inability to tolerate hypotensive effects of α-adrenergic antagonists. • 5α-RI reduce serum PSA levels by 50%. • PSA should be measured at baseline and repeated after 6 months. • If PSA does not decrease by 50% after 6 months of therapy in a compliant patient, the patient should be evaluated for prostate cancer.
- 21. 5α-Reductase Inhibitors (5α-RI) • Disadvantages of 5α-RI – requiring 6 months to maximally shrink an enlarged prostate, – being less likely to induce objective improvement, – causing more sexual dysfunction. • 5α-RI are in FDA pregnancy category X and are therefore contraindicated in pregnant females. • Pregnant and potentially pregnant women should not handle the tablets or have contact with semen from men receiving 5α-reductase inhibitors
- 22. Surgical intervention Therapy Brief Description Comments Transurethral resection of the prostate (TURP) A resectoscope is inserted into the urethra and obstructing tissue is removed a piece at a time. • considered the “gold standard” for the treatment of BPH Post-TURP syndrome: potentially life threatening, caused by the absorption of irrigating fluid. Cerebral edema and seizures may result from hypervolemia and hyponatermia. Late complications: erectile dysfunction (up to 30%), urinary incontinence, and bladder neck contractures, retrograde ejaculation(75%). Transurethral incision of the prostate (TUIP) Shallow incisions in the prostatic urethra area relieve bladder outflow obstruction. Advantageous in high-risk patients such as the elderly because it can be performed under local anesthesia.
- 23. Therapy Brief Description Comments Transurethral dilation of the prostate (TUDP) Balloon catheter is positioned in the prostatic urethra and inflated. Appropriate for men with smaller prostates who wish to avoid potential side effects of other procedures. Visual laser ablation of the prostate gland (VLAP) Laser is used to partially remove obstructing prostate. Used in men with smaller prostates. Transurethral microwave hyperthermia Local microwave hyperthermia, delivered transurethrally or transrectally. Not as effective as surgical therapy but can be completed as an outpatient in 1 hour.
- 24. Surgical intervention • TURP is the gold standard for treatment of patients with moderate or severe symptoms and for all patients with complications. complications of prostatectomy procedures. • Retrograde ejaculation in 75% of transurethral prostatectomy • Other in 2% to 15% of patients include – bleeding, – urinary incontinence – erectile dysfunction
- 25. Phytotherapy • Although widely used in Europe for BPH, phytotherapy with products such as: – saw palmetto berry (Serenoa repens), – stinging nettle (Urtica dioica), and – African plum (Pygeum africanum) should be avoided. • Studies of these herbal medicines are inconclusive, • The purity of available products is questionable.
- 26. Evaluation of therapeutic outcomes • Monitor restoring adequate urinary flow without causing adverse effects. • Outcome depends on the patient’s perception of effectiveness and acceptability of therapy. • Objective measures of bladder emptying (e.g., uro- flow meter and post-void residual urine volumes) are also useful after – 6 to 12 months of 5α-RI therapy or – 3 to 4 weeks of α-adrenergic antagonist therapy. • Laboratory tests (e.g., BUN, SCr, PSA) and urinalysis should be monitored regularly. • patients should have an annual DRE.
- 27. • G.M., a 72-year-old man, presents to the emergency department with severe lower abdominal discomfort of 4 days' duration. His history consists of having increasing difficulty initiating urination, a significant decrease in the force of his urinary stream, occasional midstream stoppage, and postvoid dribbling. • Physical examination is unremarkable except for the abdominal and rectal examination. Abdominal examination reveals distention, tenderness, and increased dullness in the hypogastrium with a large mass, believed to be the bladder. On rectal examination, the prostate is found to be severely enlarged, firm, and rubbery without nodules or undue hardness. • G.M. gives a history of nocturia (approximately four to five times a night) and daytime urinary frequency (eight to ten times a day). G.M. indicates that when he is able to urinate he does not feel relieved. • Laboratory findings are as follows: BUN, 45 mg/dL (normal, 8–18); SrCr, 3.2 mg/dL (normal, 0.6–1.2); serum prostatic acid phosphatase, 3 U/L; and serum PSA, 7.1 ng/mL (normal, 0.1–4.0). A urethral catheter was inserted, and 900 mL of urine was obtained. • What subjective & objective findings in G.M. are associated with BPH?