GASTRITIS.pptx
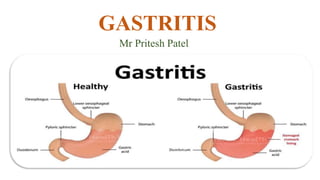
- 2. DEFINITION • Gastritis is a general term for a group of conditions with one thing in common: Inflammation of the lining of the stomach. The inflammation of gastritis is most often the result of infection with the same bacterium that causes most stomach ulcers or the regular use of certain pain relievers. Drinking too much alcohol also can contribute to gastritis.
- 3. CLASSIFICATION 1. Acute gastritis • Acute gastritis is that inflammation of the inner lining of the stomach that comes on suddenly, usually due to a bacterial infection.it is often erosive and hemorrhagic . 2. Chronic gastritis • Chronic gastritis refers to the situation in which the inflammation of the inner lining of the stomach lasts for a long time and its appearance is not sudden, but it is progressive in time.
- 4. ETIOLOGY 1. Acute gastritis :- a. person eats contaminated food b. over use of aspirin and other non –steroidal Anti –inflammatory agents (NSAIDS ) C. Excessive alcohol consumption d. bile reflux e. radiation therapy f .ingestion of strong acid or alkali g. blood infection
- 5. • 2. Chronic gastritis a. Alcohol consumption b. medication ,such as aspirin and ibuprofen c. presence of Helicobacter pylori bacteria d. weak immune system
- 6. • Chronic gastritis is organized into three types based on related causes: • Type A is caused by your immune system destroying stomach cells. And it can increase your risk of vitamin deficiencies, anemia, and cancer. • Type B, the most common type, is caused by Helicobacter pylori bacteria, and can cause stomach ulcers, intestinal ulcers, and cancer. • Type C is caused by chemical irritants like nonsteroidal anti- inflammatory drugs (NSAIDs), alcohol, or bile. And it can also cause stomach lining erosion and bleeding.
- 7. Gastritis risk factors • Risk factors include the following: • Alcohol use • Bacterial infection (e.g., Helicobacter pylori) • Certain medications • Aspirin • Chemotherapy drugs (used to destroy cancer cells) • Iron and potassium supplements • Nonsteroidal anti-inflammatory drugs (NSAIDs; e.g., ibuprofen) • Steroids • Erosion or thinning of the stomach lining (e.g., due to age) • High levels of stress • Smoking
- 9. • What are the symptoms of chronic gastritis Chronic gastritis doesn’t always result in symptoms. But people who do have symptoms often experience: • upper abdominal pain • indigestion • bloating • nausea • vomiting • belching • loss of appetite • weight loss • Upper abdominal pain or discomfort. • Feeling extra full during or after a meal
- 10. Diagnosis • Diagnosis is based on detailed history of food intake , medication taken and disorders related to gastritis. • Perform an upper GI endoscopy. This is to check for inflammation in the esophagus, stomach, and duodenum. Your doctor may take a small sample, or biopsy, of the lining of the stomach. A pathologist will examine this sample for anything unusual under a microscope. • blood test. This is to check for other causes for your gastritis symptoms or signs of complications. • stool sample. This may rule out an H. pylori infection or blood in your stool. Blood may indicate there’s bleeding in your stomach.
- 11. Medical management • Antibiotics: A single course of antibiotics can often directly treat Helicobacter pylori. A doctor may prescribe clarithromycin (Biaxin) and metronidazole (Flagyl). • Proton pump inhibitors: Omeprazole (Prilosec) or lansoprazole (Prev acid), for example, can block the production of acid and aid healing. • H2 blockers: These drugs, which include famotidine (Pepcid), can decrease acid production. • Antacids: These medications can neutralize stomach acid. Many are available for purchase online. • Coating agents: Sucralfate (Cara fate) and misoprostol (Cytotec) can coat and protect the stomach lining. • Antinausea medications: Several antinausea drugs are available for purchase online.
- 12. NURSING MANAGEMENT • Observe the signs of dehydration • Assess fluid intake and output • While assessing patient with gastritis, nurse should carefully focus on risk factors. • Help patient to assess factors which may increase symptoms,such as stress and fatigue. • Teach patient about the causes of gastritis • Instruct patient to avoid low calorie food • Reduce patient’s anxiety level • Promote optimal nutrition and fluid balance . • Administer medications as ordered. • Administer fluid as order to maintain fluid and electrolyte balance . • Provide comfort measures to patient
- 13. Nursing Process • Assessment • Obtain history • Assess the signs and symptoms of gastritis. • Evaluate the presence of abdominal pain and tenderness • Monitor vital signs and laboratory test • Nursing diagnosis 1. Acute Pain related to inflammation of gastric mucosa. 2. Risk for Deficient Fluid Volume related to inadequate intake, vomiting. 3. Imbalanced nutrition less than body requirements related to inadequate intake 4. Anxiety related to disease progress and physical weakness. 5. Knowledge Deficit: about diseases related to lack of information.
- 14. • Nursing Interventions • Relieving Pain • Assess the patient’s level of pain and extent of discomfort • Provide analgesics and assess the effectiveness of medications. • Instruct the patient to avoid foods and beverages that may be irritating to the gastric mucosa
- 15. • Promoting Fluid Balance • Monitor the patient’s vital signs • To recognize early signs of dehydration, keep track of the patient’s fluid intake and output on a daily basis. • Monitor electrolyte values • Assess the sign and symptoms of hemorrhagic gastritis (vomiting of blood, tachycardia, and hypotension) • Promoting Optimal Nutrition • Keep track of daily fluid intake and outflow and blood serum electrolyte levels. • Instruct the patient not to take foods or fluids by mouth until the acute symptoms subside • After the symptoms subside, offer clear liquids and introduce solid food as soon as possible • Discourages the intake of caffeinated beverages, alcohol use, and cigarette Smoking • Provides physical and emotional support to manage the symptoms • Initiates and refers the patient for alcohol counseling and smoking cessation programs.
- 16. • Reducing Anxiety • Use a calm approach to assess the patient • Explain all procedures and planned treatment modalities • Answer all questions as completely as possible • Promoting self and continuous care • Evaluate the patient’s knowledge about gastritis • Provide the information about prescribed medications, diet, stress management, and substances to be avoided • Given dietary instructions along with the recommendation of the dietitian • Emphasizes the importance of keeping follow-up appointments with health care providers