Gastroenteritis.pptx
- 1. GASTROENTERITIS Mr Pritesh Patel ASSISTANT PROFESSOR
- 2. •When you have diarrhea and vomiting, you may say you have the "stomach flu." These symptoms often are due to a condition called gastroenteritis. •With gastroenteritis, your stomach and intestines are irritated and inflamed. The cause is typically a viral or bacterial infection.
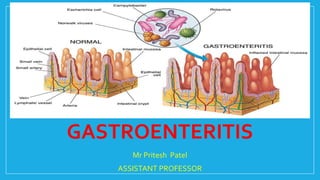
- 3. GASTROENTERITIS •Gastroenteritis is an inflammation of stomach and small intestine. Infectious diarrhea is commonly referred to as gastroenteritis. It is also known as enteritis. It may be acute or chronic. •1. Acute enteritis is self limiting and continue till the causative agent is excreted. •2. Chronic enteritis lasts for at least 4 weeks.
- 4. Etiology 1 The main cause of gastroenteritis is usually a virus or bacteria They both are very contagious. They can spread through the consumption of contaminated food or water. 2. Antibiotic therapy: Diarrhea may be caused by antibiotic therapy. 3. Other causes: Sea food, food allergies and heavy metals. The most common cause of gastroenteritis is a virus. The main types are rotavirus and norovirus. • Rotavirus is the world's most common cause of diarrhea in infants and young children. Norovirus is the most common cause of serious gastroenteritis and also foodborne disease outbreaks in the U.S. • Although not as common, bacteria such as E. coli and salmonella can also trigger the stomach flu.
- 5. Risk Factors 1. Immunocompromised. 2. Poor personal hygiene. 3. Virus gastroenteritis is associated with crowds and occurs more in fall or winter months.
- 6. Clinical Manifestations • 1. Gastrointestinal effects:- • a. Borborygmi (gurgling noise made from gas/fluid inside abdomen). • b. Diarrhoea • c. Anorexia, nausea or vomiting. • d. Abdominal pain and cramping. • 2. General effects: a. Fever • b. Headache • c. Dry skin and mucous membrane.. • d. Malaise (feelling of weakness), weakness and muscle aches.(over use,muscle injury ) • e. Poor skin turgor (a late sign of dehydration )
- 7. Diagnostic Evaluation • 1. Stool test: Patient's stool specimen may be collected for culture, ova and parasites and fecal leukocytes and determine the exact cause of vomiting and diarrhea. It may require up to 6 weeks to identify bacteria. • 2. Laboratory testing is used to identify the causative organism and to assess fluid, electrolyte and acid- base balance. • 3. Sigmoidoscopy: It is performed to differentiate in- flammatory bowel disease from infectious processes. • 4. Serum osmolality and electrolytes and ABGs are done to assess and monitor fluid, electrolyte and acid base balance.
- 8. Medical Management • Gastroenteritis Treatment:- • Prevent dehydration: • Give a child an oral rehydration solution. Call your doctor for age-appropriate dosing specifics. • Give an adult as much clear fluid as possible. • The person should drink fluids slowly in frequent, small amounts. Drinking too much too fast can make nausea worse. • As symptoms start to ease: • Gradually ease food back into the person's diet. • Start with bland, easy-to-digest food such as crackers, toast, rice, and chicken. • Avoid dairy, caffeine, and alcohol until recovery is complete.
- 9. • Rotavirus vaccine :-it is given for the prevention of rotavirus gastroenteritis • Metronidazole :- is is recommended for mild to moderate cases of colitis • IV ondansetron and metoclopramide: Helps to reduce the episodes of vomiting.
- 10. Surgical Management •Gastric lavage: • 1. It includes washing out the stomach and intestine. • 2. Gastric lavage is performed to remove unabsorbed toxins from gastrointestinal tract, if botulism is suspected. • Gastric lavage involves the passage of a tube via the mouth or nose down into the stomach followed by sequential administration and removal of small volumes of liquid. The placement of the tube in the stomach must be confirmed by pH testing a small amount of aspirated stomach contents, or x-ray. This is to ensure the tube is not in the lungs.
- 11. Prevention: • Get child vaccinated •Wash hands thoroughly • Use separate personal items around home • Keep distance • Disinfect hard surfaces • Check out child care center
- 12. Nursing Management 1. Nurse plays a significant role in preventing gastroenteritis or enteritis as educator, community health providers. 2. A nurse must carefully note a description of diarrhea, including onset, number of stools, color consistency and accompanying symptoms such as nausea or vomiting. 3. Ask patient about recurrent foreign travel, eating habits and antibiotic use. 4. Carefully examine patient's entire stool for blood and mucus. 5. Record intake and output. 6. Administer medications to treat the specific cause of diarrhea.
- 13. Nursing Care Plan • Nursing Assessment • 1. Assess patient's stool characteristics including onset, number of stools, color and consistency. • 2. Monitor patient's vital signs. • 3. Record intake and output strictly. • 4. Assess for vomiting. • 5. Assess patient's abdomen. • 6. Ask patient's recent foreign travel, eating habits and antibiotic use.
- 14. Nursing Diagnosis • 1. Diarrhea related to intestinal hypermotility.(excessive movement ) • 2. Fluid volume deficit related to gastrointestinal fluid and electrolyte loses. • 3. Hyperthermia related to dehydration. • 4. Impaired skin integrity related to constant presence of diarrheal stools.
- 15. Nursing Goals 1.To control diarrhea. 2.To maintain fluid and electrolyte level. 3.To maintain skin integrity.
- 16. Nursing Interventions 1.Educate family members about the cause and treatment of gastroenteritis. 2. Teach the importance of proper food handling and maintain appropriate temperature. 3. Patient's abdomen assessment helps to reveal hyperactive bowel sounds, distention and tenderness. 4. Examine patient's anal area for irritation. 5. Instruct patient to apply petroleum jelly after cleaning the anal area 6. Antidiarrheal may be ordered, if the diarrhea is uncontrollable. 7. If patient shows signs of fluid and electrolyte imbalance, intravenous fluids may have to start until oral fluids are tolerated. 8.Instruct family members to change diapers as soon as possible. 9. Monitor patient's weight daily. 10. Encourage patient and family members to talk about their concerns and ask questions.
- 17. Patient Education and Health Maintenance 1. Educate patient about the importance of good hand washing, particularly before handling food and after each bowel movement. 2. Instruct family members to wear gloves when handling articles contaminated with feces. 3. Instruct family members to place contaminated linens and clothing in marked containers to be processed according to facility policy. 4. Clean genital area and apply soothing protective preparation, such as lanolin A and D ointment. 5. Change diapers as quickly as possible. 6. Weight infant daily. 7. Instruct family members to maintain infant's good mouth care.