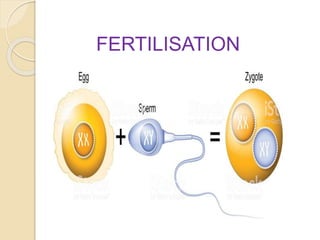
Fertilisation
- 2. Learning objectives: Upon completion of the chapter, the Students will be able to: Define fertilization Describe the process of fertilization and implantation Explain the functions of the placenta, umbilical cord, and amniotic fluid.
- 3. What is fertilization? Fertilization is the union of an ovum and a spermatozoon. This usually occurs in the outer third of a fallopian tube, the ampulla.
- 5. Process of fertilization Following ovulation the ovum which is about 0.15 mm in diameter, passes into the uterine tube and move towards the uterus. Ovum having no power of locomotion, it move by the muscular contraction of the fallopian tube. At intercourse about 300 million sperms are deposited in the posterior part of the vagina.
- 6. These are travels towards the fallopian tube & more will die on the journey. Only thousands of sperms reached the “Ampulla” of fallopian tube, where the fertilization takes place. During journey the sperm becomes mature and release the enzyme Hyaluranidase. Which helps for the penetration of cell membrane & enter into the ovum. Many sperms are needed for this but only one will enter into the ovum.
- 7. ZYGOTE
- 8. After this the membrane is sealed to prevent entry of further sperms. The sperm & ovum both contributes 23 chromosomes to make a total of 46 chromosomes. The fertilized ovum is called as zygote.
- 9. Development of fertilized ovum When the ovum has been fertilized it continues its passage & reaches the uterus 3 or 4 days later. During this travel segmentation or cell division takes place & the fertilized ovum divides into 2 cells then into 4 then 8,16 and so on, until a cluster of cells formed known as Morula
- 12. 12 hours later a fluid filled cavity blastocele appears from the Morula. It changes into blastocyst. Around the outside a layer of cells formed called Trophoblast. The remaining cells clumped together and forms Inner cell mass
- 13. The blastocyst moves into the uterus for 2 or 3 days, then the innercell mass forms a finger like projection & it becomes sticky to adhere into the endometrium (inner layer of uterus) Finally it attached with the endometrium of uterus, known as implantation.
- 14. Implantation
- 15. Decidua This is the name given to the endometrium during pregnancy. The increased secretion of estrogen during pregnancy causes the endometrium to grow four times than non pregnant time. Due to more vascular supply the endometrium becomes spongy bed in which the fertilized ovum implants.
- 16. Layers of decidua Three layers in decidua 1. Basal layer 2. Functional layer 3. Compact layer
- 17. 1. Basal layer It lies immediately above the myometrium. It remains unchanged during pregnancy. But it helps to regenerate after the delivery 2. Functional layer This layer consist of rich in nutrients, it acts like a storage of nutrients for the development of placenta & fetus.
- 18. 3. Compact layer: This layer contains more blood supply and also called as spongy layer. In which the placenta attached & gives nutrients to the developing fetus.
- 19. Blastocyst Trophoblast Innercellmass Placenta Chorion Amnion Fetus Umbilical cord
- 20. Trophoblast It helps for eroding the blood vessels to get nutrition for the growing fertilized ovum. It produces a Hormone hCG (Human Chorionic Gonadotrophin)it is responsible for informing corpus luteum, that pregnancy begins. It produces progesteron to maintain the endometrium & it suppresses the menstruation.
- 21. Inner cell mass It has three different layers: 1. Ectoderm : this layer mainly forms the skin 2. Mesoderm: this layer forms the bones, muscles, heart, blood vessels & other internal organs 3. Endoderm: this layer forms mucous membrane, & glands
- 22. Amniotic Fluid
- 23. Definition It is a fluid which is surrounding the fetus during intrauterine life.
- 24. Functions of amniotic fluid Allows for the growth & free movement of fetus Equalizes pressure & protect the fetus from injury Maintains temperature for the fetus It gives nutrients Protects placenta & membranes from pressure during labour
- 25. Origin of Amniotic Fluid The source of amniotic fluid is from both fetal & maternal. It is secreted mainly from amnion (inner covering layer of fetus) & a part from placenta. Fetal urine also contribute some amount from the 10th week of gestation. The water in the amniotic fluid exchanges as often as every 3 hours.
- 26. Volume of amniotic fluid The amount of amniotic fluid increases through out the pregnancy until 38 weeks of gestation. It is about 800- 1200 ml. After 38 weeks it diminishes and about 800ml.
- 27. Abnormal volume of amniotic fluid 1. Polyhydramnios: When the total amount of amniotic fluid exceed more than 1500 ml is called as Polyhydramnios.
- 28. 2.Oligohydramnios: When the total amount of amniotic fluid exceed less than 300 ml is called as Oligohydramnios.
- 29. Constituents of amniotic fluid It is a clear pale colour, fluid consist of 99% water and 1% includes nutrients, vernix caseosa, lanugo like solid substances
- 30. Umbilical cord It is also called as funis. It extends from the fetus to the placenta. It transmits the umbilical blood vessels. It is enclosed and protected by wharton’s jelly a gelatinous substance formed from mesoderm.
- 31. Cross section of umbilical cord It consist of 2 arteries and one vein. Covered by amnion.
- 32. Length of umbilical cord Normal length is about 50 cm Long cord : >55 cm, may wrap around the neck during labour Short cord: <40 cm, may cause premature separation of placenta.
- 33. The Placenta What is placenta? The placenta (also known as afterbirth) is an organ that connects the developing fetus to the uterine wall to allow nutrient uptake, thermo- regulation, waste elimination, and gas exchange via the mother's blood supply
- 34. The placenta provides oxygen and nutrients to growing fetuses and removes waste products from the fetus's blood.
- 35. Structure The placenta averages 22 cm (9 inch) in length and 2–2.5 cm (0.8–1 inch) in thickness, with the center being the thickest, and the edges being the thinnest. It typically weighs approximately 500 grams. It has a dark reddish-blue or crimson color. It connects to the fetus by an umbilical cord of approximately 55–60 cm (22–24 inch) in length, which contains two umbilical arteries and one umbilical vein.
- 36. Development The placenta begins to develop upon implantation of the blastocyst into the maternal endometrium. The placenta grows throughout pregnancy. Development of placenta is complete by the end of the first trimester of pregnancy (approximately 12–13 weeks).
- 37. Functions Nutrition- The placenta intermediates the transfer of nutrients between mother and fetus. Excretion -Waste products excreted from the fetus such as urea, uric acid, and creatinine are transferred to the maternal blood by diffusion across the placenta.
- 38. Storage: Placenta stores some fats, glycogen and iron. Immunity : IgG antibodies can pass through the human placenta, thereby providing protection to the fetus in utero.
- 39. Endocrine function 1. HCG:The first hormone released by the placenta is called the human chorionic gonadotropin hormone. This is responsible for stopping the process at the end of menses 2. Progesterone helps the embryo implant by assisting passage through the fallopian tubes. 3. Estrogen involves the enlargement of the breasts and uterus, allowing for growth of the fetus and production of milk. 4. Human placental lactogen is a hormone for growth and development
- 41. Genetic Factors Many genes contribute to fetal growth and birthweight. Such studies have shown that both maternal and paternal influences are present during fetal development.
- 42. Maternal Nutrition A baby derives the nourishment for its growth from the mother’s blood. Folic acid is needed for the development of neural tube, calcium for bones, proteins for muscle growth and repair etc.
- 43. Smoking Smoking definitely affects the fetal development. Smoking increase the risk of having a low birth weight baby. It also increases the risk for prematurity. Smoking reduces the supply of oxygen received by the baby and increases the risk of miscarriage
- 44. Diseases Certain diseases cause deformities in the baby. Chicken pox usually causes malformed limb or sudden labour. Viral infections causes developmental abnormalities in the baby like mental retardation, blindness etc.
- 45. Drugs Drugs and chemicals can cross into the fetal blood, affecting its development. Stay clear of addictive drugs like cocaine, heroine etc. This can also lead to addictions in the baby
- 46. Maternal Age Maternal age does influence the fetal development. There are chances for miscarriages and still births in mothers below 20 years old. There are chances for birth defects, still births, bleeding etc. in mothers over 35 years
- 47. Prenatal care Prenatal visits to the doctor are extremely important. The doctor monitors the growth of the baby. The doctor recommends supplements or other vitamins as and when necessary.
- 48. Videos Fertilization Fetal Development: https://www.youtube.com/watch?v=Wt Dknjng8TA Human life in uterus