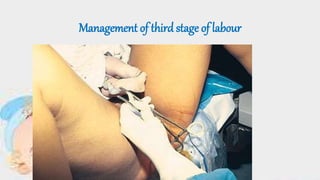
Management of third stage of labour
- 1. Management of third stage of labour
- 2. DEFINITION • The third stage of labor lasts from the birth of the baby until the placenta is expelled. It is known as the placental stage of labour.
- 3. principles • Ensure strict vigilance and to follow the management guidelines in practice to prevent complications. • The placental separation and its descent into the vagina are allowed to occur spontaneously. Constant watch is needed; the mother should not be left alone.
- 4. primary and secondary mechanismfor placental separation
- 5. Primary mechanism is the reduction in surface area of placental site as the uterus shrinks
- 6. Secondary mechanism is the formation of haematoma due to venous occlusion and vascular rupture in the placental bed caused by uterine contractions
- 7. • PHYSIOLOGICAL PROCESSES OF PLACENTAL SEPERATION AND EXPULSION • Placental separation. • Descend of the placenta. • Expulsion of the placenta.
- 8. PLACENTALSEPERATION • result of the abrupt decrease in size of the uterine cavity . • the retraction process accelerates. •The formation of retro placental clot.
- 9. Before separation • Per abdomen: • Uterus become discoid in shape, firm in feel and ballottable. • Fundal height reaches slightly below the umbilicus. • Per vaginum: • There may be slight trickling of blood. • Length of the umbilical cord as visible from outside remains static.
- 10. After separation • Per abdomen: • Uterus become globular, firm and ballottable. • fundal height is slightly raised. • supra pubic bulging • Per vaginum: • Slight gush of vagina bleeding. • Permanent lengthening of the cord.
- 11. Descend of the placenta • Sudden trickle or gush of blood. • Lengthening of the umbilical cord. • Change in the shape of the uterus, globular. • Change in the position of the uterus.
- 12. Signs of Separation andDescent • lengthening of the umbilical cord outside. • The uterusbecomes • firm and globular (Descent). • The uterus rises inthe abdomen. • A gush of blood(separation ).
- 13. EXPULSION OF THEPLACENTA The Schultz mechanism o Placenta separates in the centre and folds in on itselfas it descends into the lower part of uterus (80%). oFetal surface appears at vulva with membranes trailing behind oMinimal visible blood loss asretroplacental clot contained within membranes (inverted sac)
- 14. • Mathew Duncan mechanism • separation starts at the lower edge of placenta • lateral border separates (20%). • maternal surface appears first at vulva • Usually accompanied by more bleeding from placental site due to slower separation and no retro placental clot.
- 15. haemostasis • Retraction of the oblique uterine muscle fibres . • vigorous uterine contraction following placental separation. • transitory activation of the coagulation and fibrinolytic systems.
- 16. Assess the uterus 1 To exclude an undiagnosed twin 2 To determine a baseline fundal height 3 to detect the signs of placenta separation 4 to detect an atonic uterus.
- 17. 1. Normal blood flow through placenta site is 500-800 ml/minute (10-15% of cardiac output) 2.Strong contraction/retraction of uterus constrict blood vessles by interlacing muscle fibres in myometrium (“living ligature”) 3 . Pressure exerted on placental site by walls of contracted uterus 4 . Blood clotting mechanism (sinuses and torn vessels)
- 18. Management of the Third Stage of Labour Guard the uterus to keep yourself and anyone else from massaging it prior to placental separation. Do not massage the uterus before placental separation, except when partial separation has occurred by natural processes and excessive bleeding evident.
- 19. • Do not pull on the umbilical cord before the placenta separates or ever with an uncontracted uterus. • Do not try to deliver the placenta prior to its complete separation unless in the emergency of third stage haemorrhage. • Wait for the natural process to occur and do not interfere.
- 20. Expectant management • A hand is placed over the fundus to feelthe signs of placental separation. • the client asked to bear down simultaneously with the hardening of the uterus. • If the placenta fails to expel, one can waitfor upto 10 mts. • soon as the placenta passes through the introitus, it is grasped by both hands and twisted round and round or slightly up and down with gentle traction .
- 21. Controlled cord traction [ modified Brandt-Andrews method]:
- 22. • EXPRESSION BY FUNDALPRESSURE • This is done by placing four fingers of the hand behind the fundus and thumb in front of the uterus to use as a piston. The uterus is made to contract by gentle rubbing. When the uterus becomes hard, it is pushed downwards and backwards. The pressure should be withdrawn as soon as the placenta passes through the introitus.
- 24. •management • Active management includes a prophylactic oxytocic drug,early clamping and cutting of cord and controlled cord traction • Physiological management involves no prophylactic oxytocic drugs, no cord clamping until after placental delivery and no cord traction
- 25. Physiological Management • Passive or expectant management • No prophylactic oxytocics • Cord clampedafter delivery of placenta • No Controlled Cord Traction(CCT)
- 26. Use of oxytocic agents • Prophylacticuse • the administration of an oxytocic drug at the time of delivery of the anterior shoulder. • Therapeuticadministration • This method implies the use of an oxytocic either to stop the bleeding once it has occurred or to maintain the uterus in a contracted state when there are indications that excessive bleeding is likely to occur.
- 27. • Upright/kneeling/squatting position best- easy to observe blood loss • Hands off just check uterus contracted and observe PV loss • waits and watches for signs of separation and descent • Mother expels placenta when she feels contraction and placenta in vagina
- 28. ActiveManagement • Reduces length of 3rdstage and incidence of PPH (blood loss and need for transfusion) • Oxytocic given after birth of Shoulder (check for a twin/ no shoulder dystocia) • Cord clamped and cut •Placenta delivered by •Controlled Cord Traction
- 29. FUNDAL HEIGHT DURING THIRD STAGE • At the end of the third stage following the expulsion of the placenta, the fundus is about 4cm below the umbilicus.
- 32. Controlled cord traction • CHECKS FIRST! • Check that an oxytocic (uterotonic) has been given Why? • Check that the uterus is well contracted Why? • Check that countertraction is applied (Brandt- Andrews manoeuvre) Why? • Check for signs of separation & descent • Why? • Check that cord traction is released before countertraction is stopped Why?
- 33. COMPLETION OF THIRDSTAGE • Continuingevaluation • ensure that the uterus is wellcontracted • Slight lacerations are usuallyrepaired immediately • The vulva and perineum are gentlycleansed • mother’s blood pressure, pulseand temperature should be taken • Once the mother is comfortable theplacenta and membranes is the next priority
- 34. Which is better active or physiologic management ? Active management is superior to physiological in terms of blood loss Physiological management is only appropriate for women with low risk of PPH and who have normal physiological labour If physiological management is attempted but intervention is subsequently required ( the placenta is retained after one hour) active management should be considered.
- 35. Manual removal of retainedplacenta
- 36. After Care: Before leaving to check placenta and membranes • Check the uterus is well contracted • Check that PV loss is minimal • Inspect perineum, vulva and vagina in good light (? Repair) • Baby should be pink (respirations; heart rate) warm, fed, cord clamp secure
- 38. • Infarctions that are recent orold • Localizedcalcifications • Lobes • Bloodvessels • Insertion of thecord • Umbilicalvessels • Cordlength • Weight of placenta
- 39. Immediate care to new born
- 40. Air passage should be cleared of mucus and liquor by gentle suction (mucous sucker).
- 41. Soon after the delivery of the baby, it should be placed in a tray covered with clean dry linen with the head slightly downwards (15.0).
- 42. • It facilitates drainage of the mucus accumulated in the tracheo-bronchial tree by gravity.
- 43. APGAR rating at 1 minute and 5 minutesto be recorded which includes, the appearance, pulse, grimace, activity and respiration.
- 44. • The presence of any abnormalities of cord is noted, and then it is covered with sterile gauze piece.
- 45. A quick check is made to detect any gross abnormality and the baby is dried and wrapped with a dry warm towel
- 46. The identification tape is tied both to the baby and the mother.
- 47. One hour following the complete delivery of the baby, the baby should be fed
- 48. COMPLICATIONS OFTHE THIRD STAGE Post partum haemorrhage. Hematoma formation. Retained placenta Inversion of uterus. shock
- 49. Management of fourth stage of labour
- 50. •First postpartum hour Monitor vital signs and bleeding •Repair lacerations ensure uterus is contracted (palpate uterus and monitor uterine bleeding) •A hand is placed over the funds ◦ To note the state the uterine activity-Contraction and relaxation. ◦ To detect cupping of funds
- 51. • The uterus is palpated to assess the degree of contraction. The fundus should be firm at the level of umbilicus or below. The Perineal pad is observed for lochia, color, clots and amount.
- 52. Abnormal implantation of placenta
