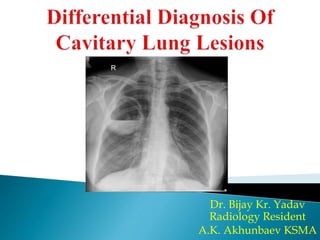
Differential diagnosis of cavitary lung lesions
- 1. Dr. Bijay Kr. Yadav Radiology Resident A.K. Akhunbaev KSMA
- 2. A lung cavity or pulmonary cavity is an abnormal, thick- walled, air-filled space within the lung. The terms cavity and cyst are frequently used interchangeably; however, a cavity is thick walled (at least 5 mm), while a cyst is thin walled (4 mm or less). The distinction is important because cystic lesions are unlikely to be cancer, while cavitary lesions are often caused by cancer. Diagnosis of a lung cavity is made with a chest X- ray or CT scan of the chest, which helps to exclude mimics like lung cysts, emphysema, bullae, and cystic bronchiectasis.
- 3. Causes: 1. Cancer: 2. Autoimmune: 3. Vascular: 4. Infection: 5. Trauma: 6. Youth:
- 4. The most common cause of a single lung cavity is lung cancer. Usually, the cavity forms because the cancer grows more rapidly then its blood supply, resulting in necrosis in the central part of the cancer. Primary bronchogenic carcinoma, especially Squamous cell carcinoma (scc) of the lung is more likely to develop cavitations than lung adenocarcinoma or large cell lung carcinoma. Other primary cancers of the lung, such as lymphoma and Kaposi’s sarcoma can also cavitate, especially in immunocompromised people.
- 5. Of all bronchial carcinomas, 10–15 % are cavitary. Cavitation is secondary to tumoural necrosis. Radiographic features: Neoplasms are typically of variable size, round with irregular thick walls of solitary mass (greater than 4 mm) on CT scan, with higher specificity for neoplasm in those with a wall thickness greater than 15 mm. Center mass outside line is spiked due to lymphangitis & Inner wall line is smooth.
- 6. I. Granulomatosis with polyangiitis (GPA): Previously known as Wegener granulomatosis, is a multisystem necrotising non-caseating granulomatous c-ANCA positive vasculitis affecting small to medium sized arteries, capillaries, and veins. Plain radiograph: Chest radiographs may show multiple nodules or masses that can be extremely variable in size (from a few millimetres to many centimetres) Although cavitation is present in ~ 50% of cases, is seen less frequently on plain film Airspace opacities may represent consolidation or pulmonary haemorrhage
- 7. II. Rheumatoid pulmonary nodule: Rheumatoid pulmonary nodules are a rare pulmonary manifestation of rheumatoid arthritis. They are thought to occur in <1% of patients with rheumatoid arthritis. Radiographic features: i. Plain Radiograph: Not very sensitive (may only be detected a very small proportion of cases on plain film). ii. CT- On HRCT or CT of the chest: Nodules can be quite variable in appearance: associated cavitation may be seen May be single or multiple Size ranges from 0.5-7 cm Rarely these nodules can have associated calcification Tend to be peripheral, subpleural or pleural
- 8. Pulmonary infarction: Pulmonary embolism (a blood clot in the lung) causes pulmonary infarction (the death of lung tissue) and only about 5% of pulmonary infarctions result in lung cavities occurs in the minority (10-15%) of patients with Pulmonary embolism. Radiographic features: wedge-shaped (less often rounded) juxtapleural opacification (Hampton hump) without air bronchograms more often in the lower lobes
- 9. Several groups of microorganisms may cause cavitary lesions in the lungs: ◦ Common bacteria are Streptococcus p., Staph. aureus, Klebsiella p., H. influenzae. ◦ Typical and atypical mycobacterium. ◦ Fungi: Aspergillosis.
- 10. Pulmonary abscess occurs as a complication of pneumonia. The most common appearance of a lung abscess is an asymmetric cavity with an air-fluid level and a wall with a ragged or smooth border. They may occur anywhere in the lungs. Usually, intermediate to thick wall thickness with a peripheral contrast enhancement and necrotizing centre is visible. If the abscess is located peripherally, there may be local pleural thickening or an empyema.
- 12. The cavities in tuberculosis, which occur in 50 percent of patients, are usually located in upper zones of the lobes. They are often surrounded by satellite nodules. The cavity wall thickness may vary considerably, and the cavity wall may show rim enhancement on CT. If there is affection of the lymph nodes, one may see nodal rim enhancement around central necrosis.
- 15. The radiological division of primary and secondary features has been debunked. However, a radiological pattern does exist; upper lobe cavitary disease is commonly seen in immunocompetent adults, while lower lung zone disease, and pleural effusions are commonly found in immunocompromised patients. Miliary tuberculosis is hematogenous spread of disease, which presents as small, 2–3 mm sized nodules. They are usually located in the lower zones of the lobes and may cavitate.
- 17. Aspergillosis is caused by a fungus: Aspergillus fumigatus. Radiographic features: On imaging, one may find a solitary cavitating or multiple cavitating opacities or masses with a crescent-shaped air collection in the nondependent part of the cavity On CT, initially there is consolidation, which may have a halo of ground glass surrounding it. The nodules may cavitate. The wall of the preexisting cavity may be affected by the aspergilloma and become irregular, but wall thickness usually remains below 3 mm.
- 18. Pneumatocele: Are intrapulmonary gas-filled cystic spaces that can have a variety of sizes and appearances. They may contain gas-fluid levels. If they are imaged during formation, they may have surrounding consolidation and be difficult to distinguish from abscesses. Features that favour a pneumatocele over an abscess are: ◦ Smooth inner margins ◦ Little if any fluid content ◦ The wall, if visible, is thin and regular ◦ Tend to persist despite an absence of symptoms
- 19. Bronchogenic cysts: Bronchogenic cysts are congenital malformations of the bronchial tree. They can present as a mediastinal mass that may enlarge and cause local compression. It is also considered the commonest of foregut duplication cysts. Plain radiograph: The cysts usually appear as soft-tissue density rounded structures. sometimes with compression of surrounding structures. Occasionally such compression can lead to air-trapping and a hyperlucent hemithorax.
