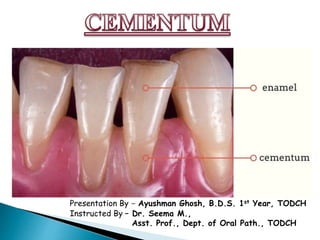
Understanding Cementum: Its Formation, Types and Functions
- 1. Presentation By - Ayushman Ghosh, B.D.S. 1st Year, TODCH Instructed By – Dr. Seema M., Asst. Prof., Dept. of Oral Path., TODCH
- 2. 1. What is Cementum? What is it consisted or made up of? 2. How is Cementum formed? 3. What are the types of Cementum? Why are they classified like that? 4. How are Cementum and Enamel connected to each other? 5. What is the function of Cementum? 6. How can we apply what we studied about Cementum in our clinics?
- 3. Cementum is the mineralized dental tissue covering the anatomic roots of human teeth. It was first demonstrated microscopically in 1835 by two pupils of Purkinje, Fränkel and Raschkow. Location/Extension/Situation: It begins at the cervical portion of tooth at CEJ and continues to the apex Anatomically: Part of Tooth Functionally: Part of Peridontium
- 4. • Hardness & Calcification < Dentin • Light yellow in colour, with dull surface, lacks luster, and is lighter than Dentin • Permeability of cementum is more than that of Dentin. However, the permeability decreases through age. Thickness • Thinnest at CEJ – 20-50µm • Thickest at apex – 150-200µm Cementum is thicker in the distal surface than the mesial surface probably because of the functional stimulation of the mesial drift. Average Thickness – 95µm at 20, 128µm at 60
- 5. On the basis of Dry weight, Cementum from fully formed permanent teeth contains: Inorganic substances – about 45% to 50% Organic material and water - 50% to 55% Inorganic portion consists • Mainly of calcium and phosphate in the form of hydroxyapatite. • Numerous trace elements are found in cementum in varying amounts. • It is of interest that cementum has the highest fluoride content of all the mineralized tissues. Organic portion consists • Primarily of type I collagen and protein polysaccharides (proteoglycans). The other types of collagen seen are types III, V, VI and XII. • Noncollagenous proteins play important roles in matrix deposition, initiation and control of mineralization and matrix remodeling. These include: Bone sialoprotein (BSP), osteopontin, Cementum derived attachment protein (CAP) • Proteoglycans: Chondroitin sulfate, heparan sulfate, hyaluronate, keratan sulfates–fibromodulin and lumican, versican, biglycan and osteoadherin • Growth Factors: TGFβ, various Bone Morphogenetic Proteins (BMPs), FGF, IGF, EGF and platelet derived growth factor (PDGF) • Cementum derived growth factor(CDGF) is seen exclusively in cementum. These are insulin like molecules and help in resorption of cementum and enhance proliferation of gingival fibroblasts and peridontontal ligament cells
- 7. Cementogenesis is the process of cementum formation which covers the tooth root by cementoblasts of mesenchymal origin. DEFINITION: Stages of Cementogenesis: Cementogenesis is subdivided into two stages: A) Prefunctional Stage: It can be divided into two stages: (i) Matrix Formation (ii) Mineralization B) Functional Stage What are the cells involved in Cementogenesis? There are mainly three types of cells involved in cementogenesis: (i) Cementoblasts (ii) Cementocytes (iii) Fibroblasts
- 8. CEMENTOBLASTS: 1. Cementoblasts are large cuboidal cells that forms from the follicular cells around the root of a tooth 2. These are found on the surface of both cellular and accellular cementum 3. Cementoblasts synthesize collagen and protein polysaccharides, which make up the organic matrix of cementum 4. These cells have numerous mitochondria, a well-formed Golgi apparatus, and large amounts of granular endoplasmic reticulum 5. At the superficial surface, the collagen fibrils produced by the cementoblast form a fibrous fringe perpendicular to periodontal space. These cells retreat and intermingle with the fibroblasts of the periodontal ligament. The processes which extend from cementoblasts to deposit cementum are known as cementoblastic processes.
- 9. Phenotype of Cementoblasts Cementoblasts are identified by 3H thymidine labeling. Apart from the inner cells of the dental follicle, cementoblasts are also reported to differentiate from HERS. The cementoblasts that are derived from the dental follicle have a similar morphology and phenotype to osteoblasts and are shown to be involved in the formation of CIFC. The cementoblasts, which are reported to be derived from HERS, have a similar morphology to fibroblasts and a different phenotype than osteoblasts and are shown to be involved in the formation of AIFC. These two types of cementoblast precursors differ in the expression of surface receptors and their reaction to signaling molecules or differentiating factors
- 12. CEMENTOCYTES: Cementocytes are spider-like cells that are incorporated into cellular cementum. The cell body is located in spaces called lacunae and their processes are present in canaliculi. A typical cementocyte has numerous cell processes or canaliculi, radiating from its cell body. These processses may branch and anastomose with those of neighbouring cells. Most of the processes are directed towards the periodontal surface of cementum. Cytoplasm of cementocytes in deeper layer of cementum contains few organelles. Endoplasmic reticulum appears dilated and mitochondria are sparse. These characteristics indicate that cementocytes are either degenerating or marginally active cells. In deeper layer cementocytes show signs of degeneration such as cytoplasmic clumping and vesiculation. In more deeper layer of cementum lacunae appear empty and suggesting complete degeneration of cementocytes
- 15. Stages of Cementogenesis Cementogenesis is subdivided into two stages: A)Prefunctional Stage: It can be divided into two stages: (i) Matrix Formation (ii) Mineralization B) Functional Stage
- 17. A) Matrix formation Once the root dentin(radicular dentin) formation has been initiated the Hertwig’s root sheath fragments into a network which allows the ectomesenchymal cells of dental follicle to pass through and contact the root dentin. The direct contact of the follicular cells of dental follicle with the newly formed dentin results in the differentiation of undifferentiated mesenchymal cells to cementoblasts.
- 18. A) Matrix formation These newly formed cementoblasts extend numerous tiny cytoplasmic processes into the loosely arranged unmineralized dentinal matrix Cementoblasts lay down cementum matrix(cementoid) leading to an intimate integration of the two different fibril populations forming dentinocemental junction. Though its not distinctive as the fibres of dentin and cementum intermingle at the interface
- 19. A) Matrix formation During matrix formation, fibroblasts form collagen fibers(Sharpey’s fibers), which become embedded in the matrix to provide attachment of the root to the surrounding bone. Discrete bundles of collagen fibers which are seen in tangential section, these bundles are known as Sharpey’s Fibers. Sharpey’s fibers make up the substantial portion of cementum When cementum remains relatively thin these sharpey’s fibers crosses the entire thickness of cementum. With further apposition of cementum the larger part of fiber is incorporated in cementum Cemental surfaces with actively mineralizing fronts have numerous small openings that correspond to site where individual Sharpey’s fibers enter the tooth The openings represent unmineralized core of fibers
- 21. The first layer of cementum that is formed by inner cells of the Hertwig’s epithelial root sheath and is deposited on the the root’s surface is known as hyaline layer of Hopewell-Smith. It is the most peripheral layer of initially unmineralized dentin that forms immediately subjacent to the cementodentinal junction (CDJ). It eventually mineralizes, but not before the rest of the dentin is already mineralized. It is 0.5-0.8 µm thick and contains enamel matrix-like protein as well as the proteins one would expect to find in dentin. It is into this hyaline layer that the initial fibers of the periodontal ligament embed themselves. It aids the cementum to bind with dentin. The role of this layer is to seal the CDJ before HERS degenerates.
- 22. A. Accellular Cementum B. Hyaline layer of Hopewell Smith C. Granular layer of Tomes D. Dentin
- 23. B) Mineralization It begins in the depth of the cementum matrix (cementoid tissue), where, fine hydroxyapetite crystals are deposited between and within the collagen fibrils Mineralization of the outermost layer of dentin matrix (mantle dentin), appears to be delayed until the implantation of the cementum matrix is established and the dentinal matrix is completely covered with the collagen fibrils of cementum
- 24. 1. These are incremental lines of cementum which represent the rest periods in cementum formation and are more mineralized than the adjacent cementum. 2. Both cellular and acellular are arranged in lamillae separated by incremental lines 3. These lines are parallel to the long axis of the root. 4. Theses can be best seen/observed in decalcified sections under light microscopy ACELLULAR CEMENTUM CELLULAR CEMENTUM
- 25. This stage of cementogenesis commences/begins when the tooth is about to reach occlusal level and continues throughout life It is associated with the attachment of root to the surrounding bone and continues throughout life. It is mainly during this stage that adaptive and reparative processes are carried out by the biological responsiveness of cementum Cementum deposition apically (near the apex) compensate attrition
- 26. Molecular Factors regulating Cementogenesis
- 29. Following are the types of Cementum: Based on CELLULARITY: Acellular Cementum: Cementum present without the cells (cementocytes) Cellular Cementum: Cementum consisting of cells (cementocytes). Based on TIME OF ORIGIN: Primary Cementum: First formed cementum. It is acellular. It consists of Peridontal ligament. Secondary Cementum: It forms after tooth reaches occlusal plane. Based on PRESENCE OF COLLAGEN FIBERS: Afibrillar Cementum: Cementum does not consist of fibers. Fibrillar Cementum: Cementum consisting of fibers. Based on ORIGIN OF CEMENTUM MATRIX FIBERS: Extrinsic Cementum: Cementum consisting of matrix fibers derived from peridontal ligament. Intrinsic Cementum: Cementum consisting of matrix fibers derived from cementoblasts. Mixed fiber Cementum: Cementum containing both extrinsic and intrinsic fibers.
- 30. Acellar Cementum Cellular Cementum 1. Located from cervical to apical third 1. Located from apical third and furcations 2. It is formed earlier and is known as primary cementum 2. Formed later and during repair and is known as secondery cementum 3. It consists of noncollagenousprotein-tenascin, fibronectin and osteocalcin are absent. 3. Noncollagenous proteins are present 4. Growth factors TGF β and IGF are not seen. 4. Growth factors are seen 5. Proteoglycans, i.e., versican, decorin, biglycan, and lumican were not identified in the matrix 5. These proteoglycans are seen in the matrix 6. Cementoid is usually absent 6. Cementoid is seen on the surface 7. It contains only extrinsic fibers of the periodontal ligament formed by fibroblast 7. Contains only intrinsic fibers produced by cementoblasts 8. Probably the only type of cementum in single rooted teeth 8. May be absent in single rooted teeth 9. Its main function is anchorage 9. Main function is adaptation and repair 10. It is formed slowly 10. It is formed rapidly 11. Incremental lines are closer to each other 11. Incremental lines therefore further apart 12. Cementocytes are not seen 12. Cementocytes, viable to varying degrees and depths seen 13. Cementoblasts are suggestive to be derived from HERS 13. Cementoblasts are suggested to be derived from inner cells of dental follicle 14. Cementocytes do not express parathormone receptors 14. Cementocytes express parathormone receptors Differences between Acellular and Cellular Cementum
- 31. SCHROEDER & PAGE CLASSIFICATION In 1986, scientists Schroeder and Page classified Cementum on into the following types considering the location, morphology and histology of the cementum: 1. Acellular Afibrillar Cementum (AAC) 2. Acellular Extrinsic Fiber Cementum (AEFC) 3. Cellular Intrinsic Fiber Cementum (CIFC) 4. Cellular Mixed Stratified Cementum (CMSC) 5. Acellular Intrinsic Fiber Cementum (AIFC)
- 32. ACELLULAR AFIBRILLAR CEMENTUM(AAC) 1. It consists of mineralized matrix 2. AAC contains neither cells nor extrinsic or intrinsic collagen fibers 3. This cementum does not have any function in tooth attachment. 4. Less homogenous 5. According to Schroeder(1986)- Cementum tissue cells are responsible for AAC formation when they come in contact with enamel surface. 6. It is a product of cementoblasts 7. It is found in coronal cementum
- 33. ACELLULAR EXTRINSIC FIBER CEMENTUM(AEFC) 1. It is composed of densely packed bundles of Sharpey’s Fibers (extrinsic fibers) & lack cells 2. AEFC is found in cervical 3rd of root – may extend apically . 3. Thickness between 30-230µm 4. AEFC is the only type of cementum seen in single rooted teeth. 5. It is a product of fibroblasts. 6. Cementoid is not found. 7. Main function is anchorage especially in single rooted teeth
- 34. ACELLULAR INTRINSIC FIBER CEMENTUM(AIFC) 1. AIFC is generally seen in close apposition to CIFC. 2. It (along with CIFC) helps in adaptive function of cementum, in maintenance of tooth position in the apical area of the tooth. 3. AIFC is formed when CIFC formation slows down in areas away from the advancing root edge. AIFC
- 35. ACELLULAR MIXED FIBER CEMENTUM(AMFC) AMFC is formed in some areas which integrates both extrinsic and intrinsic fibers in cementum. At present not much is known about its specific location or function.
- 36. CELLULAR INTRINSIC FIBER CEMENTUM(CIFC) 1. This cementum contains cells but has no extrinsic fibers. The fibers present are intrinsic fibers which are secreted by the cementoblasts. 2. CIFC fills resorption lacunae. 3. Majority of fibers organized parallel to the root surface. 4. Cells have phenotype of bone forming cells. 5. Very minor role in attachment (virtually absent in incisors and canine teeth). 6. Corresponds to cellular cementum and is seen in middle to apical third and interradicular cementum.
- 37. CELLULAR MIXED FIBER CEMENTUM(CMFC) 1. The CMFC is a variant formed at a faster rate with less mineralized fibers. 2. The fibers of CMFC are derived from the PDL fibroblasts and cementoblasts. 3. The intrinsic and extrinsic fibers form an intricate pattern running between each other at almost right angles and different orientations, though the number of intrinsic fibers is comparatively less than the extrinsic fibers. 4. The fiber bundles originating from fibroblasts are ovoid or round with 5- 7mm diameter and the fibers originating from the cementoblasts are much more delicate and smaller aroound 1-2mm in diameter.
- 38. CELLULAR MIXED STRATIFIED CEMENTUM(CMSFC) 1. In this type CIFC alternates with AEFC. 2. It contains cells and composed of both intrinsic and extrinsic(Sharpey’s) fibers. 3. It is a co-product of cementoblasts and fibroblasts. 4. It appears primarily on apical third of the root, in the apices furcation areas. 5. The thickness varies from 100 to 1000mm. 6. With light microscope this tissue is easily identified because: a) It includes cementocytes within lacunae with processes in canaliculi directed towards the PDL b) Its laminated structure c) The presence of cementoid on its surface.
- 39. d : Dentine c : Cementum Tgl : Tomes’ granular layer IF : Intrinsic fibers EF : Extrinsic fibers Cy : Cementocyte AEFC : Acellular Extrinsic Fiber Cementum CIFC : Cellular Intrinsic Fiber Cementum
- 41. DEFINITION: Cementoenamel junction represents the anatomic limit between the crown and root surface and is defined as the area of union of the cementum and enamel at the cervical region of the tooth. CEJ is of great importance in clinics. It helps to deal with various Peridontal anomalies and Conservative Dentistry. So, in order to make it easier, clinically we deal with two parts of CEJ: 1) Facial CEJ 2) Interproximal CEJ Clinical parts of CEJ:
- 42. Let Us Observe CEJ in a Radiograph:-
- 44. TYPES OF CEMENTUM: CEJ can be classified on the basis of the nature of connections between enamel and cementum. There are mainly 3 types of cementum: 1) Butt Junction(End-to-end approximating junction) 2) Overlapping Junction 3) Gap Junction
- 45. *In around 1.6% of cases enamel overlaps Cementum
- 46. 1) Butt Junction In approximately 30% of all teeth cementum meets the cervical end of enamel in a relatively sharp line. This type cemento-enamel junction where the enamel and the cementum forms an end-to-end junction is known as Butt Junction.
- 47. 2) Overlapping Junction Overlapping junction can be of two types: a) Cementum overlapping enamel / Cemento-enamel overlapping junction b) Enamel overlapping cementum / Enamelo-cementum overlapping junction
- 48. a) Cementum overlapping enamel / Cemento-enamel overlapping junction In approximately 60% of teeth, the cementum overlaps the cervical end of enamel for short distance. This occurs when the enamel epithelium degenarates at its cervical termination permitting connective tissue to come in direct contact with enamel surface which produce a laminated, electron dense, reticular material termed as afibrillar cementum
- 49. b) Enamel overlapping cementum junction Recent observations by researchers by optical microscopy showed fourth type of junction known as enamel overlapping cementum junction. In this type, CEJ enamel overlaps cementum. However, this type of CEJ is very rare. It is found only in 1.6% of cases.
- 50. 3) Gap Junction In about 10% of teeth, the cementum and the enamel do not meet. In such cases there is no cemento-enamel junction. This occurs when enamel epithelium in cervical portion of roots delayed in the separation from dentin. In this dentin is an external part of the surface of the root.
- 52. DEFINITION: The terminal apical area of cementum where it joins the internal root dentin is called cementodentinal junction or CDJ. The width of CDJ is 2 to 3µm and remains relatively stable. CLINICAL IMPORTANCE: The nature of CDJ is of particular importance, being of interest biologically because it forms an interface (a fit) between two very different mineralized tissues. It is also of clinical importance because of the processes involved in maintaining tooth function while repairing a diseased root. AF: Apical Foramen AA: Apical Apex
- 53. DIFFERENCES OF CDJ IN PERMANENT & PRIMARY DENTITION: