Mycobacterium tuerculae
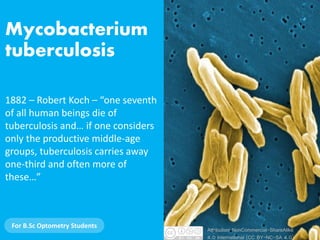
- 1. Mycobacterium tuberculosis For B.Sc Optometry Students 1882 – Robert Koch – “one seventh of all human beings die of tuberculosis and… if one considers only the productive middle-age groups, tuberculosis carries away one-third and often more of these…” Attribution-NonCommercial-ShareAlike 4.0 International (CC BY-NC-SA 4.0)
- 2. • In tissue, tubercle bacilli are thin straight rods measuring about 0.4 x 3 micro meter • On artificial media, coccoid and filamentous forms are seen with variable morphology from one species to another. • Mycobacteria cannot be classified as either gram-positive or gram- negative.
- 3. • Once stained by basic dyes they cannot be decolorized by alcohol, regardless of treatment with iodine. • True tubercle bacilli are characterized by "acid-fastness"—ie, 95% ethyl alcohol containing 3% hydrochloric acid (acid-alcohol) quickly decolorizes all bacteria except the mycobacteria. • Acid-fastness depends on the integrity of the waxy envelope. • The Ziehl-Neelsen technique of staining is employed for identification of acid-fast bacteria. • In smears of sputum or sections of tissue, mycobacteria can be demonstrated by yellow-orange fluorescence after staining with fluorochrome stains (eg, auramine, rhodamine).
- 4. • obligate aerobes • Increased CO2 tension enhances growth • growth rate is much slower than that of most bacteria. • The doubling time of tubercle bacilli is about 18 hours
- 5. • Mycobacteria are recovered in the sputum of tuberculosis patients and can be identified using a fluorescent acid-fast stain. • In the lungs, tuberculosis is identified by the tubercle, a massive granuloma of white blood cells, bacteria, fibroblasts, and epithelioid cells. • The center of the tubercle contains caseous (cheesy) pus and bacteria.
- 9. Symptoms Although your body may harbor the bacteria that cause tuberculosis, your immune system usually can prevent you from becoming sick. For this reason, doctors make a distinction between: Latent TB. In this condition, you have a TB infection, but the bacteria remain in your body in an inactive state and cause no symptoms. Latent TB, also called inactive TB or TB infection, isn't contagious. It can turn into active TB, so treatment is important for the person with latent TB and to help control the spread of TB. An estimated 2 billion people have latent TB. Active TB. This condition makes you sick and can spread to others. It can occur in the first few weeks after infection with the TB bacteria, or it might occur years later.
- 10. Symptoms Signs and symptoms of active TB include: • Coughing that lasts three or more weeks • Coughing up blood • Chest pain, or pain with breathing or coughing • Unintentional weight loss • Fatigue • Fever • Night sweats • Chills • Loss of appetite Tuberculosis can also affect other parts of your body, including your kidneys, spine or brain. When TB occurs outside your lungs, signs and symptoms vary according to the organs involved. For example, tuberculosis of the spine may give you back pain, and tuberculosis in your kidneys might cause blood in your urine.
- 11. Tuberculin test Old tuberculin: a concentrated filtrate of broth in which tubercle bacilli have grown for 6 weeks purified protein derivative (PPD): obtained by chemical fractionation of old tuberculin A positive tuberculin test • individual has been infected in the past. It does not imply that active disease or immunity to disease is present. • at risk of developing disease from reactivation of the primary infection, A negative tuberculin test • persons who have never been infected are not subject to that risk, In an individual who has not had contact with mycobacteria, there is no reaction to PPD. An individual who has had a primary infection with tubercle bacilli develops induration, edema, erythema in 24–48 hours, and, with very intense reactions, even central necrosis. The skin test should be read in 48 or 72 hours. Positive tests tend to persist for several days. Weak reactions may disappear more rapidly
- 12. Diagnosis Imaging tests • a chest X-ray or a CT scan. • This may show white spots in your lungs where • it may reveal changes in your lungs caused by active tuberculosis. • CT scans provide more-detailed images than do X-rays. Sputum tests • samples of your sputum • The samples are tested for TB bacteria. • Sputum samples can also be used to test for drug-resistant strains of TB • can take four to eight weeks to be completed.
- 13. Diaagnosis Blood tests • Blood tests may be used to confirm or rule out latent or active tuberculosis. • measure your immune system's reaction to TB bacteria. • QuantiFERON-TB Gold in-Tube test and T-Spot. TB test are two examples of TB blood tests. • A blood test may be useful if you're at high risk of TB infection but have a negative response to the skin test, or if you've recently received the BCG vaccine.
- 14. Treatment • The two major drugs used to treat tuberculosis are isoniazid and rifampin. • The other first-line drugs are pyrazinamide, ethambutol, and streptomycin. • Second-line drugs include kanamycin, capreomycin, ethionamide, cycloserine, ofloxacin, and ciprofloxacin.
- 15. DOTS Directly observed treatment, short-course (DOTS/ TB-DOTS) is the name given to the tuberculosis (TB) control strategy recommended by the World Health Organization DOTS have five main components: 1. Government commitment 2. Case detection by sputum smear microscopy 3. Standardized treatment regimen directly of six to nine months observed by a healthcare worker or community health worker for at least the first two months 4. A drug supply 5. A standardized recording and reporting system that allows assessment of treatment results
