Diabetic retinopathy for GENERAL OPHTHALMOLOGIST
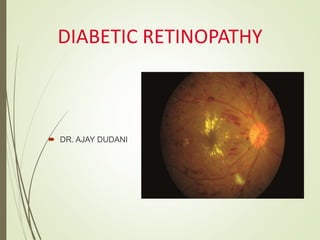
- 1. DIABETIC RETINOPATHY DR. AJAY DUDANI
- 2. Diabetic Retinopathy Damage to the blood vessels in the retina due to diabetes. https://www.contouravisionindia.com/single-post/What-causes-diabetic-retinopathy as visited on 13th Jan 2020 Biyani RS, Patre BM. Algorithms for red lesion detection in Diabetic Retinopathy: A review. Biomedicine &
- 3. Projections of DR :How big is the problem going to be ? https://www.nei.nih.gov/learn-about-eye-health/resources-for-health-educators/eye-health-data-and- Between 2010 and 2050, It is expected that the number of people with the most common eye diseases to double, and it will rise from 7.7 Mn to 14.6 Mn
- 4. Global Burden of Diabetic Retinopathy (DR) 35 studies = 22,896 patients 21 Among those with diabetes: • 34.6% with any DR • 6.95% with proliferative DR • 6.81% with diabetic macular edema • 10.2% with vision-threatening DR Among those with diabetes, increased risk of diabetic retinopathy: • Longer duration of diabetes • Poorer glycemic control • Poorer blood pressure control • Poorer control of blood cholesterol levels https://www.nei.nih.gov/learn-about-eye-health/resources-for-health-educators/eye-health-data-and- DR 35% PDR 7% DME 7% Vision Threatnein g DR 10%
- 5. PROTECTIVE FACTORS • High myopia • Choroidal degeneration • Extensive old chorio-retinopathy
- 6. Diabetic Eye Disease Key Points k best • Treatme before v nts exist but wo ision is lost RECOMMENDED EYE EXAMINATION SCHEDULE Diabetes type Recommended time of first examination Recommended follow-up* Type 1 3-5 years after diagnosis Yearly Type 2 At time of diagnosis Yearly Prior to pregnancy (type 1 or type 2) Prior to conception and early in the first trimester No retinopathy to mild- moderate NPDR - every 3-12 months rSevere NPDR or worse - every 1-3 months *Abnormal findings may dictate more frequent follow-up examinations
- 7. • Microangiopathy due to hyperglycemia • Endothelial barrier decompensation leads to serum leakage and retinal edema • Later stages, VEGF produced by ischemic retina causes neovascularisation PATHOGENESIS
- 8. Diabetic Retinopathy Five pathologic processes: • Formation of micro aneurysms (outpouchings of the small vessels) • Excessive vascular permeability (leakage) • Vascular occlusions (closure of blood vessels) • Proliferation of new vessels (± hemorrhage) • Contraction of new blood vessels: Scarring, retinal detachment https://www.nei.nih.gov/learn-about-eye-health/resources-for-health-educators/eye-health-data-and-
- 9. NON-PROLIFERATIVE DIABETIC RETINOPATHY (NPDR) NO DR Review in 12 months VERY MILD Microaneurysms only Review most patients in 12 months MILD Any or all of: microaneurysms, retinal hemorrhages, exudates, cotton wool spots Review range 6-12 months, depending on severity of signs, stability, systemic factors, and patient’s personal circumstances MODERATE Severe retinal haemorrhages in 1-3 quadrants or mild IRMA Significant venous beading in no more than 1 quadrant Cotton wool spots Review in approximately 6 months (PDR in up to 26%, high-risk PDR in up to 8% within a year) SEVERE The 4-2-1 rule- Severe retinal haemorrhages in all 4 quadrants Significant venous beading in ≥2 quadrants Moderate IRMA in ≥1 quadrants Review in 4 months (PDR in up to 50%, high-risk PDR in up to 15% within a year) VERY SEVERE ≥2 of the criteria for severe Review in 2-3 months (High-risk PDR in up to 45% within a year) ABBREVIATED EARLY TREATMENT DIABETIC RETINOPATHY STUDY (ETDRS) CLASSIFICATION CATEGORY MANAGEMENT
- 10. CATEGORY MANAGEMENT PROLIFERATIVE DIABETIC RETINOPATHY (PDR) MILD-MODERATE New vessels on the disc (NVD) < 1/3 disc area New vessels elsewhere (NVE) < 1/2 disc area Treatment considered according to severity of signs, stability, systemic factors, and patient’s personal circumstances If not treated, review in up to 2 months HIGH-RISK NVD > 1/3 disc area Any NVD with vitreous or preretinal hemorrhage NVE >1/2 disc area with vitreous or preretinal hemorrhage Laser photocoagulation Intravitreal anti-VEGF agents Intravitreal triamcinolone Pars plana vitrectomy Lipid lowering drugs ADVANCED DIABETIC EYE DISEASE Preretinal (retrohyaloid) and/or intragel hemorrhage Tractional retinal detachment Tractional retinoschisis Rubeosis iridis (iris neovascularisation) Pars plana vitrectomy PDR – formation of new vessels or fibrovascular tissue on the optic disc or inner retina
- 11. OTHER CATEGORIES • BACKGROUND DIABETIC RETINOPATHY (BDR) It’s the earliest phase of DR. Characterised by microaneurysms, dot and blot hemorrhages and exudates. • DIABETIC MACULOPATHY Refers to presence of any retinopathy at the macula. • PRE-PROLIFERATIVE DIABETIC RETINOPATHY (PPDR) Cotton wool spots, venous changes, IRMA and deep retinal hemorrhages. • DIABETIC PAPILLOPATHY It is a form of optic neuropathy seen in young type I diabetics. It is unrelated to glycemic control or any other known feature of diabetes.
- 12. APPROXIMATE EQUIVALENCE OF THE CLASSIFICATION SYSTEMS ETDRS NSC SDRGS AAO RCOphth 10 - None R0 - None R0 - None No apparent retinopathy None 20 - Microaneurysms only R1 - Background R1 - BDR Mild NPDR Low risk 35 - Mild NPDR Moderate NPDR 43 - Moderate NPDR R2 - Pre- proliferative R2 Moderate BDR High risk 47 - Moderately severe NPDR 53 A-D - Severe NPDR R3 - Severe BDR Severe NPDR 53 E - Very severe NPDR 61 - Mild PDR 65 - Moderate PDR R3 - Proliferative R4 - PDR PDR PDR 71, 75 - High risk PDR 81, 85 - Advanced PDR
- 13. MILD NPDR
- 14. MODERATE NPDR
- 17. NEW VESSELS
- 18. DIABETIC MACULAR OEDEMA • Most common cause of visual impairment in diabetic retinopathy • According to the Wisconsin Epidemiologic Study of Diabetic Retinopathy (WESDR), the prevalence rate of macular oedema is 10 % in the diabetic population. • Best detected by slit-lamp biomicroscopy and stereoscopic fundus photography.
- 19. Retinal thickening within 500 µm of centre of macula Exudates within 500 µm of centre of macula, if associated with retinal thickening Retinal thickening one disc area (1500 µm) or larger, any part for which is within one disc diameter of centre of macula CLINICALLY SIGNIFICANT MACULAR EDEMA (CSME) As defined by ETDRS-
- 20. OCT A. Diffuse edema B. Cystoid macular edema C. Serous retinal detachment D. Posterior hyaloid traction
- 21. FLUORESCEIN ANGIOGRAPHY - Identifies macular capillary non-perfusion. - Identifies subtle areas of NV causing recurrent vitreous hemorrhage.
- 22. Diabetic Retinopathy National Institutes of Health-supported Clinical Trials https://www.nei.nih.gov/learn-about-eye-health/resources-for-health-educators/eye-health-data-and-
- 23. DIABETIC RETINOPATHY STUDY (DRS) ELIGIBILITY CRITERIA 1. Visual acuity ≥ 20/100 (6/36) in each eye 2. PDR in at least one eye or severe NPDR in both 3. Both eyes suitable for photocoagulation STUDY DESIGN One eye of each patient was assigned randomly to photocoagulation. The other eye was assigned to follow-up without photocoagulation CONCLUSIONS 1. Photocoagulation reduced the risk of severe visual loss by 50 % or more 2. Modest risks of decrease in visual acuity and visual field 3. Treatment benefit outweighs risks for eye with high-risk PDR
- 24. EARLY TREATMENT DIABETIC RETINOPATHY STUDY (ETDRS) ELIGIBILITY CRITERIA 1. Visual acuity ≥ 20/40 (6/12) {20/400 (60/120) if reduction caused by macular oedema} 2. Mild NPDR to non-high risk PDR, with or without macular oedema 3. Both eyes suitable for photocoagulation STUDY DESIGN 1. One eye of each patient was assigned randomly to early photocoagulation and the to deferral (careful follow-up and photocoagulation if high risk PDR develops). 2. Patients assigned randomly to aspirin or placebo.
- 25. CONCLUSIONS 1. Focal photocoagulation - reduced the risk of moderate visual loss by 50 % or more - increased the chance of a small improvement in visual acuity - reduced retinal thickening 2. Early scatter photocoagulation - small reduction in risk of severe vision loss - not indicated in mild to moderate retinopathy - most effective in type 2 diabetes mellitus 3. Aspirin did not alter the progression of diabetic retinopathy
- 26. DIABETIC RETINOPATHY VITRECTOMY STUDY (DRVS) ELIGIBILITY CRITERIA 1. Visual acuity ≤ 5/200 (5/60) 2. Vitreous hemorrhage consistent with visual acuity, duration 1-6 months 3. Macula attached STUDY DESIGN Eligible eye or eyes assigned randomly to early vitrectomy or conventional management (vitrectomy if center of macula detaches or if vitreous hemorrhage persists for 1 year, photocoagulation as needed and as possible) CONCLUSIONS Chances of recovery of VA ≥ 10/20 (3/6) increased by early vitrectomy, at least in patients with type I diabetes, who were younger and had more severe PDR
- 27. GROUP NR – Very Severe PDR with Useful Vision MAJOR ELIGIBILITY CRITERIA 1. Visual acuity ≥ 10/200 (3/60) 2. Center of macula attached 3. Extensive, active, neovascular, or fibrovascular proliferations MAJOR DESIGN FEATURES Same as Group H (except conventional management included vitrectomy after a 6 months waiting period in eyes that developed severe VH) MAJOR CONCLUSIONS Chances of of VA ≥ 10/20 (3/6) increased by early vitrectomy, at least for eyes with severe new vessels. Early vitrectomy for eyes with recent severe VH and VA < 5/200 (5/60) was beneficial, especially for patients with type I DM. Furthermore, the chances of achieving VA of 10/20 (3/6) or better increased when early vitrectomy was performed in eyes with severe new vessels, again especially for patients with type I DM.
- 28. Treatments for Diabetic Retinopathy Standard therapies: • Laser photocoagulation • Surgical intervention (vitrectomy) • Medical therapies delivered into the eye (intravitreal injections*) • Systemic medical therapies involving blood sugar, blood pressure, and cholesterol control * Note : Some drugs are used as an off label indication for the management of DR Berco E, Rappoport D, Pollack A, Kleinmann G, Greenwald Y. Management of Diabetic Retinopathy and Other Ocular Complications in Type 1
- 29. Background : Laser and supplemental therapy for management of DR Protocol S: This study showed that ranibizumab injections are effective in treating proliferative diabetic retinopathy. At two years, vision of the ranibizumab group on average improved by half a line on an eye chart. Vision of the laser group remained unchanged • Current treatment for PDR is pan-retinal photocoagulation (PRP) Inherently destructive Adverse effects on visual function • Some eyes with PDR+DME now receive anti-VEGF as standard care for DME • Would initial treatment of PDR with intravitreal anti-VEGF delay or prevent need for PRP?
- 30. STUDY OBJECTIVE AND TREATMENT GROUPS Prompt PRP To determine if visual acuity outcomes at 2 years in eyes with PDR (with or without concurrent DME) that receive anti-VEGF therapy with deferred PRP are non-inferior to those in eyes that receive prompt PRP therapy. 0.5mg ranibizuma b with deferred PRP (Note: Study ranibizumab may be given as needed for DME using Protocol I retreatment as guidelines.) Bressler NM, Beck RW, Ferris III FL. Panretinal photocoagulation for proliferative diabetic retinopathy. New England Journal of Medicine. 2011 Oct 20;365(16):1520-6.
- 31. Endpoints for measuring the outcome Primary End Point Is visual acuity using ranibizumab for PDR not worse than treatment with PRP at 2 years? Non-inferiority margin of 5 letters Secondary End Point Are there potential benefits of ranibizumab on: Vision throughout follow-up (area under the curve) Peripheral vision Macular edema Incidence of vitrectomy
- 32. Follow-up Schedule Baseline to 1 Year PRP group: Visits every 16 weeks* Ranibizumab group: Visits every 4 weeks to assess for PDR treatment Both groups simultaneously evaluated for DME treatment 1 Year to 2Years PRP group: Visits every 16 weeks* Ranibizumab group: Visits every 4wk to 16wk to assess for PDR treatment Interval is extended if injections for PDR and DME deferred (“Defer and Extend”) Bressler NM, Beck RW, Ferris III FL. Panretinal photocoagulation for proliferative diabetic retinopathy. New England Journal of Medicine. 2011 Oct 20;365(16):1520-6. *Eyes with DME could be seen more frequently for DME treatment as needed.
- 33. Ranibizu mab Group N = 191 N = 160 (84%) N = 88% N = 22 (18, 24) Randomization Participants: N = 304 Eyes: N = 394 PRP Group N = 203 N = 168 (83%) N = 86% 2- Years 2-Years Excludi ng Death Baseli ne N = 16 (9, 22) Median (Quartiles) No. Visits over 2 years Bressler NM, Beck RW, Ferris III FL. Panretinal photocoagulation for proliferative diabetic retinopathy. New England Journal of Medicine. 2011 Oct 20;365(16):1520-6.
- 34. Baseline Characteristics Ranibizu mab Group (N = 191) PRP Group (N = 203) Age (yrs) – Median 52 51 Women 43% 45% Race White 52% 50% Type 2 diabetes 73% 76% Duration of Diabetes (yrs) 18 17 Median HbA1c (%) 8.6 8.9
- 35. Ocular Baseline Characteristics Ranibizu mab Group (N = 189) PRP Group (N = 199) Diabetic Retinopathy Severity by Reading Center NPDR† 10% 13% Mild to moderate PDR 52% 49% High risk PDR to advanced PDR 38% 37% † There were 46 eyes (12%) for which NV was not identified by the reading center on the submitted color images or quality precluded identification. In 29 of these cases (63%), subsequent review of additional images (e.g. FA) confirmed NV, leaving 17 (4%) of 394 subjects with no photographic documentation of PDR.
- 36. Ocular Baseline Characteristics Ranibizum ab Group (N = 189) PRP Group (N = 201) Mean OCT CST* (µm) 262 249 < 250 µm 66% 67% 250 to 349 µm 19% 26% ≥ 350 µm 15% 7% Presence of central- involved DME with VA loss** 22% 23% *OCT values are Stratus equivalents **Eyes with visual acuity letter score ≤ 78 (20/32 or worse) AND OCT CST ≥ machine and gender Required ranibizumab at baseline
- 37. Treatment For Proliferative Diabetic Retinopathy
- 38. PRP Group Overall (N = 203) Completed initial full PRP 98% Performed in 1 Sitting 54% Baseline PRP Overall (N = 203) Eyes given additional PRP (after completing initial full PRP) 45% Distribution of timing to additional PRP From completion of initial full PRP: median time to additional PRP ~7 months Additional PRP
- 39. Ranibizumab Group # of Ranibizumab Injections Eyes With Baseline DME (N = 36) Eyes Without Baseline DME (N = 133) Prior to 1-year Visit (Max possible = 13) Median 9 7 Mean 8.9 6.9 Prior to 2-year visit (Max possible= 26) Median 14 10 Mean 13.3 10.1 Note: 97% of protocol-required injections for PDR were given Overall N = 191 Received PRP* before 2 years 12 (6%) Received PRP for PDR *1 met failure criteria, 1 with Protocol Chair approval, 1 without Chair approval, 8 during vitrectomy (e.g., via endolaser), and 1 by non-study physician
- 40. Mean Change in Visual Acuity Outlying values were truncated to 3 SD from the mean -5 0 5 10 15 0 16 32 52 68 84 104 Mean Visual Acuity Change (Letter Score) Visit Week Ranibizumab Group PRP Group N = N = 203 + 2.8 + 0.2 N = 168 N = 160 2-Year Adjusted Mean Difference: +2.2 letters 95% Confidence Interval: (-0.5, +5.0) (Meets pre-specified non-inferiority criterion: lower bounds of the 95% CI of -0.5 letters was greater than the non- inferiority limit of - 5.0 letters)
- 41. -4 1 6 11 0 16 32 52 68 84 104 Mean Visual Acuity Change (Letter Score) Visit Week With “Baseline DME” Ranibizumab Group PRP Group + +7. -5 0 5 10 0 16 32 52 68 84 104 Visit Week Without “Baseline DME” - 0.5 +1. 8 N = 42 N = 33N = 147 N = 46 N = 37N = 155 N = 130 N = 126 *Outlying values were truncated to 3 SD from the an Change in Visual Acuity Stratified by Baseline DMEMe
- 42. Discussion DRCR.net Protocol S (PRP vs. Ranibizumab for PDR): Treatment with 0.5-mg ranibizumab met primary non-inferiority outcome for VA being no worse than PRP Summary of Ranibizumab group results vs. PRP: Mean change in VA from baseline to 2-years with ranibizumab no worse than with PRP Superior mean visual acuity over course of 2-years (area under the curve analysis) Superior mean visual field outcomes Decreased occurrence of vitrectomies Decreased development of central involved DME PRP rarely given for failure or futility of ranibizumab
- 43. Discussion No systemic safety concerns with ranibizumab identified among pre-specified major safety outcomes Increased frequency of adverse events defined by cardiac, endocrine, respiratory, infections/infestations, skin and surgical conditions MedDRA systems in ranibizumab groups could be real, due to chance, or due to ascertainment bias (more visits in ranibizumab group) Interpretation of systemic safety difficult since large proportion of PRP group received ranibizumab per protocol for DME
- 44. SYSTEMIC MANAGEMENT • Glycemic control – Insulin, OHG • Blood pressure control – Anti-hypertensive medications • Cholesterol control – Statins, Fibrates • Support renal function – ACEI, ARB • Lifestyle modification – Smoking and alcohol cessation, exercise ,weight control
- 45. DIABETES CONTROL & COMPLICATION TRIAL (DCCT) STUDY GROUP Intensive management of blood glucose (multiple daily insulin injection) vs conventional management CONCLUSIONS intensive control reduced the risk of developing retinopathy by 76% and slowed progression of retinopathy by 54%. Intensive control reduced the risk of clinical neuropathy by 60% and albuminuria (Nephropathy) by 54%
- 46. UNITED KINGDOM PROSPECTIVE DIABETES STUDY (UKPDS) Patients were assigned to a conventional policy starting with diet or to an intensive policy starting with a sulfonyl urea or insulin. If overweight and in the intensive group, patients were assigned to start treatment with metformin Patients were randomly assigned to tight control of BP (ACE inhibitor or beta blocker) or to less tight control
- 47. RESULTS Intensive control of blood glucose level slowed progression of retinopathy and reduced other microvascular complications Intensive control of BP slowed progression of diabetic reinopathy and reduced other microvascular & macrovascular complications
- 48. PROMINENT-Eye Ancillary Study To assess whether treatment with pemafibrate (0.2 mg orally BID) compared with placebo reduces the hazard rate of diabetic retinopathy worsening in adults with type 2 diabetes and diabetic retinopathy without neovascularization in at least one eye who are participating in the parent PROMINENT trial. FIELD (Fenofibrate Intervetion and Event Lowering in Diabetes) and The Action to Control Cardiovascular Risk in Diabetes (ACCORD)-eye study, have demonstrated clinically important reduction in progression of retinopathy in patients with diabetes assigned to fibrate compared with placebo.
- 49. INDICATIONS OF TREATMENT NVD > 1/3 disc in area Less extensive NVD + hemorrhage NVE > 1/2 disc in area + hemorrhage
- 50. 1. ARGON LASER (514.5 nm) • All eyes with CSMO should be considered for laser photocoagulation irrespective of the level of visual acuity. • Reduces the risk of visual loss by 50%. • Two types- focal and grid i. Focal treatment - Burns are applied to microaneurysms and microvascular lesions in the centre of rings of exudates located 500-3000 µm from the centre of the macula.
- 51. ii. Grid treatment – Burns are applied to areas of diffuse retinal thickening more than 500 µm from the centre of the macula and 500 µm from the temporal margin of the optic disc. Spot size - 50-100 µm Exposure time – 0.1-0.5sec • 70% of eyes achieve stable visual acuity after laser photocoagulation • 15% show improvement • 15% subsequently deteriorate.
- 52. 2.QUENCY-DOUBLED Nd:YAG LASER (532 nm) MICROROPULSE DIODE LASER (780-850 nm) DYE LASER (570-630 nm)
- 53. LASER SETTINGS • SPOT SIZE depends on the contact lens used. With Goldmann lens spot size is set at 200-500 µm, but with a panfundoscopic-type lens it is set at 100-300 µm because of induced magnification. Other lenses used are – Volk, Mainster, Rodenstock • DURATION OF BURN - 0.05-0.1 sec • POWER - 250-570 mW, sufficient to produce only a light intensity burn causing stimulation of the retinal pigment epithelium. The end point is a whitening or darkening of the microaneurysms.
- 54. ASSESSMENT AFTER LASER PHOTOCOAGULATION GOOD INVOLUTION POOR INVOLUTION • Regression of neovascularization leaving ‘ghost’ vessels or fibrous tissue • Decrease in venous changes • Absorption of hemorrhages • Disc pallor • Persistent neovascularization • Hemorrhage
- 56. POST LASER
- 57. ANTI VEGF Blocks VEGF molecules, thereby decreases new vessel formation & reduces macular edema BEVACIZUMAB RANIBIZUMAB AFLIBERCEPT PEGAPTANIB
- 58. BEVACIZUMAB Recombinant humanized monoclonal antibody Inhibits VEGF A & blocks angiogenesis Approved for use in metastatic colon cancer, certain lung cancer, renal and ovarian cancers Not yet approved by FDA, off label use in ophthalmology Dose: 1.25 mg in 0.05 ml
- 59. RANIBIZUMAB Monoclonal antibody fragment , binds to VEGF A 0.5 mg in 0.05 ml costly
- 60. AFLIBERCEPT Recombinant fusion protein Binds to VEGF receptors 1 and 2
- 62. INDICATIONS OF PARS PLANA VITRECTOMY Severe persistent vitreous hemorrhage Dense, persistent premacular hemorrhage Progressive proliferation despite laser therapy Retinal detachment involving macula
- 63. BENEFITS OF PPV Vitrectomy prevents or delays: • Persistent intra-gel hemorrhage • Retinal detachment • Opaque membranes • Rubeosis iridis VISUAL RESULTS OF PPV • 70 % of cases achieve visual improvement • 10 % are made worse • 20 % remain unchanged POOR PROGNOSTIC FACTORS • Age > 40 years • Preoperative iris neovascularisation • Cataract • Visual acuity < 5/200 (5/60) • Retinal detachment • No previous photocoagulation
Editor's Notes
- JKS- presenter should note that additional visits may be scheduled as standard care for DME treatment. (or may want to put this on slide)