Compartment syndrome
- 2. DEFINITION • A condition in which increased pressure within a limited space compromises the circulation and function of the tissues within that space.
- 3. SITES FORE- ARM & CALF HAND,ARM, BUTTOCK, ABDOMEN
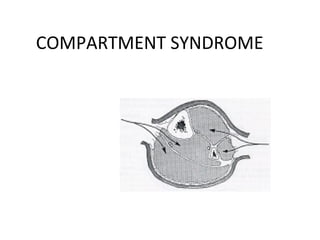
- 5. ANATOMY
- 6. Fracture Blick et al JBJS 1986
- 7. Blunt Trauma • 2nd most common cause McQueen et al; JBJS Br 2000
- 8. OTHER CAUSES…. • Temp vascular • Exertional states occlusion • GSW • Cast/dressing • IV/A-lines • Closure of fascial • Hemophiliac/coag defects • Intraosseous IV(infant) • Burns/electrical • Snake bite • Arterial injury
- 9. EFFECTS
- 10. MUSCLE NECROSIS AND NERVE DAMAGE • INFECTION, SEPTICEMIS,ABSCESS FORMATION • GANGRENE OF LIMB • CHRONIC ISCHEMIC CONTRACTURE • DISABLED LIMB • RENAL FAILURE
- 11. Compartment Syndrome Diagnosis • Pain out of proportion • Palpably tense compartment • Pain with passive stretch • Paresthesia/hypoesthesia • Paralysis • Pulselessness/pallor
- 12. Compartment Pressure • Infusion • Arterial line – manometer – 16 - 18 ga. Needle – saline (5-19 mm Hg higher) – 3-way stopcock – transducer (Whitesides, CORR 1975) – monitor • Catheter • Stryker device – wick – Side port needle – slit wick
- 13. Compartment Syndrome Pressure Measurements • Arterial line – Zero at the level of the affected limb
- 14. Compartment Syndrome Pressure Measurements • Simple Needle – 18 gauge – Least accurate – Usually gives falsely higher reading Side port • Slit Catheter and Side ported needle – No significant difference – More accurate Moed et al JBJS 1993
- 15. Surgical Treatment • Fasciotomy, Fasciotomy, Fasciotomy, – All compartments !!!
Editor's Notes
- Causes range from minor trauma to major injuries and interosseous infusion of IV fluids. Open fractures can have a 9% incidence of Compartment Syndrome-(Brumback et al). The incidence of CS in electrical injuries is proportional to the amount of voltage the patient was exposed to: minimal risk with low voltage (normal household current) and can be as high as 40% in higher voltage. Most burn literature uses the loss of pulses to decide when to perform escharotomies, however, tissue perfusion may still be compromised. Temporary vascular occlusion can occur in obtunded states(drug abuse), operative positioning (hemi and full lithotomy), and prolonged tourniquet use. If compartment syndrome is suspected, tissue pressures measurement is warranted and fasciotomies performed as indicated and supported in the literature.
- These physical findings have been described as the clinical hallmarks of CS. They are not very sensitive and if seen in the later stages it may be too late to change the underlying pathology. CS may be present with good pulses and no pallor and loss of pulses rarely occur unless arterial damage is present. Pain out of proportion and pain with passive stretch of a muscle in the compartment in question may be the most sensitive clinical finding before the onset of ischemic dysfunction of the nerves and muscles. These findings are useful only in a conscious cooperative patient and once paresthesia begin the pain may decrease. One important point to make is of CS is a possibility then regional anesthesia, continuous epidurals and PCA intravenous opiate analgesia should be avoided since they may mask the symptoms of compartment syndrome. Otherwise monitoring of the tissue pressure is warranted. There exist reports of missed compartment syndrome in tibia fracture and other surgical patients at risk managed postoperatively with these techniques and therefore they are generally avoided.
- Whitesides described the use of a 3-way stop cock connected to a mercury manometer(now against JCAH rules-biohazard) An arterial line using a large bore needle hooked up to a transducer and monitor in any ICU, OR or the recovery room will work. Remember that a standard needle will give higher results than a side port (Srtyker) or wick catheter. (Moed and Thorderson, JBJS(A), 1993) The stryker device is one of the more commonly used portable hand-held devices used for the tissue pressure measurements and since the redesign of the side port needle is very accurate. All devices must have the transducer at the level of the needle to be zeroed for an accurate reading.
- Whitesides et al have demonstrated that the pressure measurements should be done within 5 cm of the fracture (tibia) to obtain a true pressure reading within the suspected compartment.
