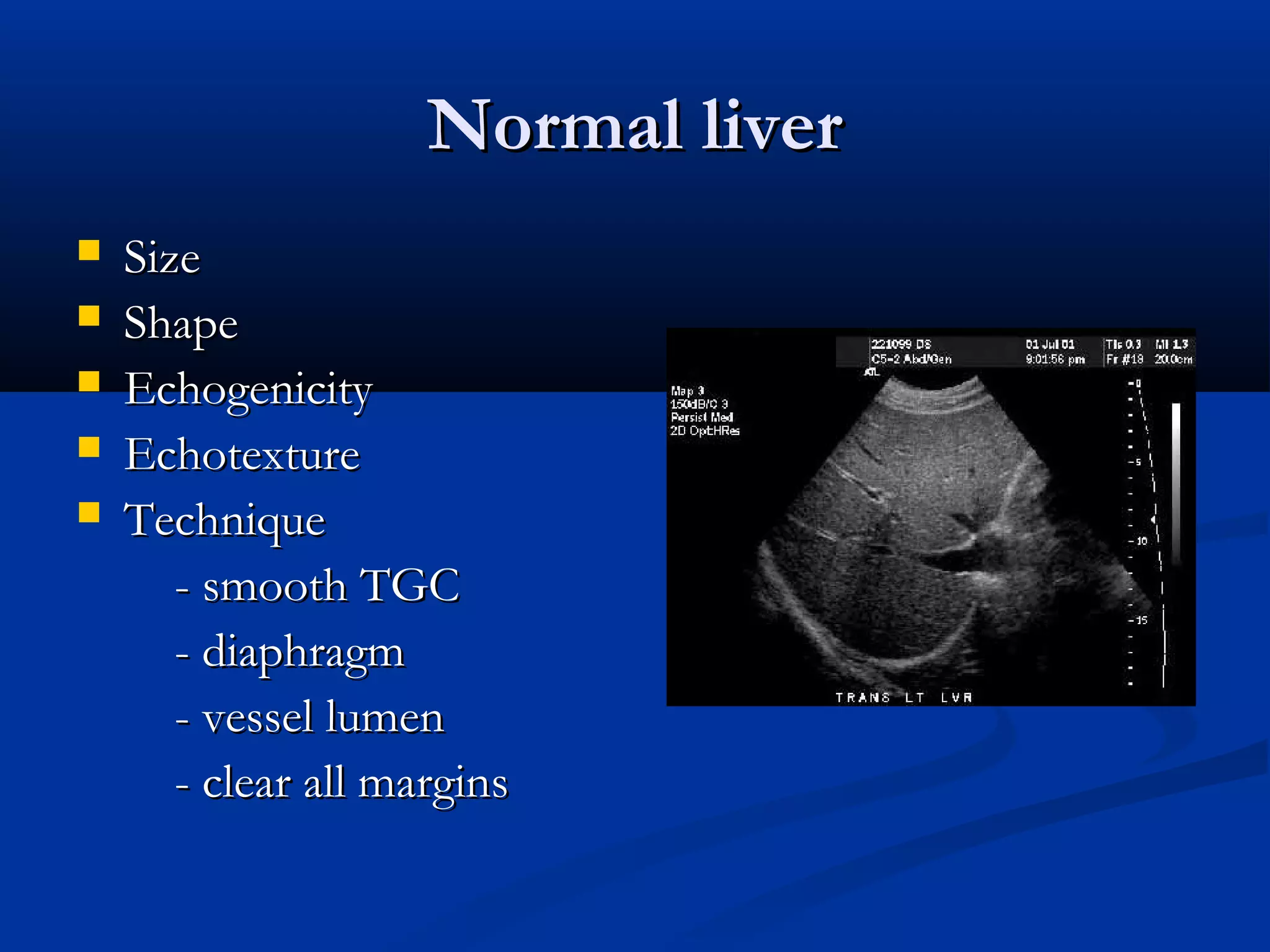
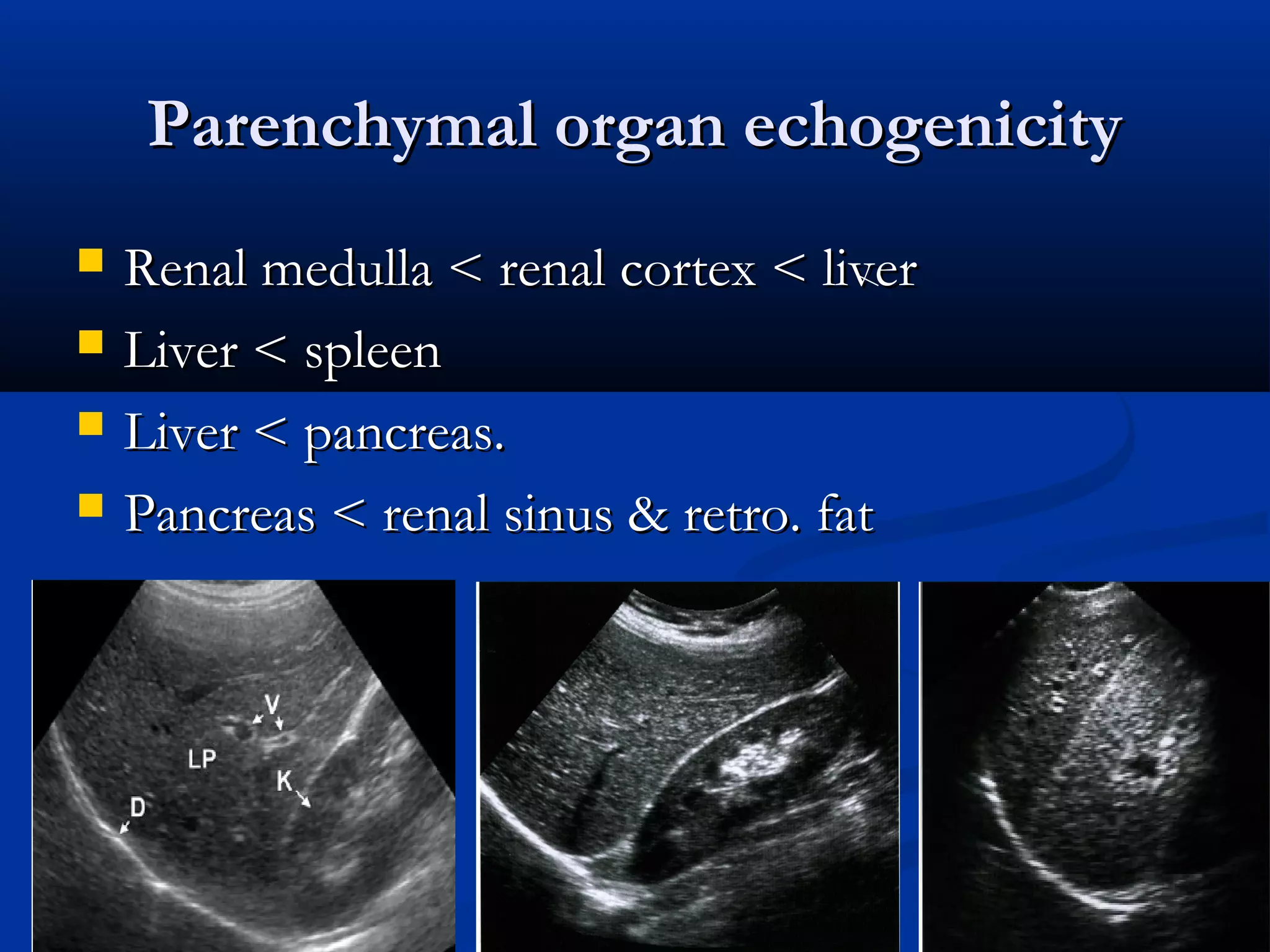
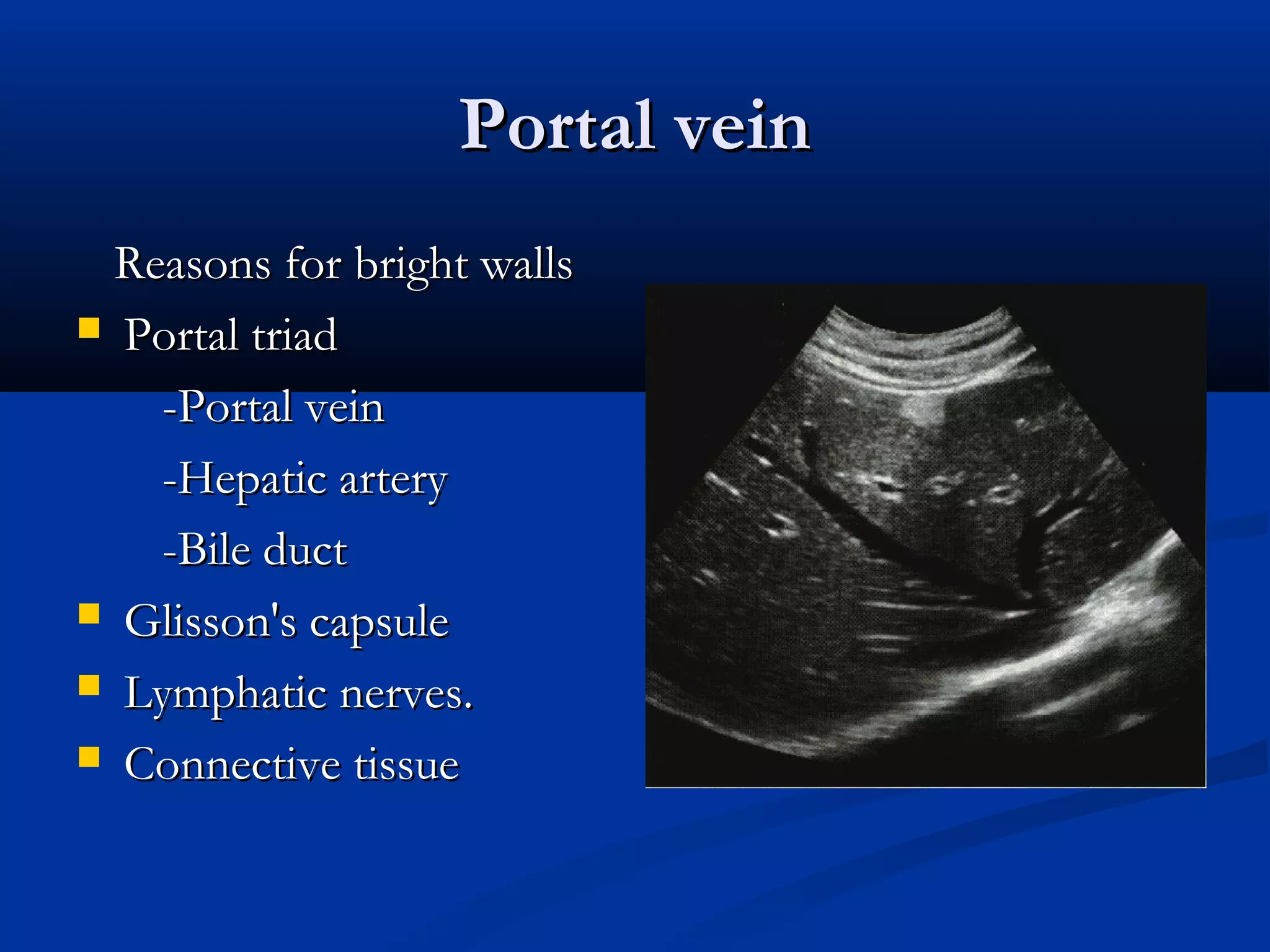
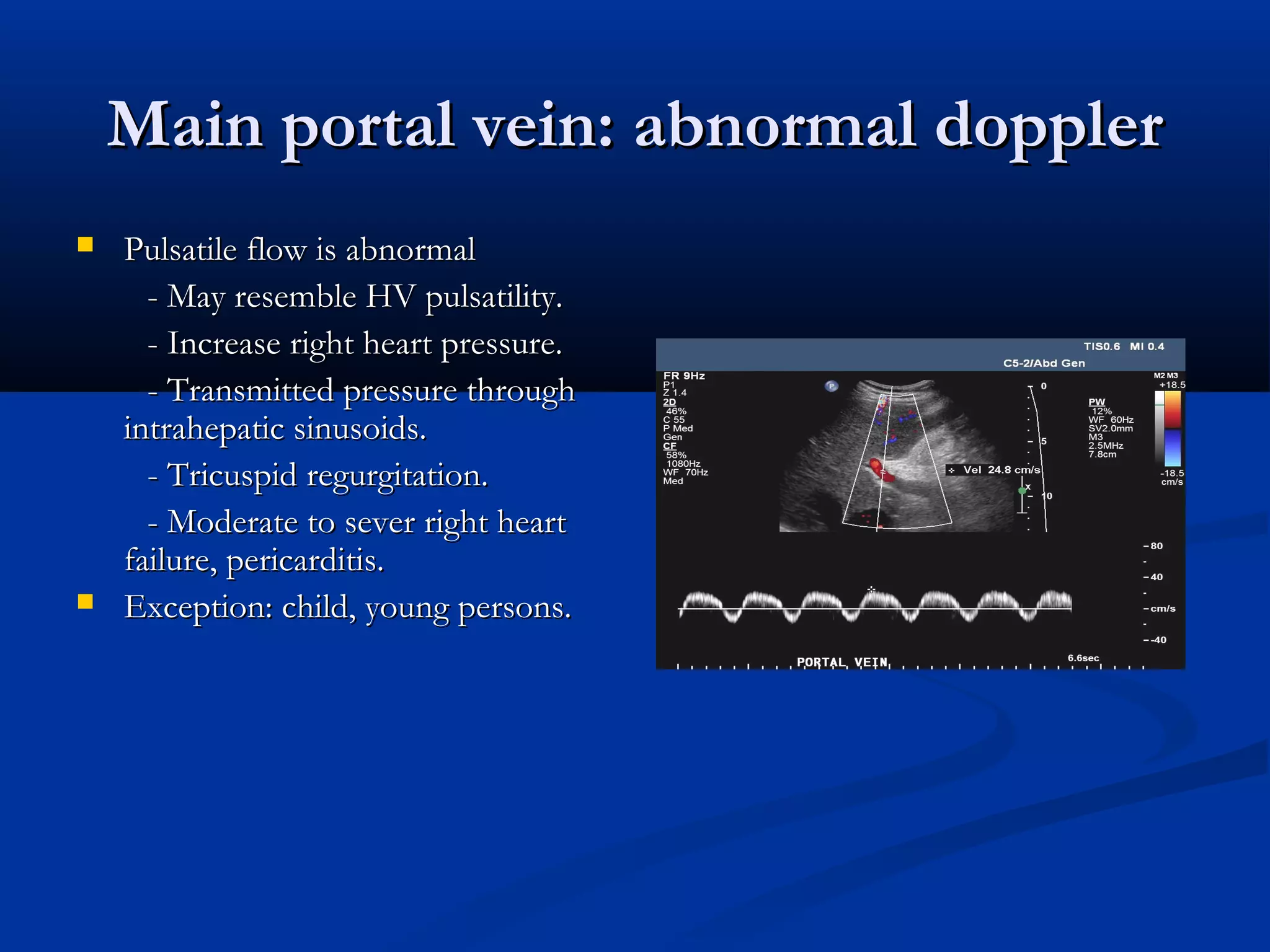
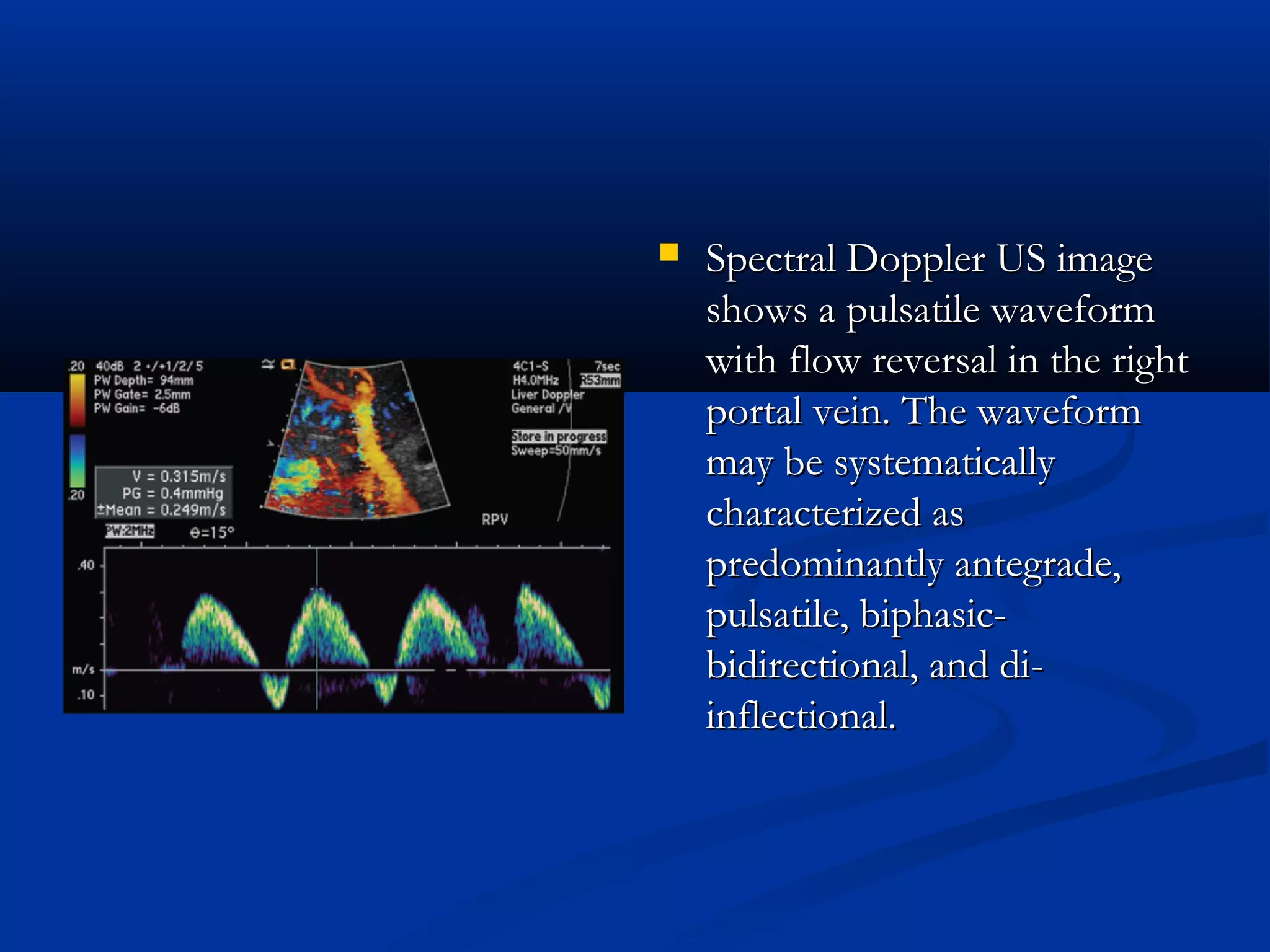
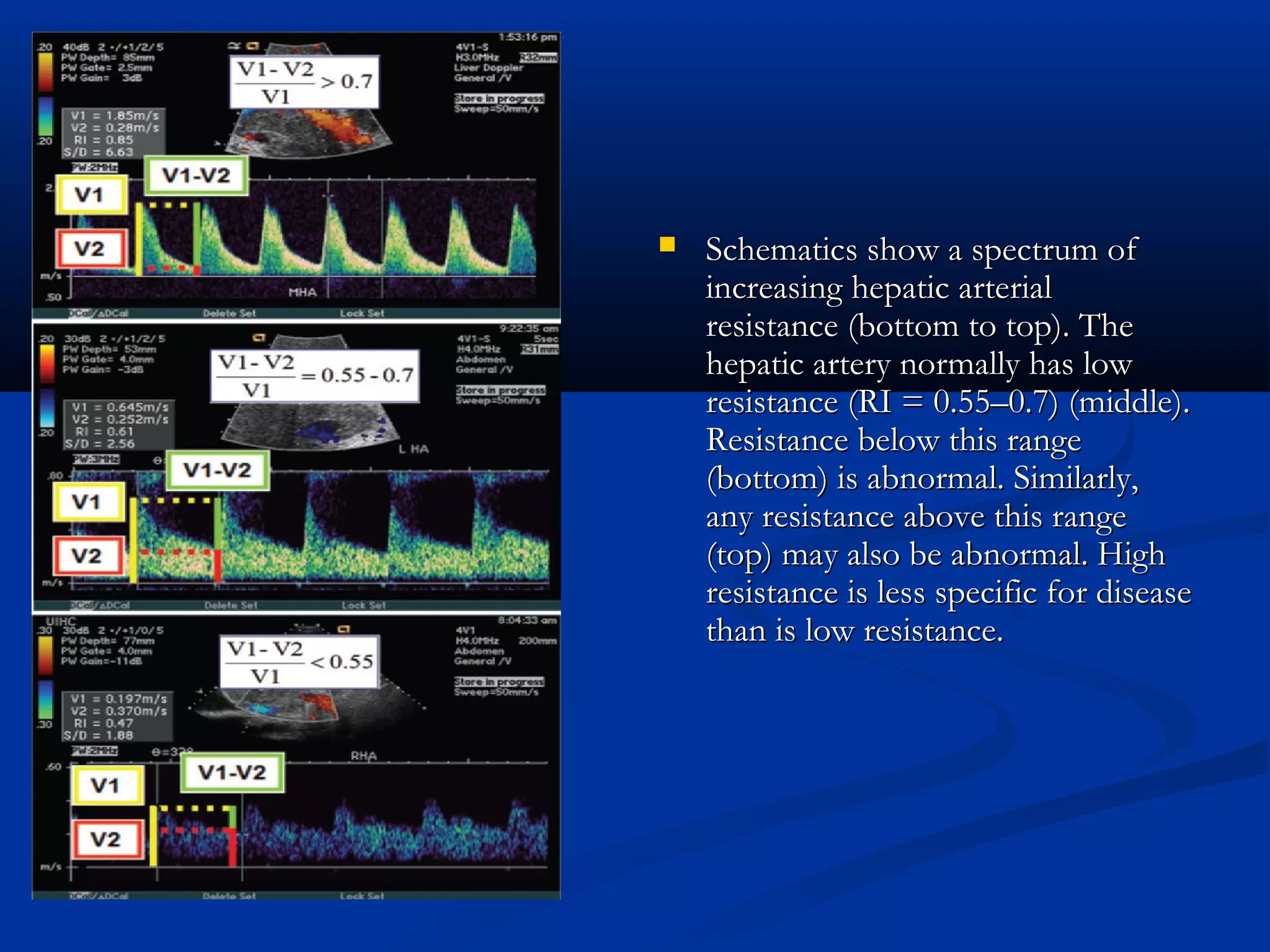
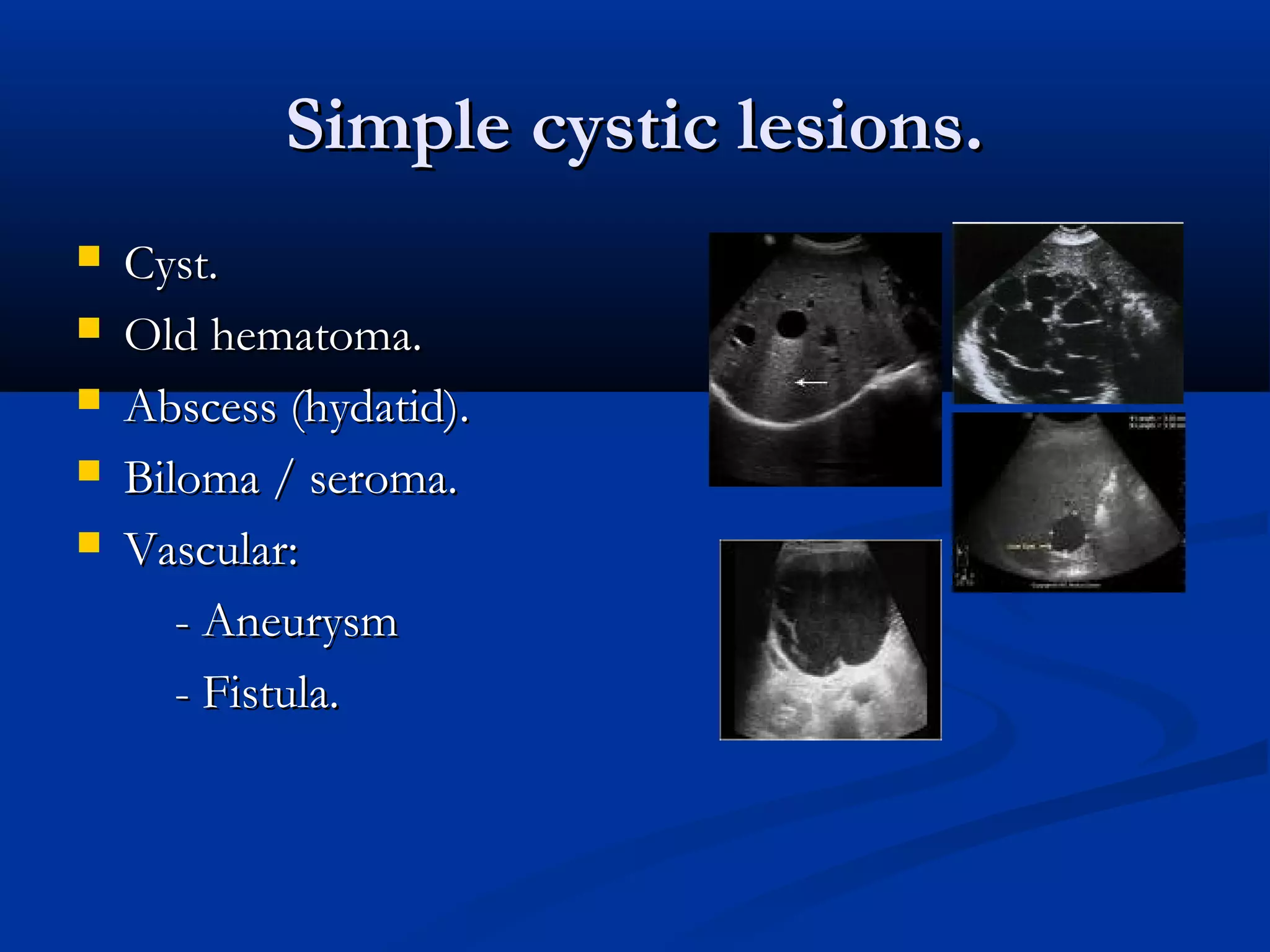
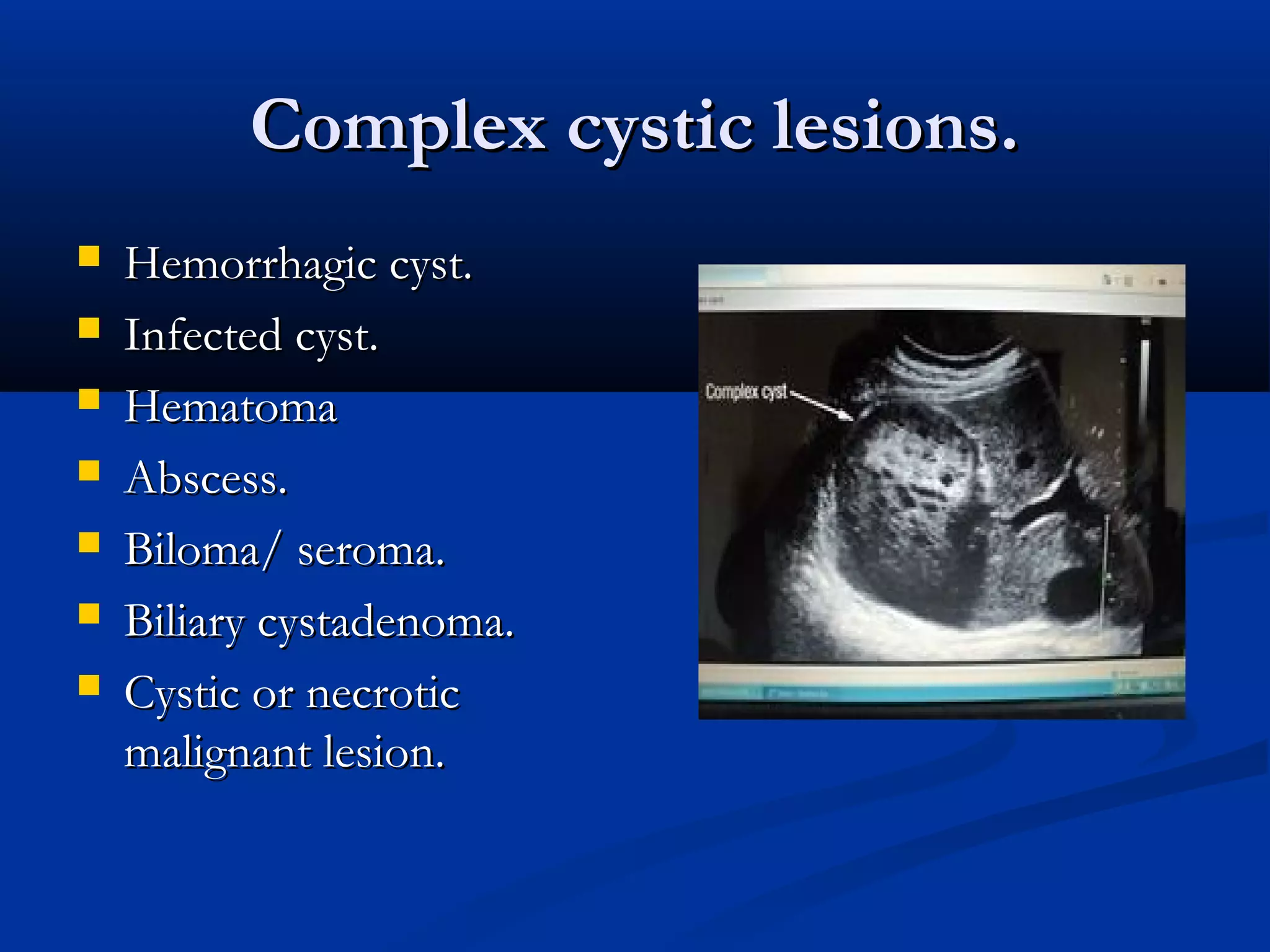
The document provides information on performing and interpreting an ultrasound of the liver. It discusses normal liver anatomy and Doppler assessments of the hepatic vessels. Key findings of a normal liver ultrasound include evaluating the size, shape, echogenicity and echotexture of the liver. Doppler ultrasound can assess blood flow in the hepatic arteries, portal veins and hepatic veins which branch throughout the liver and should demonstrate continuous flow in the expected directions. Spectral analysis of waveforms can help identify abnormalities associated with conditions like portal hypertension.