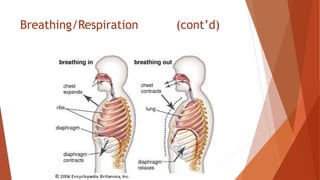
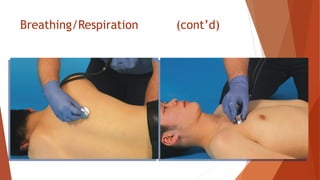
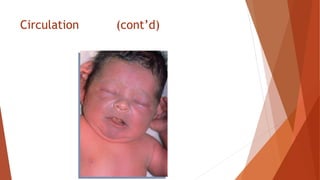
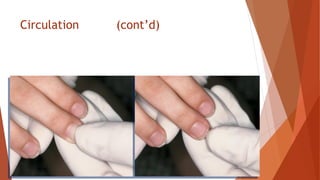
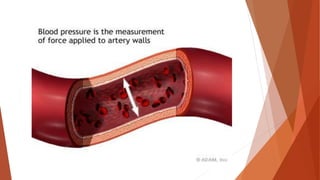
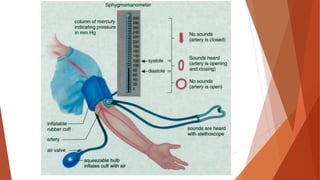
Vital signs provide important information about a patient's physiological status. They include level of consciousness, pupils, breathing, pulse, skin, blood pressure, and temperature. Assessing vital signs involves evaluating factors like respiratory rate and depth, pulse rate and quality, skin color and temperature, and blood pressure. Together, vital signs give medical responders insight into a patient's condition to determine the best treatment and need for transport.