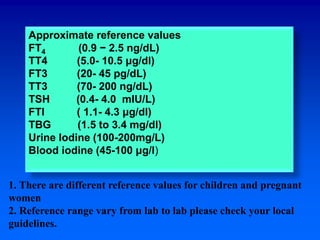
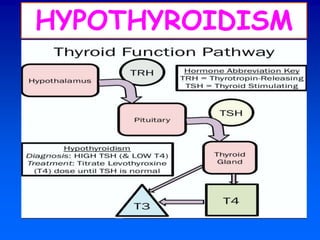
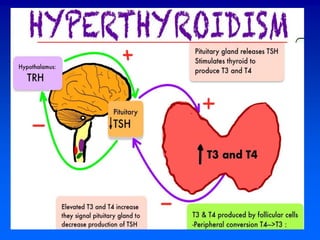
1. The serum TSH test is the best initial test for evaluating thyroid function, with a high TSH indicating hypothyroidism and a low TSH indicating hyperthyroidism.
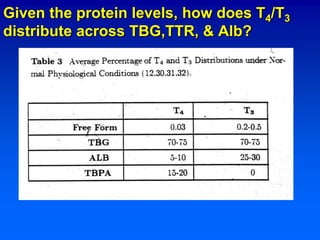
2. Additional tests like T4, T3, thyroid antibodies, and radioactive iodine uptake can help diagnose specific thyroid disorders like Hashimoto's thyroiditis or Graves' disease.
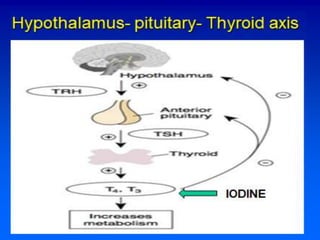
3. Examining TSH, T4, T3 levels together can differentiate between primary thyroid disorders and secondary disorders originating from the pituitary or hypothalamus.