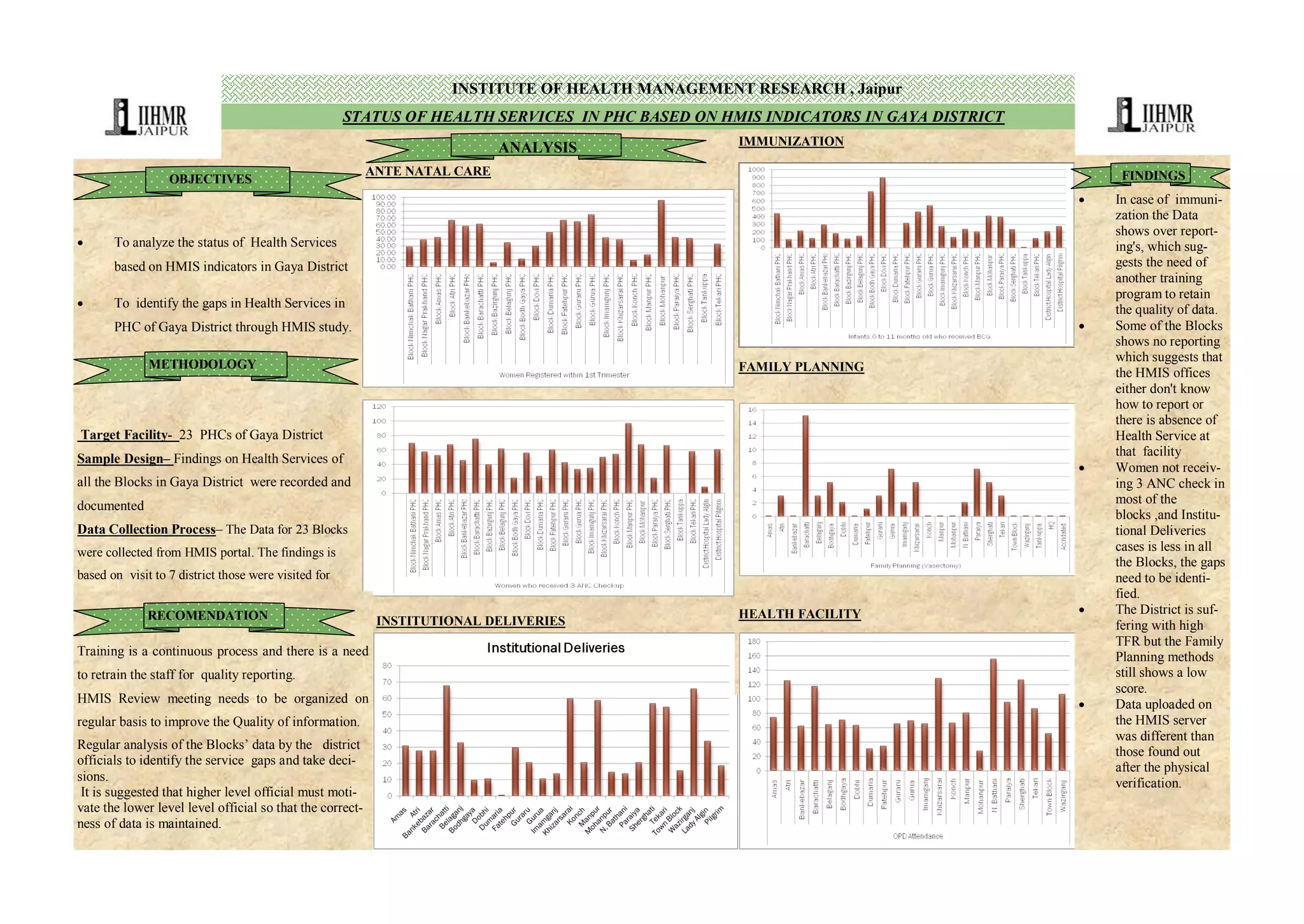
The document analyzes health services in Gaya District, India based on HMIS indicators. It collected data from 23 PHCs in the district's blocks to identify gaps in health services. Key findings include low rates of antenatal care, institutional deliveries, and family planning compared to the district's high birth rate. Some blocks showed no reporting or over-reporting of immunizations. Data uploaded to the HMIS system differed from physical verifications. Recommendations include retraining staff on quality reporting, regular HMIS review meetings, analyzing block data to identify gaps, and motivating officials to maintain correct data.