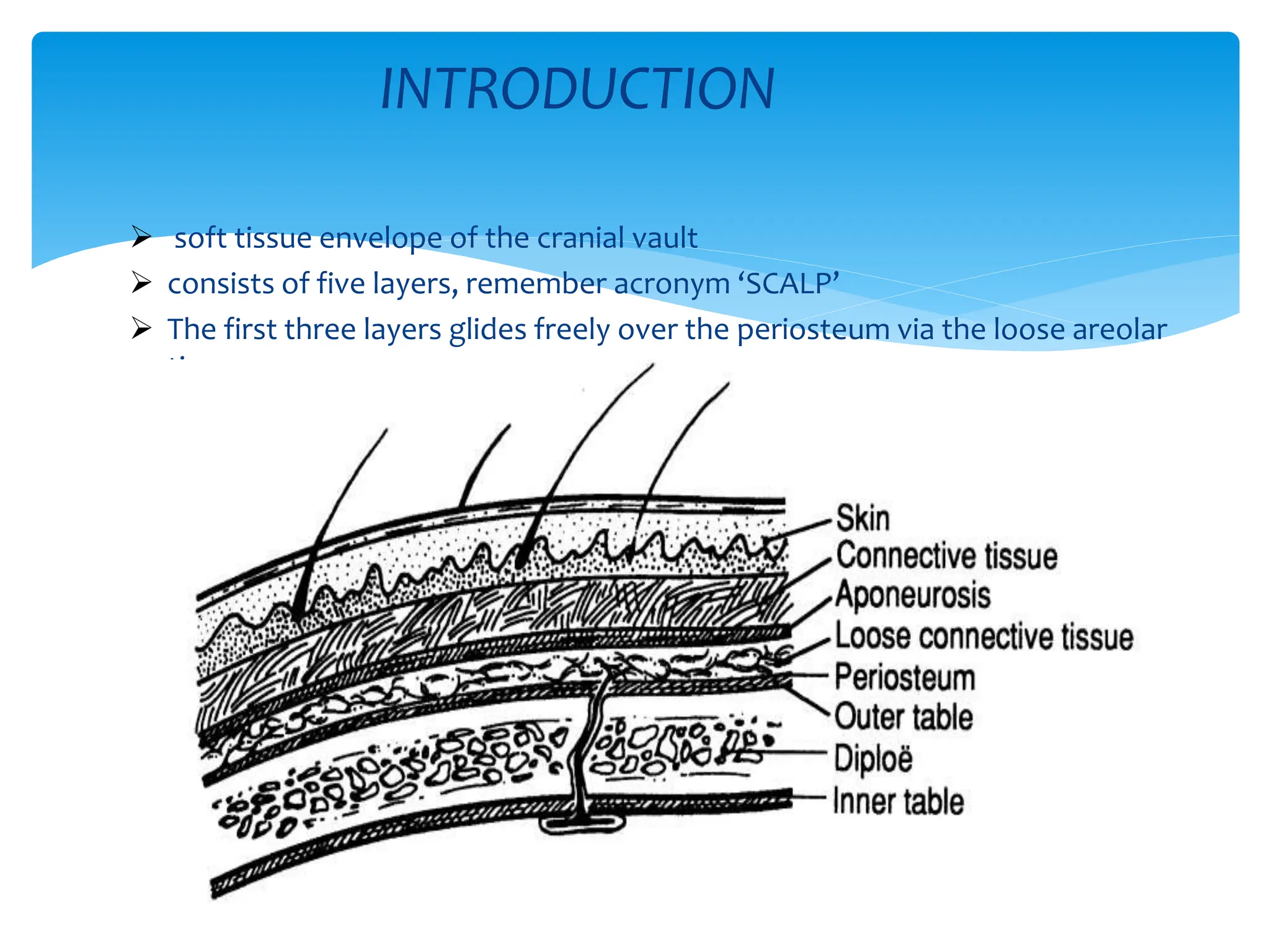
The scalp has five layers called SCALP:
- Skin
- Connective tissue which houses arteries, veins, nerves and lymphatics
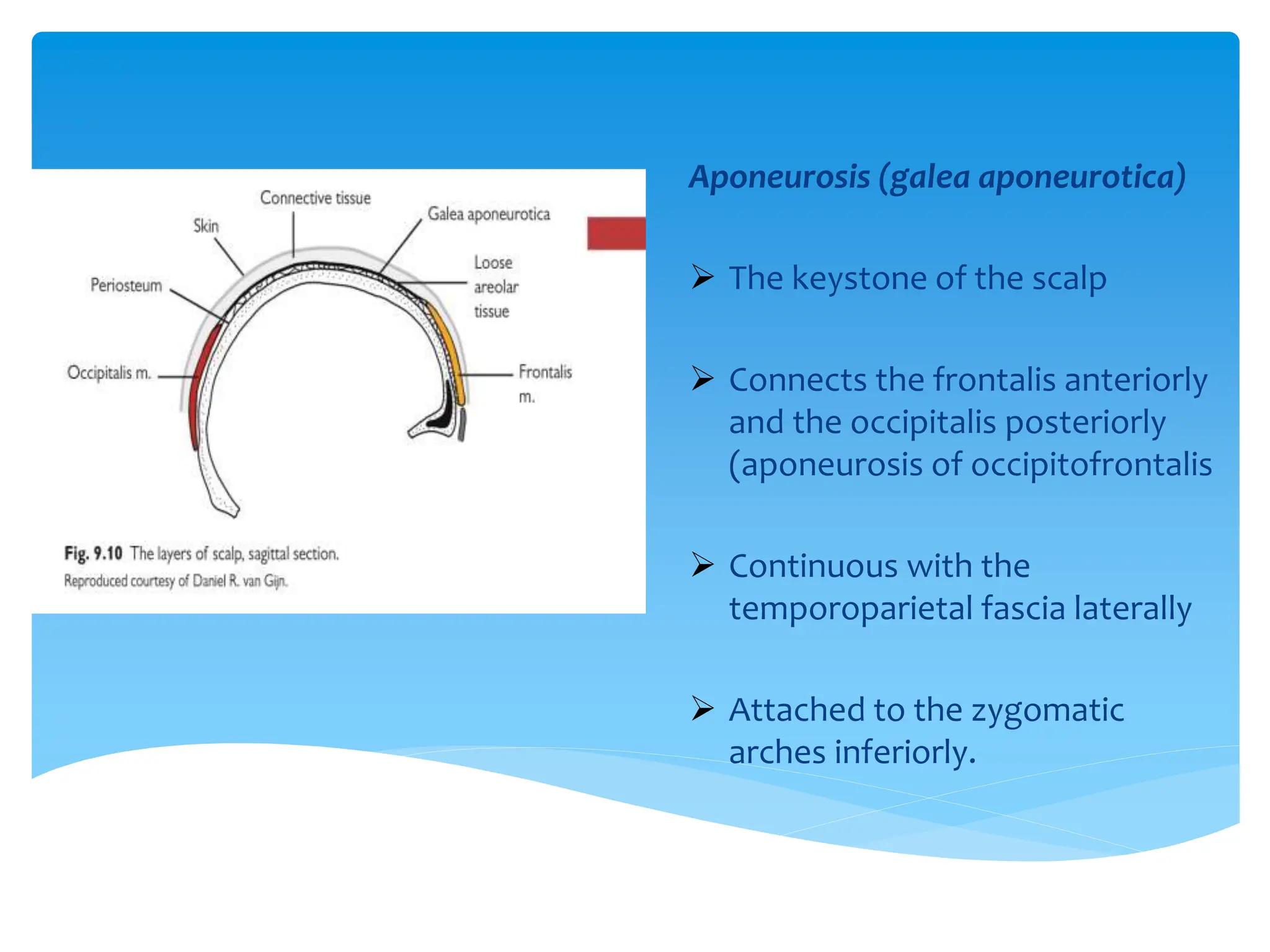
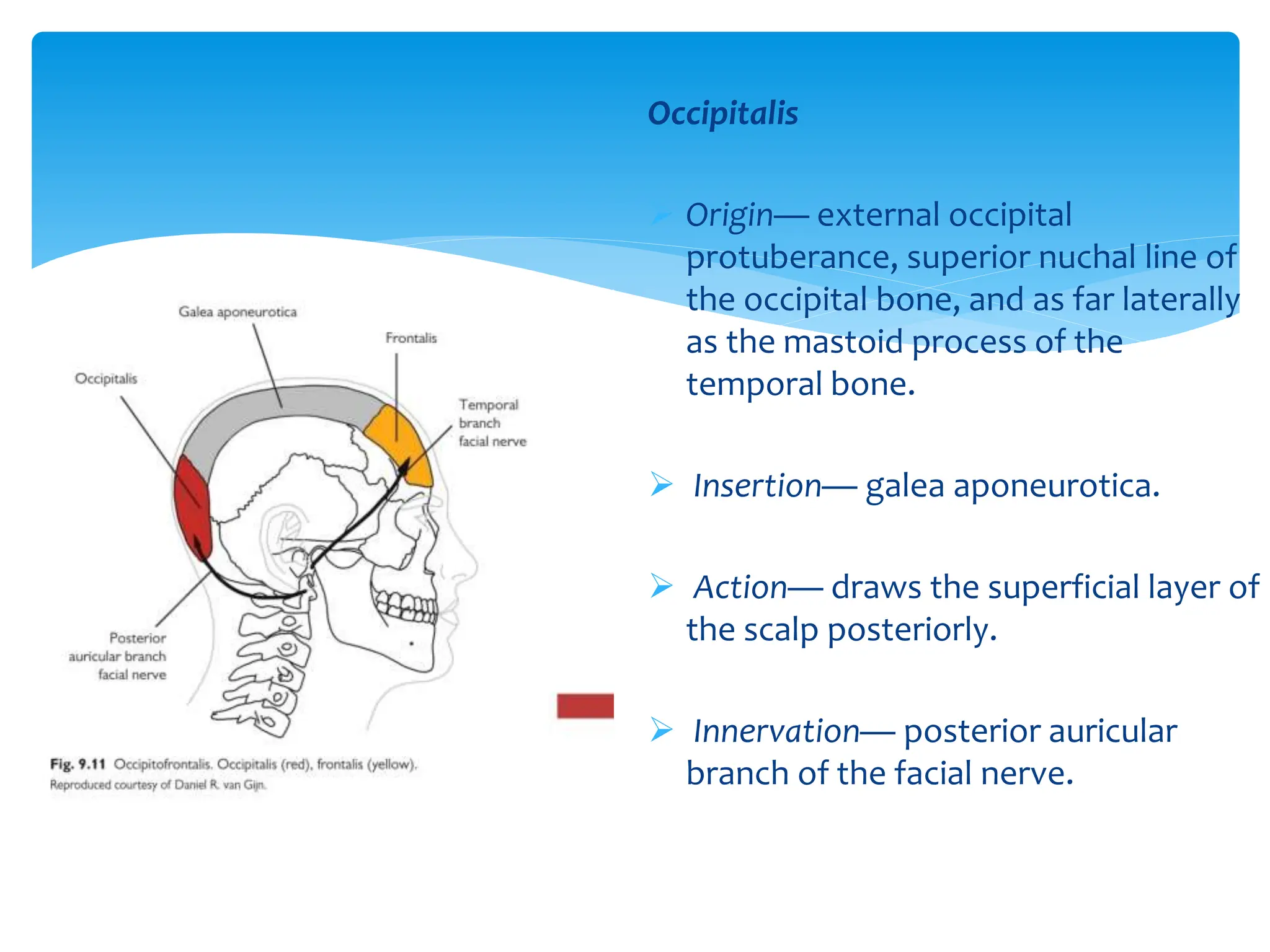
- Aponeurosis (galea aponeurotica) which connects the frontalis muscle anteriorly to the occipitalis muscle posteriorly
- Loose areolar tissue containing emissary veins connecting to intracranial venous sinuses
- Pericranium (periosteum) loosely attached to the skull