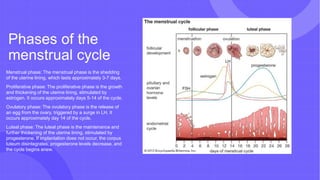
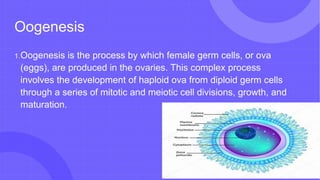
The document provides a detailed overview of the male and female reproductive systems, including external and internal structures, their functions, and the processes of spermatogenesis and oogenesis. It also outlines the menstrual cycle, pregnancy stages, labor, and delivery, highlighting the hormonal regulation involved in these reproductive processes. Key developments during pregnancy and the stages of childbirth are explained, emphasizing the physiological changes that occur in both the male and female systems.