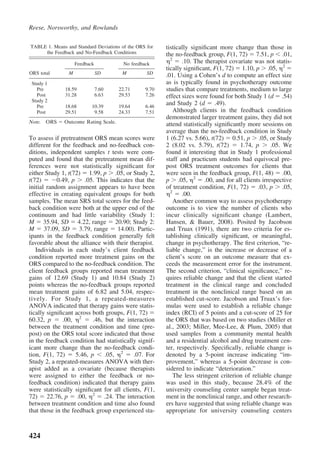
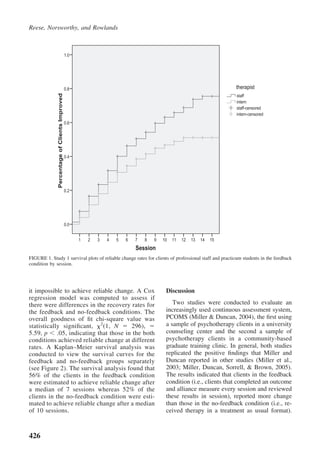
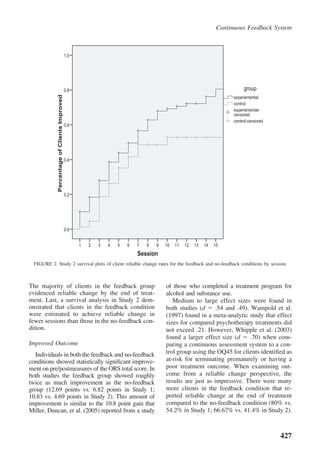
The document discusses research on whether using a continuous feedback system called the Partners for Change Outcome Management System (PCOMS) can improve psychotherapy outcomes. PCOMS involves clients completing brief measures after each session to assess treatment progress and the therapeutic relationship. Studies found that clients who used PCOMS with their therapists demonstrated statistically significant treatment gains compared to those receiving usual treatment and were more likely to experience reliable change in fewer sessions.