Radiographic Imaging of Mediastinal Masses
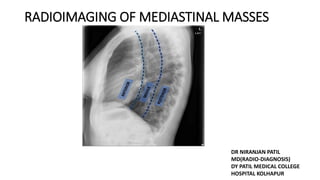
- 1. RADIOIMAGING OF MEDIASTINAL MASSES DR NIRANJAN PATIL MD(RADIO-DIAGNOSIS) DY PATIL MEDICAL COLLEGE HOSPITAL KOLHAPUR
- 3. ITMIG Definition of Mediastinal Compartments
- 9. HILUM OVERLAY SIGN • If cause of opacity arises from hilum the silhouette of normal pulmonary vessel is obliterated.causes of opacites include middle med tumours. • If edge of vessel are appreciated then cause of opacity is not in contact with hilum therefore it may be anterior or posterior to it.
- 16. POSTERIOR JUNCTION LINE • This Line is also form by apposition of visceral and parital pleura of posteromedial portion of lungs posterior to esophagus and anterior to third through fifth vertebrae. • posterior junction line demonstrates more cranial extension compare to anterior junction line,it can be seen above clavicles.
- 18. RIGHT PARATRACHEAL STRIPE • When the visceral and parietal pleura of the right upper lobe come in contact with the right lateral border of the trachea and the intervening mediastinal fat, air within the right lung and trachea outlines these entities to form the right paratracheal stripe • It begins superiorly at the level of the clavicles and extends inferiorly to the right tracheobronchial angle at the level of the azygos arch.
- 20. LEFT PARATRACHEAL STRIPE • It is formed by contact between the left upper lobe and either the mediastinal fat adjacent to the left tracheal wall or the left tracheal wall itself. Air within the trachea outlines the intervening soft tissue • the left paratracheal stripe is seen less frequently it may be obscured by contact between the left lung and either the proximal left common carotid artery anteriorly or the left subclavian artery posteriorly.
- 22. Left Paraspinal Line The left paraspinal line is formed by tangential contact of the left lung and pleura with the posterior mediastinal fat, left paraspinal muscles, and adjacent soft tissues. The left paraspinal line extends vertically from the aortic arch to the diaphragm and typically lies medial to the lateral wall of the descending thoracic aorta.
- 23. • The right paraspinal line is formed by the right lung and pleura coming in tangential contact with the posterior mediastinal soft tissues.The right paraspinal line is not a true mediastinal line. Right Paraspinal Line
- 24. Azygoesophageal Recess • The azygoesophageal recess represents a space lying lateral or posterior to the esophagus and anterior to the spine, extending from the level of the anterior turn of the azygos vein to the level of the aortic hiatus (T12) inferiorly.
- 25. Aortopulmonary Window • . It is bounded superiorly by the inferior wall of the aortic arch and inferiorly by the superior wall of the left pulmonary artery. The posterior wall of the ascending aorta forms the anterior boundary of the AP.
- 26. Lesions Fluid Fat Vascular Anterior Thymoma Lymphoma Germ-cell tumor Goiter Thymic cyst Thymoma Pericardial cyst Germ-cell tumor Lymphoma Duplication cyst Necrotic nodes Pericardial recess Germ-cell tumor Thymolipoma Fat pad Morgagni hernia Thyroid Cardiac coronary aneurysm Ascending aortic aneurysm Middle Lymph nodes Duplication cyst Arch anomaly Esophageal mass Duplication cyst Necrotic nodes Pericardial recess Lipoma Oesophageal fibrovascular polyp Arch anomaly Azygos vein Vascular node Posterior Neurogenic Bone and marrow Neuroenteric cyst Schwannoma Meningocele Extramedullary hematopoiesis Descending aorta More than One Lesion Infection Hemorrhage Lung Cancer Lymphangioma Mediastinitis Liposarcoma Hemangioma April 27, 2022 26
- 27. ANTERIOR MEDIASTINAL MASS • Silhouette with right cardiac border,ascending aorta • Obliteration of Anterior junction line • Hilum overlay Sign positive • Obliteration of CP angle & Retrosternal space • Mass effect on trachea
- 28. THYMOMAS • It is the most common primary neoplasm of Anterior Mediastinum. • Most thymomas arise near junction of heart and great vessel . • Plain Radiographs • Thymomas appear sharply marginated and smooth or lobulated in contour and usually project one side of mediastinum. • dense calcification may be seen throughout the mass or its periphery. • Computed Tomography(CT) • Almost all thymomas occur in pre-vascular space and displace great vessels. • Thymomas usually appears homogenous in attenuation with or without contrast. Some large thymomas appear cystic or contain areas of necrosis.
- 31. THYMIC CYST • Thymic cysts are cysts that occur within or arise from the thymus. • Thymic cysts can fluctuate both in size and attenuation over time on CT and MRI. • Plain radiograph • May not even be visible (especially small lesions). If visible thymic cysts often indistinguishable from other non-lobulated thymic/anterior mediastinal lesions on radiographs. • CT • Typically manifests as unilocular or multilocular cystic masses with well-defined walls. Lesions can be lobulated and may have soft-tissue attenuation components. • Some thymic cysts may have increased CT attenuation if haemorrhage or infection occurs as a complication
- 33. Germ Cell Tumors(GCT) • GCT accounts for 10% of primary mediastinal masses arises from primitive germ cells. • They are most common in anterior mediastinum. • GCT INCLUDES- • Benign and Malignant teratoma • Seminoma • Embryonal Carcinoma • Endodermal sinus tumour • choriocarcinoma
- 34. Teratomas • Mature teratomas constitute 60%-80% mediastinal GCT. • Plain Radiographs: • Usually Anterior med. mass projecting to one side of mediastinum. • Teratoma appears smooth,rounded or lobulated mass. • Computed Tomography(CT) • Usually appear in prevascular space. • CT often shows combination of fluid-filled cysts,fat,soft tissue and areas of calcification. • teratomas well encapsulated and well demarcated.
- 37. SEMINOMA Seminoma occurs entirely in men mean age is 29yrs.It is most common malignant mediastinal Germ cell tumor. PLAIN RADIOGRAPHS: Large lobulated anterior mediastinal mass projecting to one or both sides often obscuring heart borders. CT: Seminomas appear large,smooth,lobulated homogeneous soft tissue masses although small areas of low attenuation Can be seen
- 40. THYROID ENLARGEMENT • Thyroid enlargement commonly associated with extension into Anterior mediastinum. • Multinodular Goitre most common condition in which med thyroid abnormality detected. • Plain Radiographs: • sharply marginated,superior med mass causing tracheal narrowing or displacement of trachea contralateral side. • Mass appears poorly marginated above level of clavicles. • Computed Tomography(CT) • Thyroid tissue is high attenuation relative to soft tissue because of its high iodine content. • they usually dont project below arch of arota(differentiating them from thymomas &teratomas)
- 42. HODGKINS LYMPHOMA • Peak incidence third & eighth decades. • Thoracic involvement in 85% of cases at diagnosis. • HL most often involves superior mediastinal lymph nodes that is Prevascular,paratracheal and aortopulmonary LN. • HL associated with EBV infection in half of cases.it may occur in association with AIDS.
- 46. NON HODGKIN LYMPHOMA • It is more common then HL. Mean age is 55yr more common than HD in children. • Thoracic involvement is only 40-50%. • Superior mediastinal gp LN involved in nearly all patients.Involvement of single gp of LN group is common. • Posterior group of lymph node is more commonly involve then HL.
- 48. PERICARDIAL CYST • Pericardial cysts are uncommon benign congenital anomalies of the anterior and middle mediastinum. • They are most commonly found on the right side, in particular the right anterior cardiophrenic angle, but can be found almost anywhere adjacent to the heart. • Plain radiograph • Typically seen as a mass-like density at the cardiophrenic sulcus. They can be of different shapes and are not always round. May change in shape and size with inspiration and position. • CT • Usually appears as a well-defined, non-enhancing, fluid-attenuation, rounded mass next to the pericardium.
- 51. MIDDLE MEDIASTINUM • Widening of paratracheal stripe • Mass effect on trachea • Convex border of AP window • Distorsion of Azygoesophageal recess on right
- 52. Bronhiogenic cyst • Bronchiogenic cyst can be present any part of mediastinum but most commonly present in middle mediastinum. • Most occur in conatct with tracheobronchial tree and within 5cm of carina. • Plain Radiographs: • Cyst appear smooth,sharply marginated,round,or eliptical masses. • they may be large and can displace trachea or bronchii. • subcarinal cyst may result in convexity in superior part of azygoesophageal recess. • Computed Tomography(CT): • cyst appear similar as on chest radiographs. • Because of variable composition of fluid within cyst there attenuation is highly variable. • Half of cyst are of water attenuation the other half higher then muscle.
- 56. POSTERIOR MEDIASTINAL MASS • Distorsion of paraspinal lines. • poterior ribs or vertebral erosion/remodelling. • cervicothoracic sign • obliteration of posterior junction line and descending aorta • distorsion of azygoesophageal lines
- 57. NEUROGENIC TUMORS • Neurogenic tumors is more common in children comapare to adults. • 75% posterior mediastinal masses are neurogenic tumors. • Types of neurogenic tumors arise from: 1. peripheral nerves(schwanoma,neurofibroma) 2. sympathetic ganglia(ganglioneuroma,neuroblastoma)
- 58. SCHWANNOMAS • Schwannomas, less commonly called neurinomas or neurilemmomas, are benign tumors of Schwann cell origin and are the most common tumor of peripheral nerves, including cranial nerves. • Radiographic features • General imaging features of schwannomas include: • well-circumscribed masses which displace adjacent structures without direct invasion • cystic and fatty degeneration is common • the larger a schwannoma, the more likely it is to show heterogeneity because of cystic degeneration or haemorrhage • CT • low to intermediate attenuation • intense contrast enhancement • small tumors typically demonstrate homogeneous enhancement • larger tumors may show heterogeneous enhancement • adjacent bone remodelling with smooth corticated edges
- 61. NEUROBLASTOMAS • Neuroblastomas are tumours of neuroblastic origin. Although they may occur anywhere along the sympathetic chain. • They represent the most common extracranial solid childhood malignancy. Plain radiograph • Appearances are non-specific, typically demonstrating an intrathoracic soft-tissue mass or an intra-abdominal mass displacing adjacent organs. • may cause remodelling of ribs, vertebral bodies or pedicle thinning. evidence of calcification on the plain film. CT • On CT, the tumour typically is heterogeneous with calcifications seen in 80-90% of cases. • Areas of necrosis are of low attenuation.
- 64. Mediastinal Hemangioma • Med. hemangioma is most common in young patient. • Hemangioma most commonly arise from anterior mediastinum compare to posterior. • ON CT: • Tumors often hetrogenous in attenuation and fat is ocasionally present. • Enhancement may be dense,multifocal,diffuse and cenral or peripheral. • punctuate calcification maybe seen. • Dilated mediastinal vessel may be associated with mass.
- 66. THANK YOU
Editor's Notes
- prevascular compartment (purple) wraps around the heart and pericardium, which are located in the visceral compartment (blue). Yellow = paravertebral compartment, green line = visceral-paravertebral compartment boundary line. INTERNATIONAL THYMIC MAIGNANCY INTRESITING GP definition of mediastinal compartments. Sagittal CT images at the levels of the aortic arch The most common abnormalities encountered in the prevascular compartment include thymic lesions ( thymoma, thymic carcinoma, and neuroendocrine neoplasms); germ cell neoplasms ; lymphoma; and intrathoracic goiter. he most common abnormalities in the visceral compartment include lymphadenopathy (related to lymphoma or metastatic disease), duplication cysts, BRONCHIOGENIC CYST tracheal lesions, and esophageal neoplasms. most abnormalities in this region are neurogenic neoplasms that arise from the dorsal root ganglia/neurons adjacent to the intervertebral foramina. Other potential lesions in this compartment are of infectious
- (b), left pulmonary artery (c), and left atrium
- LEFT - LUNG ABUTS THE MEDIASTINAL SRF AND CREATES ACUTE ANGLE WITH LUNG RIGHT-MED MASS SIT UNDER THE SRF OF MEDSTINUM CREATES OBTUSE ANGLES WITH LUNG
- This Sign is useful differntiating whether an opacity on fronal chest radiograph in the region of lung hilum is loacted within the hilum versus anterior or posterior.
- Chest xray pa shows we can easily appreciate pulmonary vessel within the mass so this mass may be in middle med
- A-IF VESSEL CONVERGE MEDIAL TO HILAR SHADOW THEN ENLAGEMENT DT MASS B I VESSEL CONVERGE N MERGE DIRECTLY ON HILAR SHADOW THEN ENLARGEMENT IS D/T ENLARGED VESSEL.
- 1 SHOWS INFERIOR MARGIN OF MASS IS CONVERGING TOWARDS SPINE.THIS SIGNIFIES MASS IS ALMOST INTRATHORACIC 2 SHOWS INFE MARGIN OF MED MASS DIVERGES AWAY FROM MIDLINE THIS SIGNIFIES LARGE COMPENENT OF MASS LIES WITHIN ABDOMEN.
- CT scan demonstrates a normal anterior junction line (arrow) obliteration or abnormal convexity of the line suggests underlying anterior mediastinal disease such as thyroid masses, lymphadenopathy, neoplasms, thymic masses, or lipomatosis (,4). Volume loss and hyperinflation of the surrounding lung can also displace the line (,Fig 3,).
- and frontal chest radiograph demonstrate a normal posterior junction line CT scan demonstrates a normal posterior junction line (arrow) Abnormal bulging or convexity of the posterior junction line suggests a posterior mediastinal abnormality such as esophageal masses, lymphadenopathy, aortic disease, or neurogenic tumors.
- It has a maximum normal thickness of 4 mm. ARCH OF AZYGOUS VEIN T4-T5
- frontal chest radiograph demonstrate a normal right paratracheal stripe ( arrows in). cT scan shows that the right paratracheal stripe (arrow) is formed by air within the right upper lobe and trachea outlining the right lateral tracheal wall, right upper lobe pleura, and intervening soft tissues. A wide variety of disease entities can cause widening or abnormal contour of the right paratracheal stripe, such as paratracheal lymphadenopathy, thyroid or parathyroid neoplasms (,Fig 8,), and tracheal carcinoma or stenosis. Pleural disease such as effusion or thickening is among the most common causes for widening of the right paratracheal stripe (,1,,3,,4).
- The stripe extends superiorly from the aortic arch to join with the reflection from the left subclavian artery
- Normal lt paratracheal stripe seen.
- the left paraspinal line is seen more frequently than the right paraspinal line due to the presence of the descending thoracic aorta on the left, which promotes the tangential contact of the left lung necessary to produce the lung-mediastinum interface an abnormal contour of the left paraspinal line; however, tortuosity of the descending thoracic aorta may also displace it. Abnormal contour or displacement may also suggest additional posterior mediastinal abnormalities such as a mediastinal hematoma, a mass, extramedullary hematopoiesis, or esophageal varices (
- The right paraspinal line appears straight and typically extends from the 8th through the 12th thoracic vertebral levels CT ARROW SHOWS RT N LT PARASPINAL LINES The right paraspinal line may be displaced laterally by osteophytes or prominent mediastinal fat. However, abnormal contour or displacement may also suggest a posterior mediastinal abnormality such as a mediastinal hematoma
- CT scan shows that the azygoesophageal recess (arrow) is an interface formed by the right lower lobe outlining the mediastinum adjacent to the esophagus and azygos vein. XRAY demonstrate a normal azygoesophageal recess with mild leftward convexity superiorly and a straight edge in middle one third lower one third straight line. Abnormal contour and convexity may be due to lymphadenopathy, hiatal hernias,bronchopulmonary-foregut malformations, esophageal neoplasms, pleural abnormalities, and cardiomegaly with left atrial enlargement
- XRAY normal AP window as a shallow concave interface (*) between the aorta and the pulmonary artery.normal aortic-pulmonary stripe (arrows) and its relation to the AP window. AP STRIPE REPRESENTS MEDIASTINAL STRIPES reflection or interface formed by the pleura of theanterior left lung coming in contact with and tan-gentially reflecting over the mediastinal fat an-terolateral to the left pulmonary artery and aortic arch. CT scan shows the normal AP window (*). The concave interface seen in actually represents the lateral border (arrow) of the AP window formed by the left lung and pleura contacting the aortic arch and extending to the pulmonary artery.
- WE CAN LOACTE MASS ANATOMICAL LOCATION ON THE BASIS OF XRAY we can differentiate lesioN on CT N MRI IN CT WE HAVE DIFFERENT HU UNITS LIKE FOR FAT -50 TO -100 VASCULAR/BLOOD 40 FLUID -10 TO 20
- Most common age is 50-60yrs rare before 20yrs age a/w MG
- PA SHOWS LARGE THYMOMAS (T ARROE) OBSCURING RT HEaRT BORDER EXTENDING INTO RT CARDIOPHERENIC BORDER LAT SHOWS THYMOMAS(t) IS VISILE OVERLYING HEART SHADOW (ARROW)
- CT SHOWS CYSTIC FLUID ATTENUATION MASS IN RT CP ANGLE MASS SHOW DENSE CALCIFICATION INCLUDING CALCIFICATION OF CAPSULE
- axial contrast-enhanced CT image below the level of the carina shows a well-defined low-attenuation lesion (arrow) in the thymic bed of the prevascular mediastinum. The internal Hounsfield unit value was 15. MR imaging is the most useful imaging modality for distinguishing cystic from solid lesions, discerning cystic and/or necrotic components within solid masses, and identifying septa and/or soft tissue in cystic lesions.
- MOST COMMON IN 2-4 DECADE OF LIFE.
- most commonly occur in children and young 4types-mature,cystic,immature malignant
- CHEST PA SHOWS SMOOTH SHARPLY MARGINATED LEFT MED MASS IT OBSCURES LEFT HEART BORDER INDICATING ANTERIOR LOACTIONS. LAT SHOWS INC DENSITY OF RETROSTERNAL CSPACE(ARROW) BUT DISCRETE mASS NOT VISBLE
- TERATOMAS APPEARS LARGE MASS COMPRESSING RT CARDIAC STR IT CONTAINS CALCIFICATION AREAS OF FAT(ARROW)AND CYSTIC OR SOFT TISSUE REGIONS. The presence of visible regions of intralesional fat measuring between −40 and −120 HU at multidetector CT within a heterogeneous prevascular mediastinal mass is highly suggestive of a mature teratoma. These benign lesions characteristically demonstrate varying amounts of fat, fluid, calcification, and soft tissue
- PA CHEST RADIO SHOWS LARGE LOBULATED MED MASS (ARROW)OBSCURING RT HEART BORDER RT PLEURAL EFFUSION IS ALSO VISIBLE. LAT XRAY SHOWS LARGE ANTR MED MASS SEEN.
- BOTH CT SCAN IMAGE SHOWS LARGE RELATIVELY HOMOGENOUS MASS IN PREVASCULAR SPACE DISPLACING MEDIASTINAL STR TO LEFT.PLEURAL EFFUSION IS ALSO NOTED.
- with Hounsfield unit values of 70–85 due to the presence of iodine),
- ct shows enhancing mass is visble in right paratracheal med XRAY shows displacement of trachea towards contralateral side sharp margin of mass is seen pumonary vessel can be appreciated
- PLEURAL EFUSION DT LYMPHATIC OBSTRUCTION Pericardium invasion dt direct ivasion by tumor CHEST WALL INVASION TUMOR INVOLVE RIBS STERNUM RESULT IN LYTIC BONE LESION
- PA RADIOGRAPHS SHOWS B/L LOBULATED MEDSTINAL MASS LAT VIEW SHOWS MASS IN ANTERIOR MED
- CT SHOWS PREVASCULAR ANTERIOR MED LYMPHNODE ENLARGEMENT (ARROW) PRETRACHEAAL LYMPHNODE ENLARGEMENT (*) LN ENLARGE TYPICAL FOR HODGKIN LYMPHOMA BUT FOR CONFIRM DIAGNIOSIS WE NEED CT GUIDED BIOPSY
- XRAY PA SHOWS LEFT SIDE MED MASS WITH OBSCURING LEFT HEART BORDER.ELEVATION OF LEFT SIDE HEMI DIAPHRAGM MAY REFLECT DIAPHRAGMATIC PARALYSIS RELATED TO COMPRESSION OF LEFT PHERENIC NERVE. CT SHOWS THAT LYMPHADENOPATHY IS LIMITED TO PREVASCULAR COMPARTMENT(arrow).INVOLVEMENT OF SINGLE LN is common in NHL.
- XRAY PA SHOWS MASS IN RT CARDIOPHERENIC SULCUS WITH SHARP BORDERS OBSCURING RT HEART BORDERS.SIMILARLY WE CAN SEE ON LATERAL CHEST XRAY MASS IN ANTERIOR MEDIASTIUM
- axial contrast-enhanced multidetector CT image at the level of the ventricles shows a well-circumscribed, homogeneous, fluid attenuation lesion (M) with imperceptible walls in the right cardiophrenic angle. These findings are pathognomonic for a pericardial cyst.
- PA SHOWS SUBACRINAL MASS WITH INCREASE OPACITY(*) SPLAYING CARINA ABNORMAL CONVEXITY OF UPPER AND MIDDLE THIRD OF AZYGOESOPHAGEAL RECESS CT CONFIRMS SUBCARINAL MASS (ARROW)
- bronchogenic cysts appear at a subcarinal location (most commonly) oesophageal cysts appear more tubular and in close relation to the oesophagus ON CT Thin-walled bronchogenic cyst relatively thick-walled oesophageal cyst (due to the presence of smooth muscle)
- axial contrast-enhanced CT image at the level of the aortic arch shows a well-circumscribed, homogeneous, fluid attenuation mass (M) adjacent to and intimately associated with the upper thoracic esophagus. The location of the abnormality enables definitive diagnosis of an esophageal duplication cyst with imaging alone.
- PA WELL DEFINED MASS SHARP BORDERS CERVICOTHORACIC SIGN POSITIVE LARERAL VIEW MASS LOCATED POSTERIORLY
- A-WELL DEFINED HOMOGENOUS MASS VISIBLE ON CT B- CT SHOWS PARAVERTEBRAL MASS IN HETROGENOUS PERIPHERAL ENAHNCEMENT MASS EXTENDINTO NEURAL FORAMEN (ARROES)WHICH IS ENLARGED COMAPRE TO RIGHT
- mediastinal neuroblastoma- xray pa and lat shows large superior posterior med mass
- CT IMAGE SHOWS LARGE PARAVERTEBRAL POSTERIOR MEDIASTINAL MASSES CONTAING SMALL AREAS OF CALCIFICATION T2W MRI SHOWS MASS IN POSTERIOR MED TUMOR EXTEND INTO SPINAL CANAL THROUGH NEURAL FORAMEN(WHITE ARROW) DISPLACING SPINAL CORD IN RIGHT (BLACK ARROW)
- Med HEMANGIOMA CAN ARISE FROM ANY PART OF MEDIASTINUM
- mediastinal hemangioma A CT SHOWS LARGE MASS IN SUBCARINAL SPACE CONATAIN PUNCTUATE CALCIFICATION ALSO KNOWN AS PHLEBOLITHS B)AT HIGHER LEVEL SVC (large arrow) and AZYGOUS VEIN(SMALL ARROE) DILATED. DILATED VEINS ARE VISBLE IN MEDIASTINUM POSTERIOR TO SVC.