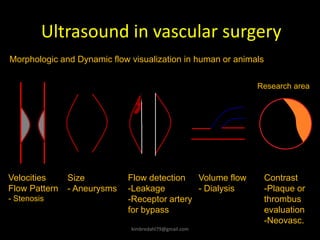
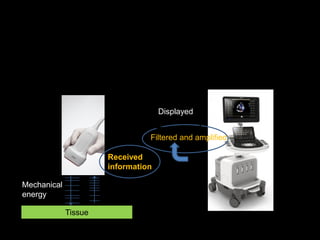
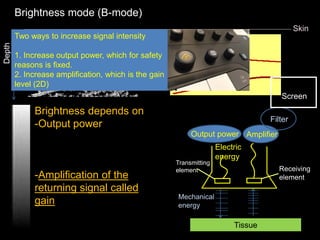
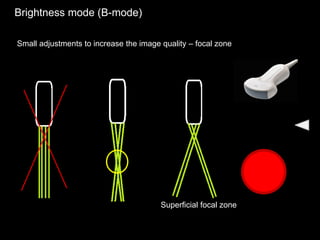
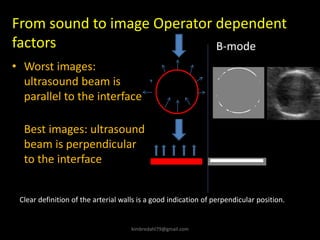
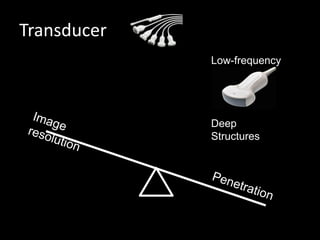
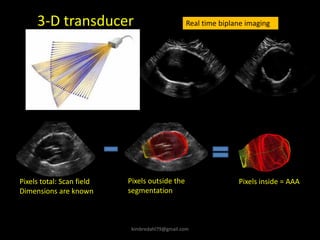
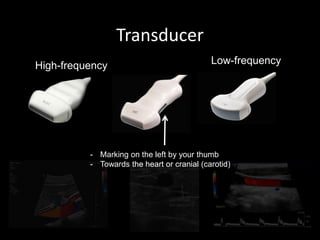
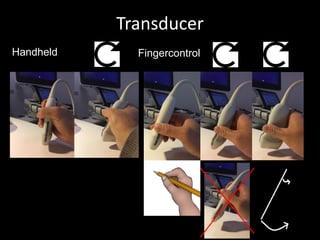
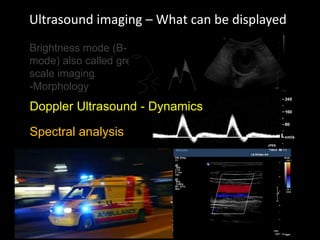
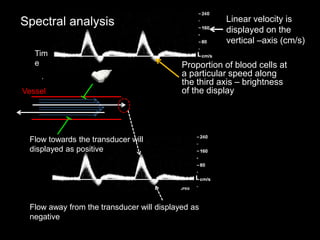
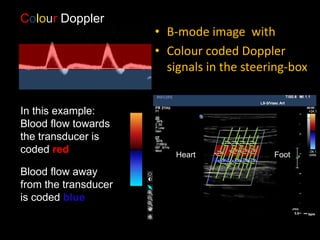
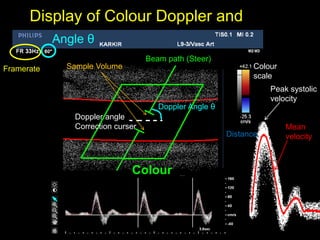
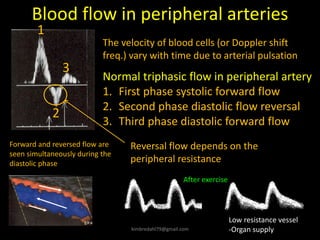
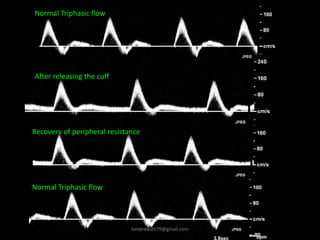
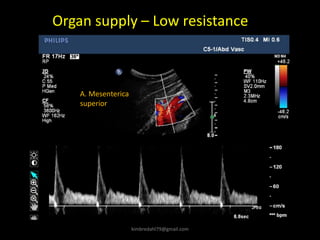
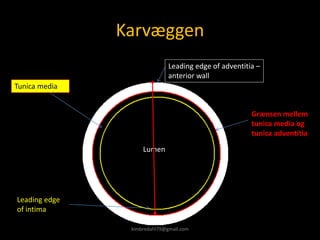
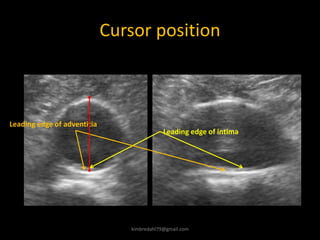
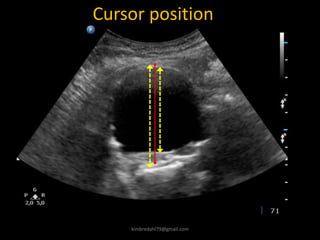
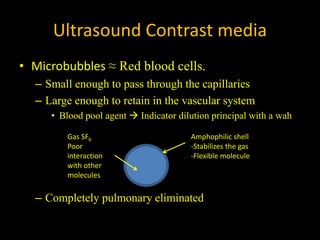
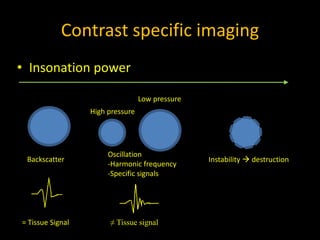
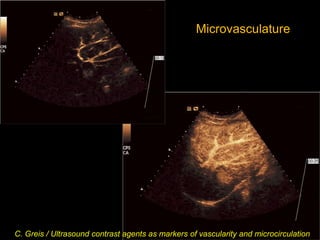
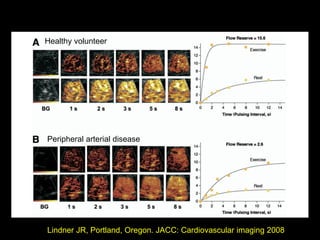
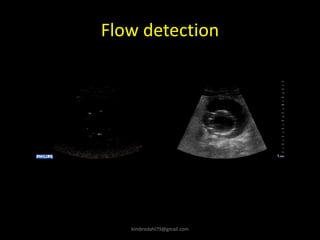
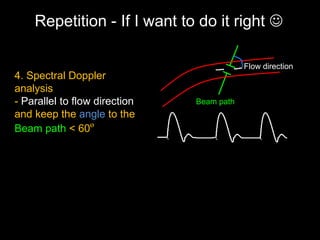
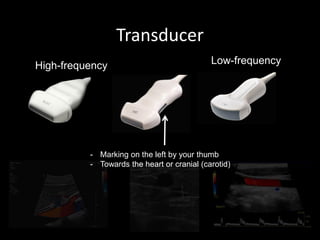
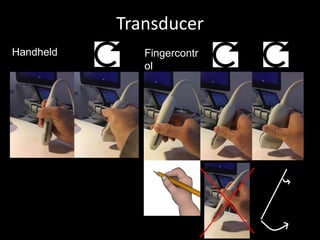
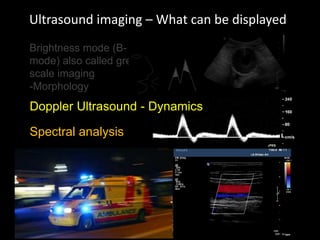
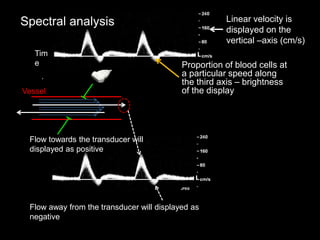
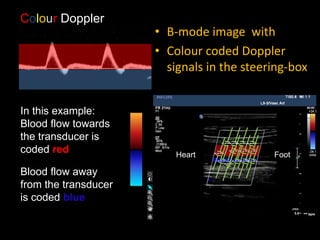
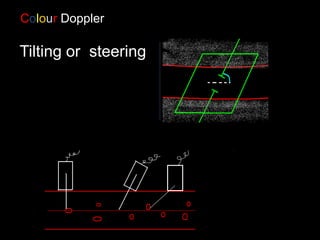
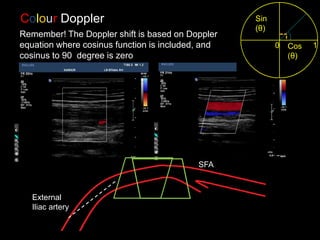
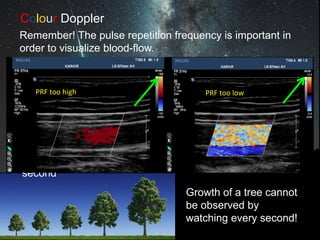
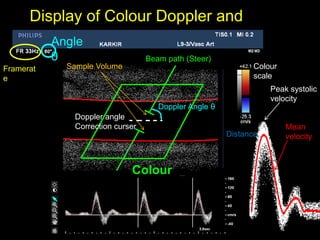
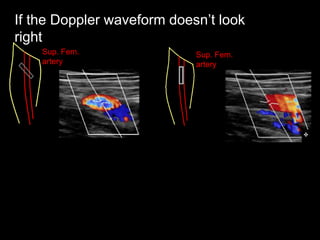
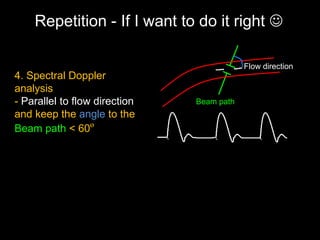
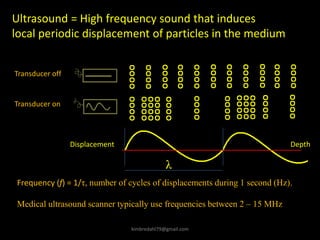
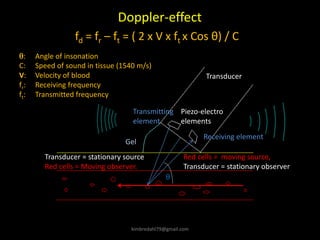
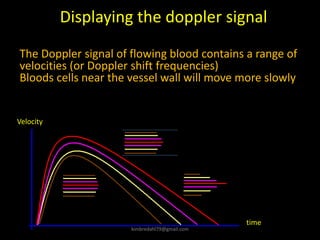
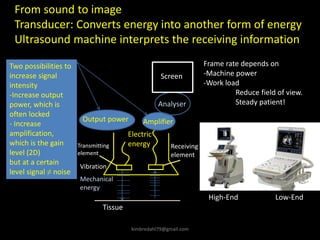
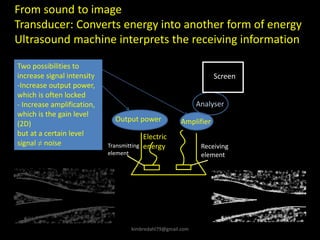
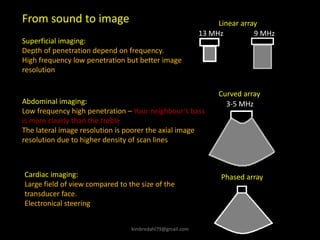
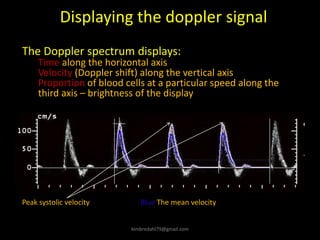
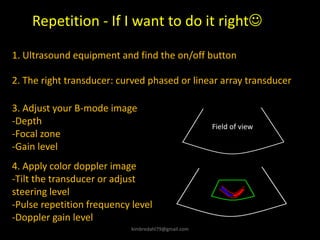
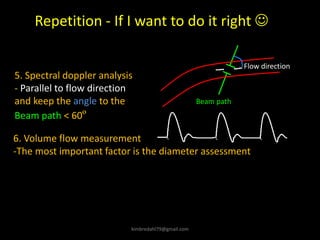
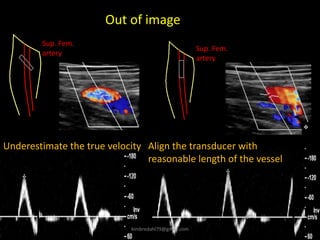
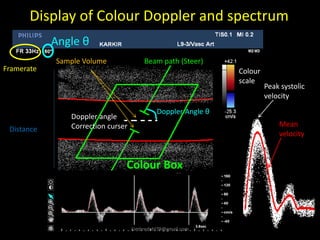
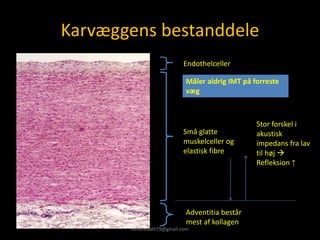
This document provides an overview of vascular ultrasound. It discusses using ultrasound to assess aneurysms, stenosis, and blood flow. Key aspects of vascular ultrasound covered include brightness mode imaging to assess morphology, color Doppler to visualize flow dynamics, and spectral analysis to measure velocities and calculate volume flow. The document reviews ultrasound equipment, transducer selection, optimizing the B-mode image, and techniques for Doppler ultrasound including avoiding angles over 60 degrees. It also discusses flow measurement pitfalls and using ultrasound contrast to enhance imaging of microvasculature and detect low flow. The goals are to provide basic knowledge of vascular ultrasound and hands-on practice of techniques.