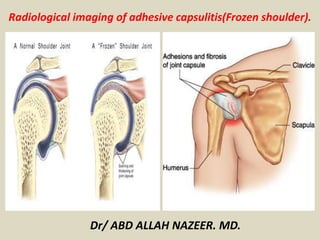
Presentation1, radiological imaging of adhesive capsulitis(frozen shoulder).
- 1. Dr/ ABD ALLAH NAZEER. MD. Radiological imaging of adhesive capsulitis(Frozen shoulder).
- 2. Adhesive capsulitis of the shoulder is a clinical condition characterized by progressive limitation of active and passive mobility of the glenohumeral joint, generally associated with high levels of pain. Although the diagnosis of adhesive capsulitis is based mainly on clinical examination, different imaging modalities including arthrography, ultrasound, magnetic resonance, and magnetic resonance arthrography may help to confirm the diagnosis, detecting a number of findings such as capsular and coracohumeral ligament thickening, poor capsular distension, extracapsular contrast leakage, and synovial hypertrophy and scar tissue formation at the rotator interval. Ultrasound can also be used to guide intra- and periarticular procedures for treating patients with adhesive capsulitis.
- 3. Clinical presentation Adhesive capsulitis presentation can be broken into three distinct stages: freezing: painful stage patients may not present during this stage because they think that eventually, the pain will resolve if self-treated as the symptoms progress, pain worsens and both active and passive range of motion (ROM) becomes more restricted this can eventually result in the patient seeking medical consultation typically lasts between 3 and 9 months and is characterised by an acute synovitis of the glenohumeral joint frozen: transitional stage most patients will progress to the second stage during this stage, shoulder pain does not necessarily worsen because of pain at the end of the range of motion, arm movement may be limited, causing muscular disuse can last between 4 to 12 months the common capsular pattern of limitation has historically been described as diminishing motions with external shoulder rotation being the most limited, followed closely by shoulder flexion, and internal rotation a point is eventually reached in the frozen stage where pain does not occur at the end of the range of motion
- 4. thawing stage(Resolution stage). begins when the range of motion starts to improve lasts anywhere from 12 to 42 months and is defined by a gradual return of shoulder mobility Pathology Adhesive capsulitis is divided into two main types: primary or idiopathic absence of preceding trauma secondary major or minor repetitive trauma shoulder or thoracic surgery endocrine, e.g. diabetes, hyperthyroidism rheumatological conditions
- 5. Radiographic features Fluoroscopic arthrography Described features include: limited injectable fluid capacity of the glenohumeral joint small dependent axillary fold small subscapularis bursa irregularity of the anterior capsular insertion at the anatomic neck of the humerus lymphatic filling may be present Ultrasound Limitation of movement of the supraspinatus is considered a sensitive feature. A thickened coracohumeral ligament (CHL) can also be a suggestive feature of adhesive capsulitis.
- 6. MRI/MR arthrography normal inferior glenohumeral ligament measures <4 mm and is best seen on coronal oblique images at the mid glenoid level; in adhesive capsulitis, the axillary recess may show thickening ≥1.3 cm joint capsule thickening abnormal soft tissue thickening within the rotator interval with signal alteration abnormal soft tissue encasing the biceps anchor variable enhancement of the capsule and synovium within the axillary recess and rotator interval Other MR arthrography features include: thickening of the coracohumeral ligament (CHL) subcoracoid triangle sign
- 7. Conventional arthrography, anteroposterior view. (a) Normal distension of the axillary recess (black arrow) and the subscapular recess (thick arrow). (b) Reduced distension of the axillary recess (black arrow) and subscapular recess associated with medial leakage of contrast (white arrow) in a patient with adhesive capsulitis.
- 8. Axillary long-axis view of the inferior glenohumeral ligament with arm in abduction. (a) Thickening of the inferior capsular profile (calipers, 3.3 mm) in a shoulder affected by adhesive capsulitis. H humerus (b) In the contralateral shoulder, the capsule has normal thickness (calipers, 1.5 mm)
- 9. Coronal oblique T2- weighted fat-saturated (a, b) and axial proton density fat-saturated (c, d) images. In a healthy subject (a, c), the capsular recess has normal signal intensity (arrows), while in a patient with adhesive capsulitis (b, d), clear signal hyperintensity can be seen (arrows). H humerus, G glenoid, S supraspinatu s tendon
- 10. Coronal oblique proton density image in a patient with adhesive capsulitis. The axillary pouch (arrows) is thickened. G glenoid, H humerus.
- 11. MR arthrography, coronal oblique T1-weighted fat-saturated image. (a) In a healthy subject, the axillary pouch is normally distensible (arrow). H humerus, G glenoid. (b). In a patient with adhesive capsulitis, the axillary pouch is contracted and poorly distended (arrow)
- 12. MRI scan showing thickened (5mm) inferior capsule (normally 1mm).
- 13. Left Shoulder. Coronal T2 FS image of a 33-years-old male patient. Shows thickened GHLI (5,58mm) synovial intraarticular liquid increase.
- 14. T2-fatsat MRI: Thickening of the capsule in the axillary recess, and intermediate signal in adjacent soft tissues.
- 15. Coronal T1 (left) and PD-fat sat (right) MRI. Thickening (left) and intermediate signal (right) of the joint capsule in the axillary recess in a patient with adhesive capsulitis.
- 16. MR arthrography, (a) coronal oblique and (b) axial T1-weighted fat-saturated image in a patient with adhesive capsulitis. Leakage of contrast agent can be seen on the anterior inferior margin of the scapula (arrow). H humerus, G glenoid
- 17. Oblique coronal PDFS image of a 45-year- old woman after recent trauma. There is thickening and edema of the axillary recess(white arrow). Oblique coronal T1 weighted image of a 57-year- old man with clinically proven adhesive capsulitis. There is thickening of the axillary recess, which is only mildly hyperintense (white arrows).
- 18. Adhesive capsulitis of the shoulder.
- 21. MRI findings are subtle in frozen shoulder. To be certain, frozen shoulder is a clinical diagnosis, and there are no specific direct signs that are pathognomonic for frozen shoulder. Described direct signs suggestive of frozen shoulder include: Thickening of the glenohumeral joint capsule along the axillary pouch Thickening of the coracohumeral ligament Obliteration of the subcoracoid fat triangle Rotator interval synovitis.
- 22. MRI shows- poor definition of coracohumeral ligament with abnormal intermediate amorphous signal (with hypointense foci on all sequences) surrounding the ligament with ill definition of superior glenohumeral ligament & rotator interval with mild free fluid in the shoulder joint – likely suggesting adhesive capsulitis.
- 23. Inferior glenohumeral ligament and the inferior joint capsule (yellow block arrow) in the axillary recess shows diffuse thickening. Diffuse thickening of the coracohumeral ligament (white arrow) extending up to the rotator cuff interval and is hyperintense on the T2 images.
- 24. (2a) The sagittal T2-weighted image demonstrates a thickened coracohumeral ligament (arrow) and soft tissue thickening in the rotator interval (arrowheads). The short arrow indicates the adjacent long head of the biceps tendon. (2b) The coronal T2-weighted fat-suppressed image demonstrates an abnormally thickened inferior glenohumeral ligament (arrow). (2a) (2b)
- 25. Adhesive capsulitis is a self-limited clinical syndrome characterized by painful, gradual loss of active and passive glenohumeral motion.
- 26. Sagittal oblique T1-weighted image (TR/TE = 550 ms/15 ms) (1A) shows thickened CHL (arrows). C = inferior margin for the coracoid process. Sagittal oblique (1B), oblique coronal (1C), and transverse (1D) fat-suppressed, proton density weighted, spin-echo image (TR/TE = 3000 ms/34 ms) show high-signal intensity soft tissue in the rotator cuff interval for the same patient (arrows). Coronal oblique (1E) and transverse (1F) fat-suppressed, proton density, weighted spin-echo image (TR/TE = 3000 ms/34 ms) demonstrate a thickened inferior glenohumeral ligament (axillary recess) for the same patient (arrows).
- 27. Magnetic Resonance Imaging, Arthrography, and Ultrasonography Reflect Clinical Impairment in Patients With Idiopathic Adhesive Capsulitis of the Shoulder.
- 28. Oblique sagittal PDFS image of a 69-year- old man. There is thickening of the CHL, and fibrovascular tissue with mild edema in the rotator cuff interval(white arrow). Fibrovascular changes are visible around CHL and around SGHL. Axial PDFS images (A,B) through the rotator cuff interval shows extensive fibrovascular tissue around the biceps tendon (white arrow).
- 29. Sagittal oblique T2-weighted image in a patient with adhesive capsulitis. The coracohumeral ligament (arrows) is markedly thickened. MR arthrography, sagittal oblique T1- weighted image. In a patient with adhesive capsulitis for 15 weeks, the fat triangle (arrowheads) signal is considerably reduced.
- 30. Oblique sagittal PD weighted image shows obliteration and fibrosis in subcoracoid space. Oblique sagittal oblique PD weighted image shows thickened CHL (arrow) in a 57-year-old man with adhesive capsulitis.
- 31. A coronal T2-weighted fat suppressed image through the anterior aspect of the shoulder demonstrates increased signal intensity (asterisk) in the rotator interval region, obscuring the normal fat, suspicious for adhesive capsulitis. Post IV gadolinium enhanced sagittal T1-weighted image with fat-suppression demonstrates enhancement in the rotator interval region (arrows), confirming the diagnosis of adhesive capsulitis.
- 32. Sagittal oblique T1 MRI. Thickened coracohumeral ligament (arrows) in a patient with frozen shoulder.
- 33. T1 sagittal oblique MRI (left): Almost complete obliteration of subcoracoid fat (arrow); T2 fat-sat sagittal oblique MRI (right): intermediate signal scar in the rotator interval.
- 34. Adhesive capsulitis with frozen Shoulder.
- 35. Thank You.
