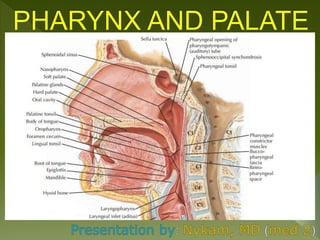
Pharynx and palate
- 2. The pharynx is a funnel shaped fibromuscular tube, extending from the base of the skull to the esophagus. It is lined through out with mucous membrane. The pharynx act as a common channel for both air (respiration) and food (deglutition). Location: It is situated behind the nose, mouth and larynx with which it communicates. Boundaries and Relations. Superior: Base of the skull including the posterior part of the body of sphenoid and basilar part of the occipital bone in front of the pharyngeal tubercle. Inferior: continous with the esophagus at the level of the the lower border of the cricoid cartilage anteriorly and lower border of C6 posteriorly.
- 3. Posterior: prevertebral fascia of the cervical spine. The pharynx is separated from prevertebral fascia only by a layer of loose areolar tissue, which allows the pharynx to slide freely on this fascia during swallowing. Anterior: opens into nasal cavities, mouth and larynx. Lateral: Neurovascular bundle of neck and styloid process with it’s attached muscles and ligaments. Subdivisions. The pharynx is divided into three parts. From above downwards, we have the following structures; - Nasopharynx, lying behind the nasal cavity. - Oropharynx, lying behind the oral cavity. - Laryngopharynx, lying behind the larynx.
- 5. 1- Nasopharynx. The nasopharynx lies behind the nasal cavity and above the soft palate. Boundaries. Roof: it is formed by the body of the sphenoid bone and basilar part of the occipital bone. Floor: it is formed by; -soft palate - pharyngeal isthmus, an opening in the floor between the free edges of soft palate and posterior pharyngeal wall. Anterior wall: it is formed by the posterior nasal apertures separated by the posterior edge of nasal septum. Posterior wall: it is formed by the anterior arch of C1 vertebrae. Lateral wall: medial pterygoid plate of the sphenoid.
- 6. Features. The features seen in the nasopharynx are as follows; a.) Nasopharyngeal (pharyngeal) tonsil: it is a collection of lymphoid tissue beneath the mucous membrane at the junction of the roof and the posterior wall of the nasopharynx. A mucous diverticulum called nasopharyngeal bursa extends upwards into the nasopharyngeal tonsil. b.) Orifice of the pharyngotympanic or auditory tube (eustachian tube). The upper and posterior margins of this opening are bounded by a tubal elevation, which is produced by a collection of lymphoid tissue called tubal tonsil or torus tubarius. Two mucous fold extend from this elevation; - salpingopharyngeal fold extends downward and fades on the side wall of the pharynx. It contains the salpingopharyngeus muscle.
- 7. - salpingopalatine fold extends downward and forward to the soft palate. It contains the levator palati muscle. c.) Pharyngeal recess. It is a deep depression behind the tubal elevation; it is called the pharyngeal recess (fossa of rosenmuller). (see diagram behind).
- 9. 2- Oropharynx. It lies behind the oral cavity and extends from the lower surface of the soft palate above to the upper surface of the epiglottis below. Boundaries. Roof: it is formed by; - soft palate - pharyngeal isthmus through which it communicates with the nasopharynx. Floor: it is formed by; - posterior 1/3 of the tongue. - interval between the tongue and epiglottis Anterior wall; it is formed by; - oropharyngeal isthmus through which it communicates with the oral cavity. - pharyngeal part of the tongue
- 10. Posterior wall: it is formed by the body of C2 and the upper part of the body of C3. Lateral wall: on each side, it is surrounded by the pterygomanidular raphe, mandible, tongue and hyoid bone. Features. The features seen in the oropharynx are; a.) lateral wall presents palatine tonsil, one on either side. It is located in the triangular fossa (tonsillar fossa) bounded anteriorly by the palatoglossal arch and posteriorly by the palatopharyngeal arch. b.) anterior wall presents; - lingual tonsil, formed by numerous nodules of lymphoid tissue underneath the pharyngeal part of the tongue. - upper free end of epiglottis, behind the tongue. - median and lateral glossoepiglottic folds, connecting the anterior surface and edges of the epiglottis.
- 11. - epiglottic valleculae, are shallow fossa between the median and lateral glossoepiglottic folds.
- 13. Oropharyngeal isthmus. It is an arched opening between the two palatoglossal folds through which the oral cavity communicates with the oropharynx. It has the following boundaries; Above, by the soft palate Below, by the dorsal surface of the posterior 1/3 of the tongue Laterally, by the palatoglossal arch/fold on either side containing palatoglossus muscle. The oropharyngeal isthmus is closed during deglutition to prevent regurgitation of food from the pharynx to the mouth.
- 16. 3- Laryngopharyx. The larygopharynx lies behind the pharyngeal inlet and the posterior wall of the larynx. It lies behind the larynx and extends from the upper border of the epiglottis to the lower border of the cricoid cartilage anteriorly and lower border of C6 vertebrae posteriorly. It communicates anteriorly with the laryngeal cavity through the laryngeal inlet and inferiorly with the esophagus at the pharyngoesophageal junction. Boundaries. Anterior wall: it is formed by; - laryngeal inlet - posterior surface of the larynx Posterior wall: it is supported by the body of C3, C4, C5 and C6 vertebrae. Lateral wall: it is supported by thyroid cartilage and thyrohoid membrane.
- 17. Features. The features seen in the laryngopharynx are as follows; Anterior wall presents the laryngeal inlet and below the inlet it is supported by cricoid and arytenoid cartilage. Lateral wall presents the piriform fossa one on either side of the laryngeal inlet.
- 19. Piriform Fossa. It is a deep recess broad above and narrow below in the anterior part of the lateral wall of the laryngopharynx, on each side of the laryngeal inlet. These recesses are produced by the bulging of the larynx into the laryngopharynx. Boundaries. Medial: Aryepiglottic fold and quadrangular membrane of larynx. Lateral: mucous membrane covering the medial surface of the lamina of thyroid cartilage and thyrohoid membrane. The internal laryngeal nerve and superior laryngeal vessels pierce the thyrohyoid membrane. Above: piriform fossa is separated from the epiglottic valleculae by the lateral epiglottic fold.
- 21. Pharyngeal wall. The walls of the pharynx consist of four layers, from within outwards, we have the following; 1- Mucous membrane/mucous coat 2- Pharyngobasilar fascia/pharyngeal aponeurosis 3- Muscular coat/pharyngeal muscles 4- Buccopharyngeal fascia/loose areolar sheath Mucous membrane/ mucous coat: The mucous membrane lining the pharynx contains a considerable amount of elastic tissue and is continuous with the mucous lining of eustachian tubes, nasal cavity, mouth, larynx and esophagus. It is lined by non keratinized stratified squamous epithelium except in the region of the nasopharynx, where it is lined by ciliated columnar epithelium(respiratory epithelium).
- 22. Pharyngobasilar fascia: it is a fibrous thickening of the submucosa. It lines the muscular coat and is thicker at the base of the skull but thin and indistinct inferiorly. Muscular coat: the muscular coat consist of the following two striated muscles; - the outer layer consist of three pairs of circular muscles called constrictors. - the inner layer consist of three pairs of longitudinal muscles. Buccopharyngeal fascia: it is a fascia which covers the outer surface of the constrictor muscles. In the upper part, it is prolonged forward to cover the buccinator muscles, hence the name buccopharyngeal fascia. Above the upper border of the superior constrictor, it blends with the pharyngobasilar fascia.
- 23. The Waldeyer’s ring. It is an interrupted circle of tonsils at the upper end of the respiratory and alimentary tract. The Waldeyer’s ring is formed by: 1. Pharyngeal tonsil (nasopharyngeal tonsil), posterosuperiorly. 2. Lingual tonsil, anteriorly. 3. Tubal and palatine tonsils, laterally. It is thought that, Waldeyer’s ring prevents the invasion of microorganisms from entering the air and food passages and this helps in the defense mechanism of the respiratory and alimentary systems.
- 26. A- Constrictor Muscles. The three constrictor muscles of the pharynx (superior, middle and inferior) are arranged like a flowerpot without base, placed one above the other and open in front for communication with the nasal, oral and laryngeal cavities. Thus the inferior constrictor overlaps the middle, which also in turn overlaps the superior constrictor. 1- Superior constrictor: it is quadrilateral in shaped. Origin: the pterygoid hamulus, pterygomandibular raphe, side of the posterior part of the tongue. Insertion: pharyngeal tubercle and median fibrous raphe. Nerve supply: pharyngeal branch of the vagus nerve carrying fibres of cranial root of the accessory nerve. Action: helps in deglutition.
- 27. 2- Middle constrictor: It is fan shaped. Origin: lower part of the stylohyoid ligament, lesser cornu of hyoid, upper border of the greater cornu of hyoid. Insertion: median fibrous raphe Nerve supply: Pharyngeal branch of the vagus nerve carrying fibres of cranial root of the accessory nerve. Action: helps in deglutition.
- 28. 3- Inferior constrictor: It is divided into two; thyropharyngeus and cricopharyngeus. Thyropharyngeus Origin: lamina of the thyroid cartilage and tendinous band between the thyroid tubercle and cricoid cartilage. Insertion: median fibrous raphe. Nerve supply: pharyngeal plexus and external laryngeal nerve. Cricopharyngeus Origin: cricoid cartilage Insertion: median fibrous raphe Nerve supply: recurrent laryngeal nerve Action: both help in deglutition.
- 30. Gaps in the pharyngeal wall. The four gaps exist on either side of the pharyngeal wall in relation with the constrictor muscles. These gaps include;
- 32. B- Longitudinal muscles. These muscles run longitudinally from above downwards to form the longitudinal muscle coat. 1- Stylopharyngeus. Origin: medial surface of the base of styloid process. Insertion: lamina of the thyroid cartilage. Nerve supply: Glossopharyngeal (IX) nerve 2- Palatopharyngeus. Origin: by two fasciculi from the upper surface of the palatine aponeurosis. Insertion: lamina of the thyroid cartilage. Nerve supply: cranial root of the accessory nerve through the pharyngeal plexus.
- 33. 3- Salpingopharyngeus. Origin: lower part of the cartilage of the auditory tube. Insertion: lamina of the thyroid cartilage. Nerve supply: cranial root of the accessory nerve through the pharyngeal plexus. Actions of the longitudinal Muscles. They elevate the larynx and shorten the pharynx during swallowing. At the same time, palatopharyngeal sphincters formed by some fibres of the palatopharyngeus muscle closes the nasopharyngeal isthmus.
- 35. Nerve supply of the pharynx. Motor supply: all pharyngeal muscles are supplied by the cranial root of the accessory nerve (through the pharyngeal branch of the vagus and the pharyngeal plexus), except the stylopharyngeus muscle which is supplied by the glossopharyngeal nerve (IX) nerve. Sensory supply: - Nasopharynx, by the pharyngeal branch of the pterygopalatine ganglion carrying fibres from the maxillary division of the trigeminal nerve. - Oropharynx, by glossopharyngeal nerve. - Laryngopharynx, by internal laryngeal nerve.
- 37. Pharyngeal plexus of the nerves. It lies on the posterolateral aspect of the pharynx over the middle constrictor below the buccopharyngeal fascia. It is formed by: - Pharyngeal branch of the vagus, carrying fibres from cranial root of the accessory nerve. - Pharyngeal branch of the glossopharyngeal nerve - Pharyngeal ganglion of the superior cervical sympathetic ganglion.
- 38. Arterial supply of the pharynx. The branches of the following arteries supply the pharynx; - Ascending pharyngeal artery (from external carotid artery). - Ascending palatine and tonsillar artery (from facial artery). - Greater palatine and pharyngeal artery (from maxillary artery). - Lingual artery (from external carotid artery). - Superior thyroid artery (from the external carotid artery). - Inferior thyroid artery (from thyrocervical trunk).
- 40. Venous drainage of the pharynx. The venous blood from pharynx is largely drained into pharyngeal venous plexus, which drains into the internal jugular vein. Lymphatic drainage of the pharynx. The lymph from pharynx is drained into the upper and lower deep cervical lymph nodes directly and through the retropharyngeal lymph nodes.
- 42. Deglutition (swallowing). Deglutition is a process by which food is moved from the mouth to the stomach. It consist of the following three successive stages/phases: - First stage (in the mouth): voluntary - Second stage (in the pharynx): involuntary - Third stage (in the esophagus): involuntary 1- First stage. In this stage, the mouth is closed, the anterior part of the mouth is raised against the hard palate to push the masticated food progressively in the posterior part of the oral cavity. The soft palate closes down onto the back of the tongue to help form the bolus of food. Now the hyoid bone moves up to push food from the oral cavity to the oropharynx through the oropharyngeal isthmus.
- 45. 2- Second stage. This stage is very rapid. The nasopharyngeal isthmus is closed by elevation of the soft palate and contraction of passavant’s ridge to prevent entry of food into the nasopharynx. The laryngeal inlet is closed by aryepiglottic folds to prevent entry of food into the larynx. Now the pharynx and larynx are elevated above the hyoid bone by the longitudinal muscles of the pharynx and the bolus of food is pushed down over the posterior surface of the epiglottis by gravity and contraction of superior and middle constrictors. Thus food passes from the oropharynx to the laryngopharynx. This is followed by rapid downward displacement of the larynx and pharynx (by infrahyoid muscles), which reopens the laryngeal orifice.
- 48. 3- Third stage. In this stage, propulsive action of the thyropharyngeus followed by relaxation of the cricopharyngeus pushes food, which passes from laryngopharynx to the esophagus. From here it enters into the stomach by peristaltic movements in the esophageal wall.
- 50. Pharyngeal spaces. These are potential spaces in respect to the pharynx; 1- Retropharyngeal space: it is situated behind the pharynx and extends from the base of the skull above to the bifurcation of trachea below. 2- Parapharyngeal space: it is situated on the side of the pharynx. It contains carotid vessels, internal jugular vein, last four cranial nerves and cervical sympathetic chain.
- 51. Palatine tonsil. There are two palatine tonsils (commonly called tonsils). Each tonsil is an almond-shaped mass of lymphoid tissue situated in the triangular fossa (tonsillar fossa) of the lateral wall of the oropharynx between the anterior and posterior pillars of fauces. The anterior pillar is formed by the palatoglossal arch and the posterior pillar is formed by the palatopharyngeal arch. Boundaries of the tonsillar fossa/sinus. Anterior : palatoglossal arch containing palatoglossus muscle. Posterior: palatopharyngeal arch containing palatopharyngeal muscle. Apex : soft palate Base :dorsal surface of the posterior 1/3 of the tongue Lateral wall (tonsillar bed): superior constrictor muscle
- 52. Tonsillar bed. It is formed from within outwards by; - pharyngobasilar fascia - superior constrictor muscle - buccopharyngeal fascia External features. The tonsil presents the following features; 1- Medial surface: it is free and bulges into the oropharynx. It is lined with non keratinized stratified squamous epithelium, which dips into the substance of tonsil forming crypts. The number of crypts vary from 12 to 15 and their openings can be seen on the medial surface. One of the crypts situated near the upper part of the tonsil is very large and deep. It is called crypta magna or intratonsillar cleft and represents the remnant of the second pharyngeal pouch. The crypts may be filled with cheesy material consisting of epithelial cells
- 54. Lateral surface: it is covered by a well defined fibrous tissue, which forms the tonsillar hemicapsule. Between the bed of tonsil and the tonsillar hemicapsule is a loose areolar tissue (peritonsillar space), it is site of collection of pus in peritonsillar abcess. The superior constrictor muscle seperates this surface from the following structures: - facial artery and two of it’s branches, the ascending palatine and tonsillar. - styloglossus muscle and glossopharyngeal nerve. - styloid process - angle of mandible and medial pterygoid muscle. - submandibular salivary gland.
- 56. Anterior border: it passes underneath the palatoglossal arch. Posterior border: it passes underneath the palapharyngeal arch. Upper pole: it extends up to the soft palate. It’s medial surface is covered by a semilunar fold extending between the anterior and posterior pillars enclosing a potential space called supratonsillar fossa. Lower pole: it is attached to the tongue by a brand of fibrous tissue called suspensory ligament of the tonsil. The palatine tonsil is seperated from the tongue by the tonsilolingual sulcus.
- 57. Arterial supply of the palatine tonsil. The following arteries supply the tonsil; - tonsillar branch of facial artery (it is the principal artery and enters the lower pole by piercing the superior constrictor muscle). - dorsalis linguae artery of the lingual artery. - ascending palatine , a branch of facial artery. - ascending pharyngeal, a branch of external carotid artery. - greater palatine (ascending palatine), a branch of the maxillary artery.
- 59. Venous drainage of the tonsil. The veins from the tonsil drain into the paratonsillar vein. The paratonsillar vein descends from the soft palate across the lateral aspect of the tonsillar capsule and pierces the superior constrictor to drain into the pharyngeal venous plexus. Lymphatic drainage of the tonsil. The lymphatics of the tonsil drain into the upper deep cervical lymph node, particularly the jugulodigastric lymph node. It is ussually called the tonsilar lymph node. Nerve supply of the tonsil. Palatine tonsil is supplied by the glossopharyngeal nerve and the lesser palatine branches of the sphenopalatine ganglion.
- 60. Pharyngotympanic tube (auditory or eustachian tube). It is a mucous lined osseocartilaginous channel, which connects the nasopharynx with the tympanic cavity. It maintains the equilibrium of air pressure on either side of the tympanic membrane for it’s proper vibration. The pharyngotympanic tube is divided into 2 parts; 1- Osseous or bony part: it forms 1/3 of the total lenght of the tube. It lies between the tympanic and petrous part of the temporal bone and opens into the middle ear cavity. 2- Cartilagenous part: it forms 2/3 of the tube. Ends of the tube. The tympanic end of the tube is small and bony. It is situated in the anterior wall of the middle ear. The pharyngeal end is large and is situated at the lateral wall of the pharynx. The pharyngeal orifice is the widest part of the tube.
- 62. Lining of the tube. The tube is lined with pseudostratified ciliated columnar epithelium with goblet cells. The cilia beat in direction of the nasopharynx thus help to drain secretions and fluids from the middle ear to the nasopharynx. Functions. The functions of the auditory tube are as follows; 1- maintains the equilibrium of air pressure on either side of the tympanic membrane. 2- protection of middle by preventing transmission of high sound pressure from nasopharynx to the middle ear. As the tube remains closed. 3- Clearance of middle ear secretions by active opening and closing of the tube. The cilia of mucous lining of the tube beat in the direction of nasopharynx and drain the secretion of the middle ear into the nasopharynx.
- 65. The term palate refers to the roof of the mouth, it also forms the floor of the nasal cavity. It forms the partition between the nasal and oral cavity. The palate consist of two parts; 1- Hard palate, which forms the anterior 4/5 of the palate 2- Soft palate, which forms the posterior 1/5 of the palate 1- Hard palate. The hard palate is the partition between the nasal and oral cavity. It’s anterior 2/3 is formed by the palatine process of the maxillary bone and the posterior 1/3 is formed by the horizontal plate of the palatine bone. The superior and inferior surfaces of the hard palate form the floor of the nasal cavity and the roof of the oral cavity, respectively.
- 66. Anteromedially, the hard palate becomes continous with the alveolar arch and gums. Posteriorly, the hard palate is free and provides attachment to the soft palate. The inferior surface of the hard palate presents the following features; 1- Incisive fossa: a small pit anteriorly in the midline behind the incisor teeth, into which open the incisive canals. Each incisive canal/foramen (right and left) pierces the corresponding side and ascend into the corresponding nasal cavity. The incisive foramen transmits terminal parts of the nasopalatine nerve and greater palatine vessels. 2- Greater palatine foramen: one on each side, lies in the posterolateral corner of the hard palate medial to the last molar teeth. It transmits the greater palatine nerve and vessels.
- 67. 3- Lesser palatine nerve: on each side are in the pyramidal process of palatine bone and are located just behind the greater palatine foramen. They provide passage to lesser palatine nerve and vessels. 4- Posterior nasal spine: is a conical projection in the median plane on the sharp free posterior border of the hard palate. 5- Palatine crest, is a curved ridge near the posterior border of the hard palate. 6- Masticatory mucosa: it is the mucous membrane lining the hard palate. The hard palate is lined by keratinized stratified squamous epithelium.
- 69. Arterial supply of the hard palate. This is by greater palatine arteries from the third part of the maxillary artery. Each artery emerges from greater palatine foramen and passes forwards around the palate (lateral to the nerve) to enter the incisive canal and pass up into the nose.
- 71. Venous drainage. The veins of the hard palate drain into pterygoid venous plexus (mainly) and pharyngeal venous plexus. Nerve supply. The hard palate is supplied by greater palatine and nasopalatine nerves derived from pterygopalatine ganglion. Lymphatic drainage. The lymphatics from palate drain mostly into the upper deep cervical lymph nodes and few into retropharyngeal lymph nodes.
- 72. 2- Soft palate. The soft palate is a mobile muscular flap, which hangs down from the posterior border of the hard palate into the pharyngeal cavity. It seperates the nasal cavity from the oral cavity. External features. The soft palate presents the following external features: 1. Anterior (oral) surface is concave and marked by a median raphe. 2. Posterior surface is convex and continuous with the floor of the nasal cavity. 3. Superior border is attached to the posterior border of the hard palate. 4. Inferior border is free and forms the anterior boundary of the pharyngeal isthmus. A conical, small, tongue-like projection hanging down from its middle is called uvula.
- 73. On each side from the base of uvula, two curved folds of mucous membrane extend laterally and downwards: (a) The anterior fold merges inferiorly with the side of the tongue (at the junction of oral and pharyngeal parts) and is known as palatoglossal fold. The palatoglossal fold contains the palatoglossus muscle and forms the lateral boundary of the oropharyngeal isthmus. (b) The posterior fold merges inferiorly with the lateral wall of the pharynx and is known as palatopharyngeal fold. The palatopharyngeal fold contains palatopharyngeus muscle and forms the posterior boundary of the tonsillar fossa.
- 74. Structure. The soft palate is made up of a fold of mucous membrane enclosing five pairs of muscles. The nasal surface of the soft palate is covered by pseudostratified ciliated columnar epithelium except posteriorly (the part that abuts on the Passavant’s ridge of posterior pharyngeal wall), which is lined by non-keratinized stratified squamous epithelium. The oral surface of the soft palate is thicker and lined by non- keratinized stratified squamous epithelium. In the submucosa of both the surfaces are mucous glands, which are in plenty around the uvula and on the oral aspect of the soft palate. The mucosa on the oral surface of the soft palate also contains some taste buds (especially in children) and lymphoid follicles.
- 75. Muscles. The soft palate consists of the five pairs of muscles; 1. Tensor palati (tensor veli palatini). 2. Levator palati (levator veli palatini). 3. Palatoglossus. 4. Palatopharyngeus. 5. Musculus uvulae. All the muscles of soft palate are extrinsic except musculus uvulae, which are intrinsic. See table below.
- 78. Functions. 1. Separates the oropharynx from nasopharynx during swallowing so that food does not enter the nose. 2. Isolates the oral cavity from oropharynx during chewing so that breathing is not affected. 3. Helps to modify the quality of voice, by varying the degree of closure of the pharyngeal isthmus. 4. Protects the damage of nasal mucosa during sneezing, by appropriately dividing and directing the blast of air through both nasal and oral cavities. 5. Prevents the entry of sputum into nose during coughing by directing it into the oral cavity.
- 79. Arterial Supply. The soft palate is supplied by the following arteries: 1. Lesser palatine branches of the maxillary artery. 2. Ascending palatine branch of the facial artery. 3. Palatine branches of the ascending pharyngeal artery. Venous Drainage. The venous blood from palate is drained into pharyngeal venous plexus and pterygoid venous plexus. Lymphatic Drainage. The lymphatics from soft palate drain into retropharyngeal and upper deep cervical lymph nodes.
- 80. Nerve Supply. Motor supply: All the muscles of soft palate are supplied by the cranial root of accessory nerve via pharyngeal plexus except tensor palati, which is supplied by the nerve to medial pterygoid, a branch of the mandibular nerve. Sensory supply: General sensations from palate are carried by: - Lesser palatine nerves to the maxillary division of trigeminal nerve via pterygopalatine ganglion. - Glossopharyngeal nerve.