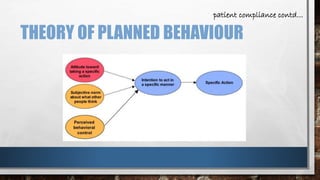
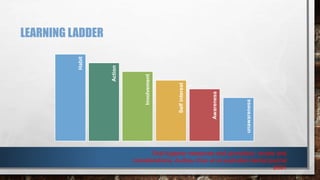
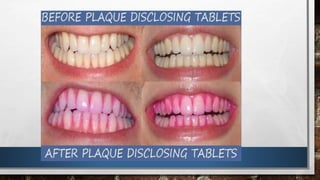
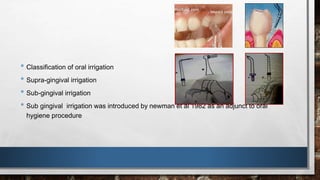
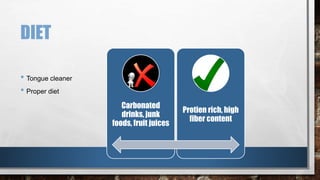
This document provides an overview of oral hygiene and preventive care. It discusses establishing a preventive program through assessing patients, developing intervention plans, implementing clinical services, and evaluating progress. Key aspects include patient counseling, compliance, and motivational interviewing. It also outlines the learning process, individual patient planning, and basic steps for oral hygiene like tooth brushing, flossing, and regular dental checkups.