This document summarizes a study that used intraoral sensors to objectively monitor patient compliance with stabilization splint therapy for myofascial pain. Some key findings:
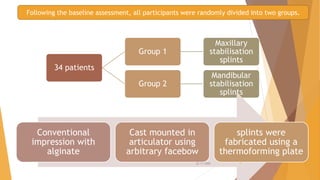
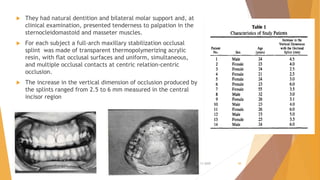
- 32 patients were randomly assigned maxillary or mandibular splints equipped with sensors recording wear time.
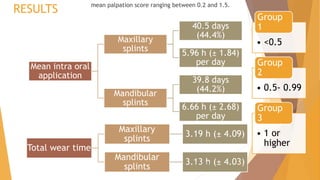
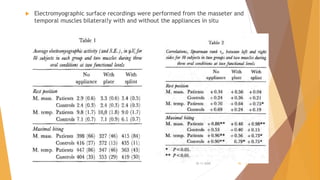
- Overall compliance was 44.4% for maxillary and 44.2% for mandibular splints, with no significant difference between the groups.
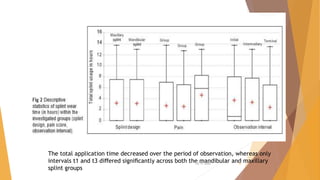
- Patients with greater pain wore their splints significantly more. Wear time decreased over the 3 observation periods as pain reduced with treatment success.
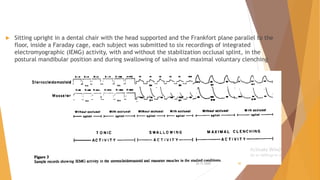
- The study demonstrated intraoral sensors are an effective way to objectively monitor splint wear compared to subjective reports.