Jamie Ranse Outlines Endocrine Organs and Functions
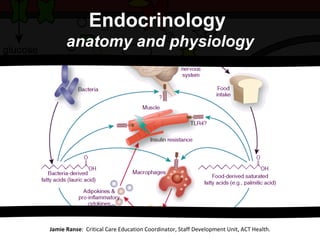
- 1. Jamie Ranse : Critical Care Education Coordinator, Staff Development Unit, ACT Health. Endocrinology anatomy and physiology
- 11. Endocrine organ thyroid and parathyroid
- 16. Summary
- 17. Summary
- 18. Summary
- 19. Jamie Ranse : Critical Care Education Coordinator, Staff Development Unit, ACT Health. Endocrinology anatomy and physiology
Editor's Notes
- Hormones: chemical substances that exert a physiological response on other cells – general hormones are secreted from exocrine glands and are carried though the blood stream to the target cells Neural impulses the dominant system Feedback mechanisms: through the secretion or inhibition of hormones.
- Hormones: chemical substances that exert a physiological response on other cells – general hormones are secreted from exocrine glands and are carried though the blood stream to the target cells
- Gross anatomy: 1cm x 1cm x .5cm, Round, weights .5gram Position: below the hypothalamus – but joined
- http://www.lpch.org/DiseaseHealthInfo/HealthLibrary/diabetes/glossary.html Adenohypophysis – anterior lobe tuberalis – surroundin the stalk distalis – bulk of the anterior lobe Neurohypophysis – posterior lobe neural - infundibular - median – for ms the attachement with the hypothalamus GH: accelerates rate of body growth, particularly growth of bone and muscle. LTH: prolacting – increase milk production TSH thyriod stimulating hormone - a hormone that helps to increase the size, number, and activity of the thyroid cells; stimulates the release of hormones that affect a person's metabolism and that are essential for normal growth and development. ATCH: adrenaline and cortisol ( a hormone secreted by the adrenal cortex which affects metabolism) FSH: sperm production and ovarian follicle growth / LH: Luteinizing hormone - ovulation MSH: skin generation and pigmentation Oxytocin: assists in childbith ADH: hormone secreted by the pituitary gland which helps the body conserve the right amount of water / contraction of smooth muscle in wall of arteries (also called vasopresin).
- Hypersecreting of growth hormone Hypersecretion of ACTH: excess ACTH stimulates excess cortisol, ‘moon face’, excess fat on back and collar bones, ADH deficiency / diabetes insipidus: trauma, tumor, haemrrahge, infarction failure to reabsord water – polyuria, excessive thirst Sudden onset 10L of u/o in 24 hours Treatment w vasopressin TREATMENT Drug Name: Desmopressin (DDAVP) Description: Synthetic analogue of arginine vasopressin with potent antidiuretic, but no vasopressor, activity. Inappropriate ADH secretion Excessive resorption of H2O in the renal system and excessive retention expands fluid volume fluid overload, hyponatremia, heamodilution Casues – malignancy, pulmonary disease, CNS disorders, drugs
- Located in the retroperitanial cavity Falt One pyramid shape One curved Blood from renal arteries or abdominal aorta 3 – 6 grams each Capsule Cortex Medula
- Cortisol Target: general Principle function: metabolism of carbohydrates – stress response Aldosterone Target: renal tubules Function: metabolism of electrolytes and water Adrenaline Target: heart muscle, smooth muscle, arterioles Function: accelerates heart rate, vasoconstriction, contraction of smooth muscle Noradrenaline Target: arterioles Function: art vasoconstriction
- Adrenocortical insufficiency Reduced cortisol (aldosterone) production by the adrenal cortex Causes Adrenal gland destruction Addison’s dx Surgical removal Adrenal infarction Infection Infiltration (eg-tumors) Hemorrhage Secondary Pituitary damage/infarction/hemorrhage Sudden exogenous steroid removal Causes of adrenal insufficiency Hypothalamus destruction Drugs Inhibit steroid production Increase hepatic metabolism Critical illness Adrenal insufficiency Investigation Low baseline cortisol confirms the diagnosis Hyponatremia, hypoglycemia, hypercalcemia, eosinophilia are common but not diagnostic ACTH is high in primary adrenal insufficiency and low in secondary adrenal insufficiency Treatment If in shock, tx the shock condition (fluids/inotropes) High dose corticosteroids b/c baseline cortisol levels are low Tx any infection Tx hypoglycemia with glucose Acute (Addisonian) crises Precipitated by stress in patient’s with unrecognized adrenal insufficiency, following sepsis, or following adrenal hemorrhage Pituitary infarction also presents the same way Apathy, hypoglycemia, hypotension, coma Suspect on all patient’s in shock if the cause is not apparent Chronic deficiency Fatigue, weakness, weight loss, fever, and nausea Hyperpigmentation from excessive melanocyte stimulating hormone production Body hair loss in females from reduced androgen production Adrenocortical excess Cushing’s syndrome (steroid use) and Cushing’s dx (pituitary tumor) increase cortisol levels Moon face, easily bruised skin, HTN, diabetes, osteoporosis, central obesity, and hypokalemia Can also have excess aldosterone secretion with adrenal adenoma
- Thyroid gland Responsible for the metabolic functions Parathyroid gland 4 in number Posterior Small (about the size of a pea)
- Thyroxine Target: general Function: T3 and T4 accelerate the metabolic rate and oxygen consumption of all body tissues Triidothyronine Target: general Function: metabolism of calcium Throcalcitonin Target: skeleton Function: metabolism of calcium Parathormone Target: skeleton, kidney and GI tract Function: metabolism of calcium Throcalcitonin Target: same as for thyroid Function:
- Hyperthyroidism Thyroidtoxicosis; increase in T3 and T4 production Permanent, or temporary, mild or severe 30% - 40% occur in people aged over 60. All metabolic activities are accelerated Goiter Flushed, warm, moist skin Heart – SVT / Atrial arrhythmias GI – increased appetie Dyspnea during activity Hypotyroidism Deficiency of thyroid hormone Recognised as an underdiagnosed condition Fatigue / lethergy Thickness of the face, hands, feet, hoarse voice and thick tounge Hypothyroidism: clinical features CNS: lassitude, apathy, coma, seizures Facial: thin hair, puffy eyes, coarse dry skin, macroglossia Peripheral: hoarse voice, goiter, bradycarida, weight gain, constipation, urinary retention, peripheral edema, bradykinesia, hypoventilation/hypoxia, low voltage EKG, flat T waves, hypoglycemia, hyponatremia Hypothyroidism Management Rewarm patient Support respiratory system Correct hypoglycemia IV thyroxine (T4) Hyperparatyroidism More common then hypoparathyroidism Not well understood Elevated Ca levels Variable S&S and non-specific GI complaints – anorexia, abdo pain, nausea / vominting or constipation Renal calculi Hypoparatyroidism Calcium is not reabsorbed from bones, kidneys or intestines S&S – spasming perpherally then facially Poor muscle contraction – pain Brittle nails, Long Q-T segment on the ecg
- glucosteroids
- stress
- Blood pressure
