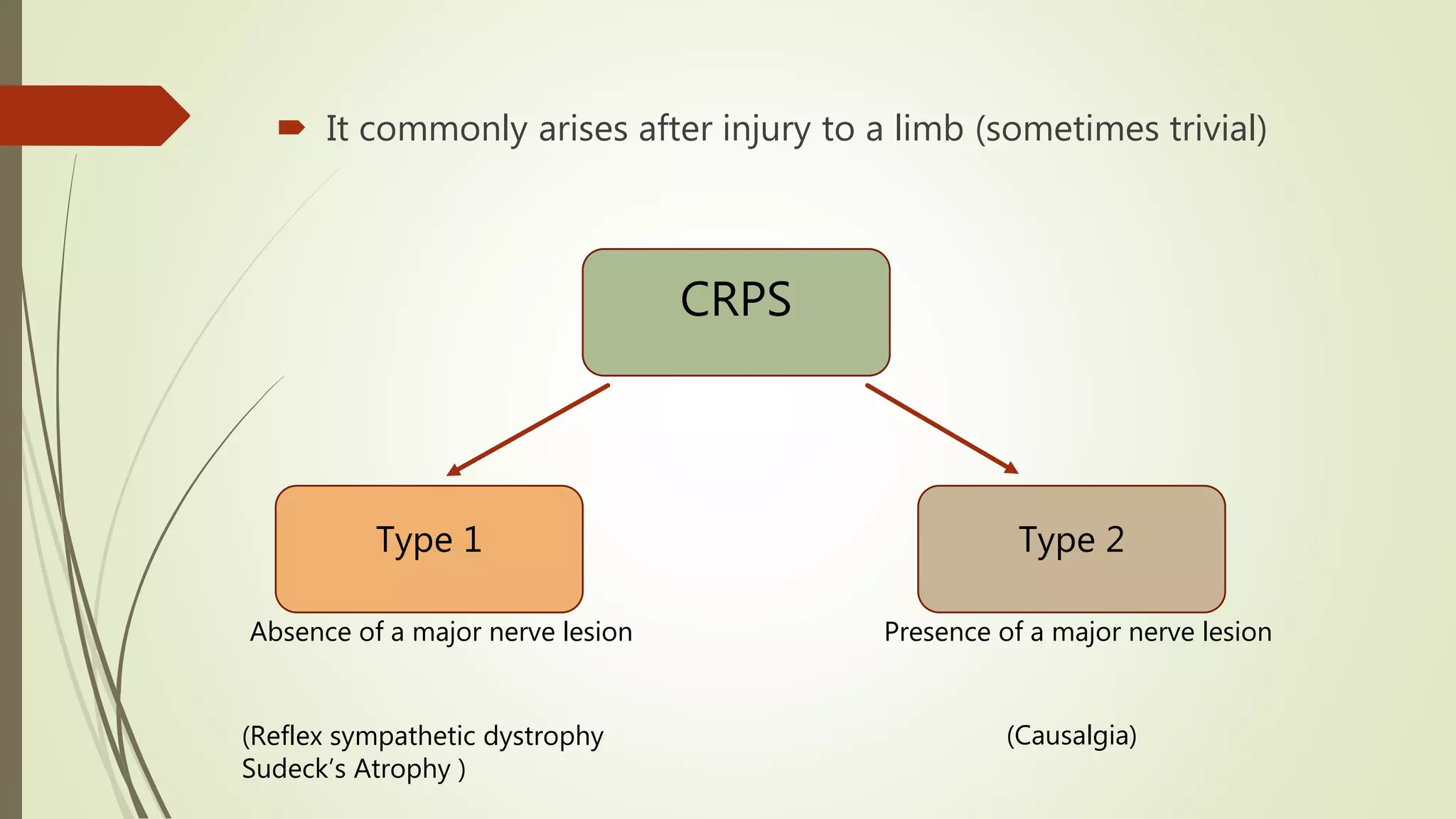
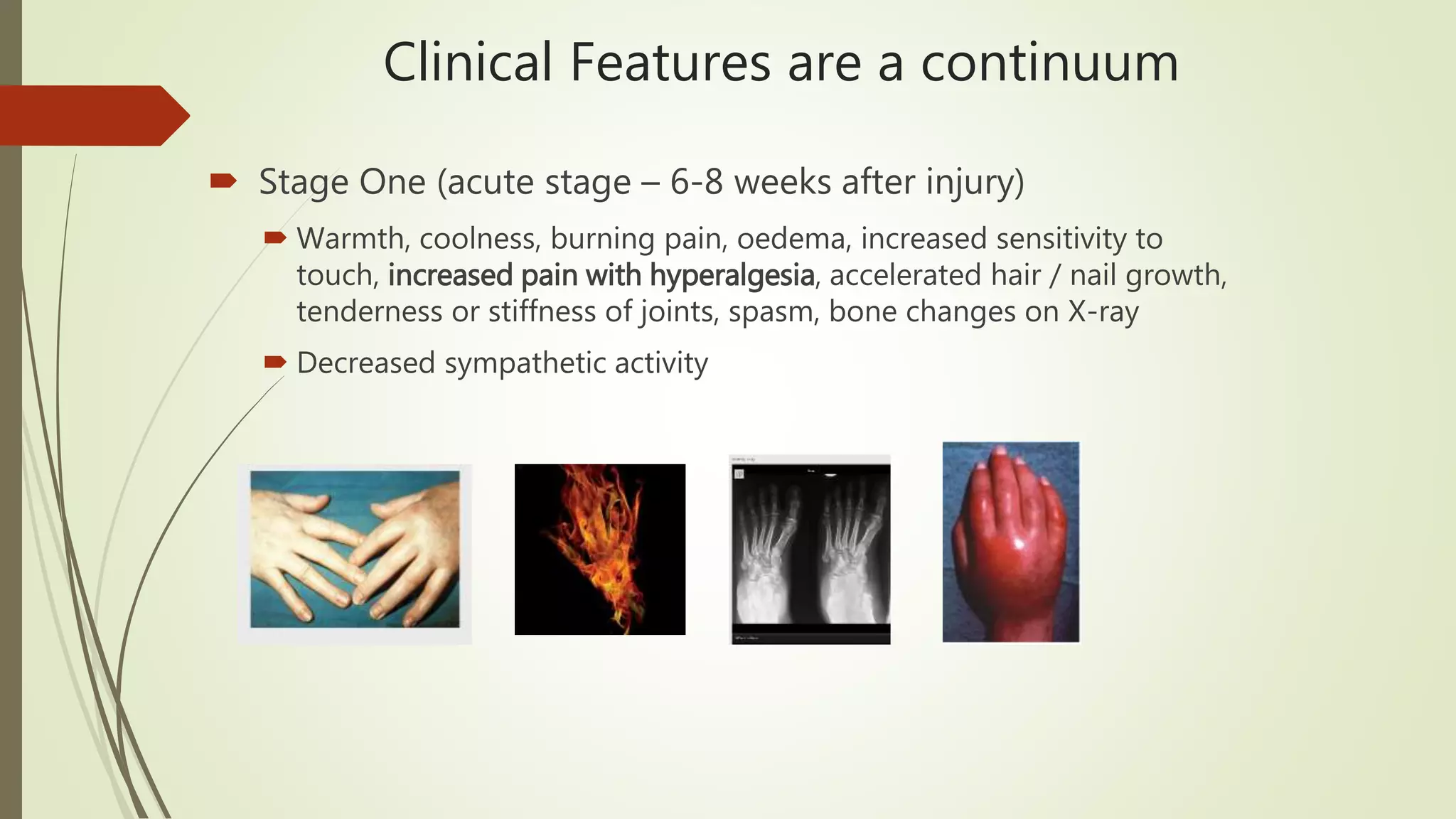
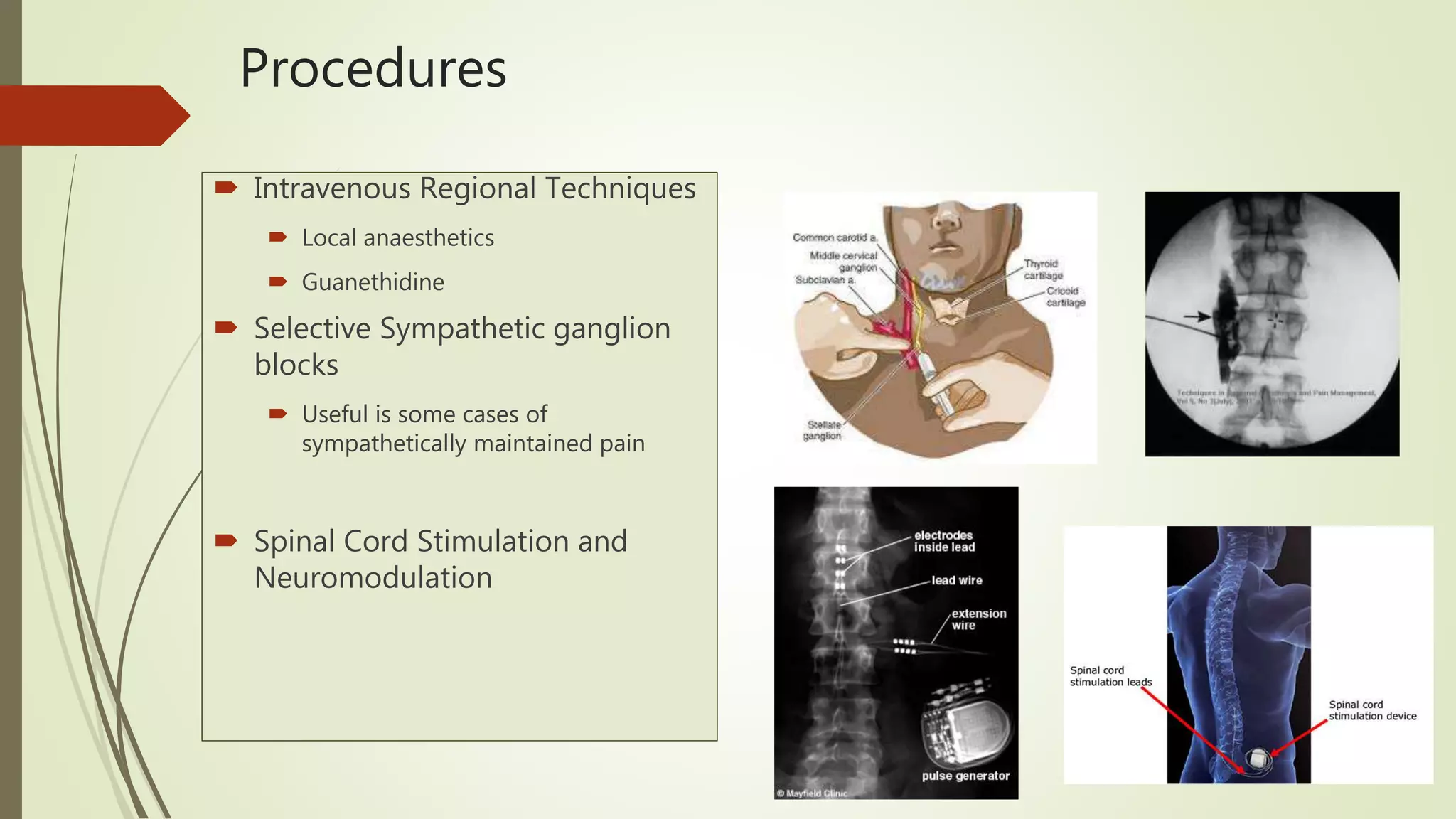
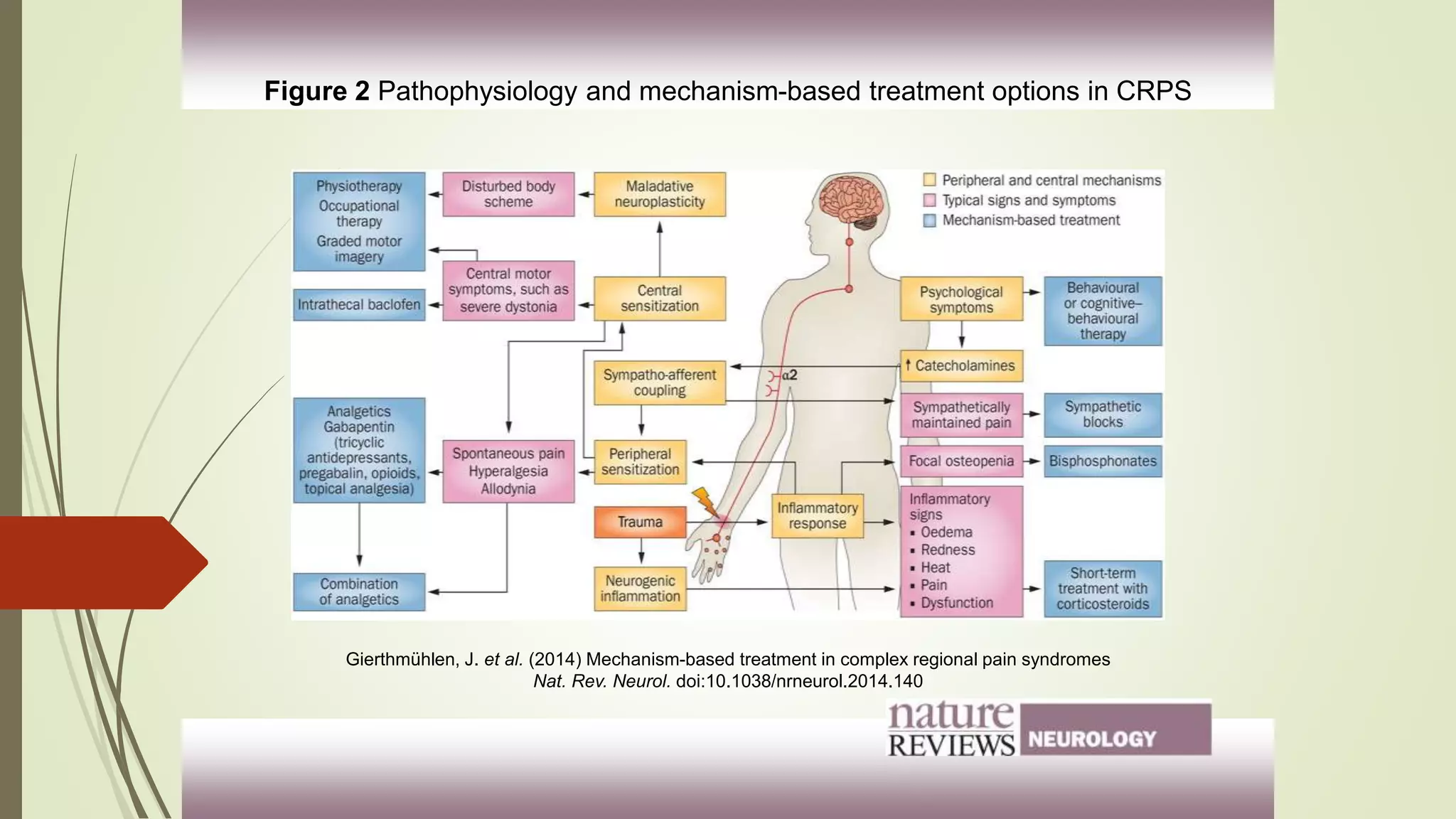
Complex Regional Pain Syndrome (CRPS) is a debilitating painful condition affecting a limb. It is associated with sensory, motor, autonomic, skin and bone abnormalities. The leading symptom is pain, which is often associated with limb dysfunction and psychological distress. CRPS arises after an injury to a limb and is classified into two types depending on whether there is a major nerve lesion present. Management involves a multidisciplinary approach with four pillars - pain relief through medications, procedures, physical and vocational therapy, and psychological therapy. Early diagnosis and treatment are important to help patients.