Athlerosclerosis Cheat Sheet
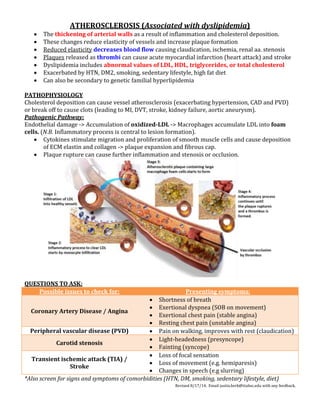
- 1. Revised 8/17/14. Email justin.berk@ttuhsc.edu with any feedback. ATHEROSCLEROSIS (Associated with dyslipidemia) The thickening of arterial walls as a result of inflammation and cholesterol deposition. These changes reduce elasticity of vessels and increase plaque formation Reduced elasticity decreases blood flow causing claudication, ischemia, renal aa. stenosis Plaques released as thrombi can cause acute myocardial infarction (heart attack) and stroke Dyslipidemia includes abnormal values of LDL, HDL, triglycerides, or total cholesterol Exacerbated by HTN, DM2, smoking, sedentary lifestyle, high fat diet Can also be secondary to genetic familial hyperlipidemia PATHOPHYSIOLOGY Cholesterol deposition can cause vessel atherosclerosis (exacerbating hypertension, CAD and PVD) or break off to cause clots (leading to MI, DVT, stroke, kidney failure, aortic aneurysm). Pathogenic Pathway: Endothelial damage -> Accumulation of oxidized-LDL -> Macrophages accumulate LDL into foam cells. (N.B. Inflammatory process is central to lesion formation). Cytokines stimulate migration and proliferation of smooth muscle cells and cause deposition of ECM elastin and collagen -> plaque expansion and fibrous cap. Plaque rupture can cause further inflammation and stenosis or occlusion. QUESTIONS TO ASK: Possible issues to check for: Presenting symptoms: Coronary Artery Disease / Angina Shortness of breath Exertional dyspnea (SOB on movement) Exertional chest pain (stable angina) Resting chest pain (unstable angina) Peripheral vascular disease (PVD) Pain on walking, improves with rest (claudication) Carotid stenosis Light-headedness (presyncope) Fainting (syncope) Transient ischemic attack (TIA) / Stroke Loss of focal sensation Loss of movement (e.g. hemiparesis) Changes in speech (e.g slurring) *Also screen for signs and symptoms of comorbidities (HTN, DM, smoking, sedentary lifestyle, diet)
- 2. Revised 8/17/14. Email justin.berk@ttuhsc.edu with any feedback. PHYSICAL EXAM Xanthomas – deposition of cholesterol in tendons Lung exam - check for pulmonary pathology, S/S of CHF CV exam – check for LVH, peripheral pulses, carotid/abdominal bruits LABS/DIAGNOSTIC TESTS Lipid panel with LDL CMP (AST/ALT) Consider carotid duplex Doppler ultrasound (if concern for TIAs or light-headedness) Ankle-Brachial-Index (ABI) of blood pressures to screen for PVD Hemoglobin A1c (to screen for diabetes) CK (if symptoms of myositis) TREATMENTS (2013 ATP4 Guidelines) DASH Diet rich in fruits, vegetables, whole grains, and low-fat dairy foods. Exercise: 40 minutes /day; 3-4 days / week Smoking cessation Statin medication (No LDL goals, 3 levels of “intensity”) Though some lipid-lowering drugs have been shown to decrease lab values, studies suggest only statins improve clinical outcomes DRUG EFFECT MECHANISM SIDE EFFECTS Fibrates (e.g. gemfibrozil) Lowers triglycerides 5 mechanisms Increased risk of myositis w/ statins Niacin Increases HDL Multiple Flushing & itching from Histamine release / Glucose intolerance / Increased uric acid Cholestyramine Decreases TC Bile acid sequestrant (results in more TC converted to bile) Cramping & Flatus / Can block medication absorption Ezetimibe Lowers LDL Decreases GI cholesterol absorption Well tolerated but no effect on clinical outcomes. Statins (e.g. pravastatin) Reduces LDL + anti- oxidant effect on endothelial lining HMG-CoA Reductase inhibitor (rate-limiting step in chol. synthesis) Elevation of liver enzymes, myositis ATP4 Guidelines for Statin Treatment: Start stains if any of the following: - DM between 40-75 years old - LDL > 190 - 10 year cardiovascular risk (ASCVD score) > 7.5% (found at http://cvdrisk.nhlbi.nih.gov/) Total cholesterol = LDL + HDL + TG* / 5 (Usually TC, HDL, TG are measured. LDL calculated) *only true if TGs <400 mg/dL LDL – carries fat molecules HDL – maintenance of endothelial function / removes fat/cholesterol from cells TG – transfer of fat and glucose – elevated TG can cause pancreatitis
- 3. Revised 8/17/14. Email justin.berk@ttuhsc.edu with any feedback. - Atherosclerotic disease (stroke, heart attacks, regular chest pain, PVD)