Embed presentation

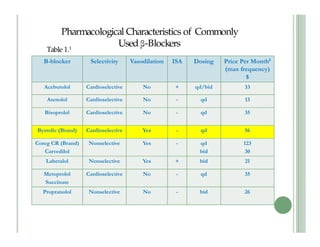





Bystolic (nebivolol) is a cardioselective beta-blocker that offers vasodilatory effects through nitric oxide, making it effective for heart failure, particularly in elderly and African American patients. It has a once-daily dosing schedule, lower side effects compared to other beta-blockers, and does not adversely affect lipid profiles or glycemic control. The medication is associated with good tolerability and can improve compliance in patients who are intolerant to other beta-blockers.






