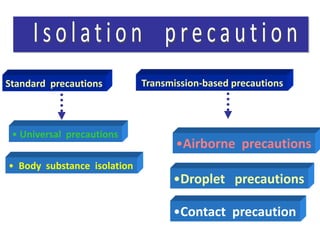
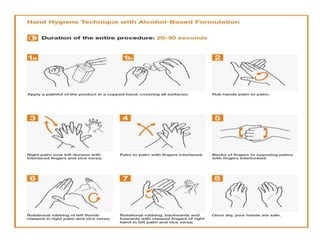
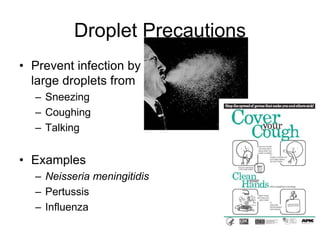
Standard precautions are the basic level of infection control precautions designed to reduce the risk of transmission of pathogens from both recognized and unrecognized sources. They include proper hand hygiene, use of personal protective equipment like gloves and gowns, safe handling of needles and other sharp instruments, respiratory hygiene and cough etiquette, cleaning and disinfection of equipment and the environment, and appropriate handling and disposal of linens and waste. Transmission-based precautions provide additional precautions for patients known or suspected to be infected by epidemiologically important pathogens spread by airborne, droplet, or contact transmission.