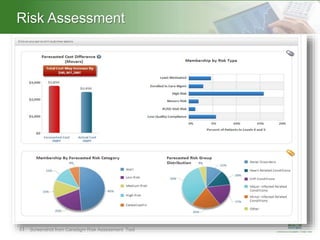
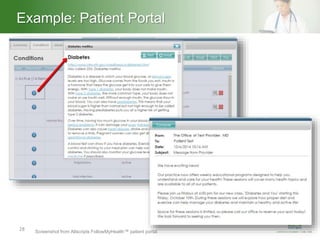
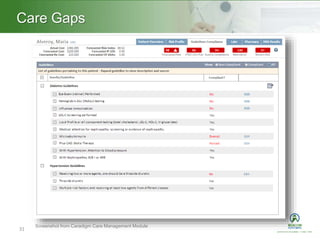
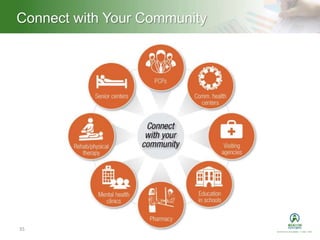
This document summarizes a presentation on population health management. It defines population health management as focusing on keeping patient populations as healthy as possible to reduce costly medical interventions. It identifies key aspects of population health management including defining targeted populations using data, establishing an effective governance structure, using technology to accomplish goals, and integrating care through community partnerships. The document provides examples of how organizations can implement population health management strategies.