Osteomyelitis
•Download as PPTX, PDF•
126 likes•52,733 views
Osteomyelitis
Report
Share
Report
Share
Recommended
More Related Content
Similar to Osteomyelitis
Similar to Osteomyelitis (20)
Chronic Osteomyelitis of bone and marrow cavity.pptx

Chronic Osteomyelitis of bone and marrow cavity.pptx
More from salman habeeb
More from salman habeeb (20)
Recently uploaded
Book Paid Powai Call Girls Mumbai 𖠋 9930245274 𖠋Low Budget Full Independent High Profile Call Girl 24×7
Booking Contact Details
WhatsApp Chat: +91-9930245274
Mumbai Escort Service includes providing maximum physical satisfaction to their clients as well as engaging conversation that keeps your time enjoyable and entertaining. Plus they look fabulously elegant; making an impressionable.
Independent Escorts Mumbai understands the value of confidentiality and discretion - they will go the extra mile to meet your needs. Simply contact them via text messaging or through their online profiles; they'd be more than delighted to accommodate any request or arrange a romantic date or fun-filled night together.
We provide -
Flexibility
Choices and options
Lists of many beauty fantasies
Turn your dream into reality
Perfect companionship
Cheap and convenient
In-call and Out-call services
And many more.
29-04-24 (Smt)Book Paid Powai Call Girls Mumbai 𖠋 9930245274 𖠋Low Budget Full Independent H...

Book Paid Powai Call Girls Mumbai 𖠋 9930245274 𖠋Low Budget Full Independent H...Call Girls in Nagpur High Profile
Recently uploaded (20)
Call Girls Varanasi Just Call 9907093804 Top Class Call Girl Service Available

Call Girls Varanasi Just Call 9907093804 Top Class Call Girl Service Available
Best Rate (Hyderabad) Call Girls Jahanuma ⟟ 8250192130 ⟟ High Class Call Girl...

Best Rate (Hyderabad) Call Girls Jahanuma ⟟ 8250192130 ⟟ High Class Call Girl...
VIP Call Girls Indore Kirti 💚😋 9256729539 🚀 Indore Escorts

VIP Call Girls Indore Kirti 💚😋 9256729539 🚀 Indore Escorts
Call Girls Dehradun Just Call 9907093804 Top Class Call Girl Service Available

Call Girls Dehradun Just Call 9907093804 Top Class Call Girl Service Available
Call Girls Aurangabad Just Call 8250077686 Top Class Call Girl Service Available

Call Girls Aurangabad Just Call 8250077686 Top Class Call Girl Service Available
Premium Bangalore Call Girls Jigani Dail 6378878445 Escort Service For Hot Ma...

Premium Bangalore Call Girls Jigani Dail 6378878445 Escort Service For Hot Ma...
Call Girls Siliguri Just Call 8250077686 Top Class Call Girl Service Available

Call Girls Siliguri Just Call 8250077686 Top Class Call Girl Service Available
Call Girls Horamavu WhatsApp Number 7001035870 Meeting With Bangalore Escorts

Call Girls Horamavu WhatsApp Number 7001035870 Meeting With Bangalore Escorts
The Most Attractive Hyderabad Call Girls Kothapet 𖠋 6297143586 𖠋 Will You Mis...

The Most Attractive Hyderabad Call Girls Kothapet 𖠋 6297143586 𖠋 Will You Mis...
Call Girls Bareilly Just Call 8250077686 Top Class Call Girl Service Available

Call Girls Bareilly Just Call 8250077686 Top Class Call Girl Service Available
Pondicherry Call Girls Book Now 9630942363 Top Class Pondicherry Escort Servi...

Pondicherry Call Girls Book Now 9630942363 Top Class Pondicherry Escort Servi...
Call Girls Jabalpur Just Call 8250077686 Top Class Call Girl Service Available

Call Girls Jabalpur Just Call 8250077686 Top Class Call Girl Service Available
Call Girls Tirupati Just Call 8250077686 Top Class Call Girl Service Available

Call Girls Tirupati Just Call 8250077686 Top Class Call Girl Service Available
Call Girls Gwalior Just Call 8617370543 Top Class Call Girl Service Available

Call Girls Gwalior Just Call 8617370543 Top Class Call Girl Service Available
Call Girls Nagpur Just Call 9907093804 Top Class Call Girl Service Available

Call Girls Nagpur Just Call 9907093804 Top Class Call Girl Service Available
Lucknow Call girls - 8800925952 - 24x7 service with hotel room

Lucknow Call girls - 8800925952 - 24x7 service with hotel room
Book Paid Powai Call Girls Mumbai 𖠋 9930245274 𖠋Low Budget Full Independent H...

Book Paid Powai Call Girls Mumbai 𖠋 9930245274 𖠋Low Budget Full Independent H...
Call Girls Kochi Just Call 8250077686 Top Class Call Girl Service Available

Call Girls Kochi Just Call 8250077686 Top Class Call Girl Service Available
Call Girls Bhubaneswar Just Call 9907093804 Top Class Call Girl Service Avail...

Call Girls Bhubaneswar Just Call 9907093804 Top Class Call Girl Service Avail...
All Time Service Available Call Girls Marine Drive 📳 9820252231 For 18+ VIP C...

All Time Service Available Call Girls Marine Drive 📳 9820252231 For 18+ VIP C...
Osteomyelitis
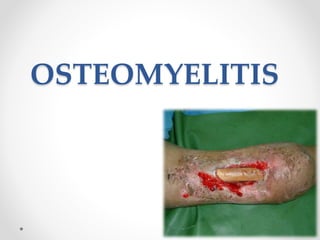
- 2. • Osteomyelitis is a severe infection of the bone, bone marrow and surrounding soft tissue
- 3. ETIOLOGY • Staphylococcus aureus causes 70% to 80% of bone infections. • Proteus , Pseudomonas species and Escherichia coli
- 4. • Bone is normally resistant to infection. However, when microorganisms are introduced into bone can cause osteomyelitis.
- 5. Pathophysiology Entry of microorganism by • Direct • Indirect
- 6. Indirect • Extension of soft tissue infection (eg, infected pressure or vascular ulcer, incisional infection) • Hematogenous (bloodborne) spread from other sites of infection (eg, infected tonsils, infected teeth, upper respiratory infections)
- 7. Direct • Direct bone contamination from bone surgery, open fracture, prosthesis or traumatic injury (eg, RTA )
- 8. Factors affect the extent of infection • Virulence of the infecting organism, • Underlying disease • Immune status of the host, • The type, location, and vascularity of the bone
- 9. • inflammation, increased vascularity, and edema • After 2 or 3 days, thrombosis of the blood vessels occurs in the area, resulting in ischemia with bone necrosis • The infection extends into the medullary cavity and under the periosteum ,cortex and marrow cavity and may spread into adjacent soft tissues and joints
- 11. • Unless the infective process is treated promptly, a bone abscess forms. The resulting abscess cavity contains dead bone tissue (the sequestrum), which does not easily liquefy and drain • New bone growth (the involucrum) forms and surrounds the sequestrum.
- 14. • When bone infection persists for months, the resulting infection is referred to as chronic osteomyelitis
- 16. CLINICAL MANIFESTATIONS • SYSTEMIC- • fever, night sweats, chills,restlessness, nausea and malaise LOCAL- constant bone pain, swelling,t enderness and warmth at the site of infection, drainage from site and restricted movement of affected part
- 17. DIAGNOSIS • History and physical examination • X-ray- Irregular decalcification, bone necrosis are evident • Biopsy, wound culture- to determine the microorganism • Blood investigation- WBC, ESR,blood culture • MRI,CT,radionuclide Bone scan - TO detect the extent of infection
- 19. Management • Goal- control and halt the infection process immobilize the body part to prevent pathological fractures • Warm wet soaks for 20 minutes several times a day may be prescribed to increase circulation
- 20. Pharmacologic management Antibiotic treatment should be based on the identification of pathogens from bone cultures at the time of bone biopsy or debridement. • Commonly used antibiotics clindamycin, rifampin, Linezolid
- 21. Pharmacologic management • IV antibiotic therapy upto 6 weeks • Oral antibiotics upto 3months
- 22. Surgical management • If the patient does not respond to antibiotic therapy, the infected bone is surgically exposed, the purulent and necrotic material is removed, and the area is irrigated with sterile saline solution • A sequestrectomy (removal of enough involucrum to enable the surgeon to remove the sequestrum) is performed
- 23. NURSING MANAGEMENT • Assessment acute onset of signs and symptoms the patient for risk factors history of previous injury, infection, or orthopedic surgery
- 24. Nursing Diagnoses • Acute pain related to inflammatory process secondary to infection as evidenced by guarding, restlessness Intervention • Assess the severity,intensity, characteristics of pain • Provide non pharmacologic pain relief methods • Immobilize and support the body part • Administer analgesics and evaluate the effectiveness of pain control
- 25. • Impaired physical mobility related to pain, immobilization devices and weight bearing devices • Interventions Assist the patient to stand and ambulate specified distance Apply or provide assistive devices Monitor patients use of crutches or other walking aids
- 26. Ineffective therapeutic regimen management related to lack of knowledge regarding long term management of osteomyelitis • Intervention • Demonstrate and teach asceptic techniques and wound care to the patient • Instruct the purpose ,dosage , action of each medication • Instruct the possible adverse effect, consequences of discontinuation of medication
