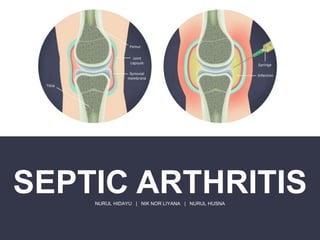
Septic Arthritis
- 1. SEPTIC ARTHRITISNURUL HIDAYU | NIK NOR LIYANA | NURUL HUSNA
- 2. Septic arthritis is an inflammation of synovial membrane with purulent effusion into the joint capsule due to infection. Also referred as infectious arthritis Septic arthritis is a key consideration in adults presenting with acute monoarticular arthritis. Considered as medical emergency Failure to initiate appropriate antibiotic therapy within the first 24 to 48 hours of onset can cause subchondral bone loss and permanent joint dysfunction. It can cause septic shock, which can be fatal. DEFINITION WHAT IS SEPTIC ARTHRITIS?
- 3. ANATOMY SYNOVIAL JOINT Protection of joint cavity Lines joint & cavity and secretes synovial fluid for lubrication Prevents grinding of the bone and allow for smooth articulation
- 4. ANATOMY
- 5. The prevalence of bacterial arthritis as the diagnosis among adults presenting with one or more acutely painful joints has been estimated to range from 8% - 27% All age groups, infants and older adults are most likely to develop septic arthritis. 50% < age 3 M = F The knee is the most commonly affected but any joint may be involved. EPIDEMIOLOGY Infants Hip Children Knee Adults Large joints IVDU Sacrioliac joint
- 6. The infection can originate anywhere in the body. May also begin as the result of an open wound, trauma, surgery, or unsterile injection. Septic arthritis occurs when the infective organism travels through blood stream to the joint. The infection can be caused by bacteria, virus or fungus. AETIOLOGY
- 7. AETIOLOGY
- 8. AETIOLOGY
- 9. AETIOLOGY 1. AGE 2. EXISTING JOINT PROBLEMS 3. MEDICATIONS Age > 80 years old Chronic diseases and conditions that affect the joints — such as osteoarthritis, gout, rheumatoid arthritis or lupus — can increase the risk of septic arthritis, as can an artificial joint, previous joint surgery and joint injury. Taking medications for rheumatoid arthritis. People with rheumatoid arthritis have a further increase in risk because of medications they take that can suppress the immune system, making infections more likely to occur. Diagnosing septic arthritis in people with rheumatoid arthritis is difficult because many of the signs and symptoms are similar. 4. SKIN FRAGILITY Skin that breaks easily and heals poorly can give bacteria access to your body. Skin conditions such as psoriasis and eczema increase your risk of septic arthritis, as do infected skin wounds. People who regularly inject drugs also have a higher risk of infection at the site of injection.
- 10. AETIOLOGY 5. WEAK IMMUNE SYSTEM 6. ALCOLOISM AND IVDU People with a weak immune system are at greater risk of septic arthritis. This includes people with diabetes, kidney and liver problems, and those taking drugs that suppress their immune systems. Having a combination of risk factors puts you at greater risk than having just one risk factor does.
- 11. AETIOLOGY
- 12. PATHOPHYSIOLOGY Hematogenous spread Direct Innoculation Continuous extension from adjacent structure
- 13. PATHOPHYSIOLOGY HEMATOGENOUS SPREAD DIRECT INNOCULATION Most common form of spread, usually affects people with underlying medical problems. May result from penetrating trauma, introduction of organisms during diagnostic and surgical procedures. E.g. intra-articular injection. DIRECT SPREAD FROM ADJACENT BONE More common in children. Osteomyelitis usually begins in the metaphyseal region, from which it breaks through the periosteum into the joint
- 14. PATHOPHYSIOLOGY
- 15. PATHOPHYSIOLOGY
- 17. IN CHILDREN Loss of spontaneous movement of the extremity Irritable Warm Tenderness Rapid pulse Tenderness Refused feeding
- 18. IN CHILDREN
- 19. DIAGNOSIS DIFFERENTIAL DIAGNOSIS 1. Acute osteomyelitis 2. Trauma 3. Hemophilic bleed 4. Rheumatic fever 5. Juvenile rheumatoid arthritis 6. Sickle-cell disease 7. Gaucher’s disease 8. Gout and pseudo-gout
- 20. WHAT IS NEXT? SEPTIC ARTHRITIS SUSPECTED BLOOD AND SYNOVIAL FLUID SAMPLE EMPIRIC PARENTERAL ANTIBIOTICS BASED ON GRAM STAIN JOINT DRAINAGE ADJUST ANTIBIOTICS BASED ON CULTURE AND SENSITIVITY RESULT
- 21. INVESTIGATIONS 1. BLOOD INVESTIGATIONS Raised WCC Raised ESR and CRP Blood culture (positive) 2. IMAGING X-ray Early stage: May look normal except widening of joint space, ultrasound helpful Late stage: Narrowing and irregularity of joint space; may have OM changes of adjacent bones MRI and radionuclide imaging are helpful in diagnosing arthritis in obscure sites such as the sacroiliac and sterno-clavicular joint. 3. SYNOVIAL FLUID ANALYSIS
- 22. FINDINGS
- 24. FINDINGS X-RAY FINDING – WIDENED JOINT SPACE
- 27. INVESTIGATION
- 28. INVESTIGATION
- 29. INVESTIGATION
- 30. INVESTIGATION
- 31. KOCHER CRITERIA Kocker et al in 1999: the presence or absence of the above 4 clinical predictors could be used to accurately predict the likelihood of a septic hip in a child with limp.
- 32. TREATMENT 1st priority – aspirate the joint and examine the fluid General supportive care – analgesics and IV fluid Splintage Antibiotics a. Neonates and infants up to 6 months – penicillin ( flucloxacillin) + 3rd gen cephalosporin b. Children from 6 months to puberty – similar to above. c. Older teenager and adults – flucloxacillin and fusidic acid and 3rd generation cephalosporin Antibiotics given IV for 4-7 days, then orally for 3 weeks.
- 33. ORGANISMS
- 34. COMPLICATIONS 1. Bone destruction and dislocation of the joint (especially hip) 2. Cartilage destruction 3. May lead to either fibrosis or bony ankylosis 4. In adult partial destruction of the joint will result in secondary osteoarthritis 5. Growth disturbance 6. Presenting as either localized deformity or shortening of the bone
Editor's Notes
- Septic arthritis of the sacroiliac joint is a relatively rare disorder, affecting between 1% and 2% of all patients with septic arthritis.
- AETIOLOGY S aureus Most common pathogen in infectious arthritis of both native & prosthetic joints Infections caused by Methicillin-resistant S aureus are usually more aggressive, w/ involvement of >1 joint S epidermidis More common in prosthetic joint infection Streptococci Next to S aureus, most common Gram positive aerobes causing infectious arthritis Group B streptococci is a common cause of infectious arthritis in neonates while S pyogenes & S pneumoniaeare are common pathogens in children ≤ 5 years old who have infectious arthritis Streptococci are important infectious arthritis pathogens in patients w/ serious infections of the genitourinary or gastrointestinal tract Gram-negative bacilli Common etiologic agents of infectious arthritis in intravenous (IV) drug users, elderly & immunocompromised persons Elderly patients frequently have underlying joint diseases & concomitant diseases like diabetes mellitus (DM) & rheumatoid arthritis Disease-modifying drugs used to treat rheumatoid arthritis (eg Infliximab & Etanercept) may predispose patients to the development of infectious arthritis H influenzae was formerly a common pathogen in infectious arthritis in children aged 1 month-5 years but widespread vaccination against the organism has drastically reduced the number of cases P aeruginosa may be a cause of infectious arthritis in IV drugs users, premature infants & patients w/ central vascular catheters N gonorrhoeae Possible etiologic agent in young, healthy, sexually active adults w/ infectious arthritis Incidence frequently related to socioeconomic status Anaerobes More common in patients w/ DM & those w/ prosthetic joint infection Mycobacterial species & fungi Much less common cause of infectious arthritis compared to bacteria Low immune system, recent travel & living in endemic areas are determinants for people susceptible to mycobacterial infections Infectious arthritis caused by these organisms usually presents w/ marked joint swelling, mild signs of acute inflammation & few systemic symptoms Tuberculous infectious arthritis may be more common in low-income groups while other mycobacterial species can cause infectious arthritis in human immunodeficiency virus (HIV)-infected persons Candida arthritis is more common in immunocompromised persons & is associated w/ the presence of a central vascular catheter MIMS MALAYSIA https://specialty.mims.com/infectious%20arthritis/signs%20and%20symptoms?channel=infectious-diseases
- Reference – Mayo Clinic & MIMS Malaysia
