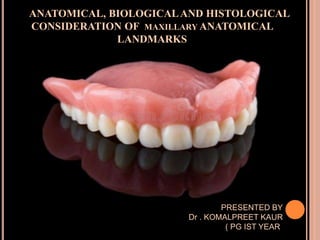
Maxillary landmarks
- 1. ANATOMICAL, BIOLOGICALAND HISTOLOGICAL CONSIDERATION OF MAXILLARY ANATOMICAL LANDMARKS PRESENTED BY Dr . KOMALPREET KAUR ( PG IST YEAR)
- 2. CONTENTS 1. Introduction 2. Osteology 3. Myology 4. Anatomy of supporting structures I. Oral mucous membrane II. Primary stress bearing areas III. Secondary stress bearing areas IV. Relief areas 3. Anatomy of limiting structure 4. REFERENCE
- 3. INTRODUCTION A prosthesis must function in harmony with the tissues that support them and surround them. Dentist must understand the macroscopic and microscopic anatomy of supporting and limiting structures of the denture The denture must extend as far as possible without interfering the health of tissues
- 4. Maxillary denture is supported by two pairs of bone The maxillae And palatine bones
- 5. OSTEOLOGY The osseous structure not only support the dentures, but have a direct bearing on Impression – making procedures , the position of teeth , and the contours of finished denture base.
- 6. There are two maxillae, each consisting of a central body and four processes
- 7. PALATINE PROCESS OF MAXILLA The palatine processes of maxillary bones arises as horizontal plates from the body of maxilla. Two horizontal plates joins in the mid line forming a suture , mid palatal suture The horizontal palatine process of the maxillary bones appear to resist resorption for longer period of time.
- 9. The horizontal plates of palatine bones articulate with the posterior rough border of the horizontal process of maxillae. Posterior border of the horizontal plates of the palatine bones unite at the midline to form a sharp spine called as POSTERIOR NASAL SPINE . It serves as attachment for the aponeurosis of soft palate.
- 10. The POSTERIOR PALTAL SEAL should follow the posterior border of the hard palate:
- 11. ALVEOLAR BONE DEFINITION :The portion of maxilla and mandible that forms and supports the tooth sockets. Based on functional adaptation : 2 types 1. Alveolar bone proper 2. Supporting alveolar bone Based on radiographic experience. 1. Type I 2. Type II
- 12. ALVEOLAR BONE PROPER The bony wall of tooth socket is alveolar bone proper. Compact bone Bundle bone RADIOGRAPHIC APPEARANCE It appears as dense white line called as Lamina dura
- 13. SUPPORTING ALVEOLAR BONE It consists of two parallel plates of cortical bone( buccolingual or labio lingual) Between cortical bone there is spongy bone. The labial and buccal cortical plates are relatively thin, especially over the cuspids and central incisor. ALVEOLAR CREST Formed when inner and outer cortical plates meet.
- 14. o TYPE I : regular interradicular and interdental trabeculae , horizontal in ladder like arrangement o common in mandible.
- 15. TYPE II : irregularly arranged , numerous , delicate ,interdental and interradicular trabeculae . Common in maxilla
- 16. PTERYGOID HAMULUS Although does not provide support for maxillary denture, its position is in osseous limits of the maxillary denture base It is thin , curved process at the terminal end of medial pterygoid plate of sphenoid bone.
- 17. It has two important relations , related to its function 1. Tensor veli palatine tendon passes immediately behind it. 2. Superior attachment of the pterygomandibular raphe
- 18. ZYGOMATIC PROCESS Distal to buccal frenum lies the root of zygoma , which is located opposite the first molar region With increase in resorption of ridge , it becomes more noticeable Relief is indicated.
- 19. MYOLOGY MUSCLES OF FACIAL EXPRESSION These muscles lies superficially under the skin the action of these muscles is responsible for the facial postures associated with smiling , laughing or frowning .
- 20. ORIGINS The origins of several of the muscles of facial expression are near enough to the denture-bearing areas that their actions must be considered as definitely influencing the denture borders. their influence is in proportion to the contour and quantity of residual ridge present in a vertical direction. The higher the residual ridge the less influence will be exerted.
- 21. INSERTION Bundles of muscles insert partly into the skin , partly into the mucous membrane of the lips and the immediate vicinity. Area situated laterally and slightly above the corner of mouth is the concentration of many fibers of this muscle group , this area is called MODIOLOUS The labial flanges of the maxillary denture frequently need to be reduced lateromedially in the area of the modiolus .
- 22. Can be studied under following groups Orbital: occipito frontalis, orbicularis oculi, corrugator supercilli Nasal: nasalis , procerus , depressor septi nasii Oral: orbicularis oris, levator anguli ori, depressor anguli oris,risorus, mentalis , buccinator , levator labii superiorus , depressor labii inferiorus , zygomaticus major , zygomaticus minor
- 23. ORBICULARIS ORIS ORIGIN Tissue surrounding lips INSERTION Underneath skin at corner of mouth. FUNCTIONS Closes the mouth Purses and protrudes the lip.
- 24. We use this muscle when we whistle or blow
- 25. BUCCINATOR ORIGIN Alveolar process of maxilla and mandible. Pterygoid hamulus and pterygomandibular raphe INSERTION In the fibres of orbicularis oris FUNCTIONS: Prevents the build up of food between cheeks and teeth. Aids in forcefull expulsion of air from mouth.
- 27. LEVATOR LABI SUPERIORUS ORIGIN Infra -orbital margin INSERTION Skin and muscle of upper lip FUNCTIONS Elevates the upper lip
- 28. ZYGMATICUS MINOR It is one of our smiling muscles. FUNCTIONS Pull the corner of mouth upwards and outwards .
- 29. ZYGOMATICUS MAJOR ORIGIN Zygomatic bone INSERTION Underneath skin at corner of mouth FUNCTIONS Draws the corner of mouth upwards and outwards.
- 30. LEVATOR ANGULI ORIS Deep to zygomaticus major there is levator anguli oris muscle ORIGIN Anterior surface of maxilla Below infra orbital foramen INSERTION modiolous FUNCTIONS Lifts the corner of mouth.
- 31. RISORIOUS Gets its name from latin “risus” which means laughter. ORIGIN Fascia surrounding parotid salivary gland INSERTION Angle of mouth FUNCTIONS Retracts the angle of mouth
- 32. DEPRESSOR ANGULI ORIS ORIGIN Anterolateral surface of body. INSERTION Angle of mouth. FUNCTION Antagonizes levator anguli oris pulls the corner of mouth downwards.
- 33. DEPRESSOR LABII INFERIORIS ORIGIN Mandible between the anterior midline and the mental foramen. INSERTION Skin of lower lip FUNCTIONS Pulls the lower lip downwards and outwards
- 34. MENTALIS ORIGIN Incisive fossa of mandible. INSERTION Skin of chin. FUNCTIONS Lifts and protrude lower lip
- 35. SIGNIFICANCE If these are not properly supported , either by natural or artificial dentition , none of the facial expression appear normal. The nasolabial sulcus , the philtrum , the commissure of lips, and mentolabial sulcus will not have their normal contour. Incorrectly contoured denture base or incorrectly positioned teeth will destroy the normal tonicity of the muscles. Lack of support leads to sagging, stretching : retards the normal contracture of muscles and results in loss of tonicity
- 36. MUSCLES OF SOFT PALATE Levator veli palatine Tensor veli palatine Glossopalatinus palatoglossus palatopharyngeus
- 38. LEVATOR VELI PALATINI Origin petrous part of temporal bone inferior aspect of auditory tube Insertion upper surface of palatal aponeurosis action elevates the soft palate
- 39. TENSOR VELI PALATINI Origin Lateral side of auditory tube Scaphoid fossa of sphenoid bone Insertion Palatine aponeurosis Action Tightens the soft palate Opens the auditory tube
- 40. PALATOPHARYNGEUS The wall of soft palte is formed principally by this muscle. Origin Superior surface of palatine aponeurosis Insertion Pharyngeal wall Action Depress the soft palate Elevates pharynx
- 41. PALATOGLOSSUS Origin Inferior surface of palatine aponeurosis Insertion Lateral margin of tongue. Action Depress palate Moves palatoglossus arch toward midline Elevates back of tongue.
- 42. MUSCULUS UVULAE Origin Posterior nasal spine of hard palate Insertion Connective tissue uvulae Action Elevates and retract uvula Thickens central of region of soft palate.
- 43. WHAT IS THE ANATOMICAL LANDMARK? Anatomical Landmark is a recognizable anatomic structure used as a point of reference. [GPT-9] They acts as positive guides to the limits of the impression
- 44. Impression surface of a denture is comprised of stress bearing areas/supporting areas Relief areas Peripheral or limiting areas
- 45. ANATOMY OF SUPPORTING STRUCTURES Foundation of denture is made up of bone of the hard palate and residual ridge ,covered by mucous membrane. The denture base rests on mucous membrane ,which serves as a cushion between the base and supporting bone.
- 46. MUCOUS MEMBRANE The mucous membrane is composed of Mucosa Sub –mucosa(it makes the bulk of mucous membrane)
- 48. MUCOSA Mucosa is formed by stratified squamous epithelium, which often is keratinized subjacent narrow layer of connective tissue is known as lamina propria. It exhibits regional modifications to suit the functional needs of specific area It can be classified as( based on function) 1. Masticatory mucosa 2. Lining / reflecting mucosa 3. Specialized mucosa
- 49. MASTICATORY MUCOSA: it is characterized by well defined keratinized layer on its outermost surface. In edentulous patient the mucosa covering the hard palate , and the crest of residual alveolar ridge ,including the residual attached gingiva
- 50. LINING OR REFLECTING MUCOSA: o Formed by non keratinized epithelium. o And thin layer of connective tissue, the lamina propria. o It covers lips , cheeks, labial & buccal mucosa, vestibular fornix, slopes of residual ridge, ventral surface of tongue, floor of mouth and soft palate
- 51. SPECIALIZED MUCOSA o It is keratinized. o Covers the dorsal surface of tongue , taste buds.
- 52. SUBMUCOSA Submucosa is formed of connective tissue that varies in character from dense to loose areolar tissue and also varies considerably in thickness. It may contain glandular, fat , or muscle cells and transmits the blood and nerve supply to mucosa. The thickness and consistency of sub mucosa are largely responsible for the support that the mucous membrane affords a denture.
- 53. In healthy mouth, submucosa is attached to the periosteum of underlying bone and will usually successfully bears the pressures of the denture. When submucosa is thin , the soft tissues will be non resilient , and the mucous membrane will get traumatized easily. When it loosely attached to periosteum , or it is inflamed or edematous , the tissue is easily displaceable , and the stability and support of the denture are adversely affected.
- 54. STRESS BEARING AREAS These are load bearing areas Denture should be made such that most of the load is concentrated on these areas PRIMARY STRESS BEARING AREAS The horizontal portion of hard palate lateral to the midline Maxillary tuberosities SECONDARY STRESS BEARING AREAS Residual alveolar ridge Rugae *bouchers 13 edition
- 55. HARD PALATE The ultimate support for a maxillary denture is Bone of two maxillae and the palatine bone
- 56. HISTOLOGY Epithelium is keratinized throughout Mucous membrane is tightly fixed to the underlying periosteum and therefore immovable Lamina propria ( a layer of dense CT) is thick in anterior part and thin in posterior region) Submucosa: it is different in various regions
- 57. Anterolateral portion With abundant adipose tissue Posterolateral portion With abundant gland tissue Although this tissue is displaceable it contribute to support
- 58. Primary support : horizontal portion of hard palate lateral to mid line
- 59. MAXILLARY TUBEROSITY The maxillary tuberosity is the most posterior part of the alveolar ridge lies distal to the position of the last molar
- 60. o The posterior part of the tuberosity rarely resorbs and it covered with dense connective tissue o SIGNIFICANCE denture base should cover the maxillary tuberosity and fill the hamular notches . The last posterior tooth should not be placed on tuberosity.
- 61. CLINICAL SIGNIFICANCE The enlarged tuberosities limits the space and will interfere the occlusal plane and distal extension of lower denture. Surgical reduction should be done
- 62. RUGAE They are folds of irregular mucous membrane extends bilaterally from midline in the region of upper 6 anteriors and sometime bicuspid In the area of rugae palate is set to an angle with residual ridge . Resist the anterior displacement of the denture
- 63. RESIDUAL RIDGE DEFINITION The portion of the alveolar ridge and its soft tissue covering which remains following the removal of teeth- GPT
- 64. The mucous membrane covering the crest of ridge in a healthy mouth is firmly attached to the periosteum of bone Submucosa is characterized by dense collagenous fibres that are contiguous with the lamina propria and provides adequate resiliency to support of denture . provides good support , however bone is subject to resorption, which limits its potential for support , unlike palate which is resistant to resorption
- 65. SLOPES OD RESIDUAL ALVEOLAR RIDGE As the mucous membrane extends from the crest along the slope of residual ridge, It loses its firm attachment to underlying bone. Epithelium is non keratinized or slightly keratinized Submucosa contains loose connective tissue and elastic fibres. This loosely attached tissue cannot withstand the forces of mastication.
- 66. RELIEF AREAS Mid palatine raphe It is the junction between two palatine processes of maxilla
- 67. submucosa is extremely thin Mucosa is in close contact with the bone
- 68. CLINICAL SIGNIFICANCE Little or no stress can be placed in this region during the making of the final impression or in the completed denture. Otherwise, the denture will tend to rock over the centre of the palate when vertical forces are applied to the teeth.
- 69. INCISIVE PAPILLA It is a small tubercle overlies incisive foramen Situated on a line immediately behind and between central incisors. Nasopalatine nerve and vessels pass through it at right angle to the bony foramen . As resorption progresses, it comes to lie nearer the crest of ridge
- 70. Anterior border and center of incisive papilla are likely to change after extraction of incisor teeth the posterior border is relatively stable . Papilla becomes round after extraction of incisor teeth due to changes in the anterior border.
- 71. Gives positional relation to central incisor which are 8-10 mm anterior to the CENTRE incisive papilla.
- 72. Beside this, canine–papilla line is a useful guide to orient the upper canine teeth in complete dentures a perpendicular is drawn posterior to centre of incisive papilla to saggital plane passes through canine.
- 73. CLINICAL SIGNFICANCE pressure should not be applied on this when final impression is made Pressure obliteration of vessels/compression nerves deprive of nutrition necrosis and paraesthesia of anterior palate
- 74. FOVEA PALATINI Several ducts of mucous glands coalesce to form fovea This acts an arbitrary guide to locate the posterior border of denture. Denture can extend 1-2 mm beyond this Secretion from this spreads as a thin film on denture which aids in retention It should be relieved in a patient with thick ropy saliva.
- 76. TORUS PALATINUS This is a hard bony enlargement that occurs in midline of the roof of the mouth Found in about 20% of population. FEMALE : MALE RATION 2:1
- 77. CLINICAL SIGNIFICANCE Relief is indicated for less extensive tori, and surgical removal for more extensive tori. Removed when it has undercuts , if impedes the normal movement of tongue , or if act as fulcrum.
- 78. ANATOMY OF LIMITING STRUCTURES Limiting structures: To determine and confine the extent of denture: 1. Labial frenum 2. Labial vestibule 3. Buccal frenum 4. Buccal vestibule 5. Hamular notch 6. Vibrating line
- 79. LABIAL FRENUM The upper medial labial frenum, or frenulum, is a fold of mucous membrane that overlies loose connective tissue . It contains no muscle fibers and insert in a vertical direction It anchors the upper lip to the gingiva. The frenum can vary in size Can be single or multiple In many edentulous patients, resorption of the alveolar bone brings the crest of the alveolar ridge closer to the frenum.
- 80. CLINICAL CONSIDERATION • Lip should be streched horizontally outwards for proper recording of frenum
- 81. The labial notch must be wide and deep enough to allow the frenum to pass through the lips without the manipulation of the lip
- 82. When it is abnormally large, it extends to the interdental papilla between the two central incisors. An enlarged upper median labial frenum is frequently found in association with a diastema .
- 83. LABIAL VESTIBULE Definition The portion of the oral cavity that is bounded on one side by teeth , gingiva, and alveolar ridge(in edentulous mouth , residual ridge) and on other by lips anterior to buccal frenum. GPT8 Main , muscle of lip which forms the outer surface of vestibule is orbicularis oris Its tone depends on the support given by labial denture flange and position of teeth
- 84. HISTOLOGY The mucous membrane lining the vestibule is thin with an epithelium that is non keratinized (lining mucosa) Submucosal layer is thick and contains large amount of loose areolar tissue and elastic fibres.
- 85. FORNIX The fornix of the vestibule is the site where the mucous membrane lining of the lips and cheeks reflects and joins the unattached gingiva, or alveolar mucosa. The depth of the vestibule in the upper and lower jaws is determined by the site of the fornix.
- 86. if while taking an upper impression, the lips are pulled vertically instead of horizontally artificially increase the depth of the vestibule the denture will extend into the subcutaneous space irritation of the mucosa / alteration of the facial appearance.
- 87. Following extraction of teeth, alveolar bone undergoes resorption and therefore the depth of the vestibule become shallower. Surgical creation of a new fornix is required.
- 88. BUCCAL FRENUM The buccal frenum is a band of tissue that overlies the levator anguli oris muscle. It is sometime single fold of mucous membrane , sometime double and sometime broad and fan shaped Buccal frenum is part of continuous band of tissue going from maxilla through the modiolous in the corner of the mouth to the buccal frenum on the mandible .
- 89. It has attachment of following muscles • Levator anguli oris: affects the position of frenum • Orbicularis oris: pulls the frenum forwards • Buccinator: pulls frenum in backward
- 90. CLINICAL SIGNIFICANCE For the proper action of these muscles , proper clearance should be provided in the denture Inadequate provision can cause dislodgement
- 91. Cheek is elevated and then pulled outward, downward, and inward and moved backward and forward to simulate movement of frenum
- 92. BUCCAL VESTIBULE The buccal vestibule lies opposite the tuberosity extends from the buccal frenum to hamular notch the size of buccal vestibule varies with the 1. contraction of buccinator muscle , 2. the position of mandible, and the 3. amount of bone lost from of the maxilla
- 93. The size and the shape of the distal end of buccal flange must be adjusted to accommodate ramus ,coronoid process and masseter muscle in function When mandible is wide opened and moved laterally, the width and height of this area is reduced. When masseter muscle contracts under heavy closing prrssures it also reduces this space
- 94. CORONO-MAXILLARY SPACE The corono-maxillary space is that anatomic region that lies medial to coronoid process ,lateral to maxillary tuberosity and bounded anteriorly by base of zygomatic process and posteriorly by pterygo-maxillary / hamular notch.
- 95. Two types of individual anatomical variations can affect the size of this space: With vertical variations, the space increases or does not vary when the mouth is opened; therefore, the prosthesis border must be thicker to obtain adequate retention. With lateral variations, the corono maxillary space is reduced when the mouth is opened; therefore, the prosthesis border must be thin.
- 97. The use of a mouth mirror provides adequate information about the height of this space
- 98. a diagnostic technique—a space impression tool— has been proposed to clinically delineate the type of space present and to help visualize dimensions. This technique consists of the use of a modified tongue blade that, in conjunction with low-fusing impression compound
- 99. If the coronomaxillary space broadens or maintains its size when the mouth is opened it is advisable not to have the patient open the mouth wide, to protrude to move laterally during border molding or impression procedures. A gentle molding of the region by pulling the cheek out, down, and in will yield more successful results.
- 100. For the patients, where opening the mandible can result in narrowing of the space Border molding procedures in this region should include opening and closing together with protrusion and lateral movements of the jaw.
- 101. HAMULAR NOTCH Lying between maxillary tuberosity and pterygoid hamulus is a groove called the hamular notch. distolateral border of denture should rest in hamular notch it is the soft area of loose areolar tissue , so can be displaced to achieve the posterior palatal seal it is located by T-shaped burnisher or mouth mirror
- 102. CLINICAL SIGNIFICANCE Over extension can cause soreness due to pressure on hamular process and interference of pterygomandibular raphe If under extended or rest on tuberosity it will lost retentive properties as the tissue there is non resilient and border seal could not be achieved
- 103. POSTERIOR PALATAL SEAL It is defined as “ the soft tissues along the junction of the hard and soft palates on which pressure within the physiologic limits of the tissues can be applied by a denture to aid in the retention of the denture.” GPT
- 104. RELEVANCE At the posterior aspect of the denture there is no cheek tissue to seal the denture border , therefore provide optimum retention. Horizontal forces and lateral torqueing of maxillary denture can only be resisted by adequate border seal Terminating the denture borders at soft tissue will allow the mucosa to move with the denture base during function and thereby maintaining denture seal .
- 105. FUNCTIONS Primary purpose is retention of maxillary denture Maintains contact with the anterior portion of the soft palate the seal prevents passage of air between the denture and the tissues .. Reduces the patient awareness to this area and also subsequent reduction in area in gag reflex. Reduces the food accumulation beneath the posterior aspect of denture.
- 106. Reduces the patient discomfort Compensate for the volumetric shrinkage Creates a partial vacuum that only gets activated when horizontal and tipping forces are directed against the denture base
- 107. The range of the soft palate movement and the degree of displaceability of seal area differ in every individual House classification: (based on the angle that soft palate makes with the hard palate and the soft palate muscle activity that is essential to establish velo phayngeal) closure Class I Class ii Class iii
- 108. •In class I, the soft palate is horizontal as it extends It extends posteriorly, requiring minimal muscular activity for velopharyngeal closure Allows more than 5 mm of seal area
- 109. Class II type of soft palatal contour lie somewhere between class I and class III classes allows 1 to 5 mm of seal area
- 110. In class III, the soft palate is more acute in relation to the hard palate necessitating marked elevation of the musculature for velopharyngeal closure permits a narrow seal of less than 1 mm
- 111. The posterior palatal seal is divided into two. The postpalatal seal extends medially from one tuberosity to the other. Laterally, the pterygomaxillary seal extends through hamular notch continuing for 3 to 4 mm anterolaterally approximating the mucogingival junction
- 112. SIGNIFICANCE Notch is covered by pterygomandibular fold, which extends from the posterior aspect of the tuberosity posterior – inferiorly to insert into retromolar pad. The fold of tissue can influence the posterior border seal if the mouth is in a wide open position during the final impression procedure..
- 113. VIBRATING LINES Anterior vibrating line is an imaginary line located at the junction of the attached tissues overlying the hard palate and movable tissues of the immediately adjacent soft palate. This should not be confused with the junction of soft and hard palate. It is always present on soft palate.
- 114. How to locate anterior vibrating line? Ask the patient to perform valsalva maneuver , which requires both nostrils be held firmly while patient blows gently from nose. And can be visualized by instructing the patient to say “ah” with short vigorous burst.
- 116. Posterior vibrating line is an imaginary line at the junction of aponeurosis of tensor veli palatine and muscular portion of soft palate. It marks the most distal extension of denture base. How to locate posterior vibrating line? It can visualized by instructing the patient to say “ah” in short burst in normal , un – exaggerated fashion.
- 117. Patient position during impression making of palatal seal area this region should be recorded in function. Therefore, an impression should be made when the patient is seated in upright position with head flexed 30 degree forward, below FH plane to allow the soft palate to reach its functionally depressed position. The patients tongue should be placed under tension against either the handle of the impression tray or the dentist's finger .
- 118. REFERENCE BOUCHER’ S Prosthodontic treatment of edentulous patients (9th ,11th and 12th edition 13th edition SHELDON WINKLER essentials of complete denture prosthodontics(2nd edition) CHARLES M HEARTWELL syllabus of complete denture (4th edition) ORBAN’S oral histology and embryology(14th edition) ARTHUR O RAHN textbook of complete denture(6th edition) Coronomaxillary space and its significance in complete denture retention-Case reportsJuly 2012General Dentistry 60(4):e263- 7SourcePubMed doi: 10.1007/s13191-012-0169-yThe Incisive Papilla: A Significant Landmark in ProsthodonticsE. G. R. Solomon1 and K. S. Arunachalam2 https://www.ijoprd.com/doi/IJOPRD/pdf/10.5005/jp-journals- 10019-1020 posterior palatal seal a literture review