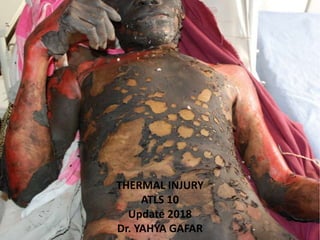
Burn injuries
- 1. THERMAL INJURIES THERMAL INJURY ATLS 10 Update 2018 Dr. YAHYA GAFAR
- 2. INTRODUCTION The most significant difference between burns and other injuries is that the consequences of burn injury are directly linked to the extent of the inflammatory response to the injury.
- 3. PRIMARY SURVEY AND RESUSCITATION Stopping the burning process, ensuring that airway and ventilation are adequate, and managing circulation are lifesaving measures
- 4. Remove clothing, do not peel off. Brush any dry chemical powders. Rinsing & irrigate with warm saline. Cover the patient ,prevent hypothermia. Stop Burning Process
- 5. ESTABLISH AIRWAY CONTROL The airway can become obstructed not only from direct injury (e.g., inhalation injury) but also from the massive edema resulting from the burn injury.
- 6. ABLS Indications For early intubation. - Signs of airway obstruction . - BSA > 40%–50%. - Extensive and deep facial or mouth burns. - Significant edema or risk for edema. - Signs of respiratory compromise. - Decreased level of consciousnes. - Difficulty swallowing. - Anticipated patient transfer without qualified personnel to intubate en route.
- 7. PITFALL Airway obstruction in a patient with burn injury may not be present immediately. - Recognize smoke inhalation. - Evaluate the patient for circumferential burns of the neck and chest. -May require bronchoscopy place an adequately sized Airway.
- 8. ENSURE ADEQUATE VENTILATION Direct thermal injury to the lower airway is very rare and essentially occurs only after exposure to superheated steam or ignition of inhaled flammable gases.
- 11. CO TREATMENT any patient in whom CO exposure could have occurred should receive high-flow (100%) oxygen via a non-rebreathing mask.
- 12. SIZE OF ETT Efforts should be made to use endotracheal tubes at least 7.5 mm ID or larger in an adult and size 4.5 mm ID ETT in a child.
- 13. USE OF PULSE OXIMETRY Pulse oximetry cannot be relied on to rule out carbon monoxide poisoning, as most oximeters cannot distinguish oxyhemoglobin from carboxyhemoglobin.
- 14. ROLE OF HYPERBARIC OXYGEN There is no role for hyperbaric oxygen therapy in the primary resuscitation of a patient with critical burn injury.
- 15. DIAGNOSIS OF SMOKE INHALATION exposure to a combustible agent Signs the lower airway, below the vocal cords, seen on bronchoscopy Smoke inhalation (ABLS)
- 16. SMOKE INHALATION (WORKUP) normal CXR & ABG on admission do not exclude inhalation injury.
- 17. SMOKE INHALATION TREATMENT SUPPORTIVE Intubation Head elevation 30 d Escharotomy.
- 18. MANAGE CIRCULATION WITH BURN SHOCK RESUSCITATION Burn resuscitation is required to replace the ongoing losses from capillary leak due to inflammation.
- 19. WHEN TO START? Resuscitation fluids for deep partial and full- thickness burns larger than 20% TBSA, taking care not to over-resuscitate.
- 20. I.V ACCESS If the extent of the burn precludes placing the catheter through unburned skin, place the IV through the burned skin into an accessible vein. • Lower& upper limb? • Number? • Size?
- 21. WHICH FLUID?? Warmed isotonic crystalloid solution, preferably lactated Ringer’s solution.
- 22. INITIAL FLUID RATE?? 2 ml of lactated Ringer’s x patient’s body weight in kg x % TBSA for second- and third- degree burns. • ½ over the first 8 h
- 23. For pediatric 3 mL/kg/% TBSA If < 30 kg, should receive maintenance fluids of D5LR
- 24. PITFALL - Remember that edema takes time to develop. - Use long IV catheters. - Do not cut endotracheal tubes, and regularly assess their position. Intravenous catheters and endotracheal tubes can become dislodged after resuscitation.
- 25. HOW TO MONITER? Urine output (30 and 50 cc/hr).
- 26. PATIENT ASSESSMENT ASSESSMENT AMPLE history Allergies. Medication. PMH. Last meal. Event. TBSA DEPTH OF THE BURN
- 27. THE ADULT BODY The palmar surface (including the fingers) of the patient’s hand represents approximately 1% of the patient’s body surface 4.5% 18% 4.5% 4.5% 9% 9% 4.5% 1% 18% 9%9% 4.5% 4.5%
- 29. PITFALL Overestimating or underestimating burn size - Do not include superficial burns. - Use the rule of nines. - For irregular or oddly sized burns, use the patient’s palm. - Remember to logroll the patient to assess their posterior aspect
- 30. DEPTH OF BURN Important in evaluating the severity of a burn, planning for wound care, and predicting functional and cosmetic results.
- 31. DEPTH OF BURN FIRST DEGREE • Superficial. • Erythema and pain. • No I.V fluid. SECOND DEGREE • Partial thickness • Painfully, hypersensitive ,blistered and blanch to touch. • I.V fluid. THIRD DEGREE • Full-thickness. • Painless,leathery or waxy white. • I.V fluid
- 32. SECONDARY SURVEY AND RELATED ADJUNCTS Documentation. Baseline investigation. Peripheral Circulation in Circumferential Extremity Burns. Gastric Tube Insertion. Narcotics, Analgesics, and Sedatives(covering the wound will decrease the pain).
- 33. WOUND CARE - Do not break blisters. - Do not apply an antiseptic agent. - Do not apply cold water to a patient with extensive burns (i.e.,> 10% TBSA). - Remove any previously applied medication before using antibacterial topical agents. - Cover the wound.
- 34. ANTIBIOTICS There is no indication for prophylactic antibiotics in the early post burn period.
- 35. TETANUS Determination of the patient’s tetanus immunization status and initiation of appropriate management is very important.
- 36. Burn Patterns Indicating Abuse It is important for clinicians to maintain awareness that intentional burn injury can occur in both children and adults.
- 37. BURN PATTERNS INDICATING ABUSE Circular burns and burns with clear edges and unique Patterns. Burns on the soles of a child’s. A burn to the posterior aspect of the lower extremities and buttocks. Old burn injuries in the setting of a new traumatic injury. Above all, the mechanism and pattern of injury should match the history of the injury.
- 38. PATIENT TRANSFER Partial-thickness burns on greater than 10% TBSA. Burns involving the face, hands, feet, genitalia, perineum, and major joints. Third-degree burns in any age group Electrical burns, including lightning injury ,Chemical burns or Inhalation injury. Burn injury in patients with preexisting medical disorders. Any patient with burns and concomitant trauma. Burned children in hospitals without qualified personnel or equipment for the care of children. Burn injury in patients who will require special social, emotional, or rehabilitative intervention.
- 39. PITFALL Patient loses airway during transfer. - Reassess airway before transfer. - When the patient has risk factors for inhalation injury or has received significant amounts of resuscitation fluid, contact the receiving facility to discuss intubation before transfer.
- 40. PITFALL - Patient experiences severe pain with dressing change. - Provide adequate analgesia before manipulating burns. - Use non-adherent dressings or burn sheets to protect burn from contamination before transfer
- 41. PITFALL Ensure that appropriate information is relayed by using transfer forms or checklist The receiving hospital is unable to discern the burn wound size from the documentation.
- 42. PITFALL The receiving hospital is unable to discern the amount of fluid resuscitation provided from the documentation. Ensure that the flow sheets documenting IV fluids and urinary output are sent with the patient.
- 43. TEAMWORK • ATLS principles. importance of limiting exposure (minimize hypothermia). Communicate early and regularly regarding concerns.
- 44. THANKS
