Rheumatoid Arthritis Treatment and Management
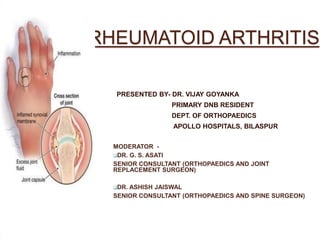
- 1. RHEUMATOID ARTHRITIS PRESENTED BY- DR. VIJAY GOYANKA PRIMARY DNB RESIDENT DEPT. OF ORTHOPAEDICS APOLLO HOSPITALS, BILASPUR MODERATOR - DR. G. S. ASATI SENIOR CONSULTANT (ORTHOPAEDICS AND JOINT REPLACEMENT SURGEON) DR. ASHISH JAISWAL SENIOR CONSULTANT (ORTHOPAEDICS AND SPINE SURGEON)
- 2. INTRODUCTION Autoimmune disorder in which immune system identifies “Synovial Membrane as foreign” and attacks it. May affect many tissue and organs but mainly affects joints with synovial membrane.
- 3. ETIOLOGY RISK FACTORS ◦ Environmental influences (Trauma, Infection) ◦ Geneticmarkers (such HLA-DR4 and HLA-DRB1) ◦ Gender- Women > Men (3:1) Age- 30 to 50 ◦ Familial ◦ Smoking ◦ Vitamin D deficiency
- 4. PATHOGENESIS OF RHEUMATOID ARTHRITIS
- 5. NORMAL JOINT V/S RHEUMATOID JOINT
- 6. PATHOLOGY Stage 1: Pre-clinical - Before RA becomes clinically apparent; Raised ESR, C-reactive protein (CRP) and RF may be detectable. Stage 2: Synovitis – Angiogenesis, synoviocytes proliferation and infiltration of the subsynovial layers by Leucocytes. ◦ Structures are still intact and mobile ◦ Potentially reversible.
- 7. Stage 3: Destruction- Persistent inflammation causes joint and tendon destruction. ◦ Articular cartilage is eroded by a pannus of granulation . ◦ At the margins of the joint, bone is eroded by tissue invasion and osteoclastic resorption. ◦ Tenosynovitis also occurs. Stage 4: Deformity – Mechanical and functional effects of joint and tendon disruption now become vital.
- 9. CLINICAL FEATURES Early feature (synovitis) Most commonly affected MCPJ and PIPJ, wrist, tendon sheaths around the joints (wrist- feet-knee-shoulder) Bilateral symmetrical polysynovitis Pain, fusiform swelling, stiffness, loss of mobility Constitutional symptom: a. Loss of Appetite, malaise and low grade fever b. Tenosynovitis
- 10. Late feature (DESTRUCTIVE) Spread to other joint - wrist, ankle, knee, shoulder (in order of frequency) Morning stiffness (more than 30 min) - improve with activity Activity of daily living will be affected -quality of life affected Rheumatoid Nodules
- 11. More later (DEFORMITY) Pain, deformity, instability, decreased ROM Thumb-Z-deformity Fingers - Swan neck deformity/ Boutonniere's deformities, ulnar deviation Wrist-radial and volar displacement Knees swollen, flexion and vulgus Toes-clawed
- 12. SOME COMMON DEFORMITIES IN RHEUMATOID ARTHRITIS
- 14. DIAGNOSIS Mostly clinical Bilateral, symmetrical Rheumatoid subcutaneous nodules, polyarthritis Involving proximal joints of hand or feet Present for at least 6 weeks Confirmed with Subcutaneous nodules or periarticular erosions on x-ray
- 15. LAB INVESTIGATIONS CBC- Normocytic hypochromic anaemia Inflammatory markers- ESR, CRP elevated Rheumatoid factor(RF)- Anti-IgG auto Ab 80% will have it Anti-cyclic citrullinated peptide(CCP) Ab
- 17. IMAGING EARLY STAGE(SYNOVITIS) Soft tissue swelling, periarticular osteopenia LATER STAGE(DESTRUCTIVE) Juxtaarticular erosions, narrowing of joint space ADVANCE STAGE(DEFORMITY) Articular destruction and joint deformity
- 20. MANAGEMENT No treatment cures RA Goals of management are- Alleviate symptoms Reduction of functional limitation Delay progreesion and maintenance of remission with disease modifying agents
- 22. PHARMACOTHERAPY
- 25. TREATMENT Early (1st 6-12 month) NSAIDs, analgesic, low dose corticosteroid Disease modifying drug Physiotherapy Splintage Progressive erosive (1-5 years) Disease modifying drug Splintage Surgical management (synovectomy, arthroscopic surgery), late (5-20 years) Reconstructive surgery (arthrodesis, osteotomy, arthroplasty)
- 26. SURGERY 1. Synovectomy When one or two joints are affected Removing the diseased synovium or lining of the joint Slowing or prevention of further joint damage 2. Arthroscopic Surgery Tissue samples taken, remove loose cartilage, repair tears It is most commonly performed on the knee and shoulder
- 27. 3. Osteotomy Literally meaning, "to cut bone," this procedure is used to increase stability by redistributing the weight on the joint. 4. Joint Replacement Surgery or Arthroplasty Usually recommended for people over 50 or who have severe disease progression. 5. Arthrodesis or fusion This procedure fuses two bones together. While it limits movement It does decrease pain and increase stability of the joints in the ankles, wrists, fingers, toes and spine.
- 28. COMPLICATIONS Fixed deformities Muscle weakness Infection Spinal cord compression Systemic vasculitis Amyloidosis- Renal failure