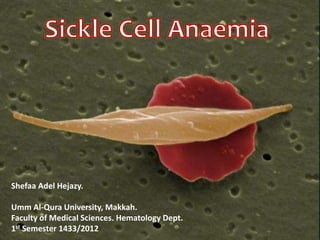
History, pathogenesis, diagnosis and treatment of sickle cell anemia (SCA
- 1. Shefaa Adel Hejazy. Umm Al-Qura University, Makkah. Faculty of Medical Sciences. Hematology Dept. 1st Semester 1433/2012
- 2. History of SCA • The first case of SCD reported in 1910 (Walter Clement-Noel). He complained of several attacks of fever and cough and a history of leg ulcers, jaundice, and exercise intolerance. Dr. J Herrick and Dr. E Irons made clinical observations and reported blood films and photomicrographs of nucleated red cells and red cells with a "slender sickle shape". • In 1915 Cook and Meyer raised the question of a genetic basis for the disorder. • In 1922 Vernon Mason coined the term Sickle Cell Anaemia. • In 1949, Pauling and his colleagues demonstrated electrophoretic differences between haemoglobins from normal one.
- 3. What is SCA ?? • Sickle cell disease/syndrome is a group of Hgb disorders and the most important structural abnormality that occur in the Hb chain (sickle β-globin gene). • Homozygous SCA (Hb SS) is the most common; while the heterozygote such as: Hb SC and Hb Sβ-thalassemia also cause sickling disease.
- 4. • Hb S results from a single-base mutation of Adenine to Thymine; causing a substitution of Val to Glu at the 6th codon of β-globin chain. • The allele responsible for sickle-cell anaemia is autosomal recessive and can be found on the short arm of chromosome 11. • Deoxygenated sickle haemoglobin polymerizes into long fibers; the cells become less flexible, rigid and take up the sickle appearance. • Hb S (Hb α2 β2S) is insoluble and forms crystals at low oxygen tension. SCA Pathogenesis
- 9. • SCA is a very widespread disorder and can be found in up to 1 in 4 west Africans, maintained at this level because of the protection against malaria that is afforded by the carrier state (balanced polymorphism). • The disease is also found in India, the Middle East, and southern Europe.
- 10. SCA Abnormal Hb S SCD Homozygous (SS) SC trait Heterozygous (SA) Other Heterozygous: (Sβ thalassemia, SC, HbH, E, O …etc Glu:Val substitution At the 6th position of β-globin chain
- 11. Homozygous disease Clinical features: 1. Severe haemolytic anaemia punctuated by crises. • Symptoms are often mild in relation to the severity of the anaemia; because Hb S gives up O2 to tissues more easily than Hb A does, and its O2 dissociation curve shifts to the right (P50 rise + low affinity of O2). • The clinical expression of Hb SS is very variable, some patients have an almost normal life, free of crises, while others develop severe crises even as infants and may die in early childhood or as young adults. • These crises can be …..
- 12. 2. Vaso-occlusive, visceral, aplastic or haemolytic crises. Others such as, 3. Ulcers of the lower legs are common, as a result of vascular stasis and local ischemia . 4. The spleen is enlarged in infancy and early childhood but later is often reduced in size as a result of infarcts (autosplenectomy). 5. A proliferative retinopathy and priapism. 6. Chronic damage to the liver may occur through microinfarcts. 7. Pigment (bilirubin) gall stones are frequent.
- 13. 8. The kidneys are vulnerable to infarctions. Failure to concentrate urine leading to dehydration and crisis. 9. Osteomyelitis.
- 15. Painful vaso-occlusive crises • The most frequent complications in SCD Precipitated by: Infection Acidosis Dehydration Deoxygenation (e.g. High altitude, operations, obstetric delivery, stasis of the circulation, exposure to cold, violent exercise, etc.). • Infarcts may occur in the bones, lungs, spleen, and brain or spinal cord. • The “hand-foot” syndrome (painful dactylitis caused by infarcts of the small bones) is frequently the first presentation of the disease.
- 18. Visceral sequestration crises These are caused by sickling within organs and pooling of blood, often with a severe exacerbation of anaemia. 1) The acute sickle chest syndrome: • It presents with dyspnoea , falling PO2, chest pain and pulmonary infiltrates on chest X-ray. • It is the most common cause of death after puberty. o Treatment: • Analgesia • Oxygen • Exchange transfusion • Ventilatory support if necessary.
- 19. 3) Hepatic and girdle sequestration crises and splenic sequestration All may lead to severe illness requiring exchange transfusions. • The splenic sequestration is typically seen in infants and presents with enlarged spleen, reduced haemoglobin and abdominal pain. o Treatment: • With transfusion patients must be monitored at regular intervals as progression may be rapid. • Recurrent attacks and splenectomy is recommended.
- 20. 3) Aplastic Crises • These may occur as a result of infection with parvovirus or folate deficiency and are characterized by a sudden fall in haemoglobin, usually requiring transfusion. • They are characterized by a fall in reticulocyte number as well as haemoglobin. 4) Haemolytic Crises • These are characterized by an in increased rate of haemolysis with a fall in haemoglobin but with reticulocytosis, and usually accompany a painful crises.
- 21. There are nearly 900 hemoglobin variants. Hence screening and confirmation of the presence of hemoglobin S must be implemented via a variety of tests…
- 22. Laboratory diagnosis 1. CBC 2. Blood Film 3. Reticulocyte Count 4. Iron Studies 5. Sickling test 6. Solubility test 7. Haemoglobinopathy Evaluation (electrophoresis, HPLC or Isoelectric focusing). Screening tests
- 23. Laboratory findings The haemoglobin is usually (6 – 9 g/dl), low in comparison to symptoms of anaemia. Sickle cells and target cells occur in the blood. Features of splenic atrophy (e.g. Howell-jolly bodies) may also be present. Screening tests for sickling are positive when the blood is deoxygenated (e.g. with dithionate and Na2HPO4). Haemoglobin electrophoresis show: Hb SS, no Hb A is detected. The Hb F is variable and is usually 5-15%, larger amounts are normally associated with milder disorder.
- 24. Sickle Cell
- 30. % F% A2% A% SMCV <1<3.562-6535-38NA/S 5-10<3.5088-93NSS 5-10>3.5088-93LS/βº Thalassaemia 1-10>3.53-3050-93LS/β+ Thalassaemia 20-35<3.5056-80NS/ HPFH <1<3.562-7028-35N/LAS/α+ Thalassaemia <1<3.568-7820-30LAS/αº Thalassaemia 1-10<3.5088-93N/LSS/α Thalassaemia
- 32. Diagnostic Screening Newborn Screening Test Genetic Study /DNAAnalysis For monitoring treatment: Amount of Hb S should be dignified and followed over the course of a treatment
- 33. Sickle cell trait • Refers to a heterozygous state (Hb AS). • It is a benign condition. Asymptomatic and appear without significant clinical/haemtological manifistations. • Haematuria is the most common symptom and is thought to be caused by minor infarcts of the renal papillae. • Failure to concentrate urine is a consistent defect in patients with sickle trait. • Care must be taken during pregnancy, with anesthesia, and at high altitudes (e.g. flights).
- 34. Sickle cell trait • There is no anaemia, and normal red cells appear in the blood smear, except that few target cells are present. • Diagnosis is made by a positive sickling and/or solubility test or by Haemoglobin electrophoresis. • On electrophoresis, typically there is approximately 60% or more of Hb A, and Hb S varies from 25 - 45% of the total Haemoglobin. • Hb A2 can be slightly increased, and Hb F is within normal range. Levels below 40% of Hb S can be seen in patients having α-thalassaemia or IDA. No treatment is required. Life span of the patient usually is not affected by this benign codition.
- 35. Combination of Haemoglobin S with other genetic defects of haemoglobin HbS/β-thalassaemia • Lower MCV and MCH than in homozygous Hb SS. • The clinical picture is of sickle cell anaemia • Splenomegaly is frequent. Hb SC Disease (clinical course similar to Hb SS) They have milder anaemia, higher incidence of retinal abnormalities, splenomegaly and generally a longer life expectancy. • Have a tendency to thrombosis and pulmonary embolism, especially in pregnancy. • Diagnosis is made by haemoglobin electrophoresis.
- 36. Haemoglobin C disease • This genetic defect of Hb is frequent in West Africa. • As a result of lysine for glutamic acid substitution. • Hb C tends to form rhomboidal crystals within the erythrocytes or they can be seen on the blood smear. The Homozygous state may show mild haemolytic anaemia with marked target cells, rhomboidal shaped cells and microspherocytes. Enlarged spleen. Homozygous show 100% Hb C; while heterozygous may show 35% Carriers show a few target cells only.
- 37. Hb C disease Hb C crystals
- 38. • Presence of HbC, but with a higher proportion of HbA: HbC trait i.e. Hb AC. • Presence of Hb C and Hb F, but no HbA: HbC disease (Hb CC), Hb C/βº-thalassemia (HbC-HPFH) • A higher proportion of HbC than HbA: HbC β+-thalassemia
- 39. Haemoglobin D disease • Homozygotes show mild haemolytic anaemia. • Heterozygotes have no haematological abnormality Haemoglobin E disease • This is the most common haemoglobin variant in South-East Asia. • In the homozygous state there is a mild microcytic, hypochromic anaemia. • Haemoglobin E/β°-thalassaemia is similar to homozygous β°- thalassaemia both clinically and haematologically.
- 40. Prenatal Diagnosis of Genetic Haemoglobin disorders • Genetic counseling is strongly recommended for couples that are suspected of having a child with a major haemoglobin defect • If both partners have an abnormality with a risk of a serious defect in the offspring, antenatal diagnosis is recommended. • Several methods are available, decision made according to the stage of pregnancy and the potential nature of the defect. • Example: Fetal DNA Analysis (amniotic fluid, chorionic villus, or fetal blood). PCR (enzyme Mst II detects the A-T change in Hb S)
- 42. Treatment 1. Prophylactic—avoid those factors precipitate crises, especially • dehydration, • anoxia, • infections, • stasis of the circulation and • cooling of the skin surface. 2. Folic acid, e.g. 5 mg daily. 3. Good general nutrition and hygiene. 4. Pneumococcal, haemophilus and meningococcal vaccination and regular oral penicillin are effective at reducing the infection rate with these organisms. • Oral penicillin should start at diagnosis and continue at least until puberty. • Hepatitis B vaccination is also given as transfusion may be needed.
- 43. 5. Crises—treat by rest, warmth, rehydration by oral fluids and/or intravenous normal saline and antibiotics if infection is present. 6. Analgesia at the appropriate should be given. Suitable drugs are paracetamol, a non-steroidal anti-inflammatory agent and opiates, e.g. continuous subcutaneous diamorphine. 7. Blood transfusion is given only if there is very severe anaemia with symptoms. 8. Exchange transfusion may be needed particularly if there is neurological damage, a visceral sequestration crisis or repeated painful crises. This is aimed at achieving an Hb S percentage of less than 30 in severe cases.
- 44. 9. Particular care is needed in pregnancy and anasthesia. • Careful anaesthetic and recovery techniques must be used to avoid hypoxaemia or acidosis. • Routine transfusions throughout pregnancy are given to those with a bad obstetric history or a history of frequent crises. 10. Transfusions • as prophylaxis to patients having frequent crises or who have had major organ damage,e.g. of the brain. • The aim is to suppress Hb S production over a period of several months or even years. • Iron overload and alloimmunization against donated blood are common problems. 11. Hydroxyurea (15.0-20.0mg/kg) can increase Hb F levels and has been shown to improve the clinical course of patients who are having three or more painful crises each year. It should not be used during pregnancy. 12. Stem cell transplantation can cure the disease and many patients have now been successfully treated. The mortality rate is less than 10%. Transplantation is only indicated in the severest of cases whose quality of life or life expectancy are substantially impaired. 13. Butyrates, to enhance Hb F synthesis or to increase the solubility of Hb S is taking place. 14. Gene therapy' is a distant prospect not yet available.
