Revised sickle cell anemia
•Download as PPTX, PDF•
0 likes•61 views
revised
Report
Share
Report
Share
Recommended
Recommended
More Related Content
What's hot
What's hot (20)
Complete Blood Count Test - Interpretation of Results

Complete Blood Count Test - Interpretation of Results
Similar to Revised sickle cell anemia
Similar to Revised sickle cell anemia (20)
Laboratory Investigation particular for Dentistry.pptx

Laboratory Investigation particular for Dentistry.pptx
Lab investigations and interpretations in periodontics

Lab investigations and interpretations in periodontics
2 Anaemia blood diseases for medical laboratory.ppt

2 Anaemia blood diseases for medical laboratory.ppt
Haematological tests (Common Blood Tests) and significance

Haematological tests (Common Blood Tests) and significance
More from Melissa Ward
More from Melissa Ward (6)
Recently uploaded
❤️ Call Girls service In Panchkula☎️9815457724☎️ Call Girl service in Panchkula☎️ Panchkula Call Girls Service ☎️ Call Girls In Panchkula BEST CALL GIRL ESCORTS SERVICE IN PANCHKULA CALL WATTSAPP 9815457724 THE MOST BEAUTIFUL INDEPENDENT ESCORT CALL GIRL SERVICE In Panchkula WE ARE PROVIDING GENUINE CALL GIRL SERVICE
I AM A a NATURAL BRUNETTES, SLIM BODY, NATURAL LONG HAIR AND ALL TYPE OF HAIR IS A NATURAL BRUNETTE IN THE MOST BEAUTIFUL MODELS INDEPENDENT ESCORT GIRL I AM A NATURAL BRUNETTE WITH ROOM AND HOTEL AND A NATURAL BRUNETTE WITH A BODY MADE FOR SIN AND ALL TYPE OF ME ALL THE TIME
I SEND YOU A HAIR, VERY SOCIABLE AND FUNNY, READY TO ENTERTAIN TO ENTERTAIN U AND MAKE FORGET ABOUT TO AGET ENTERTAINMENT YOU AND MAKE FORGET ABOUT ALL THE PROBLEMS. LET'S HAVE A WONDERFUL TIME TOGETHER AND FORGET ABOUT EVERYTHING ALL TYPE SERVICE ENJOYMENT SAFE AND SECURE IN CALL OUT CALL HOME AND HOTEL ANYTIME AVAILABLE
AND ALL TYPE SERVICE ENJOYMENTPANCHKULA INDEPENDENT BEST CALL GIRL ESCORTS SERVICE IN PANCHKULA INDEPENDENT CALL GIRLS❤️ Call Girls service In Panchkula☎️9815457724☎️ Call Girl service in Panchku...

❤️ Call Girls service In Panchkula☎️9815457724☎️ Call Girl service in Panchku...Rashmi Entertainment
❤️Amritsar Escort Service☎️98151-129OO☎️ Call Girl service in Amritsar☎️ Amritsar Call Girls Service ☎️ Call Girls In Amritsar BEST Call Girls in Amritsar Escort Service provide Cute Nice sweet and Sexy Models in beautiful Amritsar city cash in hand to hand call girl in Amritsar and Amritsar escorts. HOT & SEXY MODELS // COLLEGE GIRLS IN Amritsar AVAILABLE FOR COMPLETE ENJOYMENT WITH HIGH PROFILE INDIAN MODEL AVAILABLE HOTEL & HOME ★ SAFE AND SECURE HIGH CLASS SERVICE AFFORDABLE RATE ★ 100% SATISFACTION,UNLIMITED ENJOYMENT. ★ All Meetings are confidential and no information is provided to any one at any cost.
★ EXCLUSIVE Profiles Are Safe and Consensual with Most Limits Respected
★ Service Available In: - HOME & 24x7 :: 3 * 5 *7 *Star Hotel Service .In Call & Out call
Services :
★ A-Level (5 star escort)
★ Strip-tease
★ BBBJ (Bareback Blowjob)Receive advanced sexual techniques in different mode make their life more pleasurable.
★ Spending time in hotel rooms
★ BJ (Blowjob Without a Condom)
★ Completion (Oral to completion)
★ Covered (Covered blowjob Without a Condom)Amritsar Call Girls❤️Amritsar Escort Service☎️98151-129OO☎️ Call Girl service in Amritsar☎️ Amri...

❤️Amritsar Escort Service☎️98151-129OO☎️ Call Girl service in Amritsar☎️ Amri...shallyentertainment1
🍑👄Ludhiana Escorts Service☎️98157-77685🍑👄 Call Girl service in Ludhiana☎️Ludhiana Call Girls Service 🍑👄 Call Girls In Ludhiana Book Now :- 98157-77685
Our agency presents a selection of young, charming call girls available for bookings at Oyo Hotels. Experience high-class escort services at pocket-friendly rates, with our female escorts exuding both beauty and a delightful personality, ready to meet your desires. Whether it's Housewives, College girls, Russian girls, Muslim girls, or any other preference, we offer a diverse range of options to cater to your tastes.
We provide both in-call and out-call services for your convenience. Our in-call location in Delhi ensures cleanliness, hygiene, and 100% safety, while our out-call services offer doorstep delivery for added ease.
We value your time and money, hence we kindly request pic collectors, time-passers, and bargain hunters to refrain from contacting us. l Ludhiana, Majestic Grand Hotel, Ramada by Wyndham Ludhiana City Centre, Park Plaza Ludhiana, Windsor Fountain, G.T Road Ludhiana escort all Ludhiana service Russian available model female girls in Ludhiana VIP Lo price personal Ludhiana off class call girls payment high profile model and female escort 70% Off On Your First Booking Ludhiana Call Girls Service Cash Payment
Welcome to DILPREET Ludhiana Call Girl Service, the Trusted call girl agency around. We Offer 70% Discount On Your First Booking For Ludhiana Call Girls Service Cash Payment is available.🍑👄Ludhiana Escorts Service☎️98157-77685🍑👄 Call Girl service in Ludhiana☎️Ludh...

🍑👄Ludhiana Escorts Service☎️98157-77685🍑👄 Call Girl service in Ludhiana☎️Ludh...dilpreetentertainmen
❤️ Escorts Service in Bangalore ☎️81279-924O8☎️ Call Girl service in Bangalore☎️ Bangalore Call Girls Service ☎️ Call Girls In Bangalore BEST Call Girls in Bangalore Escort Service provide Cute Nice sweet and Sexy Models in beautiful Bangalore city cash in hand to hand call girl in Bangalore and Bangalore escorts. HOT & SEXY MODELS // COLLEGE GIRLS IN BANGALORE AVAILABLE FOR COMPLETE ENJOYMENT WITH HIGH PROFILE INDIAN MODEL AVAILABLE HOTEL & HOME ★ SAFE AND SECURE HIGH CLASS SERVICE AFFORDABLE RATE ★ 100%SATISFACTION,UNLIMITED ENJOYMENT. ★ All Meetings are confidential and no information is provided to any one at any cost. ★ EXCLUSIVE Profiles Are Safe and Consensual with Most Limits Respected ★ Service Available In: - HOME & 24x7 :: 3 * 5 *7 *Star Hotel Service .In Call & Out call Services :
★ A-Level (5 star escort)
★ Strip-tease
★ BBBJ (Bareback Blowjob)Receive advanced sexual techniques in different mode make their life more pleasurable.
★ Spending time in hotel rooms
★ BJ (Blowjob Without a Condom)
★ Completion (Oral to completion)
★ Covered (Covered blowjob Without a Condom)-Bangalore Call Girls❤️Bangalore Call Girls ☎️81279-924O8☎️ Call Girl service in Bangalore☎️ Bangalore Call Girls Service ☎️ Call Girls In Bangalore
❤️ Escorts Service in Bangalore ☎️81279-924O8☎️ Call Girl service in Bangalor...

❤️ Escorts Service in Bangalore ☎️81279-924O8☎️ Call Girl service in Bangalor...chandigarhentertainm
Recently uploaded (19)
❤️ Zirakpur Call Girl Service ☎️9878799926☎️ Call Girl service in Zirakpur ☎...

❤️ Zirakpur Call Girl Service ☎️9878799926☎️ Call Girl service in Zirakpur ☎...
Call Girls In Indore 💯Call Us 🔝 9987056364 🔝 💃 Independent Escort Service Ind...

Call Girls In Indore 💯Call Us 🔝 9987056364 🔝 💃 Independent Escort Service Ind...
Making change happen: learning from "positive deviancts"

Making change happen: learning from "positive deviancts"
❤️ Call Girls service In Panchkula☎️9815457724☎️ Call Girl service in Panchku...

❤️ Call Girls service In Panchkula☎️9815457724☎️ Call Girl service in Panchku...
💸Cash Payment No Advance Call Girls Kanpur 🧿 9332606886 🧿 High Class Call Gir...

💸Cash Payment No Advance Call Girls Kanpur 🧿 9332606886 🧿 High Class Call Gir...
👉Bangalore Call Girl Service👉📞 6378878445 👉📞 Just📲 Call Manisha Call Girls Se...

👉Bangalore Call Girl Service👉📞 6378878445 👉📞 Just📲 Call Manisha Call Girls Se...
❤️Amritsar Escort Service☎️98151-129OO☎️ Call Girl service in Amritsar☎️ Amri...

❤️Amritsar Escort Service☎️98151-129OO☎️ Call Girl service in Amritsar☎️ Amri...
💸Cash Payment No Advance Call Girls Pune 🧿 9332606886 🧿 High Class Call Girl ...

💸Cash Payment No Advance Call Girls Pune 🧿 9332606886 🧿 High Class Call Girl ...
💸Cash Payment No Advance Call Girls Nagpur 🧿 9332606886 🧿 High Class Call Gir...

💸Cash Payment No Advance Call Girls Nagpur 🧿 9332606886 🧿 High Class Call Gir...
🍑👄Ludhiana Escorts Service☎️98157-77685🍑👄 Call Girl service in Ludhiana☎️Ludh...

🍑👄Ludhiana Escorts Service☎️98157-77685🍑👄 Call Girl service in Ludhiana☎️Ludh...
💞 Safe And Secure Call Girls Coimbatore 🧿 9332606886 🧿 High Class Call Girl S...

💞 Safe And Secure Call Girls Coimbatore 🧿 9332606886 🧿 High Class Call Girl S...
💸Cash Payment No Advance Call Girls Hyderabad 🧿 9332606886 🧿 High Class Call ...

💸Cash Payment No Advance Call Girls Hyderabad 🧿 9332606886 🧿 High Class Call ...
👉Indore Call Girl Service👉📞 7718850664 👉📞 Just📲 Call Anuj Call Girls In Indor...

👉Indore Call Girl Service👉📞 7718850664 👉📞 Just📲 Call Anuj Call Girls In Indor...
TIME FOR ACTION: MAY 2024 Securing A Strong Nursing Workforce for North Carolina

TIME FOR ACTION: MAY 2024 Securing A Strong Nursing Workforce for North Carolina
❤️ Escorts Service in Bangalore ☎️81279-924O8☎️ Call Girl service in Bangalor...

❤️ Escorts Service in Bangalore ☎️81279-924O8☎️ Call Girl service in Bangalor...
💞 Safe And Secure Call Girls gaya 🧿 9332606886 🧿 High Class Call Girl Service...

💞 Safe And Secure Call Girls gaya 🧿 9332606886 🧿 High Class Call Girl Service...
💞 Safe And Secure Call Girls Mysore 🧿 9332606886 🧿 High Class Call Girl Servi...

💞 Safe And Secure Call Girls Mysore 🧿 9332606886 🧿 High Class Call Girl Servi...
Revised sickle cell anemia
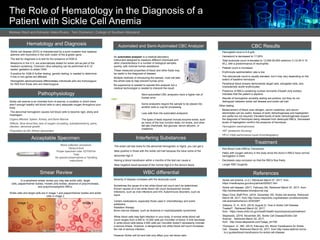
- 1. The Role of Hematology in the Diagnosis of a Patient with Sickle Cell Anemia Melissa Ward and Edmarie Velez-Rivera Terri Domenici | College of Southern Maryland Hematology and Diagnosis Sickle cell disease (SCD) is characterized by a point mutation that replaces adenine with thymidine in the sixth codon of the β-globin gene. The test for diagnosis is to test for the presence of HGB-S. Newborns in the U.S. are automatically tested for sickle cell as part of the newborn screening. Chorionic villus sampling can be performed at 8-12 weeks' gestation to obtain DNA. If positive for HGB-S further testing, genetic testing, is needed to determine if one or two genes are affected. Hemoglobin electrophoresis differentiates individuals who are homozygous for HbS from those who are heterozygous. Pathophysiology Sickle cell anemia is an inherited form of anemia, a condition in which there aren't enough healthy red blood cells to carry adequate oxygen throughout your body. .The abnormal hemoglobin causes red blood cells to become rigid, sticky and misshapen. Organs affected: Spleen, Kidney, and Bone Marrow •Effects: Slow blood flow, lack of oxygen circulating, autosplenectomy, pains, infection, abnormal growth •Population at risk: African descendant Acceptable Specimen Automated and Semi-Automated CBC Analyzer Treatment WBC differential CBC Results An automated analyser is a medical laboratory instrument designed to measure different chemicals and other characteristics in a number of biological samples quickly, with minimal human assistance. These measured properties of blood and other fluids may be useful in the diagnosis of disease. Multiple methods of introducing the sample, most will take the whole tube to help prevent human error. No experience is needed to operate this analyzer but a medical technologist is needed to interpret the result. Interfering Substances • Red Blood Cells (RBCs) Transfusion • Helps with oxygen delivery in the body since the donor’s RBCs have normal hemoglobin in them • Decreases vaso-occlusion so that the RBCs flow freely • Longer RBC longevity References • Sickle cell anemia. (n.d.). Retrieved March 07, 2017, from https://medlineplus.gov/ency/article/000527.htm • Sickle cell disease. (2017, February 09). Retrieved March 07, 2017, from http://sicklecelldisease.bloodjournal.org/ • Mayo Clinic Staff Print. (2016, December 29). Sickle cell anemia. Retrieved March 08, 2017, from http://www.mayoclinic.org/diseases-conditions/sickle- cell-anemia/home/ovc-20303267 • Gibbons, G. H., M.D. (2016, August 2). How is Sickle Cell Disease Treated? Retrieved March 02, 2017, from https://www.nhlbi.nih.gov/health/health-topics/topics/sca/treatment • Stepwards. (2016, November 26). Sickle Cell Disease/Sickle Cell Anemia. Retrieved March 02, 2017, from http://www.stepwards.com/?page_id=792 • Thompson, G., MD. (2015, February 20). Blood Transfusions for Sickle Cell Disease. Retrieved March 02, 2017, from http://www.webmd.com/a- to-z-guides/blood-transfusions-for-sickle-cell-disease Smear Review In a peripheral smear review you may see sickle cells, target cells, pappenheimer bodies, Howell-Jolly bodies, absence of polychromasia, and polychromatophilic RBCs. Sickle cells and target cells are in image 1 and pappenheimer bodies and sickle cells in image 2 Image 1 Image 2 • Hemoglobin level is 5-9 g/dL • Hematocrit is decreased to 17-29% • Total leukocyte count is elevated to 12,000-20,000 cells/mm 3 (12-20 X 10 9/L), with a predominance of neutrophils • Platelet count is increased • Erythrocyte sedimentation rate is low • The reticulocyte count is usually elevated, but it may vary depending on the extent of baseline hemolysis • Peripheral blood smears demonstrate target cells, elongated cells, and characteristic sickle erythrocytes • Presence of RBCs containing nuclear remnants (Howell-Jolly bodies) indicates that the patient is asplenic • Results of hemoglobin solubility testing are positive, but they do not distinguish between sickle cell disease and sickle cell trait Other testing • Measurement of blood urea nitrogen, serum creatinine, and serum electrolytes can be useful. Assays of lactic dehydrogenase and haptoglobin are useful but not required. Elevated levels of lactic dehydrogenase support the diagnosis of hemolysis being released from destroyed RBCs. Decreased levels of haptoglobin confirm the presence of hemolysis. • Hemoglobin electrophoresis • •IEF (isoelectric focusing) • HPLC (High performance liquid chromatography) Semi-automated CBC analyzers have a higher risk of human error. Some analyzers require the sample to be placed into another tube or cup for processing. Less safe than the automated analyzers. The types of tests required include enzyme levels, such as many of the liver function tests, ion levels, and other tell-tale chemicals, like glucose, serum albumin, or creatinine. Severity of disease increases with the leukocyte count Sometimes the cause of a low white blood cell count can't be determined. Known causes of a low white blood cell count (leukopenia) include: Infections, such as viral infections and HIV, Autoimmune disorders, such as lupus Certain medications, especially those used in chemotherapy and some antibiotics Radiation therapy Bone marrow disease, such as leukemia or myelodysplastic syndromes White blood cells help fight infection in your body. A normal white blood cell count ranges from 4,500 to 10,000 cells per microliter of blood. A mild decrease in white blood cells below 4,500 cells per microliter doesn't necessarily indicate a serious illness. However, a dangerously low white blood cell count increases the risk of serious infection. However Sickle cell full and trait only effect your red blood cells. Blood collection procedure: Venipuncture Proper specimen tube: EDTA/Pink Tube No special preservatives or handling instructions The sickle cell test looks for the abnormal hemoglobin or HgbS, you can get a false positive in those with the sickle cell trait because the have some of the abnormal Hgb S Having a blood transfusion within 4 months of the test can cause a false negative result because of the normal Hgb A in the donors blood.