HOMEOSTASIS & HEMOSTASIS.pptx
- 1. ZERA INTERNATIONAL COLLEGE OF HEALTH SCIENCES DEPARTMENT OF PATHOLOGY DR M.KATASO MD HOMEOSTASIS & HEMOSTASIS
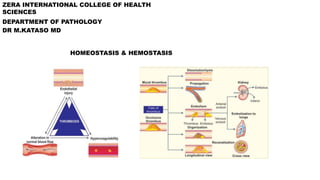
- 2. HOMEOSTASIS 1. Homeostasis ( homeo- sameness; -stasis standing still) is the condition of equilibrium (balance) in the body’s internal environment due to the constant interaction of the body’s many regulatory processes. 2. Homeostasis is a dynamic condition. In response to changing conditions, the body’s equilibrium can shift among points in a narrow range that is compatible with maintaining life. 3. Homeostasis in the human body is continually being disturbed. Fortunately, the body has many regulating systems that can usually bring the internal environment back into balance. 4. Most often, the nervous system and the endocrine system, working together or independently, provide the needed corrective measures. The nervous system regulates homeostasis by sending electrical signals known as nerve impulses (action potentials) to organs that can counteract changes from the balanced state. The endocrine system includes many glands that secrete messenger molecules called hormones into the blood. Nerve impulses typically cause rapid changes, but hormones usually work more slowly.
- 3. CONTROL OF HOMEOSTASIS • The body can regulate its internal environment through many feedback systems. • A feedback system or feedback loop is a cycle of events in which the status of a body condition is monitored, evaluated, changed, remonitored, reevaluated, and so on. • Each monitored variable, such as body temperature, blood pressure, or blood glucose level, is termed a controlled condition. Any disruption that changes a controlled condition is called a stimulus. • A feedback system includes three basic components: 1. A receptor, 2. A control center, and 3. An effector
- 4. CONTROL OF HOMEOSTASIS 1. A receptor is a body structure that monitors changes in a controlled condition and sends input to a control center. Typically, the input is in the form of nerve impulses or chemical signals. For example, certain nerve endings in the skin sense temperature and can detect changes, such as a dramatic drop in temperature. 2. A control center in the body, for example, the brain, sets the range of values within which a controlled condition should be maintained, evaluates the input it receives from receptors, and generates output commands when they are needed. Output from the control center typically occurs as nerve impulses, or hormones or other chemical signals. 3. An effector is a body structure that receives output from the control center and produces a response or effect that changes the controlled condition. Nearly every organ or tissue in the body can behave as an effector.
- 6. CONTROL OF HOMEOSTASIS • In a feedback system, the response of the system “feeds back” information to change the controlled condition in some way, either negating it (negative feedback) or enhancing it (positive feedback). • NEGATIVE FEED BACK SYSTEM: • A negative feedback system reverses a change in a controlled condition, eg regulation of high BP. • POSITIVE FEEDBACK SYSTEM. • A positive feedback system tends to strengthen or reinforce a change in one of the body’s controlled conditions. A positive feedback system operates similarly to a negative feedback system, except for the way the response affects the controlled condition. The control center still provides commands to an effector, but this time the effector produces a physiological response that adds to or reinforces the initial change in the controlled condition. Normal childbirth provides a good example of a positive feedback system
- 7. HOMEOSTASIS & BODY FLUIDS • 60% of total body weight is water. Water is compartmentalized. • The fluid within cells is intracellular fluid (intra- inside), abbreviated ICF( 2/3rd of total body water). The fluid outside body cells is extracellular fluid (extra- outside), abbreviated ECF. The ECF that fills the narrow spaces between cells of tissues is known as interstitial fluid (inter- between). • ECF within blood vessels is termed blood plasma, within lymphatic vessels it is called lymph, in and around the brain and spinal cord it is known as cerebrospinal fluid, in joints it is referred to as synovial fluid, and the ECF of the eyes is called aqueous humor and vitreous body. • The proper functioning of body cells depends on precise regulation of the composition of the interstitial fluid surrounding them. Because of this, interstitial fluid is often called the body’s internal environment. The composition of interstitial fluid changes as substances move back and forth between it and blood plasma. Such exchange of materials occurs across the thin walls of the smallest blood vessels in the body, the blood capillaries.
- 8. IMPORTANT ELECTROLYTES 1. Sodium: found more outside the cell. It has a concentration of 135-145mEq/l. higher and lower sodium levels are termed hypernatremia and hyponatremia respectively. 2. Potassium: found more inside the cell. Serum concentration is 3.5- 7.0mEq/l. higher and lower concentrations are termed hyperkalemia and hypokalemia respectively
- 9. REGULATION OF BLOOD PREASURE • HEMODYNAMIC FACTORS OF BLOOD FLOW • BP= Cardiac output X Total peripheral resistance ( afterload). CO= Heart Rate X Stroke volume. • Stroke volume is highly influenced by three other factors, they include: 1. Contractility 2. Blood volume 3. Preload. • Cardiac output is amount of blood ejected by the ventricles per minute. • Stroke volume is the amount of blood ejected by the ventricles per beat. • Preload is the amount of blood the ventricles will have at the end of diastole or before systole. • Afterload is the resistance the heart has to overcome to move blood from arteries to veins. • Tone of blood vessels determine the preload and afterload. If veins are constricted, venous return increase which in turn increases preload & if dilated venous return reduces & it reduces preload. The same is true for arteries with afterload.
- 10. REGULATION OF BP IN HYPOTENSIVE STATES • BARO-RECEPTOR REFLEX
- 11. REGULATION OF BP IN HYPOTENSIVE STATES • RENIN ANGIOTENSIN ALDOSTERONE SYSTEM A. Renal hypoperfusion B. Juxta-glomerular apparatus detects & releases renin C. Renin converts angiotensinogen to angiotensin 1. D. Angiotensin 1 is converted to angiotensin 2. E. Angiotensin 2 will do the following: 1. venoconstriction: increase preload 2. Arterioloconstriction: increase afterload ( TPR) 3. Cause release of aldosterone from the adrenal gland which causes sodium and water reabsorption: this increases blood volume- sv- co & bp. 4. causes release f ADH from the posterior pituitary: causes free water reabsorption: this increases blood volume & ultimately bp.
- 12. REGULATION OF BP IN HIGH STATES 1. BARO-RECEPTOR REFLEX: Parasympathetic is activated instead. 2. RAAS: Inhibited.
- 13. SHOCK • A state of tissue hypoxia due to imbalance between oxygen delivery & utilization. • Hypotension is the most common manifestation of shock. • They are four types of shock, namely 1. Hypovolemic shock : decreased intravascular volume 2. Cardiogenic shock: intracardiac pump failure 3. Obstructive shock: extracardiac pump failure 4. Distributive shock: excessive & extensive peripheral vasodilation
- 14. HYPOVOLEMIC SHOCK • Can be hemorrhagic & non-hemorrhagic. • Hemorrhagic causes include: trauma, git bleeding, gut bleeding etc. • Non-hemorrhagic: i. Excessive water loss: diarrhea, profuse vomiting, diuresis, burns, heat stroke etc. ii. Fluid third spacing: iii. Fluid intake restriction.
- 15. CARDIOGENIC SHOCK • Causes cab be 1. Cardiomyopathic: myocarditis, myocardial infarction, dilated cardiomyopathy etc, 2. Arrhythmic : abnormal electrical impulses: ventricular tachyacadia third degree heart blocks 3. Mechanical : vulvular diseases
- 16. OBSTRUCTIVE SHOCK • Can be pulmonary & cardiac causes • Pulmonary causes: pulmonary embolism, pulmonary hypertension, tension pneumothorax • Cardiac causes: cardiac tamponade, constrictive pericarditis, restrictive cardiomyopathy.
- 17. DISTRIBUTIVE SHOCK • Can be : 1. Septic shock: mostly due to infections 2. Anaphylactic shock: allegies 3. Neurogenic shock: autonomic nervous system dysfunction 4. Toxin induced shock: drugs, snake bites, insect bites, spider bites, blood transfusion reactions. Etc.
- 18. CLINICAL FEATURES 1. Hypotension 2. Tachycardia 3. Tachypnea 4. Oliguria 5. Altered sensorium 6. Cold peripheries, clammy hands with prolonged capillary refill time ( seen is hypovolemic, cardiogenic & obstructive shock: cold shock) 7. Warm peripheries and fast capillary refill time: seen in distributive shock. • Etc.
- 19. HEMOSTASIS • The process of halting bleeding. • Endothelial cells play an important role in both homeostasis and thrombus formation. They have both anti-thrombotic and prothrombotic (procoagulant) properties. The balance between these two opposing endothelial properties determines the thrombus formation. • FUNCTION OF ENDOTHELIUM A. Antithrombotic properties: healthy endothelium 1. Antiplatelet effects: Prostacyclin ( PGI2), nitric oxide & adenosine diphosphatase. 2. Anti coagulant effects: heparin sulfate, anti-thrombin three, thrombomodulin, protein c & s. 3. Fibrinolytic effects: produce tissue plasminogen activator B. Pro thrombotic properties: injured endothelium.
- 20. HEMOSTASIS • PRIMARY HEMOSTASIS • Von Willebrand factor- platelet adhesion –platelet activation & aggregation. Molecules involved are serotonin, ADP & calcium. • SECONDARY HEMOSTASIS: Intrinsic & extrinsic pathway.
- 21. THROMBOSIS • Thrombosis is defined as the process of formation of a solid mass in the circulating blood from the constituents of flowing blood. If the solid mass is mobile its called embolus. Clot is solid mass formation( thrombus) outside the CVS. • CAUSES: VIRCHOWS TRIADE.
- 22. FATE OF A THROMBUS
- 23. BLEEDING DISORDERS • Diseases of primary hemostasis 1. Thrombocytopenia: low platelet count < 150k. Risk of bleeding at 50k & spontaneous bleeding at 20k. 2. Qualitative platelets: uremia etc, 3. Von Willebrand disease • Diseases of secondary hemostasis: 1. Hemophilia A & B ( FACTOR 8 & 9) 2. ETC