Physiology Term 2 #8 - Gas Exchange
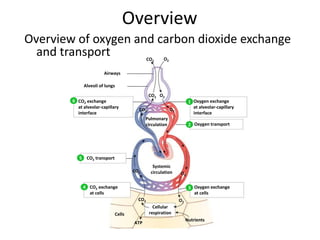
- 1. CO2 O2 Alveoli of lungs Airways CO2 CO2 O2 O2 Pulmonary circulation CO2 O2 Cellular respiration ATP Nutrients Cells Systemic circulation CO2 O2 Oxygen exchange at cells Oxygen transport CO2 exchange at alveolar-capillary interface Oxygen exchange at alveolar-capillary interface CO2 exchange at cells CO2 transport 1 2 34 5 6 Overview Overview of oxygen and carbon dioxide exchange and transport
- 2. Diffusion and Solubility These are factors that affect diffusion if membrane permeability remains the same • Surface area- diffusion rate is proportional to available surface area – Constant- remains the same over a long period of time • Concentration gradient- diffusion rate is proportional to concentration gradient – Most important factor- O2 and CO2 gradients will be present at lung and tissue capillaries • Membrane thickness – diffusion rate is inversely proportional which is why walls are so thin – Constant- number of cells in walls should not change • Diffusion distance- diffusion rate is inversely proportional, another reason why walls are thin – Constant
- 3. Movement of Gases These are factors that influence the movement of gasses from air into a liquid • Pressure gradient- drives gas flow • Solubility- the gas must be able to dissolve in the liquid, diffusion will continue until it reaches equilibrium, increased pressure may dissolve some gas if solubility is low. • Temperature- temperature is constant so it doesn’t play a role in the body unless there is pathology
- 4. Behavior of Gases in Solution PO2 = 100 mm Hg PO2 = 0 mm Hg PO2 = 100 mm Hg [O2] = 5.20 mmol/L PO2 = 100 mm Hg [O2] = 0.15 mmol/L (a) (b) (c)Initial state: no O2 in solution Oxygen dissolves. At equilibrium, PO2 in air and water is equal. Low O2 solubility means concentrations are not equal. The pressure equilibrium is not the same as the concentration dissolved.
- 5. Behavior of Gases in Solution Oxygen is less soluble in water than carbon dioxide
- 7. Gas Exchange at the Alveoli and Cells Gases move from areas of high partial presssures to areas of low partial pressure Venous blood has the same Po2 as tissues
- 8. Gas Exchange Oxygen diffuses across alveolar epithelial cells and capillary endothelial cells to enter the plasma Gas exchange is rapid and blood flow is slow which allows for equilibrium in 1 second!
- 9. Gas Exchange Hypoxia is not a disease, it is caused by something that decreases diffusion or oxygen deliver, that can cause disease
- 10. O2 O2 dissolved in plasma (~ PO2) < 2% O2 + Hb ARTERIAL BLOOD Alveolar membrane Alveolus Capillary endothelium Red blood cell Cells Oxygen Transport 98% of oxygen is bound to hemoglobin and the other 2% is dissolved in plasma
- 11. O2 O2 dissolved in plasma (~ PO2) < 2% O2 + Hb Hb•O2 > 98% ARTERIAL BLOOD Alveolar membrane Alveolus Capillary endothelium Red blood cell Cells Oxygen Transport Because oxygen is not easily dissolve in water, hemoglobin is a protein that binds O2 and dramatically increased the amount of blood in the plasma
- 12. O2 O2 dissolved in plasma (~ PO2) < 2% O2 + Hb Hb•O2 > 98% ARTERIAL BLOOD Alveolar membrane Alveolus Capillary endothelium Transport to cells Red blood cell Cells Hb•O2 Oxygen Transport One reason why blood transfussions are used is to provide hemoglobin for efficient O2 transport. Researcher are working on carrier proteins
- 13. Oxygen Transport O2 O2 O2 dissolved in plasma (~ PO2) < 2% O2 dissolved in plasma O2 + Hb Hb•O2 > 98% Hb + O2Hb•O2 ARTERIAL BLOOD Alveolar membrane Alveolus Capillary endothelium Transport to cells Red blood cell Cells Used in cellular respiration Oxygen can travel bound to hemoglobin or to be dissolved in plasma
- 14. Oxygen Transport The role of hemoglobin in oxygen transport This shows that without hemoglobin very little oxygen would dissolve into the plasma- an amount that is not sufficient for cell demand
- 15. Oxygen Transport In the presence of hemoglobin a higher concentration can be dissolved in blood when pressure equilibrium is reached
- 16. Oxygen Transport If there are no problems with hemoblogin binding oxygen, then low blood oxygen levels could be due to a problem with ventilation
- 17. The Hemoglobin Molecule The amount of oxygen bound to hemoglobin depends on the PO2 of plasma- each hemoglobin can carry 4 oxygen molecules, the % saturation tells how much is carried.
- 18. Oxygen-Hemoglobin Dissociation Curve In vitro testing reveals a varying amount of O2 saturation dependent on O2 partial pressure- it doesn’t reach 100% within physiological conditions
- 19. Oxygen Binding Physical factors alter hemoglobin’s affinity for oxygen Changes can alter the hemoglobin conformation which influence delivery at tissues more than obtaining oxygen in the lungs. Release more O2 at pH 7.2 (during exercise) than pH7.4
- 20. Oxygen Binding Higher temperature decreases saturation shifting curve to the right
- 21. Oxygen Binding Increased CO2 decreases O2 saturation
- 22. Oxygen Binding 2,3-DPG alters hemoglobin’s affinity for oxygen Released as a response to low O2 levels as can happen in anemia or high altitudes
- 23. Oxygen Binding Differences in oxygen-binding properties of maternal and fetal hemoglobin Fetal hemoglobin has greater affinity
- 24. Figure 18-13 Oxygen Binding Factors contributing to the total oxygen content of arterial blood
- 25. Carbon Dioxide Transport • Dissolved: 7% - although CO2 is more soluble in plasma than oxygen only a small amount is dissolved in it. • Converted to bicarbonate ion: 70% - an enzyme converts of the CO2 in RBCs into bicarbonate • Bound to hemoglobin: 23% - – Hemoglobin also binds H+ - hemoblogin acts as a buffer binding H+ to resists pH changes – Hb and CO2: carbaminohemoglobin – formed with CO2 and hemoglobin bind, it decreases affinity for O2
- 26. Carbon Dioxide Transport in the Blood CO2 Dissolved CO2 (7%) CO2 Cellular respiration in peripheral tissues VENOUS BLOOD Alveoli Red blood cell Capillary endothelium Cell membrane
- 27. Carbon Dioxide Transport in the Blood CO2 Dissolved CO2 (7%) CO2 + Hb Hb•CO2 (23%) CO2 + H2O HCO3 – H+ + Hb Hb•H Cellular respiration in peripheral tissues VENOUS BLOOD Alveoli Red blood cell Capillary endothelium Cell membrane H2CO3 CA
- 28. Carbon Dioxide Transport in the Blood CO2 CO2 Dissolved CO2 (7%) Dissolved CO2 Dissolved CO2 CO2 + Hb Hb + CO2 Hb•CO2 (23%) Hb•CO2 CO2 + H2O HCO3 – HCO3 – in plasma (70%) H+ + Hb Hb•H Cl– Cellular respiration in peripheral tissues VENOUS BLOOD Alveoli Transport to lungs Red blood cell Capillary endothelium Cell membrane H2CO3 CA
- 29. Carbon Dioxide Transport in the Blood CO2 CO2 Dissolved CO2 (7%) Dissolved CO2 Dissolved CO2 CO2 + Hb Hb + CO2 Hb•CO2 (23%) Hb•CO2 CO2 + H2O H2CO3 HCO3 – HCO3 – HCO3 – in plasma (70%) HCO3 – in plasma H+ + Hb Hb•H H+ + HbHb•H Cl– Cl– Cellular respiration in peripheral tissues VENOUS BLOOD Alveoli Transport to lungs Red blood cell Capillary endothelium Cell membrane H2CO3 CA Reverse chloride shift H+ disassociate H+ combine to form carbonic acid
- 30. Carbon Dioxide Transport in the Blood CO2 CO2 Dissolved CO2 (7%) Dissolved CO2 Dissolved CO2 CO2 + Hb Hb + CO2 Hb•CO2 (23%) Hb•CO2 CO2 + H2O H2O + CO2H2CO3 HCO3 – HCO3 – HCO3 – in plasma (70%) HCO3 – in plasma H+ + Hb Hb•H H+ + HbHb•H Cl– Cl– Cellular respiration in peripheral tissues VENOUS BLOOD Alveoli Transport to lungs Red blood cell Capillary endothelium Cell membrane H2CO3 CA CA
- 31. Gas Transport: Summary Gases move down their pressure gradients at the lungs and tissue capillaries
- 32. Reflex Control of Ventilation
- 33. Regulation of Ventilation Carotid body oxygen sensor releases neurotransmitter when PO2 decreases
- 34. Regulation of Ventilation Central chemoreceptors monitor CO2 in cerebrospinal fluid
- 35. Regulation of Ventilation Chemoreceptors in the brain and outside the CNS response to increased PCO2