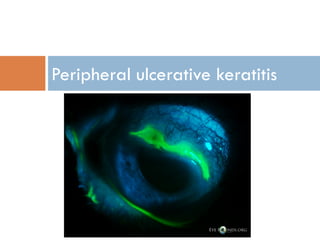
Peripheral Ulcerative Keratitis ( PUK )
- 2. Definition Term used to describe a group of destructive inflammatory diseases involving the peripheral cornea whose final common pathway is characterized by sloughing of corneal epithelium and keratolysis. Crescent-shaped, juxtalimbal corneal stroma associated with an epithelial defect, presence of stromal inflammatory cells, and stromal degradation. Conjunctival, episcleral, and scleral inflammation are usually evident Up to 50% related to systemic disorders May progressive circumferentially to involve entire cornea May progress to corneal melting leading to perforation
- 3. WHY IN PERIPHERAL CORNEA ? Peripheral cornea Unique anatomical & immunological features The peripheral cornea is adjacent to the vascularized limbus Close to sclera / episclera / conjunctiva Unlike the avascular central cornea, the peripheral cornea is closer to limbal conjunctiva and derives part of its nutrient supply from the limbal capillary arcade, a source of immunocompetent cells. Associated with sub conjunctival lymphaticsafferent arm ↑ IgM in periphery large ↑ Langerhans cells Reservoir of inflammatory cells More susceptible to immunological damage
- 4. What is the Pathogenesis? The peripheral cornea is adjacent to the vascularized posterior limbus Capillary arcades extend 0.5mm into clear cornea The peripheral cornea and nearby limbus are unique in their cellular milieu Peripheral Cornea has more Langerhans cells, higher concentrations of IgM, and complement (C1)’
- 5. .Antigen-presenting cells that express class IIMHC antigens are capable of mobilization and induction of T cell responses. Circulating immune cells, immune complexes,and complement factors tend to depositadjacent to the terminal capillary loops of thelimbal vascular arcades They produce collagenase. Vasculitic processes also cause damage to vessel walls This produces a variety of immune phenomena that manifest in the peripheral cornea
- 6. Differential diagnosis Non infectious Mooren ulcer, Terrien marginal degeneration, pellucid marginal degeneration, and furrow degeneration, marginal keratitis, blepharitis, contact lens use, chemical injury to the eyes, trauma. infectious Bacterial (staph,strept,Gonoco ccus) Viral (HS,HZ) Amebic(Acanthamoe ba) Fungal OCULAR Collagene vascular disease/vasculitis Other systemic autoimmune:Sjogrens syndrome ,Sarcoidosis(very rare),inflammatory bowel disease . -Malegnancies/leukemia Gonorrhea,Bacillary dysentery,T.B,lyme(ver y rare),VZ,Helminthiasis SYSTEMIC
- 7. History PUK is frequently a manifestation of an occult systemic disease. chief complaint/characteristics of present illness/past medical history/ family history/and a meticulous review of systems. Ocular symptoms vary, but nonspecific foreign body sensation with or without eye pain, tearing, photophobia, and reduced visual acuity (secondary to induced irregular astigmatism), are the most common symptoms for patients with PUK .Loss of vision can occur quickly when PUK progresses. PUK associated with RA, WG, PAN, and RP is often linked with scleritis, and eye pain may be pronounced in these individuals. PUK in patients with Mooren ulcer may also produce pain, although there is no scleral involvement. Bilateral disease may be present in 21% of patient
- 8. RA, SLE, PAN, WG, or RP may present with the following symptoms, which should be emphasized in the review of systems :General - Constitutional symptoms, such as chills, fever, poor appetite, recent weight loss, and fatigue Skin - Rashes, nodules, vesicles, ulcer, nail changes, and periungual infarcts Respiratory - Coughing, wheezing, pneumonia, and shortness of breath Cardiac - Chest pain or discomfort and dyspnea Gastrointestinal - Abdominal pain, nausea, vomiting, difficulty swallowing, and diarrhea Musculoskeletal - Muscle or joint pain, arthritis, back pain, and limitation of motion Neurologic - Headaches, seizures, psychiatric, paralysis, and numbness/tingling Other systemic symptoms - Deafness, swollen ear lobes, ear infections, )vertigo, and noises in ears (suggestive of RP
- 9. Ocular&Systemic Examination Physical Examination should be complete and include an overview of the head (including the nose, mouth, and external ear), trunk, joints, and extremities. Skin lesions should also be noted. Ocular Examination A complete ophthalmic examination should be performed with special emphasis on the conjunctiva, sclera, and cornea. Anterior chamber, vitreous, and fundus examinations are also important. slit lamp examination reveals a crescent-shaped destructive lesion of the juxtalimbal corneal stroma associated with an epithelial defect, stromal yellow-white infiltrates composed of inflammatory cells, and varying degrees of corneal stromal thinning (minimal to full thickness) adjacent to the limbus.in severe cases, the peripheral cornea is progressively destroyed circumferentially and centrally. PUK accompanied by necrotizing scleritis almost always indicates the presence of a potentially lethal systemic disease.The anterior chamber should be evaluated for depth and inflammation.A posterior segment examination is typically indicated to help determine the underlying etiology.
- 10. Examination of lids Blepharitis Telengiectasis (rosaecae) Posterior segment examination Posterior scleritis Vasculitis of CVD
- 11. Ocular Investigation Corneal scraping/culture Conjunctival biopsy Removes source of collagen Diagnosis of CVD fibrinoid necrosis,granulomas,vasculitis Diagnosis of Moorens justifies immune suppression in occult systemic disease
- 12. Systemic Investigations CBC ESR CRP URINE ANALYSIS RF ANA (SLE/RA) C ANCA (96% WG) ANTI-ds DNA(SLE) C3/C4 LEVELS CIRCULATING IMMUNE COMPLEXES CHEST X-RAY SINUSES (X-RAY / CT SCAN) HEPATITIS B,C Ag
- 13. Medical therapy Ocular Preservative free artificial tears, closure of puncta with plugs or cautery, and bandage soft contact lenes are used to treat associated dry eye and promote epithelialization of the ulcer. Cyanoacrylate adhesive may be applied to the ulcer bed to limit ulceration in cases of impending perforation. This may also prevent influx of white blood cells from the tear film. Amniotic membrane. If the perforation is in the very periphery of the cornea, you can create a conjunctival bridge over it Topical antibiotics are used to prevent bacterial superinfection
- 14. Systemic Systemic immunosuppression is often required to control ocular inflammation. Initial treatment initially is with steroids in the form of prednisone (1 mg/kg/day) or methylprednisolone (1 g/day x 3 days). Steroid sparing agents are indicated in the case of impending perforation, disease uncontrolled with steroids, or patients with associated rheumatoid arthritis as they are at increased risk for vascular events. Steroid sparing agents include antimetabolites such as methotrexate, azathioprine, or mycophenolate mofetil, T cell inhibitors such as cyclosporine or tacrolimus, alkylating agents such as cyclospophosphamide and chlorambucil, and biologic agents such as 5- infliximab and rituximab.systemic tetracyclin
- 15. Medical follow up Medications and dosages are adjusted based on the level of clinical response. Systemic medications may be managed in collaboration with a Rheumatologist or other medical specialist
- 16. surgical intervention Indications for surgical intervention include corneal perforation or excessive corneal thinning with impending perforation. Surgical options include lamellar, penetrating or crescentric keratoplasty, as well as possible corneo-scleral keratoplasty with a partial thickness scleral resection in cases of sceral melting. Resection of the conjunctiva adjacent to the area of peripheral ulcerative keratitis may also be performed to limit inflammation originating from the conjunctiva.
- 17. Surgical follow up Close follow up after surgical intervention is necessary. Patients should be monitored for recurrence of disease as well as infection or rejection of the graft
- 18. Complications Complications include infection and perforation of the ulcer. Prognosis Visual prognosis is related to the severity of disease. Patients with associated systemic disease have an increased mortality rate from vascular events
- 19. Thinning in the 'Quiet' Eye Dellen are localized areas of thinning, or drying, of the peripheral cornea. Dellen are usually located adjacent to an area of tissue swelling, tissue growth, inflammation, or eyelid abnormality. These abnormalities may alter the eye's normal ability to spread the tear layer uniformly
- 20. Furrow degeneration: usually asymptomatic,may occur as an idiopathic condition in elderly as a lucid area separating corneal arcus from the limbus.Epithelium is intact, No vascularization,Corneal thinning may occur .May be associated with systemic diseases such as rheumatoid arthritis.. No treatment is required in idiopathic degenerations
- 21. Pellucid marginal degeneration have severe thinning, usually inferiorly, within a couple of millimeters of the limbus. Though there's no redness, pain or inflammation, it causes significant irregular astigmatism, so the patient tends to complain of a slow, progressive worsening of vision." On topography, PMD will have an area of inferior steepening that resembles a crab claw, physicians note. "For PMD, glasses sometimes help, though the management typically involves a rigid gas permeable contact lens or a hybrid lens
- 22. Terrien's marginal degeneration. This presents as a marginal furrow, usually bilateral, and is most common in men between 20 and 40 years of age. It starts as a non-ulcerated area of thinning located superiorly, and it slowly progresses from there. "You'll see vascularization in addition to the thinning, often with a leading edge of lipid," However, the epithelium is also intact with this condition. The thinning can be progressive, and can progress circumferentially or centrally. And, since it starts superiorly, the patient usually gets against-the-rule astigmatism.
- 23. Thinning in the 'Hot' Eye no treatment for the thinning, you can manage the astigmatism with glasses or, failing that, RGPs or hybrid lenses you first assess the defect's size, location and whether it's associated with a hypopyon,""None of the immune conditions cause a hypopyon . if there's a hy- popyon, it's a bacterial infection until proven otherwise. "Scrape it, culture it . a non-infectious peripheral ulcerative keratitis, however, first suspect rheumatoid arthritis or another autoimmune condition such as wegner granulomatosis,hepatitis If Investigation is negative so think of mooren ulcer
- 24. Mooren's ulcer, or a peripheral ulcerative keratitis of unknown etiology. "Mooren's is typically more chronic, progressive and very painful,. "It will begin in the periphery and spread both circumferentially and centripetally. The key sign is that there will be a leading, undermined edge of de-epithelialized tissue. There will also usually be blood vessels crossing the edge.there's also a milder form of Mooren's ulcer that's more limited and actually responds well to medical therapy consisting of lubrication and low- dose steroids and tarsorraphy
- 25. THANK YOU