ASandler_UTI_TD.docx
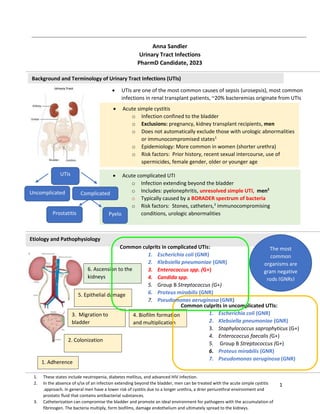
- 1. 1 CCVss Acute complicated UTI o Infection extending beyond the bladder o Includes: pyelonephritis, unresolved simple UTI, men2 o Typically caused by a BORADER spectrum of bacteria o Risk factors: Stones, catheters,3 immunocompromising conditions, urologic abnormalities Background and Terminology of Urinary Tract Infections (UTIs) Anna Sandler Urinary Tract Infections PharmD Candidate, 2023 Acute simple cystitis o Infection confined to the bladder o Exclusions: pregnancy, kidney transplant recipients, men o Does not automatically exclude those with urologic abnormalities or immunocompromised states1 o Epidemiology: More common in women (shorter urethra) o Risk factors: Prior history, recent sexual intercourse, use of spermicides, female gender, older or younger age 1. These states include neutropenia, diabetes mellitus, and advanced HIV infection. 2. In the absence of s/sx of an infection extending beyond the bladder, men can be treated with the acute simple cystitis .approach. In general men have a lower risk of cystitis due to a longer urethra, a drier periurethral environment and prostatic fluid that contains antibacterial substances. 3. Catheterization can compromise the bladder and promote an ideal environment for pathogens with the accumulation of fibrinogen. The bacteria multiply, form biofilms, damage endothelium and ultimately spread to the kidneys. UTIs Uncomplicated Complicated Pyelo Prostatitis Etiology and Pathophysiology 1. Adherence 2. Colonization 3. Migration to bladder 4. Biofilm formation and multiplication 5. Epithelial damage 6. Ascension to the kidneys UTIs are one of the most common causes of sepsis (urosepsis), most common infections in renal transplant patients, ~20% bacteremias originate from UTIs Common culprits in uncomplicated UTIs: 1. Escherichia coli (GNR) 2. Klebsiella pneumoniae (GNR) 3. Staphylococcus saprophyticus (G+) 4. Enterococcus faecalis (G+) 5. Group B Streptococcus (G+) 6. Proteus mirabilis (GNR) 7. Pseudomonas aeruginosa (GNR) Common culprits in complicated UTis: 1. Escherichia coli (GNR) 2. Klebsiella pneumoniae (GNR) 3. Enterococcus spp. (G+) 4. Candida spp. 5. Group B Streptococcus (G+) 6. Proteus mirabilis (GNR) 7. Pseudomonas aeruginosa (GNR) The most common organisms are gram negative rods (GNRs)
- 2. 2 Directed antimicrobial therapy Diagnosis and Presentation Simple UTI: o 1) Increased urinary frequency, urgency, dysuria, hematuria + 2) suspicion of urinary source Urinalysis (UA)4 o Can begin empiric antibiotics if meet these two criteria while waiting for urine cultures (cx) Do not need urine cx unless resistant organisms Complicated UTI: o Same s/sx as simple + Fever, chills, flank pain, sepsis with suspected urologic source, cystitis > 7 days, known antibiotic (abx) resistance, acute mental status changes High-risk groups: pediatrics, pregnancy, renal failure Treatment Principles 4. In women with typical acute simple cystitis symptoms, a UA is usually not necessary since pyuria is present in almost all women who present with acute cystitis. However, a UA can be helpful in determining alternative diagnoses. Differentials can include vaginitis, urethritis, and pelvic inflammatory disease. Acute simple cystitis Complicated UTIs Special Populations, Asymptomatic Bacteriuria PK/PD properties General themes: Understand complicated versus uncomplicated infection Keep in mind risk of resistant organisms and reserve specific agents for them De-escalate and transition to oral agents when appropriate
- 3. 3 Acute simple cystitis Low risk resistance Nitrofurantoin Trimethorpim- sulfamethoxazole Fosfomycin Alternatives: Oral beta lactams: Cefdinir, Cefpodoxime, Amoxicillin/Clavulanate FLQs High risk resistance Nitrofurantoin Fosfomycin Treat based off cx Empiric Treatment of Acute Simple Cystitis Depends on risk of infection with multidrug-resistant gram-negative organisms (MDROs) o Prior urinary isolates o Inpatient stays at health-care facilities o Use of broad-spectrum agents Fluoroquinolones (FLQs) Third or fourth generation cephalosporins o Obtain urine cx for high-risk patients and proceed to directed antimicrobial selection
- 4. 4 Drug MOA and coverage Dose and Duration Pearls Nitrofurantoin Coverage: GNRs, Enterococci, S. saprophyticus, Group B strep. Inhibits bacterial enzymes 100 mg PO BID X 5-7 days (Macrobid) 50-100 mg Q6H X 5- 7 days (Macrodantin) Avoid in pyelo due to poor concentration outside the bladder Admin. With food Avoid if CrCl < 30 mL/min Monitoring: Pulmonary reaction, LFTs, renal function Fosfomycin Coverage: GNRs, (+ ESBLs!) Enterococci, (+ VRE) S. saprophyticus Inhibits bacterial enzymes Cell wall synthesis inhibitor 3-gram powder mixed in water X 1 dose Typically reserved due to coverage of resistant organisms Not renally dose adjusted ADRs: N/V, headache Trimethoprim- sulfamethoxazole (TMP/SMX) Coverage: MSSA, Strep spp. GNRs TMP: Inhibits dihydrofolic acid reduction SMP: Interferes with bacterial folic acid synthesis One double- strength (DS) tablet 160/800 mg PO BID X 3 days Monitoring: CBC, CMP, renal, function, LFTs. Amoxicillin- clavulanate Coverage: GNRs, anaerobes, strep spp. enterococci Beta lactam/beta lactamase inhibitor inhibit cell wall synthesis 500 mg PO BID X 5-7 days Renal dosing based on amoxicillin component ADRs: Diarrhea, Monitoring; Hypersensitivity reactions Cefdinir Coverage: GNRs, strep. spp. Cell wall synthesis inhibitor, 3rd gen cephalosporin 300 mg PO BID X 5-7 days Monitoring; Thrombocytopenia, hypersensitivity reactions Drug table: Acute Simple Cystitis Obtain urine cx from all and initiate empiric tx right away Empiric tx is dependent on: o Severity of illness o Risk factors for MDR o Host factors (+/- urologic abnormalities, etc.) o Prior susceptibilities and cultures, prior hx of extended-spectrum beta lactamase- (ESBL) or carbapenemase (CRE)-producing organisms. o Hx abx use Always keep in mind suspected culprits and resistant patterns Switch to appropriate oral regimen once sx improve and culture results return Empiric Treatment of Complicated Cystitis What organisms are we not covering? What organisms are not covered by cephalosporins ? Why is are CBC and CMP panels required for TMP/SMX?
- 5. 5 Drug MOA and Coverage Dose and Duration Pearls Meropenem Coverage: PsA, Anaerobes, GNRs (+ESBLs) strep, MSSA, Cell wall synthesis inhibitor 1 g IV every eight hours X 5-14 days Renally dose adjusted Has extended and continuous infusion methods Monitoring: Hypersensitivity, CNS toxicity Piperacillin/tazobactam Coverage: PsA Anaerobes, GNRs, GNRs (+ESBLs) strep, MSSA, Beta lactam/beta lactamase inhibitor 3.375 g IV every 6-8 hours X 5-14 days Pay attention to extended vs. conventional infusion methods and renal function Complicated Cystitis Critical illness/sepsis Anti-pseudomonal (PsA) carbapenem (imi or mero) + vanco/dapto/linezolid Reserved: fosfo, cefideroocol, combos Low risk MDROs Ceftriaxone or Piperacillin/Tazobactam (Pip/tazo) Alternatives: FLQs High risk MDROs Pip/tazo5 Cefepime Imi or mero Empiric Treatment of Complicated Cystitis Drug Table: Complicated Cystitis ESBLs are seen most commonly in? CREs are seen most commonly in?
- 6. 6 Drug MOA and Coverage Dose and Duration Pearls Ceftriaxone Coverage: GNRs, strep, 3rd generation cephalosporin 1 g IV once daily X 5-14 days Not renally dose adjusted Monitoring: Hypersensitivity reactions Cefepime Coverage: PsA Anaerobes, GNRs, GNRs strep spp., 4th generation cephalosporin 2 g IV every 12 hours X 5-14 days Avoid if patients have risk-factors for ESBL- producing organisms Monitoring: Thrombocytopenia, hypersensitivity reactions Vancomycin Coverage: Gram positive organisms only: MRSA, strep. Spp., enterococci, Follow institutional dosing protocols Monitoring: Renal function Linezolid Coverage: Gram positive organisms only: MRSA, strep. Spp., enterococci (+ VRE) Bacterial protein synthesis inhibitor 600 mg IV every 12 hours X 7-10 days ADRs: Diarrhea, decreased white blood cell count, increased serum lipase, anemia, thrombocytopenia, peripheral/optical neuropathy Not renally dose adjusted Ciprofloxacin Coverage: Atypicals, strep spp. Enterococci, GNRs, PsA DNA gyrase inhibitor breakage of DNA 400 mg IV every 12 hours X 5-7 days Monitoring: QTc, drug- drug interactions, neuropathy, tendon rupture, CBC, LFTs and renal function, glucose Avoid in those with a hx of myasthenia gravis Ceftazidime-avibactam (Avycaz) Coverage: PsA Anaerobes, GNRs, GNRs (+ESBLs) strep, carbapenem- resistant enterobacterales (CREs) 2.5 g Every 8 hours X 5- 14 days Monitoring: anaphylaxis after first dose, renal function Cefiderocol (Fetroja) Coverage: GNRs, PsA, CREs, 2 g IV every 8 hours X 5- 14 days Monitoring: LFTs, CMP, neurotoxicity Renally dose adjusted,
- 7. 7 Bacteria Agents Notes GNRs Levofloxacin 750 mg PO once daily Ciprofloxacin 500 mg PO BID or 1000 mg ER PO once daily TMP-SMX One DS tab PO BID Oral beta lactams may be less effective but may be appropriate alternatives Enterococcus Amoxicillin 500 mg PO every 8 hours or 875 mg BID PsA Simple cystitis: Fosfomycin, ciprofloxacin Complicated: Ciprofloxacin Duration in acute simple: 3-5 days Pyelonephritis duration: 2-3 weeks Staphylococcus TMP-SMX One DS tab PO BID S. aureus is an uncommon isolate but when present, blood cultures should be sent to r/o bacteremia Directed antimicrobial therapy Acute simple cystitis: o Often times only treated empirically unless there is risk of resistance Complicated UTIs o Often times, broad-spectrum regimens can be replaced with narrow-spectrum agents Always try to tailor to susceptibility results
- 8. 8 •Mainly gram negative organisms (E. coli, PsA, Enterobacter, Klebsiella) •Simple or complex •Prophylaxis:TMP/SMX (alternatives: atovaquone, nitrofurantoin, cephalexin) six months-one year post- transplant •Simple: Oral agents (cipro, nitro,cefdinir, amoxicillin-clavulanate) X 10-14 days or 5-7 days if > 6 months post-transplant •Complicated: Cover PsA (Pip/Tazo 4.5 g IV every six hours, Meropenem, vancomycin + cefepime) X ?14-21 days Kidney Transplant Recipients5 •Lack of treatment benefits in most •Special populations: Pregnancy, Renal Transplant recipients, Planned urologic interventions •Pregnancy: Beta-lactams, nitro, fosfo, TMP/SMX6 X 5-7 days Asymptomatic Bacteruria •Acute Empiric: Cover gram-negative organisms: Oral- TMP/SMX or FLQ; IV-FLQ +/- AMG or beta-lactam treated up to 4 weeks •Consider N. gonorrhoeae and C. trachomatis coverage in select populations7 •Chronic empiric: FLQ 8 > TMP/SMX, macrolide, doxycycline or oral beta-lactams X 4-6 weeks (TMP/SMX > 6 weeks), fosfo Acute and Chronic Prostatatitis •Education: Increased fluid intake, frequent voiding, contraception modification •Continous prophylaxis for recurrent simple cystitis in females: Nitro, TMP/SMX with lower doses < treatment Reccurent UTIs and Education Special Populations and Asymptomatic Bacteriuria 5. Kidney transplant recipients are susceptible to UTIs due to absence of a sphincter between the transplanted ureter and the native bladder. Ureteral stents that are placed during transplantation serve as reservoirs for bacteria, placing patients at higher risks of recurrent UTIs. The highest risk of developing a UTI is believed to be within the first month after transplant. 6. Avoid during first trimester and at term but only appropriate during these periods when the alternatives cannot be used. 7. Men < 35 y/o who are sexually active and men >35 who engage in high-risk sexual behavior. 8. FLQs have better penetration into prostatic fluid; the prostatic fluid has a low pH, resulting in higher concentrations of drugs with alkaline pKas. Do not use prophylactic agents for tx!
- 9. 9 1. Harris PNA, Tambyah PA, Lye DC, et al. Effect of Piperacillin-Tazobactam vs Meropenem on 30- Day Mortality for Patients With E coli or Klebsiella pneumoniae Bloodstream Infection and Ceftriaxone Resistance: A Randomized Clinical Trial. JAMA. 2018;320(10):984. doi:10.1001/jama.2018.12163 2. Gupta K, Hooton TM, Naber KG, et al. International Clinical Practice Guidelines for the Treatment of Acute Uncomplicated Cystitis and Pyelonephritis in Women: A 2010 Update by the Infectious Diseases Society of America and the European Society for Microbiology and Infectious Diseases. Clinical Infectious Diseases. 2011;52(5):e103-e120. doi:10.1093/cid/ciq257 3. Bono MJ, Leslie SW, Reygaert WC, Doerr C. Urinary Tract Infection (Nursing). In: StatPearls. StatPearls Publishing; 2022. Accessed September 4, 2022. http://www.ncbi.nlm.nih.gov/books/NBK568701/ 4. Flores-Mireles AL, Walker JN, Caparon M, Hultgren SJ. Urinary tract infections: epidemiology, mechanisms of infection and treatment options. Nat Rev Microbiol. 2015;13(5):269-284. doi:10.1038/nrmicro3432 UpToDate Links: 1. https://www.uptodate.com/contents/acute-complicated-urinary-tract-infection-including- pyelonephritis-in- adults?search=complicated%20cystitis%20treatment&source=search_result&selectedTitle=1~15 0&usage_type=default&display_rank=1#H2417976538 2. https://www.uptodate.com/contents/acute-simple-cystitis-in- women?search=urinary%20tract%20infection%20&source=search_result&selectedTitle=5~150& usage_type=default#H88979215 3. https://www.uptodate.com/contents/image?imageKey=ID%2F98083&topicKey=ID%2F8065&se arch=asymptomatic%20bacteriuria%20pregnancy&source=see_link 4. https://www.uptodate.com/contents/urinary-tract-infection-in-kidney-transplant- recipients?search=complicated%20uti%20&source=search_result&selectedTitle=9~113&usage_ type=default#H1473408516 5. https://www.uptodate.com/contents/acute-bacterial- prostatitis?search=prostatitis%20treatment&source=search_result&selectedTitle=1~99&usage_ type=default&display_rank=1#H29437530 Picture Links: 1. https://www.niddk.nih.gov/health-information/diagnostic-tests/urinary-tract-imaging 2. https://www.labtestsguide.com/urine-culture 3. https://todayhealth24.com/the-main-causes-of-kidney-infection-and-treatment.html 4. https://infectionsinsurgery.org/core-elements-of-antibiotic-stewardship/ 5. https://www.nhsbt.nhs.uk/organ-transplantation/kidney/at-the-transplant-centre/kidney- transplant-surgery/ References
- 10. 10 Appendix Common pathogens in complicated and uncomplicated UTIs Ureteral stent placed during kidney transplantation
- 11. 11 Spectrum of beta-lactam resistance