ASandler_HF2022_IM_TD.docx
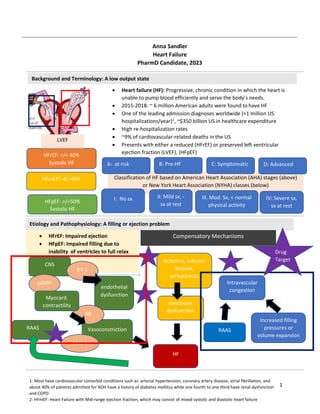
- 1. 1 Classification of HF based on American Heart Association (AHA) stages (above) or New York Heart Association (NYHA) classes (below) Background and Terminology: A low output state Etiology and Pathophysiology: A filling or ejection problem Anna Sandler Heart Failure PharmD Candidate, 2023 Heart failure (HF): Progressive, chronic condition in which the heart is unable to pump blood efficiently and serve the body’s needs. 2015-2018: ~ 6 million American adults were found to have HF One of the leading admission diagnoses worldwide (>1 million US hospitalizations/year)1 , ~$350 billion US in healthcare expenditure High re-hospitalization rates ~9% of cardiovascular-related deaths in the US Presents with either a reduced (HFrEF) or preserved left ventricular ejection fraction (LVEF), (HFpEF) 1: Most have cardiovascular comorbid conditions such as arterial hypertension, coronary artery disease, atrial fibrillation, and about 40% of patients admitted for ADH have a history of diabetes mellitus while one fourth to one third have renal dysfunction and COPD 2: HFmEF: Heart Failure with Mid-range ejection fraction, which may consist of mixed systolic and diastolic heart failure HFrEF: </= 40% Systolic HF HFmEF2 : 41-49% HFpEF: >/=50% Systolic HF I: No sx II: Mild sx, - sx at rest III. Mod. Sx, < normal physical activity IV: Severe sx, sx at rest A: at-risk B: Pre-HF C: Symptomatic D: Advanced LVEF Vasoconstriction endothelial dysfunction Ischemia, valvular disease, arrhythmias Ionotropic dysfunction Increased filling pressures or volume expansion Intravascular congestion HF Drug Target Compensatory Mechanisms HFrEF: Impaired ejection HFpEF: Impaired filling due to inability of ventricles to full relax CNS ET-1 NE cAMP Myocard. contractility RAAS ANG II RAAS
- 2. 2 Mechanism S/sx Fluid accumulation Dyspnea, orthopnea, edema, abdominal discomfort, exercise intolerance Fluid on CXR Increased NT-proBNP Low output state Fluid-filled lungs Cardiomegaly Hypotension Right-sided heart failure Hepatomegaly Elevated Jugular Venous Pressure Physical Exam Pitting edema HFmEF Non-pharm Rusk factors, Presentation, and Diagnosis Increased congestion+ adrenergic activity Increased wall stretch Increased ANP and BNP Increased NT- proBNP HFpEF rsik factors: Aging, hypertension, obesity, diabetes HFrEF risk factors: Smoking, Ischemic heart disease Right-sided heart failure risk factors: Left-sided heart failure, congenital defects BNP and NT-proBNP can both assist in diagnosing HF3 NT-proBNP preferred o ARNi: neprilysin degrades BNP Diagnosis= clinical features + ECHO+ Serum natriuretic peptides NT-proBNP > 125 pg/mL BNP >/= 35 pg/mL General Treatment Principles HFrEF HFpEF Guideline- directed medical therapy (GDMT) It is important to identify the cause of HF o Genetic, infectious, endocrine, medications4 Specific treatments based off HF stages Keep in mind level of evidence behind each recommendation ARNi: Angiotensin receptor-neprilysin inhibitor BNP: B-type natriuretic peptide; ECHO: echocardiogram, NT-proBNP: N-terminal pro-BNP 3. Not useful in patients with renal insufficiency due to accumulation-no clear cut-off values. Obesity is also associated with lower levels, reducing diagnostic sensitivity. There is also insufficient evidence for utilizing serial measurements for guiding treatments. Rather these levels can help assist diagnosis when the cause of dyspnea is unclear. Other causes may include myocarditis, renal failure, and atrial fibrillation. 4. These medications may include chemotherapies that cause cardiotoxicity (e.g., doxorubicin), TNF-alpha inhibitors
- 3. 3 Stage B LVEF </= 40% ACEi or ARB Evidence-based BB Metoprolol succinate Carvedilol Bisoprolol Recent MI or ACS Statin Heart Failure with Reduced Ejection Fraction: Stage B-Pre-HF Recall: This stage represents clinically asymptomatic structural and functional cardiac abnormalities that increase risk of developing symptomatic HF Goal: Prevent symptomatic HF in patients with structural and functional cardiac abnormalities ACS: Acute coronary syndrome; ACEi: Angiotensin converting enzyme inhibitor; ARB: angiotensin receptor blocker; BB: Beta Blocker CV: Cardiovascular; CVD: Cardiovascular disease; DMII: Diabetes Type II; MI: Myocardial infarction; SGLT2i: Sodium-Glucose 2 transport inhibitor Heart Failure with Reduced Ejection Fraction: Stage A-At risk for HF Blood pressure control SGLT2i to prevent hospitalizations o DMII + CVD or high-CV risk Regular physical activity Weight control
- 4. 4 Drug/Class Initial Dosing Target Dosing7 Indication and Pearls Mortality benefit ? ACE inhibitors Lisinopril: 2.5-5 mg PO once daily Enalapril: 2.5 mg PO BID Lisinopril: 20-40 mg PO once daily Enalapril: 10-20 mg PO BID When ARNi is not feasible NYHA II-IV (C-1, A) Angiotensin receptor blockers Losartan: 25-50 mg PO once daily Valsartan: 20-40 mg once daily Losartan: 50-150 mg PO once daily Valsartan: 160 mg PO BID Used in patients intolerant to ACEi or ARNi (C-1, A) Angiotensin receptor and Neprilysin Inhibitor: Sacubitril/Valsartan 49 mg/51 mg PO BID 97 mg/ 103 mg PO BID Sx+ NYHA II-III 36-hour washout period required when switching from an ACEi (C-1, A) PARADIGM-HF trial Beta Blockers Carvedilol: 3.125 mg PO BID Carvedilol: 25-50 mg PO BID Current or previous sx (C-1, A) Heart Failure with Reduced Ejection Fraction: GDMT Heart Failure with Reduced Ejection Fraction: Stages C and D-Roadmap Routine assessment, optimization, and titration MRA SGLT2i ACEi, ARB, or ARNi PRN diuretics5 Persistent sx, LVEF </= 40% GDMT: Titrated as appropriate very 1-2 weeks Hydralazine + Isosorbide dinitrate ICD CRT Refractory (Stage D) Palliative care Transplant BB Consider Additional Txs
- 5. 5 Metoprolol succinate: 12.5-25 mg PO once daily Metoprolol: 200 mg PO once daily Do not delay therapy even when patients are asx COPERNICIS MERIT-HF trials MRA Spironolactone: 12.5-25 mg PO once daily Eplerenone: 25 mg PO once daily Spironolactone: 25- 50 mg PO once daily Eplerenone: 50 mg PO once daily NYHA II-IV eGFR > 30 mL/min/1.73m2 K < 5.0 mEq/L (C1-A) (C-1, A) RALES and EMPHASIS-HF trials SGLT2i Dapagliflozin: 10 mg PO once daily Empagliflozin: 10 mg PO once daily N/A Symptomatic, chronic HFrEF (C-1, A) EMPEROR- REDUCED DAPA-HF Loop diuretics Bumetanide: 0.1-1.0 mg once or twice Furosemide: 20-40 mg once or twice Torsemide: 10-20 mg once Bumetanide total daily dose (TDD): 10mg Furosemide TDD: 600 mg Torsemide: 200 mg Monitoring: Renal function, CMP, BP, relief of congestion The OPTIMIZE HF study6 Reduced 30-day mortality and hospitalizations Improved QOL Thiazide diuretics Chlorthalidone: 12.5-25 mg once Hydrochlorothiazide (HCTZ): 25 mg once or twice Chlor: 100 mg HCTZ: 200 mg Congestive sx+ unresponsive to loop diuretics Drug Initial dose Target Dose Indication and Pearls Mortality Benefit? Isosorbide dinitrate and hydralazine Fixed dose: 20 mg/37.5 mg PO TID Fixed dose: 40 mg/75 mg TID African American+ NYHA III-IV + GDMT OR if unable to receive ARNi, ACEi, or ARB (2b, C) Lots of ADRs and thus low usage Monitoring: hypotension, palpitations, dizziness, fluid/Na retention, bradycardia, V-HeFT I and A-HeFT trials8 Heart Failure with Reduced Ejection Fraction: Hydralazine+ Isosorbide Dinitrate CMP: Complete metabolic panel; K: Potassium; MRA: Mineralocorticoid receptor antagonist; 5. Consider maintenance diuretics in any patient with a history of congestion in order to avoid recurrent symptoms. 6. Non-randomized registry trial 7. Doses should be titrated to prevent the CV outcomes of HF, rather than to achieve a specific goal (e.g, BP) 8. However, benefit in these trials was seen at doses higher than what is typically used in practice with short-acting nitrates. Heart Failure with Reduced Ejection Fraction: Additional Medical Therapies for Stage C
- 6. 6 Drug/MOA Starting Dose Target Dose Indications and Pearls Mortality benefits? Ivabradine/If Channel Inhibitor within sinoatrial note prolonged depolarization and slowed firing reduced HR 5 mg PO BID 7.5 mg PO BID NYHA II-III + LVEF </=35% + GDMT w/ max dose BB+ NSR + HR >/=70 BPM (2a, B-R) Monitoring: HR, BP, EKG (afib) CI in heart black, concomitant use with strong CYP3A4 inhibitors SHIFT trial: Greatest benefit in hospitalizations Benefit results from the reduction in HR Digoxin 0.125-0.25 mg PO daily Individualize doses to maintain conc. 0.5-< 0.9 ng/mL Symptomatic HFrEF despite GDMT (2b-BR) May decrease hospitalizations The DIG trial Vericiguat Guanylyl cyclase stimulator increased cGMP vasodilation, improved endothelial function 2.5 mg PO once daily 10 mg PO once daily NYHA II-IV; LVEF < 45%; recent hospitalization or IV diuretic use; elevated NP levels GDMT/intolerance (2b, B-R) Monitoring: BP, daily weights Warning: Not studied in patients with longer-acting nitrates or PDE-5 inhibitors VICTORIA trial: Reduction in composite of hospitalizations or CV-death
- 7. 7 Symptomatic HFmEF PRN diuretics SGLT2i ACEi, ARB, or ARNi MRA BB Symptomatic HFpEF PRN diuretics SGLT2i ARNi MRA ARB Drug Indications Evidence and Pearls SGLT2i: Empagliflozin 2a, B-R Reduce HF hospitalizations +CV mortality EMPEROR Preserved trial MRA 2b, B-R Reduce HF hospitalizations TOP-CAT trial ARB 2b, B-R Reduce HF hospitalizations CHARM Trail ARNi 2b, B-R Reduce HF hospitalizations PARAGON-HF trial Drug Recommendation Evidence and Pearls SGLT2i: Empagliflozin 2a, B-R Reduce HF hospitalizations +CV mortality EMPEROR Preserved trial BBs: Evidence- based 2b, B-NR Reduce HF hospitalizations +CV mortality ACEi, or ARB 2b, B-NR Reduce HF hospitalizations +CV mortality CHARM Trail ARNi 2b, B-NR Reduce HF hospitalizations +CV mortality PARAGON-HF trial MRA 2b, B-NR Reduce HF hospitalizations +CV mortality TOP-CAT trial (+) HTN pts. What about dapagliflozin? What are the limitations and errors associated with post-hoc analyses? RCT: Randomized controlled trials Heart Failure with Mildly Reduced or Preserved Ejection Fraction No prospective RCTs Patients on lower end of LVEF spectrum (LVEF 41-49%) respond similarly as HFrEF patients Patients should have repeat LVEF evaluation to determine trajectory of disease process Titrate medications to achieve BP targets Manage comorbidities (e.g., atrial fibrillation) to improve sx
- 8. 8 HF Drug 2017 Recommendation 2022 recommendation HFrEF ARNi ARNi only if cannot do ACEi or ARB ARNi > ACEi or ARB HFrEF SGLT2i ? SGLT2i as initial GDMT HFpEF SGLT2i ? SGLT2i could be used HFpEF ACEi, ARB BBs May be considered (2b-C) May be reasonable (2b- BR) – the BBs HFpEF MRA ? May be considered but confirmatory studies needed Might be considered to decrease hospitalizations (2b-BR) 1. Yancy CW, Jessup M, Bozkurt B, et al. 2017 ACC/AHA/HFSA Focused Update of the 2013 ACCF/AHA Guideline for the Management of Heart Failure: A Report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines and the Heart Failure Society of America. Circulation. 2017;136(6). doi:10.1161/CIR.0000000000000509 2. Heidenreich PA, Bozkurt B, Aguilar D, et al. 2022 AHA/ACC/HFSA Guideline for the Management of Heart Failure. Journal of the American College of Cardiology. 2022;79(17):e263-e421. doi:10.1016/j.jacc.2021.12.012 3. Solomon SD, McMurray JJV, Anand IS, et al. Angiotensin–Neprilysin Inhibition in Heart Failure with Preserved Ejection Fraction. N Engl J Med. 2019;381(17):1609-1620. doi:10.1056/NEJMoa1908655 4. McMurray JJV, Packer M, Desai AS, et al. Angiotensin–Neprilysin Inhibition versus Enalapril in Heart Failure. N Engl J Med. 2014;371(11):993-1004. doi:10.1056/NEJMoa1409077 5. Packer M, Anker SD, Butler J, et al. Cardiovascular and Renal Outcomes with Empagliflozin in Heart Failure. N Engl J Med. 2020;383(15):1413-1424. doi:10.1056/NEJMoa2022190 6. Wollert KC, Drexler H. Carvedilol Prospective Randomized Cumulative Survival (COPERNICUS) Trial: Carvedilol as the Sun and Center of the β-Blocker World? Circulation. 2002;106(17):2164-2166. doi:10.1161/01.CIR.0000038702.35084.D6 7. Taylor AL, Ziesche S, Yancy C, et al. Combination of Isosorbide Dinitrate and Hydralazine in Blacks with Heart Failure. N Engl J Med. 2004;351(20):2049-2057. doi:10.1056/NEJMoa042934 8. Malik A, Brito D, Vaqar S, Chhabra L. Congestive Heart Failure. In: StatPearls. References Blast from the Past: What has changes from the 2017 Focused Update Guidelines?
- 9. 9 StatPearls Publishing; 2022. Accessed September 7, 2022. http://www.ncbi.nlm.nih.gov/books/NBK430873/ 9. McMurray JJV, Solomon SD, Inzucchi SE, et al. Dapagliflozin in Patients with Heart Failure and Reduced Ejection Fraction. N Engl J Med. 2019;381(21):1995-2008. doi:10.1056/NEJMoa1911303 10. Effect of metoprolol CR/XL in chronic heart failure: Metoprolol CR/XL Randomised Intervention Trial in-Congestive Heart Failure (MERIT-HF). The Lancet. 1999;353(9169):2001-2007. doi:10.1016/S0140-6736(99)04440-2 11. Cohn JN, Archibald DG, Ziesche S, et al. Effect of Vasodilator Therapy on Mortality in Chronic Congestive Heart Failure. N Engl J Med. 1986;314(24):1547-1552. doi:10.1056/NEJM198606123142404 12. Yusuf S, Pfeffer MA, Swedberg K, et al. Effects of candesartan in patients with chronic heart failure and preserved left-ventricular ejection fraction: the CHARM-Preserved Trial. Lancet. 2003;362(9386):777-781. doi:10.1016/S0140-6736(03)14285-7 13. Anker SD, Butler J, Filippatos G, et al. Empagliflozin in Heart Failure with a Preserved Ejection Fraction. N Engl J Med. 2021;385(16):1451-1461. doi:10.1056/NEJMoa2107038 14. Zannad F, McMurray JJV, Krum H, et al. Eplerenone in Patients with Systolic Heart Failure and Mild Symptoms. N Engl J Med. 2011;364(1):11-21. doi:10.1056/NEJMoa1009492 15. Fonarow GC, Abraham WT, Albert NM, et al. Organized program to initiate lifesaving treatment in hospitalized patients with heart failure (OPTIMIZE-HF): rationale and design. American Heart Journal. 2004;148(1):43-51. doi:10.1016/j.ahj.2004.03.004 16. Pitt B, Pfeffer MA, Assmann SF, et al. Spironolactone for Heart Failure with Preserved Ejection Fraction. N Engl J Med. 2014;370(15):1383-1392. doi:10.1056/NEJMoa1313731 17. The Effect of Digoxin on Mortality and Morbidity in Patients with Heart Failure. N Engl J Med. 1997;336(8):525-533. doi:10.1056/NEJM199702203360801 18. Pitt B, Zannad F, Remme WJ, et al. The Effect of Spironolactone on Morbidity and Mortality in Patients with Severe Heart Failure. N Engl J Med. 1999;341(10):709-717. doi:10.1056/NEJM199909023411001 19. Armstrong PW, Pieske B, Anstrom KJ, et al. Vericiguat in Patients with Heart Failure and Reduced Ejection Fraction. N Engl J Med. 2020;382(20):1883-1893. doi:10.1056/NEJMoa1915928 UpToDate Link https://www.uptodate.com/contents/natriuretic-peptide-measurement-in-heart- failure?search=bnp%20and%20probnp&source=search_result&selectedTitle=1~150&usage_type=defaul t&display_rank=1#H4