2 microcytic anemia i-iron deficiency.ppt
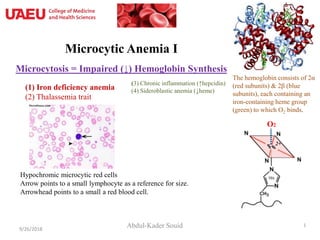
- 1. Microcytic Anemia I Microcytosis = Impaired (↓) Hemoglobin Synthesis Abdul-Kader Souid9/26/2018 1 Hypochromic microcytic red cells Arrow points to a small lymphocyte as a reference for size. Arrowhead points to a small a red blood cell. (3) Chronic inflammation (↑hepcidin) (4) Sideroblastic anemia (↓heme)(1) Iron deficiency anemia (2) Thalassemia trait The hemoglobin consists of 2α (red subunits) & 2β (blue subunits), each containing an iron-containing heme group (green) to which O2 binds. O2 2+
- 2. Iron Deficiency Anemia (‘hypochromic microcytic anemia’) 9/26/2018 2 Normal Iron deficiency anemia showing hypochromic (pale) red cells, some small (microcytic) red cells, ↑size variation (anisocytosis, ↑RDW)
- 3. Microcytosis (MCV <80 fL) Microcytosis =↓hemoglobin synthesis (↓iron, ↓globin, or ↓protoporphyrin): • Iron deficiency (iron-limiting erythropoiesis; nutritional vs. blood loss) • Thalassemia trait (↓a or b globin synthesis) • Inflammation (↓Fe bioavailability due to ↑hepcidin [blocks Fe absorption]) • ↓Protoporphyrin (hereditary sidroblastic anemia) 9/26/2018 3 Must know
- 4. Intestinal Iron Absorption Heme can be taken up by endocytosis (heme carrier protein 1, HCP1) and Fe2+ is liberated in the lysosome into the enterocyte. Fe3+ is reduced to Fe2+ by duodenal ferrireductase cytochrome b (dcytb) and transported via the divalent metal-ion transporter-1 (DMT-1) into the enterocyte. Vitamin C also reduces Fe3+ to Fe2+. Enterocyte Fe2 is exported into the blood by ferroportin or stored as ferritin. Hepcidin blocks ferroportin. Fe2 in blood is carried by transferrin (Fe2Tf). Must Know: Ferroportin → Releases Fe2+ from enterocytes and macrophages into the blood. Hepcidin binds to ferroportin → Retains Fe2+ inside enterocytes and macrophages. 9/26/2018 4 HO, heme oxygenase Fe2Tf, diferric transferrin Blocked by hepcidin
- 5. Hepcidin ↓ Iron Bioavailability • Hepcidin is a 25-amino-acid protein. • It prevents the release of iron from enterocytes and macrophages by binding to ferroportin. – Once hepcidin is bound to ferroportin, the ferroportin undergoes proteolysis. – With membrane ferroportin depleted, Fe cannot be transported into the blood. • Inflammation → ↑hepcidin → iron-deficiency anemia • Hypoxia → ↓hepcidin → ↑Fe bioavailability → polycythemia 9/26/2018 5 Must Know
- 6. 9/26/2018 6 • Ferritin is a measure of stored iron. • Serum iron is a measure of circulating iron bound to transferrin. • Total iron binding capacity (TIBC) is a measure of transferrin capacity to bind iron. • Percent transferrin saturation = serum iron ÷ TIBC. Serum Iron Studies serum iron UIBC TIBC Must watch video: https://www.youtube.com/watch?v=YczPj71BFPY Serum ferritin Serum iron Total iron binding capacity (TIBC) Per cent transferrin saturation Iron deficiency Low Low High Low Inflammation High Low Low Normal
- 7. Evolution of Iron Deficiency 9/26/2018 7 Prussian blue staining of marrow iron stores. Iron stores can be graded on a scale of 0 to 4+. A: a marrow with excess iron stores (>4+); B: normal stores (2–3+); C: minimal stores (1+); D: absent iron stores (0). Serum Iron
- 8. Iron Deficiency Anemia: Summary • Microcytic anemia with RDW and reticulocytopenia • Ferritin • Serum iron • TIBC (total iron binding capacity) • Transferrin saturation • ZPP (zinc protoporphyrin) • sTfR (serum transferrin receptor) Must Know Plasma ferritin <12 µg/L is indicative of absent iron stores.
- 9. Iron Deficiency Anemia Prevalence • Adult males <1% • Adult females 20% Mechanisms of iron deficiency • ↑ Need for iron: Infants during their rapid growth, premature infants, growth spurt during puberty, pregnancy, lactation, etc. • ↓ Iron intake (nutritional iron deficiency due to poor diet): Prolonged breastfeeding, iron-poor diet (vegetables and milk have low iron bioavailability). • ↑ Loss: Menorrhagia, GI bleeding (bleeding ulcer, colorectal cancer [fecal occult blood], infants on whole milk (milk-induced colitis), non-steroidal anti- inflammatory drug (NSAID)-induced gastritis, hereditary hemorrhagic telangiectasia (HHT). • ↓ Absorption (relatively rare): Gastric or duodenal resection, coeliac disease, etc. Notes: Iron absorption from meat is better than that from plants. Phytates (cereals, nuts, legumes) inhibit iron absorption. Vitamin C promotes Fe absorption. Must Know
- 10. Who gets Fe-deficiency and why? • Malabsorption – Stomach (resection; cancer; H. pylori; gastritis) – Duodenum (coeliac disease, resection) • Blood loss – Hiatus hernia, gastritis, peptic ulcer, H. pylori, esophageal varices, tumors, NSAID, telangiectasias, menstrual periods, hookworm, Ancylostoma caninum, nose bleeding. • Fe absorption from meat is better than from plants. – Phytates (cereals, nuts, legumes) inhibit absorption of non-hem Fe. – Vitamin C promotes hem Fe absorption. Pica
- 11. Patient 1 • An 18-month-old boy presents with pallor and irritability. For the last 6 months, his diet was whole milk. • Hemoglobin = 50 g/L, RBC = 2 x1012/L, reticulocyte count = 14 x109/L, MCV = 59 fL, and RDW = 21%. • Problem list: Microcytic anemia with increased RDW and reticulocytopenia, consistent with milk-induced iron deficiency. 9/26/2018 11 Normal Iron deficiency anemia
- 12. Principles of Treatment 1. Treating the primary cause of iron deficiency – Diet history – Identify the site of blood loss (e.g., menorrhagia, stool occult blood, endoscopy, colonoscopy, video capsule endoscopy) 2. Iron-rich food ± iron supplementation – Ferrous sulfate (FeSO4), 325 mg once to three times per day: • 120 to 180 mg elemental Fe/day (adults) • 2-6 mg/kg elemental Fe/day (children) • Treat 3 months after correction of anemia.
- 13. Required Reading • Harrison’s Online – Chapter 103 (Iron Deficiency) • Petry N, Olofin I, Hurrell RF, et al. The proportion of anemia associated with iron deficiency in low, medium, and high human development index countries: a systematic analysis of national surveys. Nutrients. 2016;8(11). pii: E693. • Amin SB, Orlando M, Wang H. Latent iron deficiency in utero is associated with abnormal auditory neural myelination in ≥ 35 weeks gestational age infants. J Pediatr. 2013;163:1267-71. • De-Regil LM, Jefferds ME, Sylvetsky AC, Dowswell T. Intermittent iron supplementation for improving nutrition and development in children under 12 years of age. Cochrane Database Syst Rev. 2011;12:CD009085. • Zimmermann MB, Hurrell RF. Nutritional iron deficiency. Lancet 2007;370:511–520. 9/26/2018 13
- 14. Optional Reading Total iron binding capacity (TIBC) is a colorimetric assay that uses two reagents sequentially. The first one is an acidic reagent that contains an iron-binding dye. The acidic pH causes transferrin to release all iron, which are captured by the iron- binding dye along, producing a colored complex. The second one, is a neutral reagent that raises the pH and restores transferrin’s affinity for iron. The transferrin extracts iron from the dye-iron complex and becomes 100% saturated. The decrease in absorbance of the colored dye-iron complex is measured spectrophotometrically at 660 nm and is directly proportional to the TIBC of the serum sample (http://www.randox.com/brochures/reagents/LT116.pdf). 9/26/2018 14