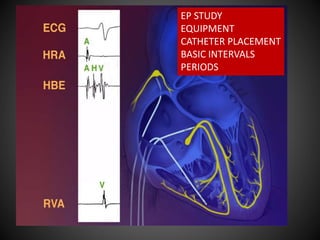
Electrophysiology study basics
- 1. EP STUDY EQUIPMENT CATHETER PLACEMENT BASIC INTERVALS PERIODS
- 3. EQUIPMENT • Radiographic Table, Image intensifier • Specialized EP equipment – Cardiac stimulator – Diagnostic and mapping catheters – Data monitor and recorder – RF energy generator • Temporary pacemaker, External pacemaker • External Defibrillator • Hemodynamic monitoring • Resuscitation equipment
- 4. PATIENT PREPARATION • Stopping Anti-arrhythmics – 2-3 days • Fasting – 6 hrs • IV access • ECG electrodes for 12 lead ECG and Monitoring • External Remote Defib pads • Indifferent skin electrode in RFA • Pulse Ox/NIBP/Invasive BP • Conscious sedation
- 5. EP CATHETERS
- 6. EP Catheters • Electrode catheters are used during EP testing for recording and pacing. • These catheters consist of insulated wires • At the distal tip of the catheter, each wire is attached to an electrode, which is exposed to the intracardiac surface. • Proximal end of the catheter, wire is attached to a plug, which can be connected to an external recording device • Woven Dacron or polyurethane.
- 7. EP Catheters Dacron Polyurethane Advantage of stiffness that helps maintain catheter shape with enough softness at body temperature that allows formation of loops cannot be easily manipulated and change shapes within the body expensive less expensive
- 8. EP Catheters • Electrode catheters come in different sizes -2 to 10 Fr. • In adults, sizes 5, 6, and 7 Fr catheters are the most commonly used • Recordings derived from electrodes can be unipolar (one pole) or bipolar (two poles). • The electrodes are typically 1 to 2 mm in length • The interelectrode distance can range from 1 to 10 mm or more • Catheters with a 2- or 5-mm interelectrode distance are most commonly used
- 12. NUMBER OF ELECTRODES 2mm2mm 5mm Quadrapolar 2-5-2 1234 Quadrapolar 5-5-5 Lum en 5mm5mm 5mm LUMEN 1234 4 3 2 1 2 (bipolar), 3 (tripolar), 4 (quadripolar), 6 (hexapolar), 8 (octapolar), 10 (decapolar), 20 (duodecapolar)
- 15. EP Catheters • Large number of multipolar electrode catheters have been developed - facilitate placement of the catheter in the desired place and fulfill various recording requirements. • Variety of preformed distal curve shapes and sizes. • Multipolar recording electrode catheters are placed within the coronary sinus (CS) or along the crista terminalis in the right atrium (RA) • Halo catheter is a multipolar catheter used to map reentrant electrical activity around the tricuspid annulus during RA macroreentry
- 16. Multipolar electrode catheters with different preformed curve shapes. Multipolar electrode catheters with different electrode numbers and curve shape. , Duodecapolar catheter, quadripolar catheter, and Halo catheter.
- 17. A decapolar catheter with a distal ring configuration (Lasso catheter) is used to record electrical activity from the pulmonary vein. Basket catheters capable of conforming to the chamber size and shape have also been used for mapping atrial and ventricular arrhythmias
- 20. EP Catheters • Catheters can have a fixed or deflectable tip • Steerable catheters (deflectable tip) allow deflection of the tip of the catheter in one or two directions in a single plane; some of these catheters have asymmetrical bidirectional deflectable curves • Radiofrequency ablation catheters have three different tips: 4 mm, 8 mm, and a cooled tip (ranging between 3.5 mm and 5 mm)
- 23. Ablation catheters with different tip electrode sizes and shapes. Left to right, Peanut 8-mm, 2-mm, 4-mm, and 8-mm tip electrodes. Deflectable multipolar electrode catheters with different curve sizes and shapes.
- 25. ANATOMY FOR EPS CATHETER PLACEMENT
- 26. Standard Catheter Electrodes • High RA – Quadripolar – Femoral route – Tip - superolateral – near SVC/RA junction
- 27. Standard Catheter Electrodes • RV apex – Quadripolar – Femoral route – Tip – as close to RV apex as possible
- 28. Standard Catheter Electrodes • Coronary Sinus – Decapolar – Easiest access via SVC - IJV/SCV route
- 29. Standard Catheter Electrodes • His Bundle – Quadripolar; 2-2-2 – Femoral route – Tip – straddles tricuspid annulus in its superior portion
- 30. Anatomy of RA • Components – RA appendage – Venous part – Vestibule, inferiorly near TV annulus – Septum – Sulcus Terminalis / Crista separates RAA and venous part – Sinus node situated in the Sulcus terminalis at SVC – RA junction
- 31. RAO view
- 32. Anatomy of RA - RAO view
- 39. BASIC EP INTERVALS AND PROTOCOLS
- 43. Right, The distal portion of the CS is closer to the ventricle (originating as great cardiac vein on the anterior wall); the CS crosses the atrioventricular (AV) groove at the lateral margin and becomes an entirely atrial structure as it empties into the right atrium (RA). Left, Thus, proximal CS recordings show large atrial and small ventricular signals, whereas more distal recordings show small atrial, large ventricular signals.
- 46. MEASUREMENT OF CONDUCTION INTERVALS • Range of screen or paper speed generally used is 100 to 400mm/sec • To evaluate sinus node function 100mm/sec is adequate • Routine refractory period studies require slightly faster speeds (150 to 200mm/sec) • For detailed mapping of endocardial activation paper speeds of ≥200mm/sec or more should be used. • Accuracy at 100mm/sec is approx ± 5msec • Accuracy at 400mm/sec is approx ± 1msec
- 47. P Wave-Atrial Interval • The P wave-atrial interval is measured from the first evidence of sinus node depolarization, whether on the intracardiac or surface ECG, to the atrial deflection as recorded in the HB lead. It represents conduction through the RA to the inferoposterior interatrial septum (in the region of the AVN and HB). • The normal range of the PA interval is 25 to 55 milliseconds • Rarely, diseased atrial conduction can underlie first-degree AV block, indicated by a prolonged PA interval. A short PA interval suggests an ectopic source of atrial activation.
- 48. Atrial–His Bundle Interval • The AH interval is measured from the first rapid deflection of the atrial deflection in the HB recording to the first evidence of HB depolarization in the HB recording • Is an approximation of the AVN conduction time, because it represents conduction time from the low RA at the interatrial septum through the AVN to the HB. • The AH interval has a wide range in normal subjects (55 to 125 milliseconds) and is markedly influenced by the autonomic nervous system
- 49. ASSESSMENT OF H-V INTERVAL • Time from depolarization of proximal His bundle to the onset of ventricular depolarization ranges from 35 to 55 msec. NOTE- RBB deflection invariably occurs 30msec or less before ventricular activation. Thus , during sinus rhythm an apparent His deflection of less than 30msec either reflects recording of a bundle branch potential or the presence of preexcitation. • Shorter than 35msec – an accessory pathway is usually present producing ventricular preexcitation during sinus rhythm. • Prolonged H-V interval longer than 70msec suggest a possible AV block • More than 100 msec is severe abnormalitry and warrants permanent pacemaker
- 56. 56 Drive train with a single extra stimulus S1 S1 S1 S1 S1 S1 S1 S1 S2Sensed PAUSEDRIVETRAIN S1-S2 Interval Sense-S1 Interval
- 57. 57 Extra stimuli S 1 S 1 S 1 S 1 S 1 S 1 S 1 S 1 S 2Sensed DRIVETRAIN S 3 S 4 S1 S1 S1 S1 S1 S1 S1 S1 S2Sensed DRIVETRAIN S 1 S 1 S 1 S 1 S 1 S 1 S 1 S 1 S2Sensed DRIVETRAIN S3 single double triple
- 58. Sinus Node Recovery Time • It is the interval measured in the HRA from the last paced complex to the first spontaneous complex after the cessation of pacing • Evaluate the effect of overdrive suppression on sinus node automaticity
- 60. When corrected for the underlying baseline sinus cycle length CSNRT = SNRT – SCL Pacing at several cycle lengths (e.g. 600, 500, 400, 350, 300) Reasonable values: maximum SNRT < 1500 ms maximum CSNRT < 550 ms
- 61. 61 SNRT:1180 CSNRT: SNRT- SINUS CYCLE LENGTH = 400
- 62. SACT- defined as the conduction time between sinus node and the adjacent atrial tissue A2A3 = A1A1 + 2 X SACT SACT =(A2A3-A1A1) / 2 Ref. val. 50-115 ms
- 64. ….NEXT presentations • Basic EP protocols • Atrial arrhythmias • Ventricular Pre-excitation and AVRT • Ventricular arrhythmias • Catheter ablation
