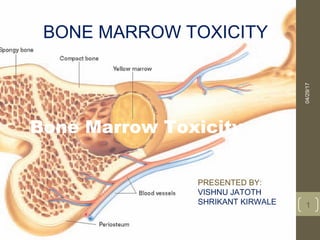
bone marrow toxicity& structure and function of bone marrow
- 1. Bone Marrow Toxicity 04/29/17bonemarrowtoxicity 1 BONE MARROW TOXICITY PRESENTED BY: VISHNU JATOTH SHRIKANT KIRWALE
- 2. Bone Marrow Specialized type of soft, diffuse connective tissue; called myeloid tissue Site for the production of blood cells Found in medullary cavities of long bones and in the spaces of spongy bone 04/29/17bonemarrowtoxicity 2
- 3. Bone Marrow Two types of marrow are present during a person’s lifetime: Red marrow Found in virtually all bones in an infant’s or child’s, adults body Functions to produce red blood cells Yellow marrow As an individual ages, red marrow is replaced by yellow marrow Marrow cells become saturated with fat and are no longer active in blood cell production 04/29/17bonemarrowtoxicity 3
- 4. Bone Marrow The main bones in an adult that still contain red marrow include the ribs, bodies of the vertebrae, the humerus, the pelvis, and the femur Yellow marrow can alter to red marrow during times of decreased blood supply, such as with anemia, exposure to radiation, and certain diseases 04/29/17bonemarrowtoxicity 4
- 5. Functions of Bone • Support—bones form the framework of the body and contribute to the shape, alignment, and positioning of the body parts • Protection—bony “boxes” protect the delicate structures they enclose • Movement—bones with their joints constitute levers that move as muscles contract • Mineral storage—bones are the major reservoir for calcium, phosphorus, and other minerals • Hematopoiesis—blood cell formation is carried out by myeloid tissue 04/29/17bonemarrowtoxicity 5
- 6. Regulation of Blood Calcium Levels • Skeletal system serves as a storehouse for about 98% of body calcium reserves • Helps maintain constancy of blood calcium levels • Calcium is mobilized and moves in and out of blood during bone remodeling • During bone formation, osteoblasts remove calcium from blood and lower circulating levels • During breakdown of bone, osteoclasts release calcium into blood and increase circulating levels 04/29/17bonemarrowtoxicity 6
- 7. Regulation of Blood Calcium Levels Skeletal system Homeostasis of calcium ion concentration essential for the following: Bone formation, remodeling, and repair Blood clotting Transmission of nerve impulses Maintenance of skeletal and cardiac muscle contraction 04/29/17bonemarrowtoxicity 7
- 8. Regulation of Blood Calcium Levels Mechanisms of calcium homeostasis Parathyroid hormone Primary regulator of calcium homeostasis Stimulates osteoclasts to initiate breakdown of bone matrix and increase blood calcium levels Increases renal absorption of calcium from urine Stimulates vitamin D synthesis 04/29/17bonemarrowtoxicity 8
- 9. Regulation of Blood Calcium Levels Mechanisms of calcium homeostasis Calcitonin Protein hormone produced in the thyroid gland Produced in response to high blood calcium levels Stimulates bone deposition by osteoblasts Inhibits osteoclast activity Less important in homeostasis of blood calcium levels than parathyroid hormone 04/29/17bonemarrowtoxicity 9
- 10. Development of Bone Osteogenesis—development of bone from small cartilage model to an adult bone Intramembranous ossification Occurs within a connective tissue membrane Flat bones begin when groups of cells differentiate into osteoblasts Osteoblasts are clustered together in centers of ossification Osteoblasts secrete matrix material and collagenous fibrils 04/29/17bonemarrowtoxicity 10
- 11. Development of Bone Cont….. Large amounts of ground substance accumulate around each osteoblast Collagenous fibers become embedded in the ground substance and constitute the bone matrix Bone matrix calcifies when calcium salts are deposited Trabeculae appear and join in a network to form spongy bone Apposition growth occurs by adding of osseous tissue 04/29/17bonemarrowtoxicity 11
- 12. Development of Bone Endochondral ossification Most bones begin as a cartilage model, with bone formation spreading essentially from the center to the ends Periosteum develops and enlarges, producing a collar of bone Primary ossification center forms Blood vessel enters the cartilage model at the midpoint of the diaphysis 04/29/17bonemarrowtoxicity 12
- 13. Development of Bone Endochondral ossification Bone grows in length as endochondral ossification progresses from the diaphysis toward each epiphysis Secondary ossification centers appear in the epiphysis, and bone growth proceeds toward the diaphysis Epiphyseal plate remains between diaphysis and each epiphysis until bone growth in length is complete 04/29/17bonemarrowtoxicity 13
- 14. Development of Bone Endochondral ossification Epiphyseal plate is composed of four layers: “Resting” cartilage cells—point of attachment joining the epiphysis to the shaft Zone of proliferation—cartilage cells undergoing active mitosis, causing the layer to thicken and the plate to increase in length Zone of hypertrophy—older, enlarged cells undergoing degenerative changes associated with calcium deposition Zone of calcification—dead or dying cartilage cells undergoing rapid calcification 04/29/17 bone marrow toxicity 14
- 15. Bone Growth and Resorption Bones grow in diameter by the combined action of osteoclasts and osteoblasts Osteoclasts enlarge the diameter of the medullary cavity Osteoblasts from the periosteum build new bone around the outside of the bone 04/29/17bonemarrowtoxicity 15
- 16. Repair of Bone Fractures Fracture—break in the continuity of a bone Fracture healing Fracture tears and destroys blood vessels that carry nutrients to osteocytes Vascular damage initiates repair sequence Callus—specialized repair tissue that binds the broken ends of the fracture together Fracture hematoma—blood clot occurring immediately after the fracture, is then resorbed and replaced by callus 04/29/17bonemarrowtoxicity 16
- 17. Cartilage Characteristics Avascular connective tissue Fibers of cartilage are embedded in a firm gel Has the flexibility of firm plastic No canal system or blood vessels Chondrocytes receive oxygen and nutrients by diffusion Perichondrium—fibrous covering of the cartilage Cartilage types differ because of the amount of matrix present and the amounts of elastic and collagenous fibers 04/29/17bonemarrowtoxicity 17
- 18. Cartilage Types of cartilage Hyaline cartilage Most common type Covers the articular surfaces of bones Forms the costal cartilages, cartilage rings in the trachea, bronchi of the lungs, and the tip of the nose Forms from specialized cells in centers of chondrification, which secrete matrix material Chondrocytes are isolated into lacunae 04/29/17bonemarrowtoxicity 18
- 19. Cartilage Types of cartilage Elastic cartilage Forms external ear, epiglottis, and eustachian tubes Large number of elastic fibers confers elasticity and resiliency Fibrocartilage Occurs in symphysis pubis and intervertebral disks Small quantities of matrix and abundant fibrous elements Strong and rigid 04/29/17bonemarrowtoxicity 19
- 20. Cartilage Growth of cartilage Interstitial or endogenous growth Cartilage cells divide and secrete additional matrix Seen during childhood and early adolescence while cartilage is still soft and capable of expansion from within 04/29/17bonemarrowtoxicity 20
- 21. Cartilage Growth of cartilage Appositional or exogenous growth Chondrocytes in the deep layer of the perichondrium divide and secrete matrix New matrix is deposited on the surface, increasing its size Unusual in early childhood but, once initiated, continues throughout life 04/29/17bonemarrowtoxicity 21
- 22. DRUGS THAT CAUSE BONEMARROW TOXICITY • CYTOTOXIC CHEMOTHERAPEUTIC DRUGS • NSAIDS • ANTI THYROID DRUGS • BONEMARROW TRANSPLANTATION 04/29/17bonemarrowtoxicity 22
- 23. DRUGS THAT CAUSE …… • vincristine • zidovudine: postmarketing, uncommon • zidovudine • 6-mercaptopurine • EDTA • allopurinol • amiodarone • amitriptyline • anthracycline • azathioprine 04/29/17bonemarrowtoxicity 23 • carbamazepine • chloramphenicol • doxorubicin • imatinib: uncommon • imipramine • methotrexate • methyldopa • metronidazole • valproate Cytopenia is a reduction in the number of blood cells.
- 24. Azathioprine Induced Pancytopenia Azathioprine is commonly used for management of lupus nephritis Mild myelotoxicity is a common side effect of azathioprine, however, severe myelosuppression leading to pancytopenia is uncommon In vivo , it is converted, non-enzymatically, to 6-mercaptopurine, Further metabolism of this drug involves various enzymes like, hypoxanthine guanine phosphoribosyl transferase (HGPRT) thiopurine methyltransferase, xanthine oxidase HGPRT is responsible for its bio-activation and converts it to 6-thioinosine 5-monophosphate which is further metabolized to 6-thioguinine nucleotides (6-TGNs) 6-GTNs get incorporated into DNA and RNA and are possibly, responsible for cytotoxic effect 04/29/17 bone marrow toxicity 24
- 25. CDK FAMILY among the first targeted therapy approaches pursued for the treatment of cancer Palbociclib Palbociclib was recently approved by the FDA in combination with letrozole for the treatment of first-line advanced breast cancer. FLAVOPERIDOL
- 26. MEGALOBLASTIC ANEMIA DHFRas e reductas e Inhibitors like MTX,BARBITURATES,PHEN YTOIN Examination of peripheral blood shows an increase in the mean corpuscular hemoglobin concentration. VITAMINE B12, FOLATE CONCENTRATION CAN DIAGNOSE.
- 27. RIBAVARIN hepatitis C infection
- 28. Reference • T.M. Fliedner, D. Graessle, C. Paulsen, and K. Reimers. Cancer Biotherapy and Radiopharmaceuticals. July 2004, 17(4): 405-426 • GREGORY S. TRAVLOS, Normal Structure, Function, and Histology of the Bone Marrow Toxicologic Pathology, 34:548–565, 2006 • Rinaldo Florencio-Silva et al: Biology of Bone Tissue: Structure, Function, and Factors That Influence Bone Cells, BioMed Research International Volume 2015 :52-65 • Kamakshi Rao, Drug-Induced Hematologic Disorders, chapter 24, section 2 , McGraw-Hill Education, 367, 2014. • Wenyue Hu1, Tae Sung1, Bart A. Jessen1, Stephane Thibault1, Martin B. Finkelstein2,Nasir K. Khan3, and Aida I. Sacaan1, Mechanistic Investigation of Bone Marrow Suppression Associated with Palbociclib and its Differentiation from Cytotoxic ChemotherapiesPublished OnlineFirst December 2, 2015; DOI: 10.1158/1078-0432.CCR-15-1421 04/29/17bonemarrowtoxicity 28
