Perianal Diseases Guide
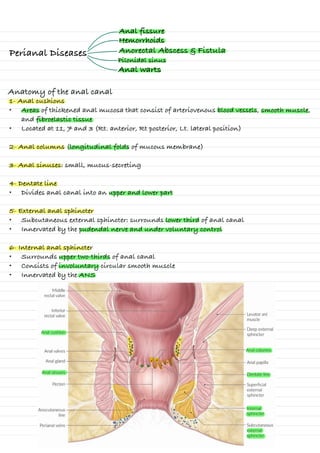
- 1. Perianal Diseases Anal fissure Hemorrhoids Anatomy of the anal canal 1- Anal cushions • Areas of thickened anal mucosa that consist of arteriovenous blood vessels, smooth muscle, and fibroelastic tissue • Located at 11, 7 and 3 (Rt. anterior, Rt posterior, Lt. lateral position) 2- Anal columns (longitudinal folds of mucous membrane) 3- Anal sinuses: small, mucus-secreting 4- Dentate line • Divides anal canal into an upper and lower part 5- External anal sphincter • Subcutaneous external sphincter: surrounds lower third of anal canal • Innervated by the pudendal nerve and under voluntary control 6- Internal anal sphincter • Surrounds upper two-thirds of anal canal • Consists of involuntary circular smooth muscle • Innervated by the ANS Anorectal Abscess & Fistula Pilonidal sinus Anal warts
- 2. Perianal Diseases Anatomy • The surgical anal canal is about 4 cm in length • Dentate line is the junction between the superior 2/3 and inferior1/3 anal canal • The dentate line is surrounded by longitudinal mucosal folds External sphincter (Red) • Bulk of the anal sphincter complex • Voluntary muscle • Innervated by Pudendal Nerve Internal sphincter (white) • Thickened distal • Involuntary • Innervated by ANS Intersphincteric plane • A potential space between ES & IS. it contains intersphincteric anal glands Anal fissure A longitudinal tear in the anoderm (epithelial) of the distal anal canal posterior midline in >85% of cases, anterior midline(10-15%) Symptoms • Pain at defecation • Bleeding (fresh) “Hematochezia” • Pruritus and discharge • Constipation Signs Acute: • Anal skin is puckered Chronic: • Skin tag(sentinel tag) • Hypertrophied anal papilla Etiology Primary (Local Trauma) • Chronic constipation or diarrhea • Anal sex Secondary (Underlying disease) • IBD (Crohn disease) Diagnostics • History • Clinical examination . ~ is 1 A. 10-15%. 9 - - 3 P 8s Acute fissure cronich fissure arouich fissure #yperbrophied And Papilla ⑧ E Skin Tag Skin tag op
- 3. Treatment • Perianal ulcer • Anal fistula or abscess • Anal carcinoma Differential diagnoses Conservative • Dietary improvement (Increase dietary fiber and water) • Stool softeners (e.g., docusate) • Anti‑inflammatory and analgesic creams and/or suppositories (e.g., 2% lidocaine) • Sitz baths • Topical vasodilator therapy (calcium channel blocker gel) Outpatient procedures • Bot. toxin A (botox) injection into the internal anal sphincter Surgical (lateral internal sphincterotomy) • when conservative treatment is unsuccessful • Disadvantage is risk of fecal incontinence Hemorrhoids Are dilated submucosal vascular cushions within the anal canal • Excessive straining (Chronic constipation) • Extended periods of sitting • Pregnancy • Older age Etiology Classificatio n 1-Internal hemorrhoids • Develop above the dentate line, which is not innervated by cutaneous nerves; distension does not cause pain. 2- External hemorrhoids • Develop below the dentate line, which is innervated by cutaneous nerves; distention of this innervated skin due to thrombosis results in severe pain. Grading of internal hemorrhoids Grade Palpation findings I Hemorrhoids bleed but do not prolapse. II Prolapse when straining, but spontaneously reduce at rest III Prolapse when straining; only reducible manually IV Irreducible prolapse; may be strangulated and thrombosed with possible ulceration
- 4. Clinical features 1- Internal hemorrhoids • Painless • Bright red bleeding at the end of defecation • Perianal mass in the event of prolapse • Pruritus 2- External hemorrhoids • Bright red bleeding • pruritus • perianal mass • perianal pain Diagnostics 1- History 2- physical Examination • Perianal examination • Digital rectal examination • Anoscopy • Proctoscopy • Anal skin tags (Polyps) • Hypertrophied anal papillae (Anal fissures) • Anal carcinoma • Anorectal varices DDx Treatment 1- Conservative treatment (Grade I II) • Dietary improvement (Increase dietary fiber and water) • Stool softeners (e.g., docusate) • Anti‑inflammatory and analgesic creams and/or suppositories (e.g., 2% lidocaine) • Sitz baths 2- Non-Surgery (procedures) (Grade I , II) • Rubber band ligation • Sclerotherapy • Infrared coagulation 3- Surgery (Grade III IV + Unsuccessful treatment) • Hemorrhoidectomy ASK GOOgIe NOT ME ASK GOOgIe NOT ME ASK GOOgIe NOT ME ⑤ II I I= I 'f -many means
- 5. Is a pus-filled develops from an infected anal gland following obstruction and bacterial overgrowth Anorectal Abscess Etiology • Obstruction and infection of the anal crypt glands (90%) • IBD (Crohn's disease, ulcerative colitis) • Malignancy (colorectal cancer) Classification Anal abscesses and fistulae • Perianal (most common) ◦ Abscess under the perianal skin ◦ Does not transverse the external sphincter • Ischiorectal: abscess below the levator ani muscle • Intersphincteric: abscess between the internal and external sphincters • Supralevator (least common): abscess above the levator ani muscle 2- Fistulas (Park's classification) • Intersphincteric (Park's Type I) • Transsphincteric (Park's Type II) • Suprasphincteric (Park's Type III) • Extrasphincteric (Park's Type IV) • Subcutaneous 1- Abscesses Most Common Clinical features • pruritus • Erythematous • subcutaneous mass • Pain Diagnostics • CT • MRI • Endoscopy and U/S Treatment 1- Abscesses • Surgical incision and drainage • Postoperative ◦ Sitz baths ◦ Analgesics and stool softeners ◦ Antibiotics 2- Fistulae • Fistulotomy (standard approach) • Possible seton placement (enables adequate drainage and fibrosis) • Possible fibrin glue or fistula plug • Antibiotics fi 0 - ⑮ . . . . . . )>)=>)* .js an
- 6. Pilonidal sinus Is a skin condition caused by local inflammation of the superior midline gluteal cleft, which may progress to a local abscess or fistula. • Young men with excessive body hair • Obesity • Deep gluteal cleft • Poor anal hygiene Risk factors • fever • painful • Erythematous swelling • Discharge (Possible purulent discharge) Clinical features Differential diagnoses • Anal fistula (e.g., due to Crohn disease) • Hidradenitis suppurativa • Anorectal abscess • Sacrococcygeal teratoma Treatment Conservative treatment • Indications ◦ Asymptomatic patients ◦ Postsurgical care of symptomatic patients • Approach ◦ Improved local hygiene Surgical treatment • Indication ◦ symptomatic patients • Procedures 1- Acute pilonidal cyst: incision and drainage, with secondary wound closure 2- Chronic or recurrent pilonidal sinus: surgical resection ▪ Primary wound closure ▪ Secondary wound closure
- 7. Anal warts • HPV types 6 and 11 They spread by ❖ Anal Sex ❖ Directly from the genitals • Exophytic • Pruritus • Discharge • Bleeding in rare cases • Pain Infections of the skin and mucous membranes by HPV, HPV may lead to anal cancer Etiology Clinical features Diagnostics • Application of 5% acetic acid turns lesions white • biopsy Treatment 1- Pharmacotherapy • local cytostatic treatment (podophyllin) • Immune response modifiers (imiquimod) 2- Surgical excision
