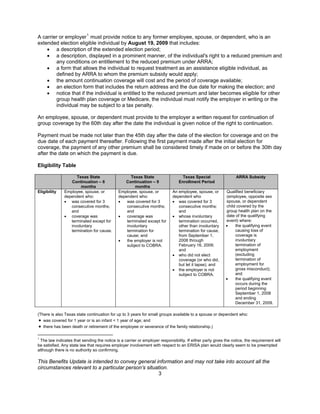
Texas has extended its state continuation coverage program temporarily for small groups. Eligible employees whose coverage was terminated, except for cause, can now continue coverage for up to nine months. There is also a special enrollment period for those terminated between September 2008 and February 2009. This aims to allow access to the new federal premium subsidy under ARRA. However, eligibility is limited as an individual must not have been fired for cause. Employers must notify former employees of the new provisions by August 2009.