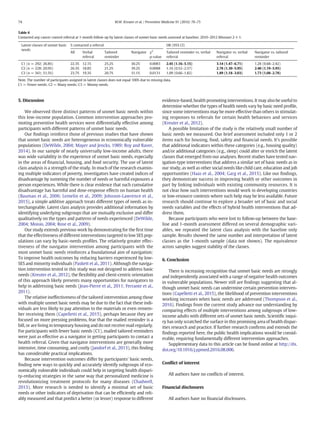
This document describes a study that examined how unmet basic needs cluster in low-income populations and how the effectiveness of health interventions may vary based on levels of unmet basic needs. The study analyzed data from a randomized controlled trial where low-income callers to a 211 helpline received cancer screening referrals along with one of three interventions: verbal referral only, verbal referral plus a printed reminder, or verbal referral plus navigation from a health coach. Latent class analysis identified three classes of unmet basic needs among participants. Logistic regression found that for those with relatively more or money-specific unmet needs, the navigator intervention was more effective at linking them to health referrals, while the printed reminder worked as well as the navigator for those