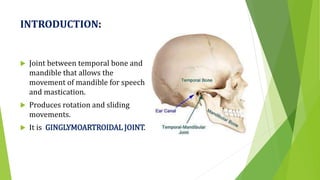
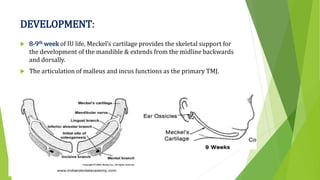
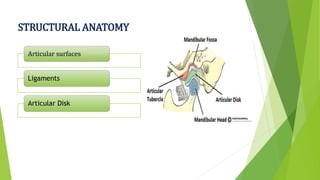
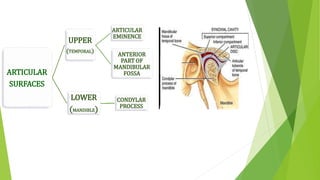
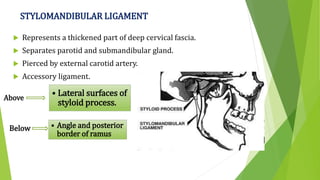
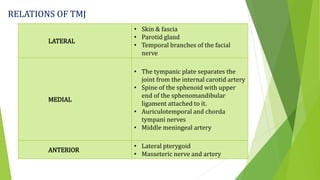
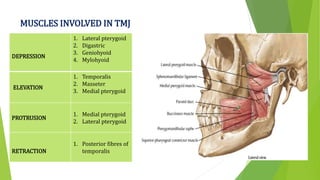
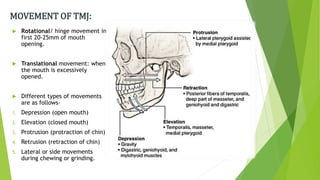
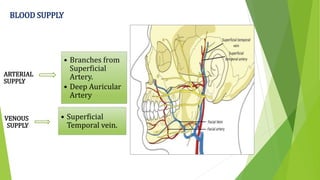
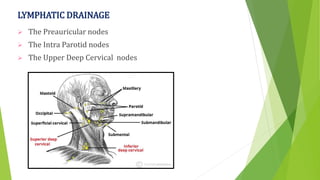
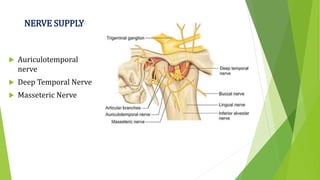
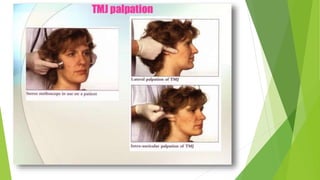
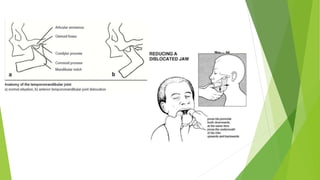
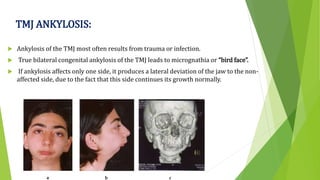
The document provides a comprehensive overview of the temporomandibular joint (TMJ), including its anatomy, developmental stages, functions, and associated disorders. It highlights the unique characteristics of TMJ as a mobile joint in the skull, its movements, and the various factors leading to temporomandibular disorders (TMD). Additionally, it discusses examination techniques and conditions such as dislocation, ankylosis, and osteoarthritis affecting the TMJ.