Dr. Jawarkar's Guide to Sputum Examination
- 1. 1 Notes on sputum examination…By Dr. Ashish V. Jawarkar Contact: pathologybasics@gmail.com Website: pathologybasics.wix.com/notes SPUTUM EXAMINATION
- 2. 2 Notes on sputum examination…By Dr. Ashish V. Jawarkar Contact: pathologybasics@gmail.com Website: pathologybasics.wix.com/notes OVERVIEW 1. Indications 2. Collection of sputum 3. Sample transport 4. Sample analysis a. Physical examination b. Microbiological examination 1. Gram stain 2. Culture and sensitivity 3. Examination for acid fast bacilli a. Zn stain b. Fluorescent stain c. Culture on conventional media d. Commercial automated culture system e. Molecular methods 4. Examination for other specific organisms c. Cytological examination
- 3. 3 Notes on sputum examination…By Dr. Ashish V. Jawarkar Contact: pathologybasics@gmail.com Website: pathologybasics.wix.com/notes * Indications 1. Smear and culture Identification of causative organism in a suspected infection - like pneumonia, TB, fungal infection, P. carinii in HIV, bronchiectasis 2. Cytological examination 1. for malignant cells 2. Looking for viral inclusions 3. asbestosis * Collection of sputum 1. Early morning deep cough sample is preferred 2. If unable to cough, induction of sputum can be done by a.15% NaCl aerosol spray & propylene glycol for 20 min or b.Nebulized hypertonic saline and distilled water Collected in: 1. dry wide mouthed container with 25 ml capacity 2. leak proof – to prevent aerosols 3. break resistant – to prevent dessication * Sample transport 1. samples should be immediately transported to laboratory as such if nearby 2. if distant laboratory, transport in 25 ml of the following solution N acetyl pyridinium chloride 5g Sodium chloride 10g Distilled water 1 lt If sputum is allowed to stand without medium – a. rapid proliferation of contaminating bacterial flora from oral cavity and throat b. H. influenzae donot survive for long Donot refrigerate in any case
- 4. 4 Notes on sputum examination…By Dr. Ashish V. Jawarkar Contact: pathologybasics@gmail.com Website: pathologybasics.wix.com/notes * SAMPLE ANALYSIS (i) Physical appearance Bloody (hemoptysis) Pulmonary TB Lung abcess Bronchiectasis Bronchogenic carcinoma Mitral stenosis Pulmonary infarction Rusty Pneumococcal lobar pneumonia Red currant jelly Klebsiella Green Pseudomonas Purulent Pneumonia, lung abcess Pink and frothy Pulmonary edema (ii) Microbiological examination #GRAM STAIN: Prerequisites 1. There should not be squamous cells covered with masses of bacteria – indicates sample is mostly from mouth or throat 2. If PMNs are <10 per epithelial cell – no need for culture 3. Knowledge of flora of mouth and pharynx necessary before analyzing Normal flora of oral cavity and pharynx GRAM POSITIVE 1. staphylococcus aureus and epidermidis 2. streptococcus viridans and pneumonia 3. diphtheroids 4. enterococci 5. micrococci 6. lactobacilli 7. yeasts (candida) GRAM NEGATIVE 1. neiserria 2. H. influenzae 3. fusobacterium 4. coliforms 5. m. catarrhalis
- 5. 5 Notes on sputum examination…By Dr. Ashish V. Jawarkar Contact: pathologybasics@gmail.com Website: pathologybasics.wix.com/notes Analysis Streptococcus Pneumoniae Gram positive diplococci with surrounding clear space Staphylococcus aureus Gram positive cocci in grape like clusters Candida Gram positive yeast cells with budding yeasts and pseudohyphae H. influenzae Gram negative coccobacilli M. catarrhalis Gram negative diplococci both intra and extracellular Actinomyces Large granules with center gram negative and periphery gram positive #CULTURE: Ideal sample for culture 1. should contain <25 squamous cells per low power filed or <10 squamous cells per high power field 2. sample should contain alveolar macrophages 3. neutrophils should be >10 per epithelial cell or >5 per high power field 4. bronchial epithelial cells present 5. sample should be washed with normal saline to wash the saliva Method: Inoculate the sample on blood agar and chocolate agar Incubate in an atmosphere of extra CO2 Inspect plates after 18 hours If growth is significant, antibiotic sensitivity testing is carried out
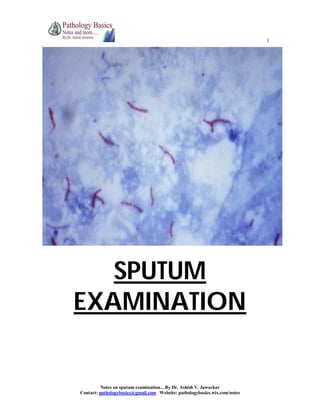
- 6. 6 Notes on sputum examination…By Dr. Ashish V. Jawarkar Contact: pathologybasics@gmail.com Website: pathologybasics.wix.com/notes #EXAMINATION FOR ACID FAST BACILLI !. ZEIHL NEELSON STAINING (AFB stain) Sample: 1. According to RNTCP guidelines, 2 samples are collected, one stat and one early next morning sample. It should be deep cough sputum sample 2. for children, gastric aspirate can be used as they often swallow sputum Preparation: smear is prepared with blood tinged/opaque/grayish/yellowish portion of the sputum stained with ZN stain Examined under microscope Reporting guidelines (RNTCP): 1. Mycobacteria appear as bright red, slightly curved or red beaded rods, 2-4 µm in length and 0.2 to 0.5 µm wide, against a blue green background. 2. Atleast 100 fields should be examined before declaring negative. Drawbacks: 1. sensitivity 60-80% 2. minimum 5000-10000 bacilli / ml should be present for smear to be positive Bleaching technique: 1. A solution of sodium hypochlorite is added to sputum sample – it leads to liquefaction of mucous and killing of microbes 2. smears are prepared from sediment and stained with ZN stain
- 7. 7 Notes on sputum examination…By Dr. Ashish V. Jawarkar Contact: pathologybasics@gmail.com Website: pathologybasics.wix.com/notes 2. FLUORESCENCE MICROSCOPY 1. Slides are stained with fluorescent auramine-rhodamine or auramine O 2. Observed under fluorescent microscope – mycobacteria appear bright yellow against green background 3. CULTURE ON CONVENTIONAL MEDIA Indications: 1. drug susceptibility testing 2. species identification if other than M. tuberculosis suspected 3. sputum smear negative and strong clinical suspicion Prerequisites: 1. 4% NaOH should be added before inoculation 2. this is because sputum samples are contaminated with normal flora, which grow and digest the media before MTB can grow 3. 4% NaOH kills this flora Media used: 1. solid media – LJ media (egg based) or Middle brook (agar based) 2. Liquid media – middle brook, TH9, TH 12 Advantage: 1. sensitivity 80-85% 2. can detect as low as 10-100 bacteria/ml Drawbacks: 1. expensive 2. requires 6 weeks for results 4. COMMERCIAL AUTOMATED CULTURE METHODS (BACTEC) 1. Can give results in 2 weeks 2. mycobacteria are inoculated in a broth containing 14 C palmitate 3. mycobacteria metabolise 14 C palmitate and release 14 CO2 which is detected by the instrument 5. MOLECULAR METHODS (PCR) 1. DNA sequences identified in MTB genome by PCR 2. can detect bacteria as low as 10-100 organisms / ml of sputum 3. direct sputum sample or culture samples can be used 4. laboratory cross contamination is an important issue here
- 8. 8 Notes on sputum examination…By Dr. Ashish V. Jawarkar Contact: pathologybasics@gmail.com Website: pathologybasics.wix.com/notes #EXAMINATION OF OTHER ORGANISMS ON SMEAR SPECIFIC INVESTIGATIONS P. carinii Use BAL and stain with silver stain and giemsa Yersinia Giemsa stain Fungus SDA/KOH mount Histoplasma Giemsa Aspergillus KOH Paragonimus Saline wet mount of sputum for eggs
- 9. 9 Notes on sputum examination…By Dr. Ashish V. Jawarkar Contact: pathologybasics@gmail.com Website: pathologybasics.wix.com/notes (iv) Cytological examination Prerequisites: 1. fresh morning sample 2. transport without delay 3. for suspected lung Ca collect sample for 5 consecutive days 4. if delay anticipated, prefix with Saccomano’s fixative (50% ethyl alcohol and 2% carbowax) Method: 1. smears are made from blood tinged portion or tissue fragments and stained with pap stain 2. to be adequate, bronchial epithelial cells and alveolar macrophages must be seen Drawback: Sensitivity is only 65% This sensitivity is more if – 1. smears are examined from multiple samples 2. lesion is located centrally 3. larger tumor size 4. histologic type is SCC rather than adenocarcinoma