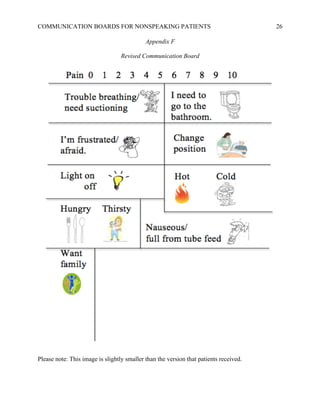
When nonspeaking patients on a specialized medical-surgical unit were provided with a simplified communication board, nurse-patient communication improved and patient frustration decreased. Patients and nurses completed surveys before and after the communication board was provided. The final results showed reduced time to communicate, improved understanding between nurses and patients, and lower frustration levels for both patients and nurses.